Key Words
eyelids, ectropion, facial burns, corneal injury, exposure keratopathy, facial contracture, periorbital region
Synopsis
The sequelae of facial burn injury can be devastating. Involvement of the eyelid area is of particular importance, both functionally and esthetically. It is essential to recognize eyelid injuries early and to institute aggressive management to prevent immediate and long-term consequences. Although injuries to the globe and loss of vision are very uncommon, inappropriate management of these injuries may lead to corneal and ocular problems that, in the majority of cases, are preventable if they were not part of the presenting burn. With appropriate and proactive management and judicious attention to fundamental principles, these injuries may be managed with confidence and excellent outcomes, even in the most severely injured patients.
Clinical Problem
Presentation
The periorbital region, in particular the eyelids, is a common site of involvement in facial burns. This area is of critical functional and esthetic importance. The loss of the eye itself is thankfully a rare sequela of thermal, and even caustic, injury. It is beyond the scope of this chapter to discuss the ocular management of facial burns. Suffice it to say that close collaboration and consultation from colleagues in ophthalmology are mandatory and will help ensure optimal care of these injuries in the acute and chronic stages of evaluation and management. The majority of this chapter will focus on secondary management of eyelid burns and the reconstruction options typically used in our practice.
Etiology
Thermal and caustic injuries will compromise the majority of pathology seen. Scald and flame burn injuries appear to be the most common thermal burns suffered in the periorbital area. Caustic burns from acid attacks are also common injuries seen, in particular in certain geographical distributions in the world, such as Africa and India. The highest at-risk populations include the elderly, those who are disabled, children, and those populations in high-prevalence areas of acid attacks, as retribution injury victims.
The release of contractures and placement of autografts have been and continue to be a mainstay of treatment. Today, we are fortunate to have learned much about burn scar biology and behavior and about how to use old and new methods to optimize management and outcomes. Many of the recommendations made herein are also steeped in decades of observation, experience, and fundamental principles that have allowed for excellent outcomes and that have limited additional morbidity in this area of reconstructive burn surgery.
Associated Conditions
Many of these injuries have low incidences of scleroconjunctival, corneal, or eyelid injuries that require more than conservative treatment. When injuries are more substantial and that is not the case, appropriate acute and chronic management of these patients will dictate short- and long-term outcomes. Corneal injury or scleroconjunctival irritation or exposure is best managed in close collaboration with an ophthalmologist.
Pre-Operative Management
Physical Examination and Key Anatomy
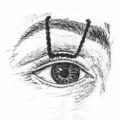
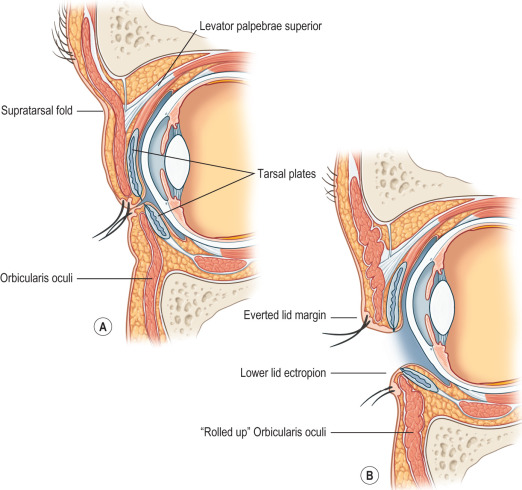
The periorbital region is notable for being very thin and an area with minimal to no subcutaneous fat, which results in burns that are generally deeper than similar burns suffered elsewhere on the body. We know that the depth of burn injury is dependent on numerous factors, including intensity of exposure, duration of exposure, and the associated epidermal and dermal thickness in the region of injury. The pattern of injury is also not typical and is dependent on these factors. Injuries that initially may appear to indicate partial-thickness involvement may progress to full-thickness if not managed appropriately. In the periorbital region, there is very little room for diagnostic or management error because the aforementioned facts make this area prone to devastating long-term sequelae. The delicate lamellar anatomy of the periorbital region must be considered in preservation of eyelid function and in any reconstructive efforts instituted in a treatment algorithm ( Fig. 4.3.1 ). There are excellent references that discuss the patterns of burn injury and the burn wound model as a dynamic, evolving process (for further exploration, see the References section).
Pre-Operative Testing
It is recommended that formal ophthalmological consultation be obtained. Examining gross visual acuity with a Snellen eye chart, performing light perception checks, and evaluating for any foreign bodies or debris are very quick things the reconstructive surgeon can do as part of the initial workup and examination. It is important to understand the degree of burn injury as it relates particularly to the eyelids. For the purposes of this chapter, we will outline the classification system typically used in our practice not only to help understand the appropriate diagnosis but also to demonstrate how these various depths of injury will dictate modifications to plan management and treatment execution and facilitate pre-operative planning.
First-degree (epidermal) burns are limited to the epidermis and do not involve blistering. Typically, healing is seen within approximately 7 days, and scarring of any remarkable nature is uncommon.
Second-degree (partial-thickness) burns break the epidermal barrier and invade the dermis to varying depths. These are divided into superficial and deep partial-thickness burns. In superficial partial-thickness burns, the epidermis and the superficial papillary dermal layer are involved, and typically blistering is seen. These injuries predictably heal within approximately 14 days with minimal scarring. In deep partial-thickness burns, the depth of involvement reaches to the reticular dermal layer and is a more complicated matter. Blistering is seen, but the underlying dermal elements are more difficult to assess and there are fewer viable skin-regenerative elements. The healing is slower and takes approximately 21 or more days with resultant scar contracture. These injuries require early operative management to limit such sequelae of secondary eyelid contracture and malposition.
Third-degree (full-thickness) burns violate all dermal layers and all regenerative elements. These injuries are noted to be painless due to sensory innervation loss. Healing in these injuries will occur only via epithelialization from wound edges and will predictably lead to remarkable wound contraction and scar hypertrophy. Early, tangential burn wound excision and autologous skin grafting are the mainstay of management here.
Fourth-degree (deep) burns violate underlying muscle, connective tissue, bone, and vital structures. These injuries require complex management and are beyond the scope of this chapter. Complicated reconstructive surgical techniques such as loco-regional flaps, free tissue transfer, and even vascularized composite allotransplantation consideration are necessary to mitigate the substantial functional and esthetic deformities encountered in these injuries.
Optimal Timing of Surgery
Based on the aforementioned classification system, burn depth and degree will dictate much of operative intervention considerations and timing. In the acute stages, very little from a surgical perspective needs to be done other than aggressive globe protection and lubrication. If the eyelid domain is compromised, immediate intervention is indicated to prevent exposure keratopathy. Otherwise, most surgical management decisions can be made in the weeks after initial injury, when it becomes clear what the depth of injury and resultant deformities will be.
Supplies Needed
The majority of supplies needed for management of these injuries are available within the emergency room or acute care environment. Eye lubricants, globe protective shields, patches, and such items should be readily available. In more complicated or extensive burn injuries, the operating theater is the best place to address close evaluation and management with all relevant supplies available, including eyelid retractors, debridement kits, and suture materials for temporary tarsorrhaphy.
Anesthesia Concerns
As with all burn injury evaluations, possible airway injury and inhalational-associated sequelae are important and should be discussed with the anesthesiology team before operative consideration. Additionally, it may be difficult in the acute setting of extensive facial burns or airway edema to secure an appropriate nasotracheal or orotracheal airway, and in such circumstances tracheostomy should be discussed.
Surgery
The entire periorbital region and the adjacent areas of the face and neck are all of importance when discussing burn reconstruction of the eyelids and adnexa. Eyelid skin is the thinnest skin of the entire body, and burn injuries to this area have a high risk of developing early and late wound healing complications. Whether a burn injury is in the acute or later phases, the goal is the same: to protect the globe from exposure complications and to preserve corneal and scleroconjunctival integrity so that visual loss can be prevented.
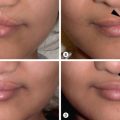
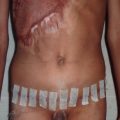
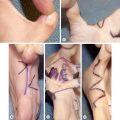
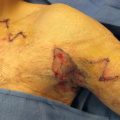
In the acute phase, upper and lower eyelid ectropion may occur from direct injury to the eyelid tissues, causing intrinsic contractures. After burn wounds have healed or have been closed by grafting, the prolonged processes of wound contraction and scar maturation create tension that can secondarily cause ectropion of the eyelids without a direct injury to the eyelid tissues having occurred ( Fig. 4.3.2 ). This is called extrinsic ectropion and frequently occurs from contracted scars and grafts on the cheeks and even the neck. Accurate diagnosis of the cause of eyelid ectropion is essential to direct therapy at the correct cause and obtain the best possible outcome. In cases of severe ectropion, early surgical intervention is mandatory to prevent irreversible visual impairment, particularly corneal ulceration ( Fig. 4.3.3 ). Temporary maneuvers such as tarsorrhaphy or special contact lens coverage can offer short-term solutions, but these are not effective practically for more than a few days to a week without other adjunctive surgical intervention. Definitive treatment involves the release of contracture with skin grafting (split-thickness or full-thickness) and can be utilized in the presence of nearby wounds or other complicating factors to restore protective eyelid functional globe coverage ( Figs. 4.3.4 and 4.3.5 ).