21 Eyelid Reconstruction
GOALS AND PRINCIPLES
Loss of eyelid tissues most often results from trauma and surgical excision of neoplasms. Congenital colobomas and necrosis or cicatricial contraction following periocular infections, radiation, cryotherapy, or thermal burns also may cause eyelid defects. The goals of eyelid reconstruction are to reestablish functional eyelids, with an acceptable cosmetic appearance, that provide adequate protection of the globe.
Surgeons who plan to perform eyelid reconstruction must bear in mind the anatomic and functional components of the eyelids. A smooth, mucous membrane internal lining is mandatory to maintain lubrication of the ocular surface and avoid corneal irritation. A rigid support normally provided by the tarsus is essential to retain the eyelid shape and its vertical position, yet it must be flexible enough to mold to the curvature of the globe. A stable eyelid margin is necessary to keep the lashes and skin directed away from the cornea and to retain a smooth contour in contact with the eye. Proper fixation of the medial and lateral canthal attachments of the lids will add to the eyelid stability and its proper orientation. A muscle layer is needed to provide enough tone and power to achieve eyelid closure. Finally, the overlying skin has to be thin and supple to accommodate eyelid excursion.
Upper eyelid defects are especially challenging to reconstruct, given the additional requirements for mobility and the upper lid’s major contribution to corneal protection. Levator muscle action must be adequate to elevate the eyelid above the visual axis; also, the lid must be of sufficient size and be elastic enough to cover the cornea. Upper lid defects are poorly tolerated by the exposed ocular surface and usually require an expeditious repair. The integrity of the eye protective mechanisms, such as Bell’s phenomenon and tear film quality and production, affects the duration that the cornea will tolerate the increased exposure.
The eyelids may be anatomically divided into two layers, both of which must be replaced in the repair of full-thickness defects to satisfy their functional requirements. The anterior lamella, which consists of the skin and orbicularis muscle, partly supports the lower lid position, provides dynamic closure of the upper and lower lids, and contributes to the lacrimal pump mechanism. It may be reconstructed with advancement or rotation myocutaneous flaps or full-thickness skin grafts. The tarsus and its conjunctival lining constitute the posterior lamella and provide structural integrity to the lid with a mucosal surface. Reconstruction of this layer may involve tarsal transposition or rotation flaps, free autogenous tarsal grafts, sliding tarsal conjunctival flaps, or tarsal substitutes, including auricular cartilage, nasal septal chondromucosa, and hard palate mucosa. Commercially available xenografts, such as ENDURAGen collagen implants (Porex Surgical, Inc., Newnan, Georgia), and allografts, such as preserved sclera and AlloDerm Regenerative Tissue Matrix (LifeCell Corporation, Branchburg, New Jersey), have become popular for use as posterior lamellar grafts as they are readily available and do not require the additional surgical time and effort needed to harvest an autogenous graft. The surgeon should consider, however, that there is a rare possibility of disease transmission with any nonautogenous graft. When reconstructive methods are utilized to create this bilamellar configuration, at least one of the two layers must have its own inherent blood supply.
Techniques for eyelid reconstruction can be grouped according to the tissues employed. Adjacent tissues used for repair of lid defects, such as direct closure, the Tenzel semicircle flap, and myocutaneous advancement flaps, are ideal because they provide their own blood supply, maintain the same color and surface characteristics as the normal lid tissues, and contract less than a graft. Eyelid tissue from the opposite lid may be transposed, as in the Cutler-Beard and Hughes procedures, which also use tissues similar in character. Contiguous, but more remote, periocular tissues can be used, such as the temporal forehead (Fricke) flap, or glabellar and median forehead flaps. The remaining alternative technique of autogenous grafts, including contralateral eyelid and postauricular skin, tarsus, nasal or ear cartilage grafts, allografts, and xenografts, is usually applied for repair of extensive eyelid defects. The reconstructive surgeon should be familiar with a variety of techniques, given that variations or different combinations of multiple methods may be necessary to properly reconstruct the eyelids.
PREOPERATIVE EVALUATION AND MANAGEMENT
Before deciding which technique to apply, examine the defect, noting its size, location, configuration, and depth, as well as consider the patient’s age. Full-thickness eyelid marginal defects are divided according to size into small (<25%), moderate (25%–50%), and large defects (>50%). Table 21.1 indicates the techniques described in this chapter according to defect size. The availability of tissues utilized in different reconstructive methods is also determined by whether the defect is located centrally, medially, or laterally.
Reconstructive techniques also differ for defects in the medial and lateral canthus (see Table 21.1). When the defect is superficial, only the anterior lamella may need to be repaired, whereas full-thickness defects require re-formation of both anatomic layers. The periocular tissues in elderly patients typically exhibit greater elasticity than those in young patients, allowing them to stretch more easily to reduce the defect size. Finally, if a patient requires lid reconstruction with only one functioning eye on the same side, alternative techniques to avoid a lid-sharing procedure should be considered.
A thorough knowledge of the anatomy and blood supply of the eyelids, lacrimal drainage system, and periocular tissues is essential before performing eyelid reconstruction. Previous radiation, surgery, and chemical or thermal burns may compromise the blood supply to the tissues employed for reconstruction; in such cases, use of tissues that provide their own blood supply is preferable. Methods to salvage the canaliculi might be necessary for repair of defects involving the medial eyelid.
Before reconstruction of an eyelid defect that resulted from the excision of a malignancy, it is imperative that the margins of the remaining tissue are free of tumor. This can be ascertained histologically during the surgical removal of the neoplasm by Mohs micrographic surgical techniques or by frozen-section analysis. This precaution is taken not only to minimize the chance of recurrent tumor but also to prevent spread of tumor along newly created surgical planes or transposed tissues, such as from the lower lid to the upper lid following a Hughes reconstruction. Violation of intact bone should also be avoided for at least 1 to 2 years following the initial excision of periocular malignancies, allowing time for monitoring the area for tumor recurrence. Such methods as creating an osteotomy for conjunctival dacryocystorhinostomy with a Jones tube or transnasal wiring create a potential pathway for spread of recurrent tumor into the adjacent sinuses and nasal cavity.
The patient should refrain from taking aspirin or aspirin-containing products for 2 weeks before surgery. Also, prior to surgery, the discontinuation of taking other products that inhibit platelet aggregation, such as clopidogrel bisulfate and dipyridamole, or interfere with clotting factor synthesis, such as warfarin, is also advised to reduce intraoperative and postoperative bleeding; however, before stopping any of these medications, the patient’s prescribing physician should be consulted. The techniques described in this chapter are the author’s procedures of choice or are standard procedures with which the reconstructive surgeon should be familiar. These methods singly or in combination should be effective in the repair of most eyelid defects.
Anesthesia
Eyelid reconstruction can be performed under local anesthesia, with or without mild sedation, in almost all patients except children and very anxious adults. Subcutaneous infiltration of 2% lidocaine with a 1:100,000 dilution of epinephrine should be administered at the edges of the defect as well as in those tissues that the surgeon anticipates will be manipulated for the reconstruction. If a lengthy procedure is anticipated, 0.75% bupivicaine with a 1:100,000 dilution of epinephrine can be mixed with lidocaine to prolong the anesthetic effect. Once the tissues are infiltrated, the surgeon should wait approximately 10 minutes to allow the epinephrine to achieve the vasoconstrictive effects that facilitate hemostasis. Topical 1% tetracaine hydrochloride drops will provide adequate anesthesia for the ocular surface.
Lower eyelid reconstruction
Direct closure with or without lateral cantholysis
Eyelid defects involving up to one third of the central lower lid margin can be repaired by primary closure techniques. Depending on the laxity of the periocular tissues, a lateral cantholysis may be necessary to provide sufficient relaxation of the lower lid attachments to directly close the defect without excessive tension. This method of reconstruction is the most commonly employed for lid margin defects and has the advantage of being a single-staged technique that maintains an anatomically normal lid margin with preservation of eyelashes.
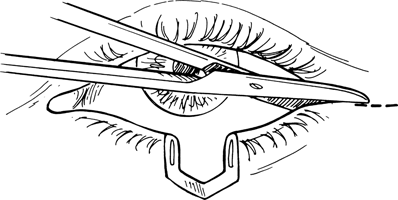
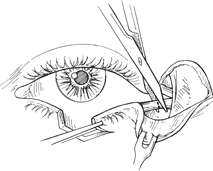
Figure 21-1. The edges of the eyelid defect should be trimmed, if necessary, so that the tarsal borders are sharp and perpendicular to the lid margin and the tissues inferior to the tarsus are cut into a wedge, forming a pentagonal-shaped defect. Bleeding should be meticulously controlled with a bipolar cautery. While grasping each end of the defect with a toothed forceps, if the borders of the defect can be approximated without extensive tension on the wound edge, a direct closure can be undertaken; however, if the edges cannot be brought together easily, a lateral cantholysis is necessary.
To perform a cantholysis, a 4- to 5-mm horizontal incision is made with a Stevens scissors from the lateral canthal angle toward the orbital rim through skin and orbicularis muscle (see Fig. 21-1). With the canthal tendon split into the superior and inferior division, medial traction is applied to the lateral lid margin, and the tip of Westcott scissors is used to identify the firm lateral attachments of the lower lid.
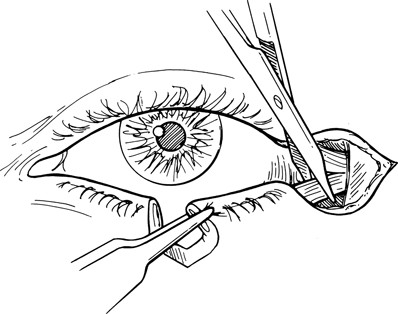
Figure 21-2. The inferior crus of the lateral canthal tendon is then either partially or completely transected by making a vertical incision with scissors until the lateral margin of the defect can be mobilized medially to close the wound without tension. Disruption of the conjunctiva during the cantholysis should be avoided. The canthotomy incision is closed with interrupted 7–0 nylon or 6–0 fast-absorbing plain gut sutures.
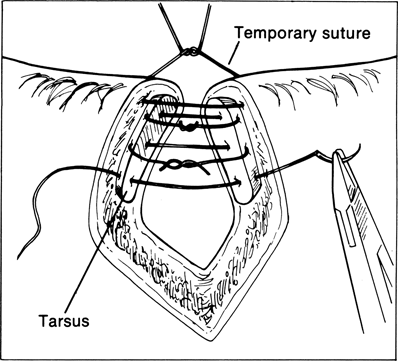
Figure 21-3. The first and most important step to primarily close a lid margin defect is the approximation of the edges of the tarsus. Exact vertical alignment of these edges is necessary to yield a satisfactory lid margin repair and this layer provides most of the tension-bearing support of the wound.
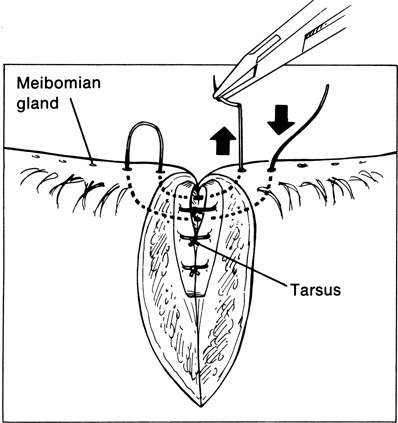
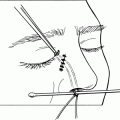
Figure 21-4. Closure of the lid margin is achieved by placing a vertical mattress suture through the lid margin for proper anteroposterior alignment. A 6–0 silk suture enters a meibomian gland orifice 3 mm from the wound edge and exits through the tarsal plate 3 mm from the lid margin; it then enters the tarsus on the opposing edge, 3 mm from the lid margin and exits from a meibomian gland orifice 3 mm from the cut edge. The suture is then passed back through the lid margin in a near-to-near fashion, entering and exiting through a meibomian gland orifice only 1 mm from the wound edge. This suture is tied tightly enough to achieve moderate eversion of the lid margin.
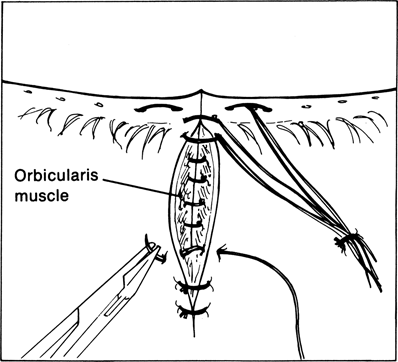
Figure 21-5. Two additional interrupted 6–0 silk sutures are passed, one just posterior to the lashes and one just beneath the lashes. The ends of these three silk sutures are left long and secured away from the wound on the lower lid skin with a suture or Steri-strip at the conclusion of the procedure to prevent them from irritating the cornea. The anterior lamella is closed in a layered manner by first suturing together the edges of orbicularis muscle with interrupted 6–0 or 7–0 Vicryl sutures with their knots buried.
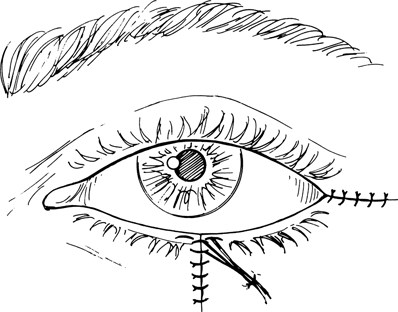
Figure 21-6. Skin closure is achieved with 7–0 nylon or 6–0 silk interrupted sutures. A dog ear of redundant skin at the inferior edge of the wound, if present, should be trimmed.
Periosteal strip and myocutaneous advancement flap
A periosteal strip and myocutaneous flap can be used to reconstruct the lateral one third of the lower lid when there is no tarsus remaining at the lateral margin of the defect. The periosteal strip can also be used in combination with other reconstructive methods for larger defects. The basic premise of this technique is that the hinged strip of periosteum obtained from the lateral orbital rim provides the posterior lamellar support of the re-formed lateral lower lid with proper posterior fixation.
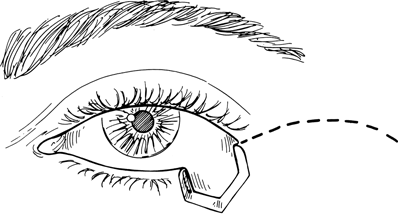
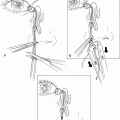
Figure 21-7. Mobilization of a composite skin and orbicularis muscle flap is first performed by outlining an advancement flap with a marker pen either in a semicircular manner or as a cheek flap extended 1 to 2 cm beyond the lateral commissure. The skin incision is made with a size 15 Bard-Parker blade, and scissors are used to cut through the orbicularis muscle down to the orbital rim. Extensive undermining of the temporal eyelid and cheek skin and muscle is performed with Stevens scissors, as needed, to allow mobilization of the myocutaneous flap nasally.
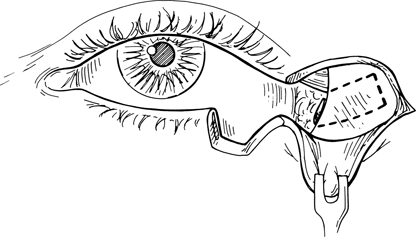
Figure 21-8. With retraction of the skin-muscle flap, the lateral orbital rim is exposed, and a rectangular strip of periosteum is fashioned, with an intact base at the inner aspect of the rim. The strip is 1 cm wide and is angled superiorly 45° to follow the lower lid contour. The length of the strip is determined by the distance measured from the rim to the lateral edge of the tarsal defect. If the strip needs to be >1 cm in length, the adjacent temporalis fascia can be incorporated by extending the periosteal incisions laterally.
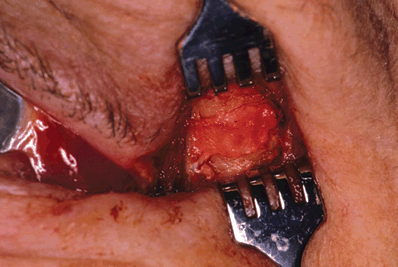
Figure 21-9. The fascia is then bluntly dissected from the underlying temporalis muscle, and the periosteal portion of the strip is separated from the bony rim with a periosteal elevator.
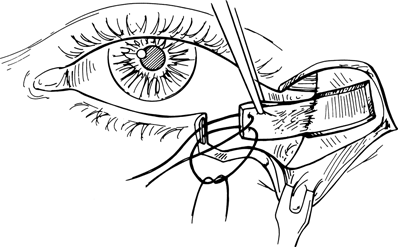
Figure 21-10. The strip is reflected medially so that the anterior surface of the periosteum lies against the globe and its distal end is sutured to the anterior portion (partial-thickness) of the lateral border of tarsus with 5–0 Vicryl sutures. This provides a posterior lamella and anchors the reconstructed lower lid to the orbital rim.
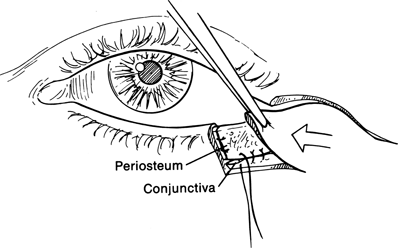
Figure 21-11. The edge of the inferior forniceal conjunctiva can be secured to the inferior edge of the periosteal strip and the inner surface of the strip will epithelialize. Symblepharon should not develop as long as the opposing bulbar conjunctiva is intact.
The myocutaneous flap is advanced nasally to reestablish an anterior lamella and tension-bearing 6–0 Vicryl buried-interrupted sutures are placed at the level of the muscular layer.
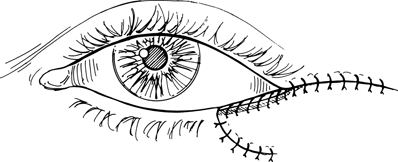
Figure 21-12. The superior skin edge of the myocutaneous flap along the lateral lid margin is joined to the superior border of the periosteal strip with a running 7–0 Vicryl suture. The skin is closed with 7–0 nylon or 6–0 silk sutures.
Semicircular rotational flap
Reconstruction of up to two thirds of the central lower lid can be achieved by combining the primary closure technique with a lateral semicircular musculocutaneous flap as described by Tenzel (1975). The tarsus must be present on both sides of the defect, and the edges of the wound should be prepared as described earlier for direct closure.
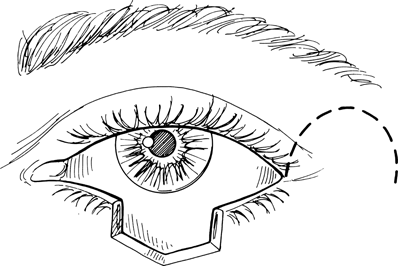
Figure 21-13. A marker pen is used to outline a semicircle, approximately 20 mm in diameter, beginning at the lateral canthal angle, arching superiorly and temporally no farther than the lateral extent of the brow. A skin incision is made along this mark with a size 15 Bard-Parker blade. The skin edges are tented up with forceps, and a Westcott or Stevens scissors is used to dissect through the orbicularis muscle fibers down to the lateral orbital rim.
