Many dermatologic conditions, inflammatory, immunologic, infectious, or neoplastic, can also occur in the oral mucosa, with essentially similar clinicopathologic features. Occasionally, the mouth is the sole manifestation of a dermatologic condition as in the case with lichen planus and mucous membrane pemphigoid. There are also common conditions that are unique to the oral mucosa, such as recurrent aphthous stomatitis (canker sores) and geographic tongue. In this chapter, the reader will be introduced to the clinical characteristics, differential diagnosis, and management of common oral conditions.
With the exception of the posterior one-third of the tongue, which is of endodermal origin, the epithelium that lines the oral mucosa derives mostly from ectoderm. In contrast to the skin, the oral epithelium exhibits different patterns of keratinization. For example:
The masticatory mucosa (hard palate, gingiva, and alveolar mucosa) has keratinized or parakeratinized (retained nuclei in the stratum corneum) squamous epithelium.
The tongue has parakeratinized, nonkeratinized, and specialized epithelia (papillae).
The buccal mucosa and vestibule have nonkeratinized stratified or parakeratinized squamous epithelia, respectively.
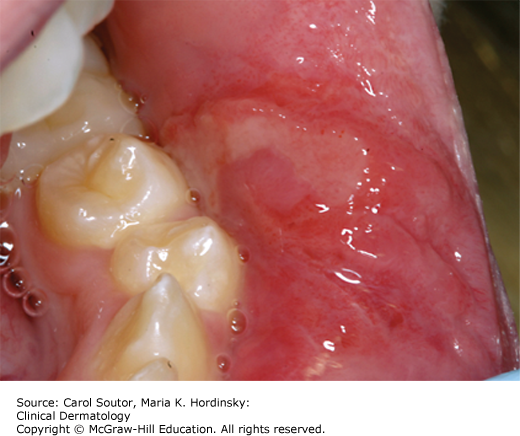
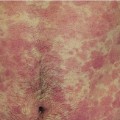
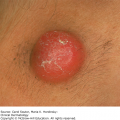
The supporting connective tissue is of ectomesenchymal origin. Adnexal elements are not present in the connective tissue of the oral mucosa, with the exception of sebaceous glands, known as Fordyce granules/spots (Figure 38-1), which are present in 70% to 90% of individuals. However, the mouth has 800 to 1000 lobules of minor salivary glands, with the exception of the gingiva and the anterior aspect of the hard palate.
Clinically, oral lesions can be (1) ulcerated, (2) vesiculobullous, (3) maculopapular, (4) exophytic, papillary, or fungating, (5) nodular or polypoid, and (6) pigmented. Special attention should be given to lesions that are white (leukoplakic), or red (erythroplakic) patches or a mixture of the two (erythroleukoplakic) and lesions that are gray, black, or brown, as these lesions may be malignant or premalignant.
Oral ulcers have various etiologies, which include trauma, immunologic diseases, infections (bacterial, deep fungal, or viral), and neoplasms (squamous cell carcinoma, lymphoma, malignant salivary gland tumors, etc). They are generally painful, except for squamous cell carcinoma, which may be asymptomatic, when it presents as an ulcer.
Traumatic ulcers are usually the result of physical injury (eg, accidental biting during mastication, contact with sharp or broken cusps of teeth, and sharp food), and less often, thermal or chemical burn (eg, chemicals used during dental or surgical procedures, aspirin, alcohol, peroxide, and other acidic substances). Rarely, electrical injury can occur, especially in very young children who accidentally chew on an electrical wire.
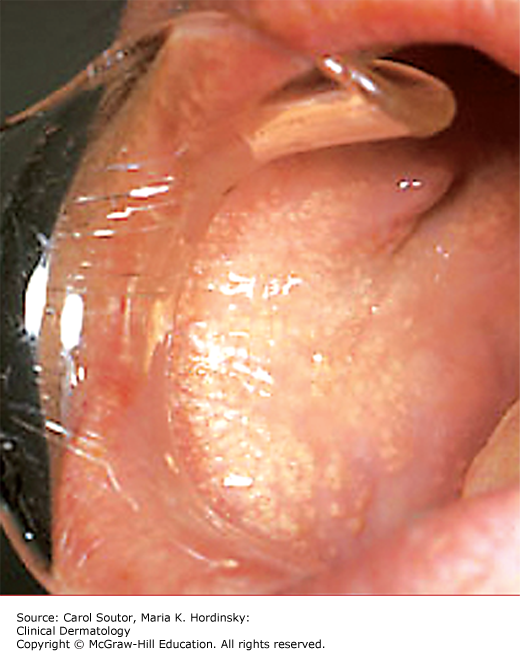
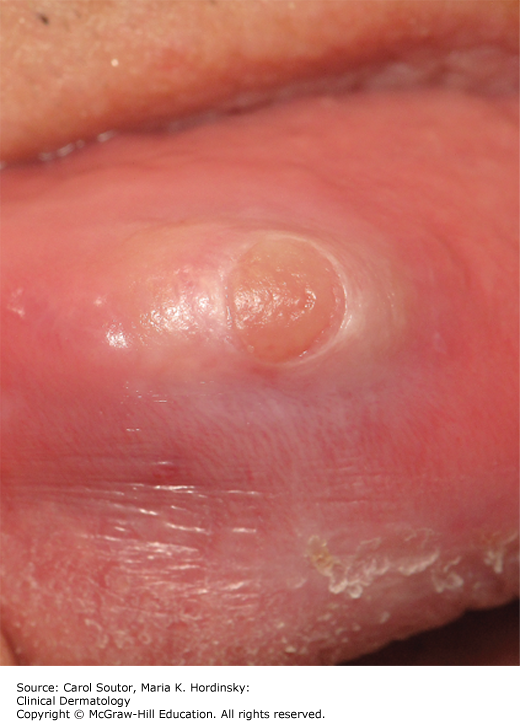
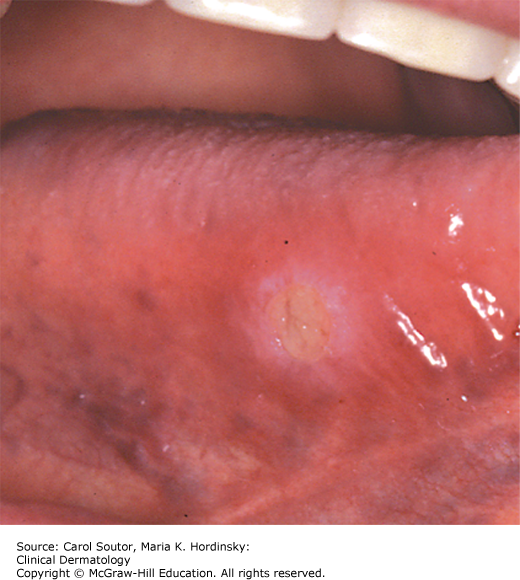
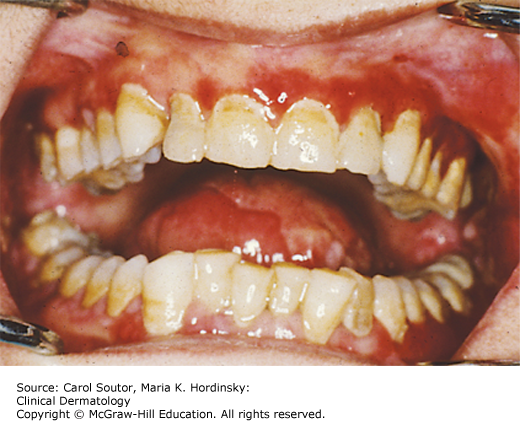
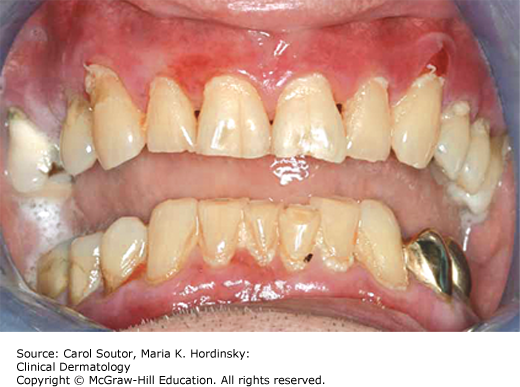
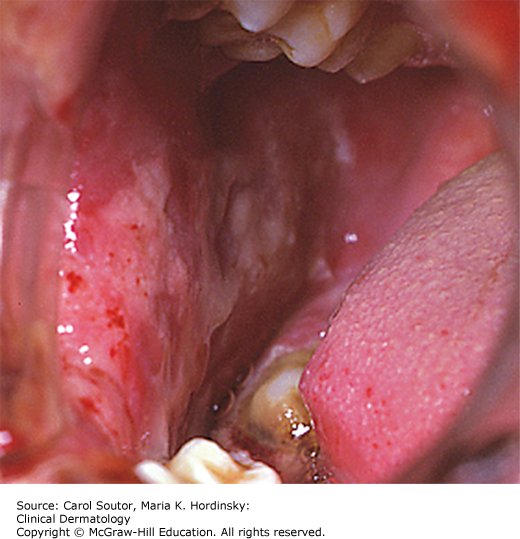
Traumatic ulcers frequently affect the tongue, lips, and buccal mucosa (Figures 38-2, 38-3, 38-4) and in cases of vigorous tooth brushing, small and often multiple ulcerations can occur on the gingiva. In general, traumatic ulcers present as round, ovoid or irregular, erythematous lesions usually covered by a pseudomembrane and surrounded by a white border that represents reactive epithelial regeneration.
Traumatic ulcers heal after removal of the cause and depending on the size and the location; they usually heal within 1 to 2 weeks. Over the counter topical dyclonine hydrochloride, hydroxypropyl cellulose, lidocaine, or benzocaine can relieve the pain associated with ulcerations. Treatment with topical corticosteroids (gels are preferred over creams and ointments since they adhere better to the oral soft tissues) can be used in some instances. Chronic large ulcers may require topical steroids. Ulcers of the tongue may take more time to resolve due to the unique nature and composition of the tongue, which is, a movable muscle. Ulcerated lesions that last longer than 3 weeks without an obvious etiology should raise a clinician’s suspicion of neoplasia, and these lesions should be biopsied with incisional or excisional techniques.
Recurrent aphthous stomatitis (canker sores) is one of the most common oral mucosal lesions presenting with one or multiple ulcers NOT preceded by vesicles or bullae.1 RAS affects between 5% and 60% (mean 20%) of people with a predilection for females, caucasians, and children of higher socioeconomic status.
Many predisposing factors have been implicated with the development of RAS. In some patients there is genetic predisposition with certain HLA types. Hypersensitivity to certain foods such as citrus fruits, chocolate, coffee, gluten, nuts, strawberries, tomatoes, medications (eg, -nonsteroidal anti-inflammatory drugs [NSAIDs], and beta blockers), sodium lauryl sulfate in toothpastes, smoking cessation, stress, trauma, infectious agents (eg, Helicobacter pylori, herpes simplex, and streptococci), and female hormonal changes have been associated with development of RAS.
Systemic diseases presenting with oral ulcers akin to RAS include nutritional deficiencies (iron, folate, and vitamin B complex), IgA deficiency, Behçet’s disease, Sweet’s syndrome (acute neutrophilic dermatosis), PFAPA syndrome (periodic fever, aphthae, pharyngitis, and cervical adenitis), inflammatory bowel disease, reactive arthritis (Reiter syndrome, cyclic neutropenia, and AIDS).
RAS ulcers are mostly round or ovoid and generally painful. They are usually covered by a pseudomembrane and surrounded by an erythematous halo. There are three types of aphthae, minor, major, and herpetiform.
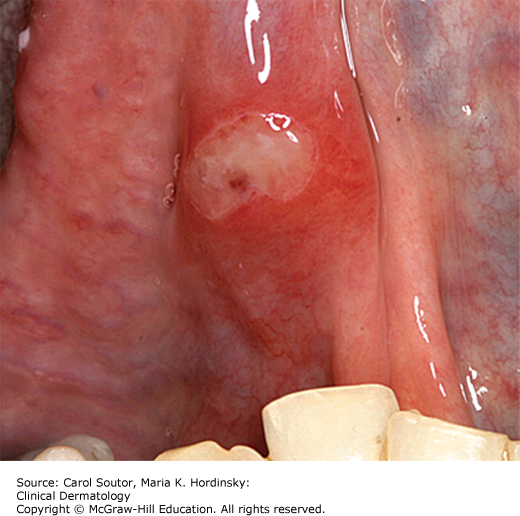
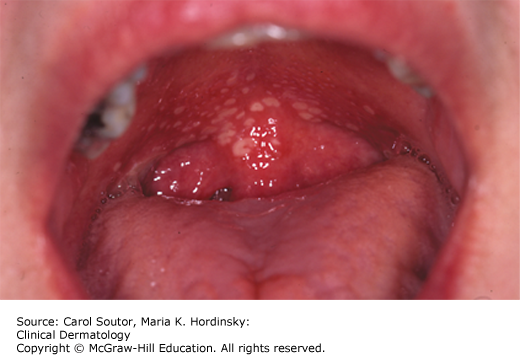
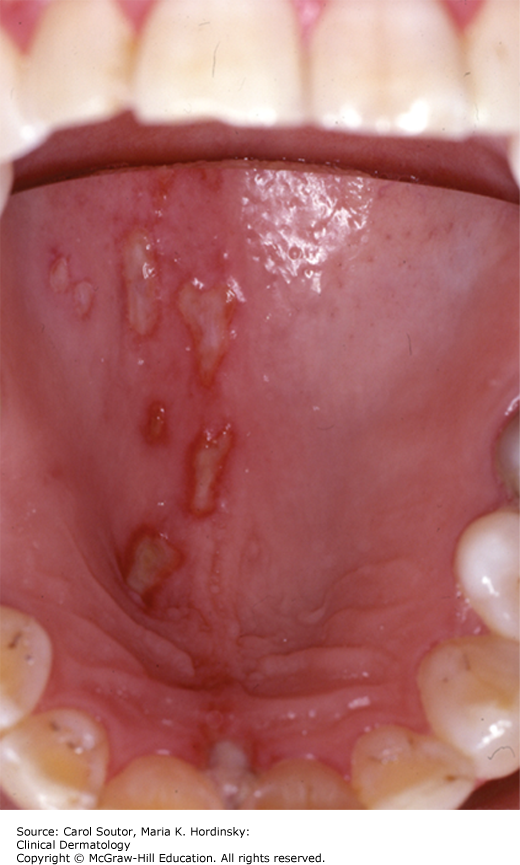
Minor aphthae (Figure 38-5) are the most common form of RAS and typically present with recurring episodes of 1 to 5 small ulcers, less than 1 cm in greatest diameter. They predominantly affect the nonmasticatory mucosa and are usually seen in the anterior part of the mouth. They last 7 to 14 days, if left untreated.
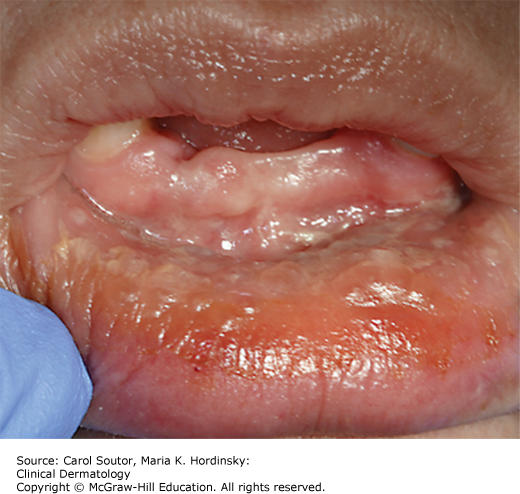
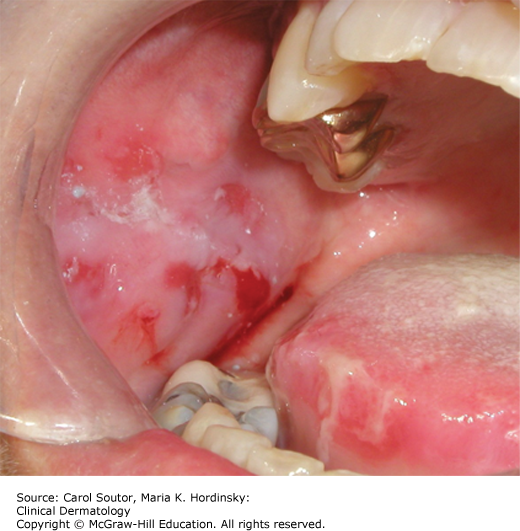
Major aphthae (Figure 38-6) are larger, deeper, last longer (2 to 6 weeks) and are very painful. Major aphthae are most frequently seen on the lips and the posterior oropharynx.
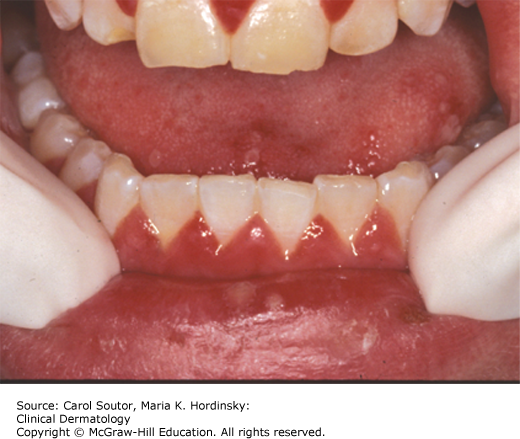
Herpetiform RAS (Figure 38-7) is characterized by as many as 50 to 100 small ulcers and may clinically resemble ulcers of primary herpes simplex, thus the confusing term “herpetiform.” Recurrences are usually closely spaced and lesions, although favoring the nonmasticatory mucosa, can be seen throughout the mouth.
The treatment for RAS depends on the extent and degree of pain of the lesions. Some patients can tolerate the lesions and associated pain, but other patients have difficulty eating or even functioning during episodes. Over the counter topical anesthetics or protective bioadhesive products such as Orajel, Orabase, and Zilactin may be of some benefit. Fluocinonide or betamethasone dipropionate 0.05% gels can be used topically 2 to 3 times a day. They should be applied to early lesions at the onset of prodromal pain and tingling. Steroid solutions, such as dexamethasone 0.5 mg/5 mL, and prednisolone or betamethasone syrups may be used in patients who have widespread lesions. In hard to reach areas, such as tonsillar pillars, beclomethasone dipropionate aerosol spray can be used as an alternative. Systemic steroids can be used in patients with very painful major aphthae and in herpetiform lesions. Occasionally, systemic steroids are used in conjunction with topical steroids. RAS that does not respond to steroids should be referred to specialists who may prescribe dapsone, tacrolimus, thalidomide, tetracycline, levamisole, MAO inhibitors, and other medications as alternatives to steroids. Cauterization with silver nitrate and laser ablation are not recommended. Besides using medications to treat RAS, the clinician should review the eating habits of patients, which may be contributing to RAS. If indicated, an evaluation should be done for systemic diseases, which could be related to RAS.
Vesiculobullous lesions of the oral mucosa may be due to trauma, allergic reactions (Figure 38-8), infections (herpes simplex or zoster), or immune-mediated disease (pemphigus vulgaris and mucous membrane pemphigoid). Intact vesicles are rarely identified and generally vesiculobullous processes manifest as erosions and ulcerations as most blisters rupture spontaneously. Therefore, a clinician should specifically ask about the presence or absence of oral blisters when evaluating a patient with oral erosions and ulcerations.
Oral HSV is generally due to HSV type I.2 In rare cases, HSV type II may be the cause due to orogenital sexual contact. Primary infection by herpes simplex presents as gingivostomatitis (Figure 38-9). Direct contact with an asymptomatic individual shedding the virus in saliva, or with a person with recurrent infection such as herpes labialis are modes of transmission. The vast majority of individuals without antibodies against HSV type I, when infected, do not have clinical symptoms or signs. After the primary infection, the virus is transported to sensory or autonomic ganglia where it remains in a latent state.
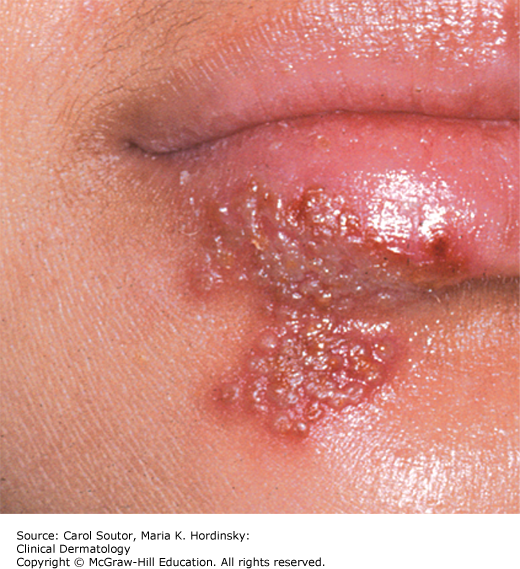
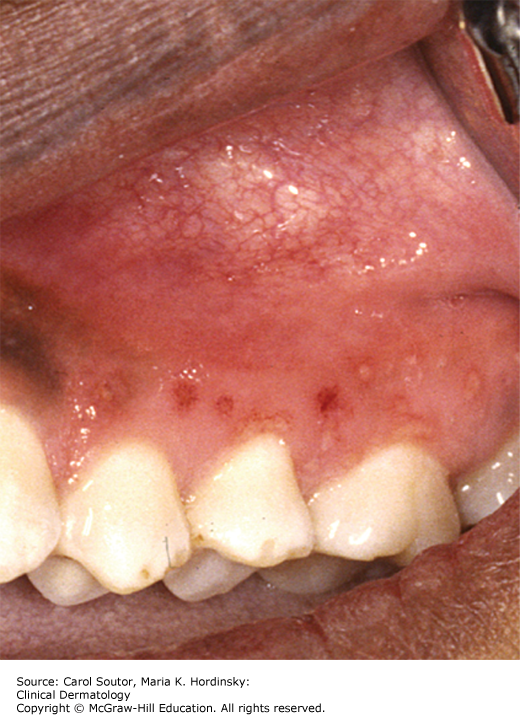
Reactivation of the virus is responsible for recurrent disease which usually affects the lips (herpes labialis or cold sore) (Figure 38-10) or, intra-orally on the hard palate or gingiva (Figure 38-11). Perioral lesions may also occur on the skin of the nose, cheek, or chin. Triggering factors include immunosuppression, menstruation, stress, ultraviolet light, and local trauma. Prodromal symptoms (burning, itching, or tingling) occur in many patients.
Primary HSV infection may present as acute gingivostomatitis in children and adolescents with multiple, 1 to 2 mm vesicles that rapidly rupture to form multiple small red, white, or yellow ulcerations throughout the mouth (Figure 38-9). The lips of the patients become crusted with serum and blood, and the gingivae are edematous and erythematous and covered with small ulcers. Patients may also have anterior cervical lymphadenopathy, chills, high fever (103 to 105°F), nausea, and irritability. Self-inoculation to the fingers, eyes, and genitals can occur. Older patients with primary disease may have pharyngotonsillitis. Recurrent herpes labialis presents as coalescing vesicles that rupture and subsequently crust. Without treatment complete healing occurs after 1 to 2 weeks. Intraoral recurrent herpes presents as small shallow and coalescing yellowish-white or erythematous ulcers preceded by vesicles that heal within 1 to 2 weeks.
Reactivation in immunocompromised patients such as HIV-positive3 and transplant patients may lead to a chronic herpetic infection that is persistent and characterized by atypical lesions that can mimic major aphthae or necrotizing stomatitis. In some patients these atypical ulcers harbor also cytomegalovirus co-infection. These patients should be referred to specialists for evaluation to confirm the diagnosis and to infectious disease specialists for management.
Pediatric primary infections can be treated with palliative topical rinsing with 0.5% to 1% dyclonine hydrochloride and if needed with acyclovir suspension during the first 3 symptomatic days in a rinse-and-swallow mode (15 mg/kg or up to the adult dose of 200 mg daily for 5 days).
If needed, oral medications for primary and recurrent herpes simplex can be used. Table 38-1 lists selected treatment options for adolescents and adults. Topical medications are also available (Table 38-2).
| Medication | Brand Name Examples | Selected Dosing Options | Duration (Days) |
|---|---|---|---|
| Acyclovir | Zovirax | Primary: 400 mg 3 times a day | 7-10 |
| Recurrent: 800 mg twice a day | 5 | ||
| Famciclovir | Famvir | Primary: 250 mg 3 times a day | 7-10 |
| Recurrent: 1500 mg one dose | 1 | ||
| Valacyclovir | Valtrex | Primary: 1000 mg twice a day | 7-10 |
| Recurrent: 2000 mg every 12 h | 1 |
Varicella and herpes zoster are caused by the varicella-zoster virus (VZV). Varicella is the primary infection and patients present primarily with cutaneous lesions; however, oral lesions are not uncommon and may precede the skin lesions. Vesicular lesions usually appear on the lips and the palate and in contrast to primary herpes are generally painless. VZV establishes latency in the dorsal spinal ganglia.
Herpes zoster is the reactivation of VZV. The prevalence increases with age and occurs in 10% to 20% of infected individuals. Most affected patients have a single episode. Predisposing factors include stress, immunosuppression, treatment with cytotoxic medications, presence of malignancies, and older age. For head and neck cases, dental manipulation may be the trigger.
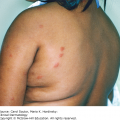
The lesions of herpes zoster can affect the face and oral mucosa unilaterally and follow the path of the involved nerve (Figure 38-12). Since affected nerve endings can cross the midline, a few lesions can be seen on the other side of the midline. Patients present with very small vesicles that rupture and leave behind shallow painful ulcerations. Occasionally if the maxilla is involved, tooth necrosis and in rare cases bone necrosis can occur.
Treatment for herpes zoster should begin as soon as the diagnosis is established. Valacyclovir 1 g 3 times a day for 7 days or famciclovir 500 mg 3 times a day for 7 days or acyclovir 800 mg 5 times a day for 7 days or acyclovir 800 mg 5 times a day for 7 days are the drugs of choice. Analgesics and antiepileptics (gabapentin and carbamazepine) and tricyclic antidepressants can be used for pain relief. Also oral corticosteroids are sometimes prescribed to older, immunocompetent patients (with no contraindications to steroids) to decrease the incidence of postherpetic neuralgia.
Mucous membrane pemphigoid4 and pemphigus vulgaris5 are uncommon immunologic vesiculobullous diseases that can have oral manifestations. MMP (Figure 38-13), also known as cicatricial pemphigoid, generally involves only the mouth which is in contrast to bullous pemphigoid (the most common type of cutaneous pemphigoid) rarely presents with oral manifestations.
In PV (Figure 38-14), oral lesions may be the “first to show and last to go” and oral mucosal involvement is seen in almost all cases. Lesions present as painful erosions or ulcerations preceded by vesicles. If intact vesicles are seen, MMP is more likely the diagnosis. This is because the vesicles in MMP are subepithelial and thus more deeply seated, in contrast to the vesiculobullous process in PV that is intraepithelial. Patients with PV rarely present with intact vesicles. It is important for the clinician to question the patient about a history of vesicles or bullae when multiple shallow ulcerations are identified in the mouth. Also, in patients presenting with PV, but more importantly with MMP, synchronous or metachronous ocular involvement may occur leading to scarring of the conjunctiva.
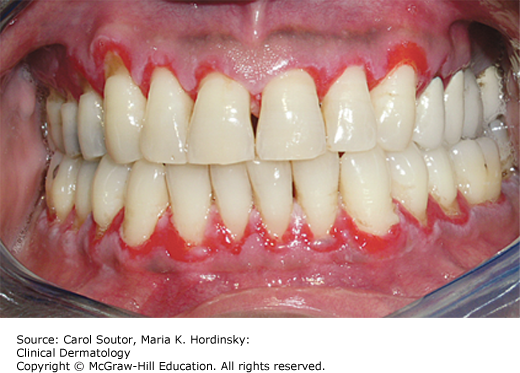
When the gingiva is involved in MMP and PV, the clinical presentation is that of mucosal sloughing and erosions. This is referred to as desquamative gingivitis and diffuse erythematous lesions covering most, if not all of the gingiva can occur (Figure 38-15). Desquamative gingivitis is a clinical descriptive term and not a diagnosis. In order of frequency, the underlying condition can be erosive lichen planus, MMP or pemphigus.6 Patients with oral PV can present occasionally with multiple shallow ulcerations of the free gingiva (Figure 38-16). Such lesions can persist after successful treatment of all other mucocutaneous lesions and achieving resolution is difficult.
In the differential diagnosis of immunologically mediated oral vesiculobullous and ulcerative processes one should include erythema multiforme, hypersensitivity reactions, angina bullosa hemorrhagica, linear IgA disease, and rarely, bullous lichen planus.
Treatment for MMP depends on the severity of lesions and the areas affected. Topical steroids including fluocinonide, betamethasone dipropionate, or clobetasol propionate 0.05% gels may be used for mild disease. For widely distributed lesions, dexamethasone 0.5/5 mL rinse may be prescribed. Secondary candidiasis may develop as a side effect to topical corticosteroid treatment and can be treated with oral antifungal medications. Systemic therapy is typically required and is usually managed by a team approach with clinicians in clinical oral pathology, dermatology, and ophthalmology. These specialists often use systemic treatment with prednisone in more severe cases. Other systemic medications for the treatment of MMP include azathioprine, dapsone, and mycophenolate mofetil. Combination treatment for MMP with tetracycline 1 to 2 g/day and nicotinamide 1 to 2 g/day has been used as alternative to corticosteroids and the other immunosuppressive agents. For patients with gingival manifestations, excellent dental hygiene is important for good results. Also, the fabrication of customized trays by the patient’s dentist as a vehicle for better delivery is recommended.
Treatment for oral lesions of PV is more complicated since the disease is widespread. Systemic treatment should start immediately after the diagnosis is established. Ideally, a patient with pemphigus should be treated by a physician with expertise in immunosuppressive therapy. Combination of systemic corticosteroids and immunosuppressive drugs such as azathioprine is chosen in many cases. Topical steroids may be used for persistent oral lesions.
EM and SJ/TEN present with oral and cutaneous lesions.7 EM usually affects teenagers and young adults and is typically triggered by a herpes simplex infection or it may be caused by medications including antibiotics or anticonvulsants. SJS/TEN is commonly caused by medications and less commonly by infections. Chapter 23 has detailed information about these conditions.
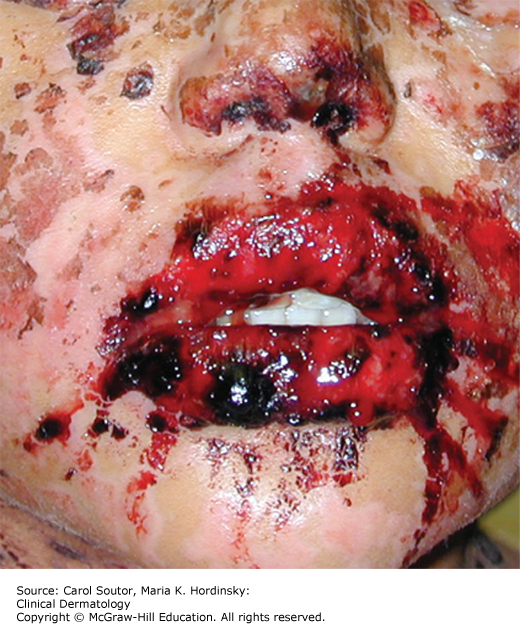
Oral lesions may precede or be concomitant with skin lesions, which present as erythematous papules and macules frequently having a target or targetoid appearance. EM and SJS/TEN have an acute onset and may be accompanied by malaise, fever, headache, and sore throat. In most patients the lesions usually occur in the nonmasticatory mucosa, the anterior part of the mouth with the gingiva, and hard palate being relatively spared. Oral lesions (Figure 38-17) usually start as erythematous patches, with or without vesicle formation, which ulcerate leaving extensive and painful erosions and ulcerations covered by pseudomembrane, as well as areas of necrosis. Many patients present with blood-crusted lips, which is a useful clinical sign (Figure 38-18). Besides oral and cutaneous lesions, patients can have genital, pharyngolaryngeal, esophageal, and bronchial lesions.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree