Key points
- •
Understanding the differences in hair structure and haircare practices in African Americans compared with white, Hispanic, and Asian patients is essential when evaluating and treating hair concerns in this population.
- •
Structural characteristics of Afro-textured hair include a retroverted hair bulb, an S-shaped follicle, and an elliptical-shaped hair shaft.
- •
Hairstyles such as tight buns and ponytails, braids, dreadlocks, and weaves increase the risk of developing traction alopecia, which is present in approximately one-third of women of African descent.
- •
Both scarring and nonscarring alopecias can affect the skin of non-white patients. However, some types of hair loss appear to be more common in men and women of African descent, including traction alopecia, acquired trichorrhexis nodosa, seborrheic dermatitis, alopecia areata, central centrifugal cicatricial alopecia, folliculitis decalvans, acne keloidalis nuchae, and dissecting cellulitis.
- •
Various treatment options exist for alopecia in patients with skin of color, and the choice of treatment depends on the underlying diagnosis.
- •
Effective treatment options for androgenetic alopecia include topical minoxidil and low-level laser light therapy in men and women and oral 5α-reductase inhibitors in men.
Introduction
Non-white patients, specifically those of African descent, have unique hair characteristics and haircare practices. Understanding the differences seen in the hair of African Americans compared with white, Hispanic, and Asian patients is essential when evaluating and treating hair concerns in this population. Hair is classified into three types: African, Asian, and Caucasian ( Fig. 2.1 ). Each of these differ in structure, growth rate, and density. This chapter will focus on Afro-textured hair.
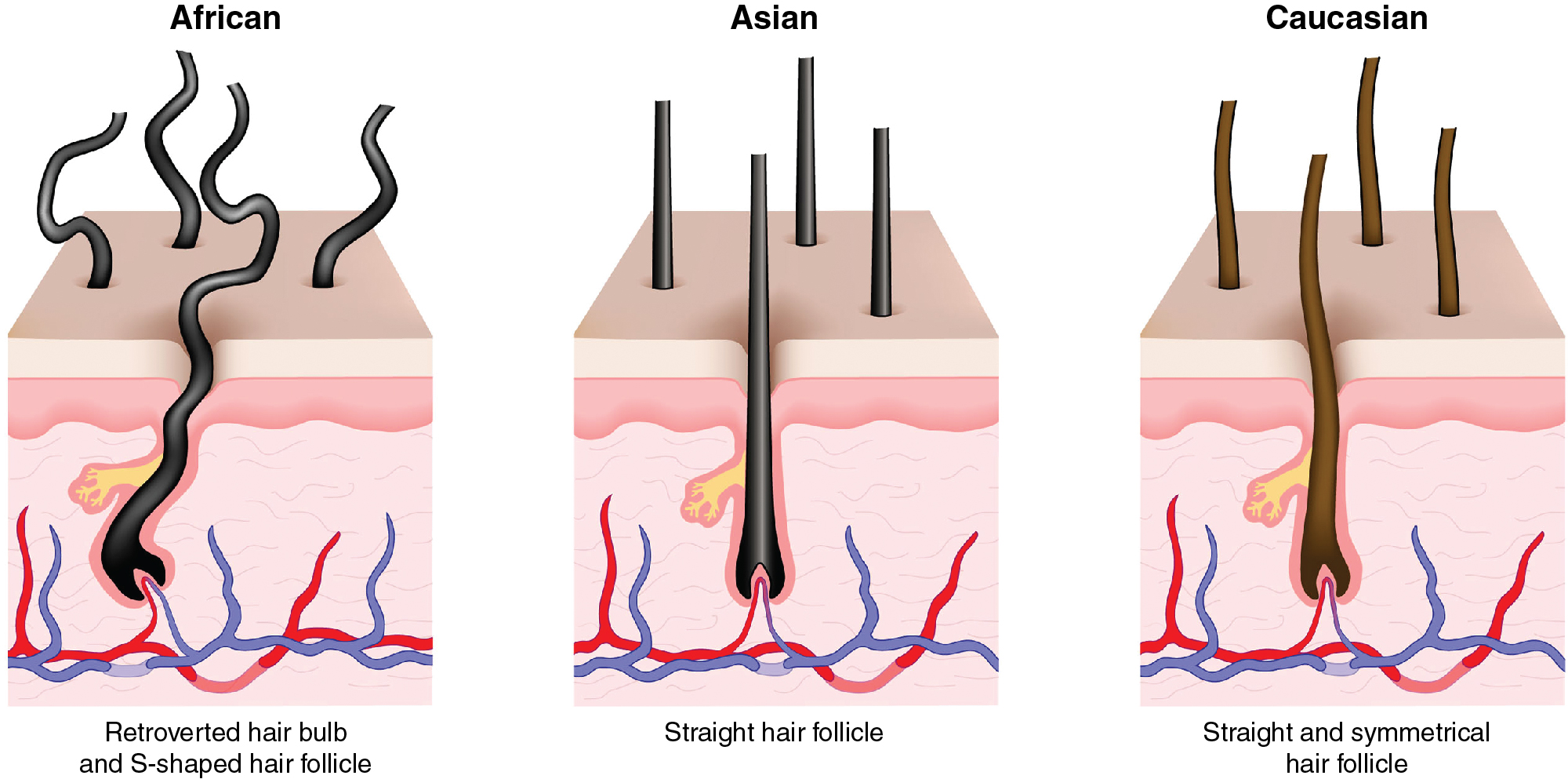
The structural characteristics of Afro-textured hair include a retroverted hair bulb that resembles the shape of a golf club, an S-shaped follicle, and an elliptical-shaped hair shaft (level of evidence: 2b). The retroverted hair bulb is responsible for the curly configuration of Afro-textured hair (level of evidence: 2b). One theory is that the curly nature of the hair prevents even distribution of sebum along the hair shaft, leaving the scalp oily and hair shaft prone to dryness (level of evidence: 5). Additionally, Afro-textured hair is lower in density and has a slower growth rate compared with Caucasian hair (level of evidence: 5), regardless of scalp region or gender (level of evidence: 2b). It is important for dermatologists to understand the unique features of Afro-textured hair in addition to cultural haircare practices and hairstyles, as this may facilitate compliance with treatment and help discern practices that may negatively affect scalp disease.
Cultural differences in persons with skin of color
Societal beauty standards have often valued the European aesthetic, which can negatively affect Black women’s perception of their own body image (level of evidence: 2b). In a research study conducted by Awad et al., a cohort of black women were surveyed on body image concerns. Researchers found that hair was the most important body image domain. Participants reported that their hair influenced their self-confidence. Additionally, the pressure to adhere to societal and personal beauty standards led to significant sacrifices of time and money. Recognition of these factors can help dermatologists understand why patients may be hesitant to change haircare practices or styles, even if recommended as part of a hair-loss treatment regimen.
Exercise also affects haircare practices. A study completed by Ahn et al. found that women of African descent modified their hairstyles to accommodate physical activity. This included wearing braids, a ponytail or bun, or the use of a scarf or hair wrap (level of evidence: 2b). Additionally, 18% of these women exercised less often to avoid sweating out hairstyles.
When evaluating a patient with hair loss, the place to begin is with a thorough hair-loss history. In the case of patients with Afro-textured hair, asking the right questions is paramount ( Pearl 2.1 ). Onset and type of symptoms and the affected location of the scalp are important for all patients with hair loss, but for those with Afro-textured hair, a number of specific haircare questions must be included: use of chemical relaxers, traction-related hair styles (hair weaves, braids, locks) (level of evidence: 5), , frequency of hair washing, use of heat for straightening, and other product use. Moreover, clinicians should approach these encounters with empathy and acknowledge the significant psychosocial implications that may accompany hair loss (level of evidence: 5).
Obtaining a hair history and completing a thorough examination of the scalp are essential in diagnosing alopecia in patients with Afro-textured hair.
Common forms of hair loss that affect patients with skin of color
Although we will focus on androgenetic alopecia (AGA), several other forms of hair loss are important to discuss, as they may be in the differential diagnosis of AGA or complicating the treatment of AGA ( Pearl 2.2 ).
It is important to successfully treat inflammatory scalp disease prior to beginning any topical treatments for pattern hair loss, because the presence of inflammation can complicate treatment.
Nonscarring alopecias
Nonscarring alopecias are common and can be associated with hairstyles and haircare practices. With prompt diagnosis and treatment, hair regrowth is attainable. In this section, we present several nonscarring alopecias that may be seen in patients with Afro-textured hair.
Androgenetic alopecia or pattern hair loss
Androgenetic alopecia (AGA), also known as female or male pattern hair loss (FPHL/MPHL), is a common nonscarring alopecia with a characteristic pattern distribution. The population frequency and severity increase with age in both men and women. Patients typically experience slow, progressive hair loss, and associated symptoms may include pruritus and trichodynia (level of evidence: 5). The prevalence of pattern hair loss is highest in Caucasian males and females compared with Asians (level of evidence: 2b). There is currently no data on the prevalence of pattern hair loss in men and women of African descent.
FPHL presents as a reduction in scalp hair density, primarily in the vertex and frontal scalp. This is caused by follicular miniaturization and an increase in vellus follicles (level of evidence: 2b). The vellus hair follicles have a reduced anagen cycle, leading to short, fine hair shafts (level of evidence: 5). As the hairs become thinner, the central part appears wider on the frontal scalp compared with the occipital scalp (level of evidence: 5). Women may present with diffuse thinning in the vertex scalp, thinning that is more prominent in the frontal scalp, resulting in a “Christmas tree pattern” (level of evidence: 5), or bitemporal thinning. Although bitemporal hair loss is common in FPHL, it can also be seen in traction alopecia, telogen effluvium (TE), alopecia areata (AA), frontal fibrosing alopecia (FFA), central centrifugal cicatricial alopecia (CCCA), and seborrheic dermatitis (level of evidence: 5). In FPHL, the frontal hairline is typically spared ( Pearl 2.3 ). The etiology is likely caused by an interplay of genetics, hormones, and environmental factors. Although some women with FPHL have excessive androgen production, others have normal levels of androgens, leaving the exact role of androgens in FPHL poorly understood.
Bitemporal hair loss can be a manifestation of pattern hair loss, traction alopecia, telogen effluvium, alopecia areata, frontal fibrosing alopecia, central centrifugal cicatricial alopecia, or seborrheic dermatitis.
MPHL presents as hair loss in the temporal, midfrontal, or vertex scalp. Dihydrotestosterone binds to androgen receptors in hair follicles, which leads to suppression of hair growth by miniaturization of hair follicles (level of evidence: 5). The severity and areas of involvement are variable. Different regional patterns of hair loss are caused by differences in follicle sensitivity to dihydrotestosterone.
The differential diagnosis of pattern hair loss is extensive and includes CCCA, FFA, folliculitis decalvans (FD), and, rarely, dissecting cellulitis (DC). The presence of inflammation or scarring is not consistent with pattern hair loss and should prompt consideration of another cause of alopecia. Underlying medical conditions such as eating disorders leading to malnutrition, iron deficiency, or thyroid dysfunction should also be explored, as they may result in diffuse hair loss that may appear more pronounced on the vertex scalp caused by mild underlying pattern hair loss (level of evidence: 5). The goal of treatment is to prevent progression of hair loss and reverse the miniaturization process. Treatment options that have proven to be effective in randomized controlled trials include topical minoxidil and low-level laser light therapy in men and women, and oral 5α-reductase inhibitors in men (level of evidence: 1b). Other off-label treatment options for women include oral 5α-reductase inhibitors, as well as antiandrogen therapies such as spironolactone, cyproterone acetate (outside the United States), and flutamide (level of evidence: 5). In the twenty-first century, low-dose, oral minoxidil has been gaining favor for the treatment of pattern hair loss in both men and women. Scalp hair restoration may be performed for men and women with severe cases (level of evidence: 5).
Traction alopecia
Approximately one-third of women of African descent have traction alopecia, which clinically appears as thinning and hair loss at the frontotemporal scalp. Although it is typically believed that traction alopecia is caused by excessive tension on the hair shaft (level of evidence: 2b) as a result of tight hair styling and haircare practices (level of evidence: 5), it is not known if there is genetic predisposition contributing to the development of traction alopecia. Hairstyles that result in increased risk of traction alopecia include tight buns and ponytails, braids, dreadlocks, and weaves (level of evidence: 2b). The prevalence is higher in long, relaxed hair and when styles such as braids are applied to relaxed hair ( Pearl 2.4 ). Scalp symptoms in the frontotemporal scalp, such as stinging, pain, pustules, and crusting, are the harbingers of tight hair styles and increase the likelihood of the clinical appearance of traction alopecia (level of evidence: 2b). , Clinically, perifollicular erythema is the first sign of traction alopecia (level of evidence: 2b). The fringe sign, or presence of vellus hairs along the frontal or temporal scalp, is both sensitive and specific to traction alopecia. Tenting of the hair follicle, which occurs when the hair is pulled so tightly that it raises the scalp, is also indicative of excessive tension. Early intervention is paramount in treatment of traction alopecia, as only early stages are thought to be nonscarring; long-standing traction can be unresponsive to treatments or changes in haircare practices. Patients should be encouraged to discontinue high-risk hairstyles immediately. A discussion including gentle hair-style recommendations that can replace high-traction styles should occur. Even nocturnal hair treatments such as hair wrapping that can aggravate traction should be discussed, as they must be discontinued as well (level of evidence: 5). Medical treatments include oral and topical antibiotics if there is folliculitis, and topical or intralesional corticosteroids if inflammation is present (level of evidence: 5). Intralesional corticosteroids combined with topical minoxidil have shown to be effective (level of evidence: 2b), as has topical minoxidil alone (level of evidence: 1a). There have been reports of successful hair transplantation, punch grafting, and rotation flaps for advanced traction alopecia (level of evidence: 4). ,
Hairstyles such as tight buns and ponytails, braids, dreadlocks, and weaves increase the risk of developing traction alopecia, which is present in approximately one-third of women of African descent.
Acquired trichorrhexis nodosa
Afro-textured hair retains less moisture and is more fragile than other hair types, which increases susceptibility to breakage (level of evidence: 2b). , In acquired trichorrhexis nodosa (ATN), the hair shaft is fragile, dull, and may have visible nodes (level of evidence: 5). Clinically, ATN can be identified by broken hair shafts with frayed ends of uneven lengths (level of evidence: 5). Gentle tugging on the distal ends of the hair shaft (tug test) may result in breakage of small hair fragments (level of evidence: 5). Topical minoxidil may cause scalp dryness, which is more commonly seen when the 5% solution is used for its increased propylene glycol content (level of evidence: 5). This dryness may extend down the hair shaft, making it difficult to use topical minoxidil. Khumalo et al. found that Afro-textured hair has the same distribution of cysteine-rich proteins as white and Asian hair, suggesting physical trauma rather than trichothiodystrophy triggers the hair fragility seen in patients of African descent (level of evidence: 2b). Additionally, haircare practices such as chemical relaxers, permanent hair color, drying agents such as gels and spritzes, and thermal straightening, including the use of ceramic flat irons, have been associated with an increased risk of ATN (level of evidence: 5). , , Treatment of ATN includes screening for and treating underlying conditions such as hypothyroidism, iron deficiency, and nutritional deficiencies followed by discontinuation of haircare practices that increase risk of breakage. A healthy haircare routine that consists of moisturizing shampoo and moisturizing products used no more than once per week and the use of leave-in hair shaft conditioners to help moisturize the hair is recommended (level of evidence: 5).
Seborrheic dermatitis
Seborrheic dermatitis is a chronic inflammatory condition that affects sebaceous-rich areas such as the forehead, eyebrows, nasolabial folds, and scalp. Although the etiology is unknown, Malassezia furfur is likely involved in the pathogenesis (level of evidence: 5). African American patients commonly seek help from dermatologists for this condition, which was the third most common diagnosis in a large database study and in the top five conditions seen in a study of patients in a skin of color clinic (level of evidence: 2b). , As the presence of inflammation can complicate the topical treatment of pattern hair loss, it is important to successfully treat seborrheic dermatitis prior to beginning any topical treatments for pattern hair loss.
Clinically, seborrheic dermatitis presents as scaly, flaky, and sometimes hypopigmented plaques. Inflammation and pruritis of the scalp can cause the patient to repetitively scratch the affected area, which may result in hair loss (level of evidence: 2b). To effectively treat seborrheic dermatitis, dermatologists must be aware of the cultural differences in haircare practices of patients with skin of color. Infrequent washing and the use of hair oils and pomades, both of which commonly occur in this population, may exacerbate seborrheic dermatitis (level of evidence: 5). Patients often apply these products to improve flaking and pruritus. Treatment modalities include antidandruff shampoos that contain zinc pyrithione, selenium sulfide, and tar. The shampoo should be applied only to the scalp to minimize dryness along the hair shaft. Topical corticosteroids, antifungals, and calcineurin inhibitors have also proven effective (level of evidence: 5). Patients with Afro-textured hair should be encouraged to wash their hair once a week or biweekly and refrain from excessive use of hair oils and pomades on the scalp.
Alopecia areata
Alopecia areata (AA) is autoimmune, inflammatory hair loss that may affect the scalp and/or body. Although the pathogenesis is not completely understood, studies have shown that cytotoxic NKD2+ T cells are necessary and sufficient to induce alopecia in mice. This work led to the understanding that IL-15 (required for the growth of natural killer cells) has been identified as a potential therapeutic target with Janus kinase (JAK) inhibitors affecting the signaling pathway of IL-15 (level of evidence: 2b). , In a study completed using the National Alopecia Areata Registry, researchers found that African Americans have higher odds of AA compared with their Caucasian counterparts (level of evidence: 3b). Clinically, AA presents as a sudden onset of patchy hair loss without signs of scarring or inflammation (level of evidence: 5). The extent of hair loss can vary from a small patch to complete loss of hair over the entire scalp and body. Rarely, bitemporal or vertex hair loss in AA may mimic pattern hair loss. Exclamation point hairs (short hairs that are thicker distally compared with proximally) are pathognomonic for AA (level of evidence: 5). Patients are typically asymptomatic, but some may experience itching, tingling, or dysesthesia prior to the onset of hair loss. Spontaneous hair regrowth may occur with subsequent relapse. Treatment includes topical, oral, or intralesional corticosteroids, topical minoxidil, and methotrexate (level of evidence: 1b). , ,
Scarring alopecias
Scarring or cicatricial alopecias are a result of inflammation that leads to follicular unit destruction. Once the hair follicle is no longer viable, hair loss is irreversible. This section includes details about clinical appearance and treatment options for scarring alopecias commonly seen in patients with Afro-textured hair. CCCA and FD are often in the differential diagnosis of pattern hair loss, and vertex and frontal thinning may occur in all these entities. Acne keloidalis nuchae (AKN) can interfere with donor area hair growth in patients with pattern hair loss, so this form of hair loss should be effectively treated.
Central centrifugal cicatricial alopecia
Central centrifugal cicatricial alopecia (CCCA) is the most common cause of scarring hair loss in patients of African descent (level of evidence: 5). It is a chronic, progressive, and inflammatory form of hair loss that begins on the vertex of the scalp and spreads centrifugally (level of evidence: 3b). The prevalence has been reported to range from 2.7% to 5.6%, and the average age of presentation is 36 years (level of evidence: 2b). , , Hair breakage in the vertex of the scalp has been reported as an early manifestation of CCCA (level of evidence: 4). This may be difficult for patients to visualize and appreciate, emphasizing the importance of a thorough scalp and hair examination when patients present to the dermatologist. It is also crucial to illicit a family history of hair loss, as one study found CCCA to be inherited in an autosomal dominant fashion with partial penetrance (level of evidence: 2b). Additionally, various research studies have found that haircare practices such as wearing braids with extensions, sew-in weaves, and glue-in weaves are associated with the development of CCCA (level of evidence: 3b). , A 2019 study by Malki et al. sought to identify a genetic association of CCCA (level of evidence: 3b). They found that mutations in the PADI3 gene, which is responsible for proper hair-shaft formation, are associated with CCCA. This data, combined with studies that noted an association between haircare practices and CCCA, suggest that the pathogenesis of CCCA is likely multifactorial. Clinical examination will reveal a smooth, shiny scalp with decreased or absent follicular ostia (level of evidence: 4). Although this disease may be asymptomatic, some patients experience pruritis, pain, pustules, or tenderness. , , The goal of treatment is to stop inflammation and scarring to preserve any remaining hair follicles. First, patients should be encouraged to discontinue all traumatic hair styling. Medical treatment includes the use of topical and intralesional corticosteroids, antidandruff shampoos, antimalarials, and oral and topical antibiotics (level of evidence: 5). Topical minoxidil can be used to prolong the anagen phase and treat coexisting FPHL (level of evidence: 5). If the inflammation has been controlled for a year, hair transplantation may be an option (level of evidence: 4). However, it is important to note that presence of scarring may hinder successful hair restoration. Discussion of realistic expectations with the patient is paramount and should focus on preventing progression of disease rather than hair regrowth.
Folliculitis decalvans
Folliculitis decalvans (FD) is a neutrophilic cicatricial alopecia that presents with alopecic patches, pustules, crusts, and tufted hairs (level of evidence: 2b). The patches most commonly occur in the vertex of the scalp, and associated symptoms include pruritus, pain, and burning (level of evidence: 2b). , It predominately affects young to middle-aged African American males (level of evidence: 2b). , The etiology of FD is unknown. However, it is believed to be a result of an abnormal immune response to Staphylococcus aureus (level of evidence: 4). , Treatment aims to reduce inflammation and pustules. Oral and topical antibiotics and topical and intralesional corticosteroids have shown to be effective in disease remission (level of evidence: 5). Additionally, isotretinoin and red-light photodynamic therapy have been reported to result in disease remission ( Pearl 2.5 ).