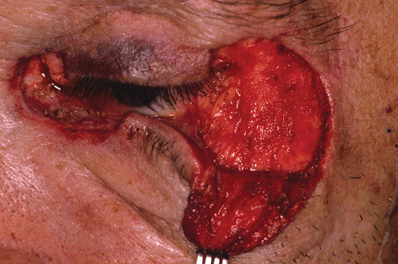
Figure 21-14. The myocutaneous flap is undermined thoroughly inferiorly to mobilize this tissue medially. All bleeding points should be cauterized with a bipolar electrocautery.
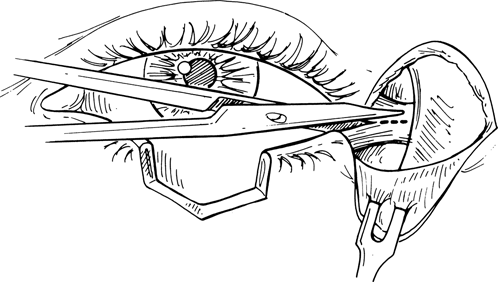
Figure 21-15. With the flap retracted inferiorly, a canthotomy is performed with the scissors extending to the inside of the orbital rim.
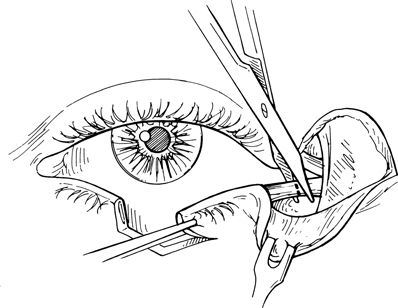
Figure 21-16. The inferior crus of the lateral canthal tendon is cut at the rim. The superior crus of the canthal tendon should be left undisturbed. The lateral portion of the lower lid and adjacent flap are rotated medially until the edges of the lid margin defect can be apposed without undue tension, and the defect is directly closed as previously described. If the lateral aspect of the lid cannot be adequately mobilized, its attachments to the orbital septum and lower lid retractors must be severed. Scissors can be introduced just beneath the inferior tarsal border, anterior to the conjunctiva and posterior to the orbicularis muscle, and the septum and retractors are detached from lateral to medial until the lid can be freely rotated nasally.
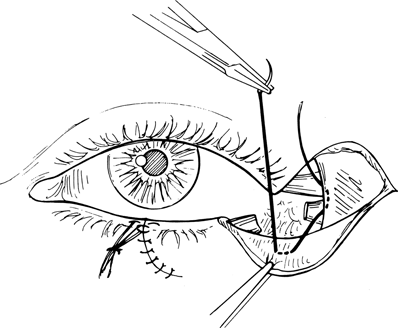
Figure 21-17. Re-formation of the lateral canthus begins with proper fixation of the lateral aspect of the flap to provide adequate posterior and lateral vector forces so that the reconstructed lower lid lies in apposition with the globe. This is achieved by suturing the deep edge of the myocutaneous flap to the inner aspect of the lateral orbital rim just inferior to the attached superior crus of the canthal tendon with a 4–0 Vicryl suture passed on a small semicircle needle.
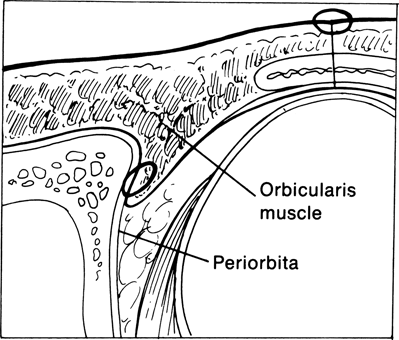
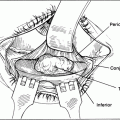
Figure 21-18. A cross-sectional view of the lateral orbit and lower eyelid demonstrates suture fixation of the deep tissues of the semicircular flap to the inner aspect of the lateral orbital rim to provide adequate apposition of the reconstructed lid with the globe. The lid must be tight and have the proper contour following this suture placement to avoid postoperative sagging or lid margin malpositions.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree