7 Ectropion
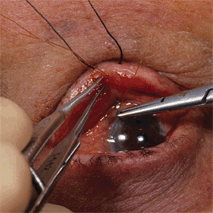
Ectropion is a condition commonly encountered in clinical practice. The pathogenesis of ectropion varies. Frueh and Schoengarth (1982), in an excellent paper, succinctly summarized the evaluation and treatment of the six elements of pathology that may be present in an ectropic eyelid. These factors include horizontal lid laxity, medial canthal tendon laxity, punctal malposition, vertical tightness of the skin, orbicularis paresis secondary to seventh nerve palsy, and lower eyelid retractors disinsertion.
The presence of each factor is determined by clinical examination. One or more of these components may be present in an ectropic eyelid. Proper recognition of the underlying anatomic defect will enable the surgeon to select the appropriate surgical procedure for correction. There are many procedures described for the treatment of each of these eyelid malpositions. In this chapter, one technique is recommended for each of the conditions.
HORIZONTAL LID LAXITY
Horizontal lid laxity is most likely a result of stretching of the lateral and medial canthal tendons, rather than actual elongation of the tarsal plate. This produces a redundancy in the lid tissues, causing the lid margin to fall away from the globe. Horizontal lid laxity can be corrected surgically by several procedures. One popular method is full-thickness excision of a wedge of eyelid tissue and closing the defect primarily. One disadvantage of this method of horizontal lid shortening is that it often leads to lateral canthal deformities, such as blunting of the lateral canthal angle. Additionally, a block resection technique often exaggerates the laxity of the medial and lateral canthal tendon and may produce a horizontally narrowed palpebral fissure. More importantly, surgical correction is not aimed at the underlying defect, namely, stretching of the lateral canthal tendon.
In correcting this element of lid malposition, the lateral tarsal strip procedure advocated by Anderson (1979) is preferred. In this technique, the eyelid is shortened at the lateral canthal end of the lid. The advantages of this technique are that (a) surgery is directed at correcting the anatomic defect, (b) there are no marginal lid sutures, (c) the danger of lid notching or misdirected lashes irritating the cornea is avoided, (d) canthal malposition and lid shortening may be corrected simultaneously, (e) the procedure can be performed quickly, and (f) the almond-shaped canthal angle is preserved.
Procedure: lateral tarsal strip
Lidocaine 2% with 1:100,000 epinephrine is injected into the lateral canthal region with a 30-gauge needle. A small amount of anesthetic is also delivered to the periosteum of the lateral orbital rim and the temporal inferior fornix.
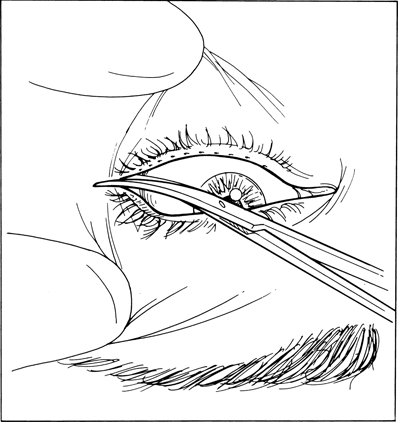
Figure 7-1. Surgeon’s view from the head of the operating table. The procedure is being performed on the left lower eyelid. A lateral canthotomy is made with a Stevens scissors until the lateral orbital rim is exposed.
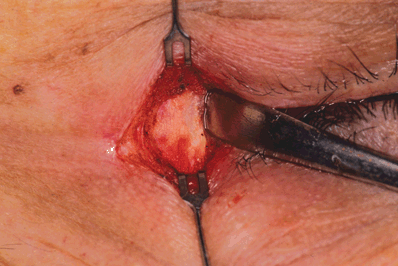
Figure 7-2. The tip of the Freer periosteal elevator is inside the bony rim. The periosteum is exposed. One should avoid cutting into the periosteum, as it will serve as an anchoring structure for the lid later on.
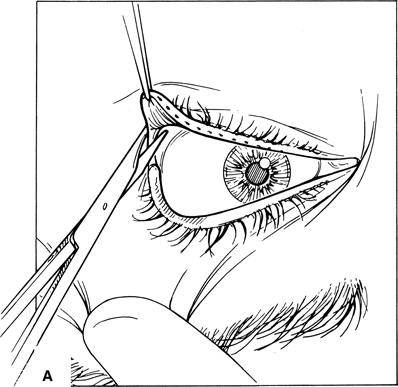
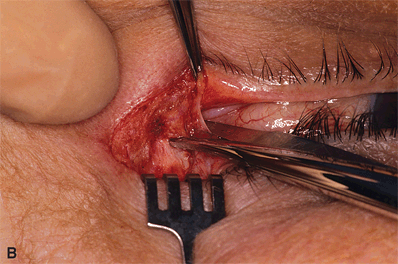
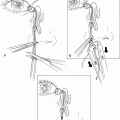
Figure 7-3A and B. An inferior cantholysis is performed by incising the attachment of the inferior crus of the lateral canthal tendon from the lateral orbital rim. Once the inferior crus of the lateral canthal tendon is severed, the entire eyelid becomes mobile. Occasionally, the temporal pocket of the preaponeurotic fat pad may prolapse through this incision. The prolapsing fat pad can be cauterized with a bipolar cautery.
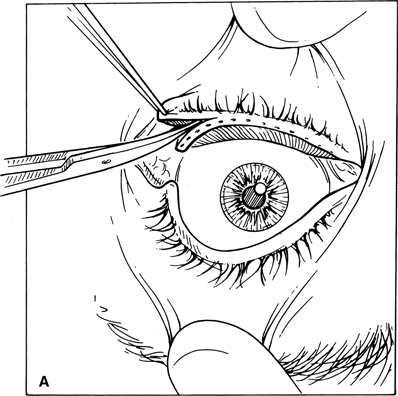
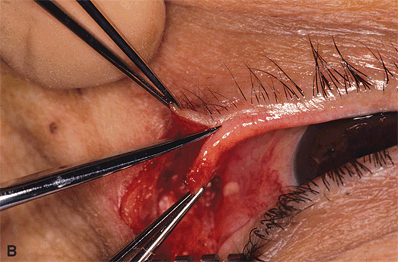
Figure 7-4A and B. With a straight scissors, the eyelid is separated horizontally at the gray line into anterior and posterior lamellae. Incision should be made in the gray line, without cutting into the tarsal plate. At times, the gray line may be indistinct owing to erythema from chronic irritation. One way to identify this landmark is to gently pinch on the lid margin with a nontoothed forceps to look for secretions from the meibomian gland openings. The gray line is located immediately anterior to the secretions. The length of incision along the gray line depends on the amount of lid shortening needed.
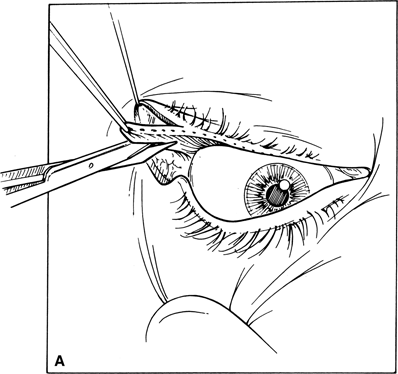
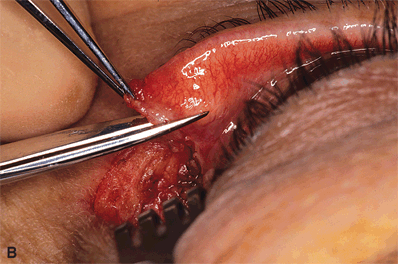
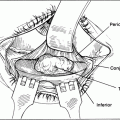
Figure 7-5A and B. A horizontal incision, equal in length to the amount of lid splitting, is made with a scissors at the inferior margin of the tarsal plate. This maneuver severs the conjunctiva and lower eyelid retractors from the tarsal plate, thereby creating a 4- to 4.5-mm wide strip of tarsus.
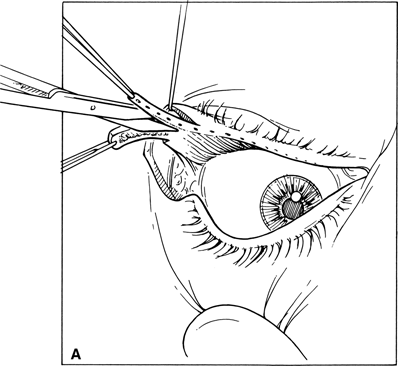
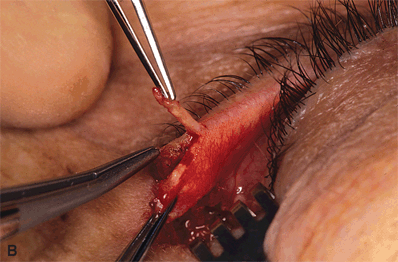
Figure 7-6A and B. The mucosal lining at the superior margin of the tarsal plate is then trimmed off with a straight scissors. One should avoid excising any tarsal substance. While the tarsal plate is stabilized by a tissue forceps over a metal plate, a size 15 Bard-Parker blade is used to scrape the palpebral conjunctiva off the tarsus. The tarsus must be denuded of conjunctiva to avoid epithelial inclusion cyst formation in the area of the new lateral canthus.
The tarsal plate is grasped with a tissue forceps and pulled with sufficient tension in a lateral direction to place the lower punctum slightly lateral to the upper punctum.
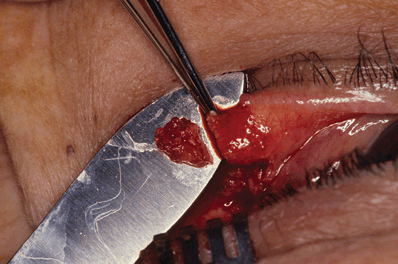
Figure 7-7. The amount of redundant lid tissue is determined by draping the tarsal plate over the lateral orbital rim. The excessive tissue is excised with a scalpel blade. A strip of tarsus, free of any epithelial lining, is thus fashioned.
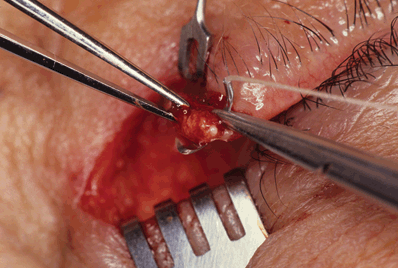
Figure 7-8. The tarsal strip is sutured to the periosteum on the inner aspect of the lateral orbital wall with a double-armed 5–0 Mersilene suture on a spatula needle. The needle is first passed full-thickness through the superior pole of the tarsal strip. A firm bite, at least 1.5 to 2 mm from the tarsal edge, should be taken; this avoids the potential problem of suture “cheese-wiring” through the tarsal substance.
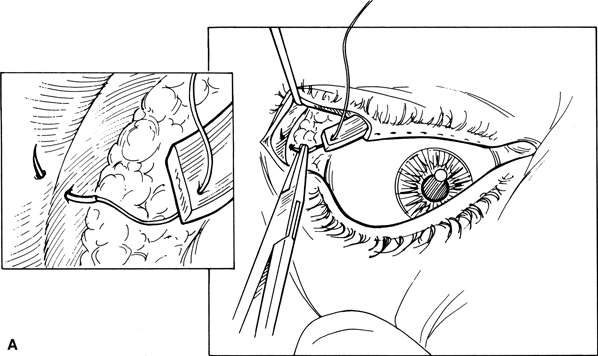
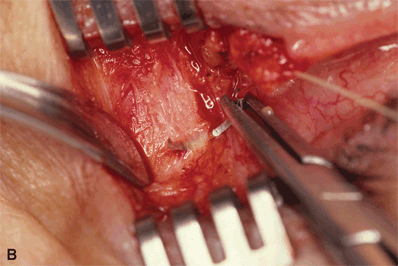
Figure 7-9A and B. The needle then engages the periosteum immediately inside the lateral orbital wall and exits at the anterior surface of the rim to prevent anterior displacement of the canthus. Another suture is passed through the inferior pole of the tarsal strip and engages the periosteum in the same fashion. When correcting lid laxity and canthal malposition in an anophthalmic socket, an additional suture may be placed to augment lid support of the prosthesis. Larger needles are difficult to maneuver at the tight lateral orbital rim region, and needles with a smaller curvature may bend or break on attempted passage through the periosteum. A slight overcorrection in both tightness and elevation at the lateral canthus should be achieved at surgery to allow for slight stretching of tissue in the early postoperative period.
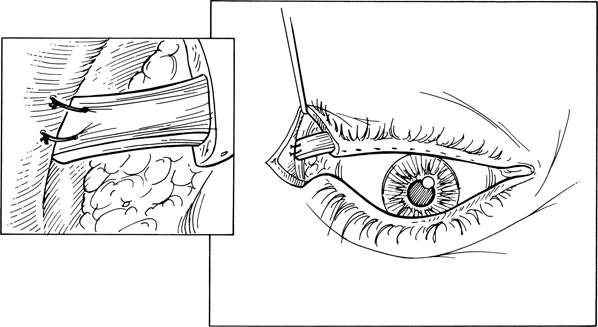
Figure 7-10. After securing the tarsal strip to the orbital rim, a wedge of anterior lamella, including the eyelash follicles, is excised.
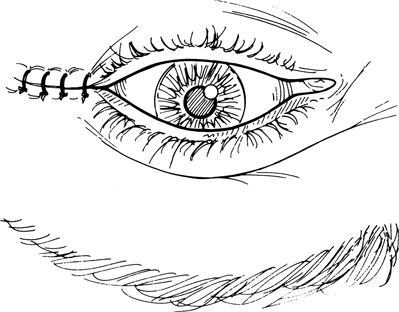
Figure 7-11. The lateral canthotomy incision is closed with 6–0 nylon sutures in an interrupted fashion. The skin sutures are removed in 1 week.
Medial canthal tendon laxity is detected by observing the lateral displacement of the lower punctum with lateral traction on the nasal eyelid. When the lower punctum is no longer aligned vertically with the upper punctum and can be displaced to the nasal limbus when the eye is in primary position, the medial canthal tendon should be repaired. It is unusual to find medial canthal tendon laxity alone, without concomitant lateral canthal laxity. The medial canthal laxity should be corrected first, before proceeding with the horizontal-shortening procedure. The aim of medial canthal tendon plication is to restore the anatomic position of the inferior punctum, so that it is in apposition with the globe and tear lake. The technique involves the exposure of the tendon, anchoring the lid nasally and posteriorly and protecting the inferior canaliculus.
Procedure: medial canthal tendon plication
A curved, vertical incision is made over the medial canthal tendon and continued inferiorly to the medial lid margin, about 3 mm below the punctum.
A Bowman probe is placed in the lower canaliculus to identify and protect the structure throughout the operation. Blunt dissection is carried through the orbicularis muscle fibers with a Freer periosteal elevator to expose the medial canthal tendon and the nasal-most end of the tarsus beneath the punctum.
A double-armed 4–0 Polydek suture on an ME-2 half-circle needle is used.
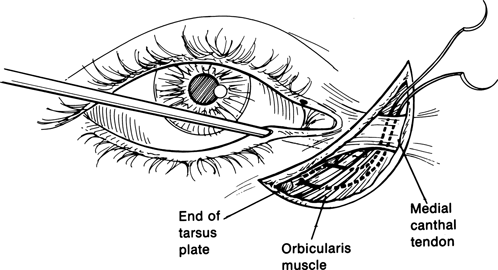
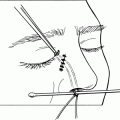
Figure 7-12. The suture passes through the nasal-most end of the tarsal plate, tunnels beneath the orbicularis muscle, and exits at the superior margin of the medial canthal tendon insertion. The other arm of the suture is passed parallel to the first in the same fashion. While passing the needle through the orbicularis, it is important to always keep the needle anterior to the Bowman probe. Passing the needle behind the Bowman probe will incarcerate the canaliculus and compromise lacrimal drainage when the sutures are tied. Care should also be taken to avoid injuring the canaliculus. The two arms of the sutures are tied with sufficient tension to bring the lower punctum to a point just slightly lateral to the superior punctum. Do not tie too tightly, because this will bunch up the inferior canaliculus and displace the punctum away from the tear lake.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree