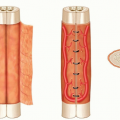
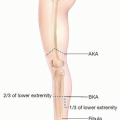
Drainage of Abscesses of Lower Leg and Foot
Michael C. Holland
Scott L. Hansen
DEFINITION
Infections of the foot, ankle, and lower leg range in severity from minor local cellulitis to rapidly progressive necrotizing fasciitis.
Abscesses are a result of infection leading to inflammation and cell death, whereby a cavity is created that is filled with a mixture of bacteria, inflammatory cells, and necrotic tissue.
Painful areas of fluctuance can be identified on physical exam and are most commonly surrounded by signs of inflammation (redness, warmth, pain, and swelling) but may also be found in isolation.
Abscesses of the lower extremity and foot are frequently the result of trauma creating a break in the skin’s natural barrier, allowing for colonizing or environmental pathogens to proliferate in the skin and deeper subcutaneous tissues.
ANATOMY
The lower leg, ankle, and foot are comprised of 28 bones.
Soft tissues include the overlying skin and subcutaneous tissue as well as muscles that are divided into anatomically distinct compartments in both the lower leg as well as the foot.
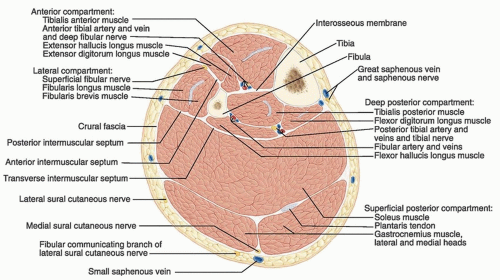
The four compartments of the lower leg include the anterior, lateral, superficial posterior, and deep posterior divided by fascia.
The nine compartments of the foot include the calcaneal —communicating with the deep posterior compartment of the leg, superficial, medial, lateral, adductor, and four interosseous.
The primary neurovascular structures include the anterior tibial, peroneal, and posterior tibial arteries and paired veins; superficial peroneal, deep peroneal (fibular), tibial, saphenous, and sural nerves; and greater and lesser saphenous veins in the superficial tissues (FIG 1).
PATIENT HISTORY AND PHYSICAL FINDINGS
The patient’s initial complaint is typically of pain and swelling at the site of infection. They may also notice changes in skin color and drainage of fluid. There may be a history of antecedent trauma.
Systemic symptoms such as fevers, chills, malaise may not be present early in the disease.
Past medical history of diabetes mellitus, vascular disease, immunodeficiency, injection drug use prior fracture, and prior surgery may predispose to infection and abscess formation.
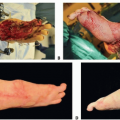
Physical exam may reveal erythema, swelling, tenderness, warmth, fluctuance, visible drainage, and eschar. Many times, erythema and tenderness will be the only physical exam findings, so a high index of suspicion for underlying fluid collection is necessary.
IMAGING
Despite its inability to well characterize fluid collections, standard multiple view radiographs are the first initial test to identify any bony injury or radiopaque foreign bodies as well as gas from anaerobic bacteria. Subtle soft tissue changes may also be demonstrated but are harder to appreciate by the untrained examiner.
Ultrasonography may show cobble stoning of the subcutaneous tissues, which is indicative of edema. Discrete, hypoechoic fluid collections may also be identified.
When multiple abscesses are suspected or ultrasound findings are equivocal, CT with IV contrast of the lower extremity can be extremely valuable.
MRI is similar to CT in its ability to diagnose soft tissue infections; however, its use is limited by cost and time required to obtain the study.
DIFFERENTIAL DIAGNOSIS
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree