| Vertical puncta |
| Punctal eversion or ectropion |
| Epiphora and foreign body sensation secondary to ectropion |
| Lower eyelid snap back test |
| Lower eyelid distraction test |
| Finger test to manually tighten eyelid – look at puncta for inversion |
| Orbicularis tone |
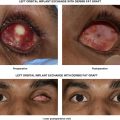
| Assess for anterior lamellar shortage to determine need for skin graft |
| Prior eyelid, facial surgery or trauma |
| Assess for co-existent punctal stenosis |
| Assess for co-existent lacrimal duct obstruction |
Introduction
Punctal eversion is often the first sign of ectropion. Normally, the punctum rests apposed to the globe and with slight inversion of the medial eyelid. Under slit lamp examination, the punctum is normally not visible. With relaxation and attenuation of the lower eyelid retractors, punctal eversion begins. If the punctum becomes vertical or everted, by definition, punctal ectropion is present.
Symptoms occur as the punctum loses its apposition to the ocular surface and tear film. Epiphora begins and worsens as the punctum continues to evert. If eversion worsens, eyelid imbrication may occur with blinking as the upper eyelid closes internally to the lower eyelid. This can cause further irritation to the ectropic lower eyelid and irritation to the tarsal conjunctiva, resulting in discomfort, foreign body sensation, and redness.
Often co-existent with punctal eversion is punctal stenosis. With the punctum not in contact with the tear film, there is no flow of tears and the punctum may become stenotic. Punctoplasty may be necessary to allow tears to drain, in addition to punctal ectropion repair ( Chapter 63 ).
Repair of the ectropic medial eyelid margin alone is often successful in alleviating symptoms. However, also frequently present is horizontal eyelid laxity, which can be addressed simultaneously with an eyelid-shortening procedure or canthopexy. Additionally, canalicular irrigation should be performed to rule out lacrimal outflow obstruction, as this may occasionally be present.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree