Key Words
post-burn contracture, burn scar contracture, elbow contracture, wrist contracture, Z-plasty
Synopsis
Burns continue to be a significant source of morbidity and mortality in low- and middle-income countries. Patients that survive the original injury often develop burn scar contracture because burns across the neck, axilla, elbow, and wrist are forced to heal by secondary intention. The physical examination is the most important part of evaluating a patient with wrist or elbow contracture. The surgeon must identify scar bands causing contracture, inspect soft tissue quality surrounding the joint, and examine donor sites (groin, back, thighs, etc.) for possible grafts and/or flaps. Local tissue, compared with skin grafts, is preferable for joint resurfacing after contracture release, as it is more resistant to recurrent contracture. Compliance with splinting and post-operative physiotherapy is paramount in preventing recurrent burn scar contracture.
Clinical Problem
According to the World Health Organization, burns account for an estimated 265,000 deaths every year, the majority of which occur in low- and middle-income countries. Those who survive the acute burn injury often suffer significant lifelong morbidity. Burn patients living in remote villages do not have easy access to health care, let alone the specialized resources necessary to acutely treat a burn. Without early burn excision and skin grafting, splinting, and physiotherapy, burn scar contracture is inevitable for patients with deep partial-thickness and full-thickness burns. Although the ultimate solution for preventing burn scar contracture is to eradicate all burns, this is not today’s reality. Flame burns occur commonly because people of all ages are exposed to open flames for cooking, warmth in the home, and prayer. Whereas women and children are more likely to sustain flame or scald burns related to cooking in the home, men are more likely to sustain flame, scald, electrical, or chemical burns in the workplace.
Most cases of post-burn scar contracture present years to decades after the original burn injury. It is common to see teenage patients with burn scar contracture, possibly reflecting the high incidence of burn injuries sustained by children at home; the teenagers are now of working age and desire a functional limb. The patient will present with a gross deformity and limited range of motion about the affected joint. Epilepsy can be associated with post-burn scar contracture because patients can fall into flames and/or scalding liquids during a seizure. More commonly associated conditions include malnutrition and anemia.
Pre-Operative Management
The physical examination is the most critical component of the pre-operative management of a patient with post-burn contracture of the elbow or wrist. The elbow is most commonly contracted in a flexed position, whereas the wrist can be contracted in either a flexed or an extended position. Dorsal hand/wrist burns cause contracture of the wrist in hyperextension, whereas volar hand/wrist burns cause contracture of the wrist in flexion. Examine the involved joint, identify scar bands, assess range of motion, and document the degree of flexion or extension contracture.
Inspect the quality of the soft tissue surrounding the scar bands causing joint contracture to determine whether local tissue can be used for resurfacing the joint after contracture release. Also assess the patient’s groin, thighs, back, chest, and abdomen, because these areas may be necessary donor sites for skin grafts and/or flaps. Examine joints proximal and distal to the involved joint because patients with elbow joint contracture can have concomitant axillary and wrist contractures, and digit contractures commonly occur with wrist contractures.
Pre-operative testing needs are minimal for patients undergoing post-burn contracture release. A plain radiograph, if available, to assess the integrity of the affected joint can help the surgeon plan appropriately for surgery. The presence of growth abnormalities from prolonged joint contracture, heterotopic ossification, and so on, can result in marked range-of-motion restrictions that will not be corrected by soft tissue scar release alone. A hemoglobin concentration can be useful if an extensive surgery is planned due to the prevalence of associated anemia in low- and middle-income countries. The upcoming surgery can also be used as a time to screen patients for blood-borne infectious disease such as hepatitis B, hepatitis C, and HIV/AIDS because many people do not have routine access to health care/screenings.
Surgery should not be delayed in children because prolonged joint contracture can restrict growth of the joint and surrounding long bones, causing significant functional impairment. Additionally, the social stigmata of burn scar contracture can have a lifelong psychological impact on young patients. If no other more pressing medical or surgical issues exist, release of the joint near the time of presentation can help the patient to develop more normally and to reintegrate into society in a timely fashion.
Supplies necessary for surgery include surgical instruments, suture, soft dressings, and splinting materials. Only 5 surgical instruments are critical for this case: a scalpel with #10 or #15 surgical blade, a forceps (preferably Adson), skin hooks (single or double), dissecting scissors (Littler or tenotomy), and a needle holder. A monopolar or bipolar electrosurgery unit is necessary to achieve hemostasis. If one of these units is not available, a handheld electrocautery device can be used instead. A tourniquet, if available, can be helpful for extremity surgery because it facilitates safe dissection by creating a bloodless field, and minimizes overall blood loss during the operation. A dermatome is useful if the case requires a split-thickness skin graft, but it is not absolutely necessary because a graft can be harvested with a handheld knife. When choosing suture, use what is available. 3-0 or 4-0 absorbable suture can be used to secure deep tissue, and 3-0 or 4-0 chromic gut or plain gut can be used for the skin. Preferentially use absorbable sutures (chromic gut or plain gut) instead of permanent sutures (nylon or silk) when performing elbow/wrist burn scar contracture release in children to avoid the fear and perceived/real pain associated with suture removal in children. Dressings should include emollient gauze and 4×4s.
The splint is arguably the most important part of the operation because failure to splint the patient in the appropriate post-operative position can lead to early recurrence of joint contracture. To fashion a proper splint, the surgeon will need plaster or fiberglass splint material and cotton cast padding. It is critical to use some form of cast padding to prevent pressure wounds from an ill-fitting splint.
The choice of general anesthesia versus local anesthesia, with or without sedation, is largely determined by the patient’s age and the extent of surgery that is planned. If the patient has a neck contracture, release the neck contracture under local anesthesia before inducing general anesthesia or giving any sedatives. It is extremely difficult to intubate a patient with a neck contracture, so the contracture must be released before intubation. A child should be at least 3 months of age to safely undergo general anesthesia. It is reasonable to test a serum alkaline phosphatase level pre-operatively if the patient will undergo general anesthesia and has had general anesthesia in the past because some inhalation anesthetics can have the side effect of elevated serum alkaline phosphatase levels. Several local anesthetics are acceptable for joint contracture release, including lidocaine, with or without epinephrine, and bupivacaine, with or without epinephrine. Bupivacaine is less preferable due to its increased cardiotoxicity compared with lidocaine and its unknown effects in children under the age of 12. Remember the following cumulative safe doses for the aforementioned local anesthetics:
Lidocaine (0.5% or 1%) with 1 : 200,000 epinephrine—7 mg/kg
Lidocaine (0.5% or 1%) without epinephrine—4 mg/kg
Surgery
During the pre-operative physical examination, prominent scar bands causing elbow or wrist contracture are identified. Additionally, the quality of soft tissue surrounding the joint should be assessed. One should be fully aware of critical structures that may be injured during scar contracture release.
At the level of the elbow, there are several critical structures that may be closely adhered to the overlying scar. The brachial artery and median nerve lie just underneath the lacertus fibrosus. The biceps tendon, critical for active elbow flexion, may become the limiting structure preventing further elbow extension. This should not be transected. At the level of the wrist, critical volar structures include the median nerve and radial nerve, which are fairly superficial. The ulnar artery and ulnar nerve lie protected underneath the flexor carpi ulnaris tendon, but they are still at risk in deep burn contractures.
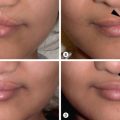
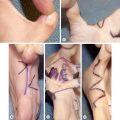
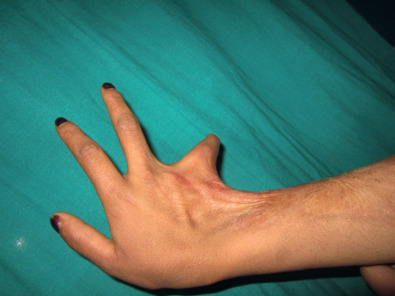
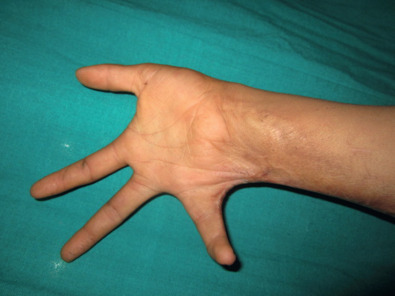
The patient in Figs. 4.7.1 and 4.7.2 has a post-burn contracture of the right hand and wrist that is causing ulnar deviation of the wrist and hyperabduction of the ulnar-most digit. The scar band along the ulnar aspect of the wrist and hand is responsible for this contracture. The remaining skin of the dorsal and volar hand and wrist is soft and mobile. This indicates that local tissue rearrangement in the form of several Z-plasties is the preferred method for contracture release and soft tissue coverage. The four fundamental functions of a Z-plasty are to lengthen a scar, to break up a straight line, to move tissues from one area to another, and to obliterate or create a web or cleft ( Table 4.7.1 ). Local flaps should be utilized as much as possible because they have a lower incidence of recurrent contracture compared with skin grafts and do not require an additional donor site.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree