and Zhou Xiao2
(1)
The Second Xiangya Hospital of Central South University, Changsha, China
(2)
Hunan Cancer Hospital/The Affiliated Cancer Hospital of Xiangya School of Medicine, Central South University, Changsha, China
1 Overview
The lip cancers refer to the cancers occurred in the lip vermilion mucosa (the exposed lip vermilion mucosa when the lips are naturally closed) and the joint mucosa in the corner of the mouth (within the range of 1 cm backward from the oral fissure). The cancers occurred in the inner side of the lip mucosa belong to the category of buccal mucosa carcinoma. The vast majority of cancers occurred in the lip vermilion mucosa are squamous cell carcinomas, and most of them are better differentiated; a small part of lip cancers are the basal cell carcinomas, which are caused due to the fact that the lip skin is invaded, and the adenocarcinoma is rarely seen.
The incidence of lip cancer is 1.8/100,000, accounting for 0.6% of the malignant tumors in the whole body and 9.57% of oral and maxillofacial squamous cell carcinoma. About 90% of lip cancers occur in the middle-aged and elderly people over the age of 40, more than half of them occur in the elderly people over the age of 60, and they occur more in men than women. More than 90% of lip cancers occur in the lower lip and occasionally occur in the upper lip. The lip cancers are more likely to occur in the mucosa of the prolabium at the junction of the middle and outer one third of the lower lip, and it is occasionally observed that the lip cancer occurs in the corner of the mouth. Most of lip cancers are solitary, and they have a slow disease progression and a longer disease course of usually 6 months to more than a year. The early lesions are presented as small herpes, induration, uncured chronic ulceration, or limited thickening and hardening of lip vermilion mucosa; the lesion is slowly increased and extended to the lip lump protruding outwardly or the deeper ulcer with a slightly elevated edge; the patients often have no self-conscious symptom and occasionally have mild pain and a little bleeding. Later on, the lesions are extended to the surrounding mucosa and skins, and the deep muscles are violated, and the cauliflower-like mass with edge eversion or crater-like ulcer is formed; the mass surface is covered with a gray-black eschar; the surface is presented as uneven small nodular shape. After the eschar is removed, the erosive wound and a little bleeding can be observed; the pain often occurs and is gradually aggravated. In the advanced stage, the lesion can be spread to the most part of the lip and even the whole lip, buccal cavity, and mandible, and the salivation, eating disorders, and more severe pain will occur [1, 2].
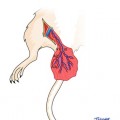
The blood supply of the lip comes, respectively, from the superior and inferior labial arteries and the branch of the facial artery, the labial arteries surround the mouth to form an arterial arch, and, therefore, the lesion in the one side of the lip is supplied with blood by the blood vessel from the middle part and one side of the lip. The sensations in the skin around the lip and at the junction of the skin and mucous membrane are controlled by the branches of the maxillary and mandibular divisions of trigeminal nerve. The movements of the orbicularis oris muscle and the muscle above and under the corner of the mouth are dominated by the branches of the facial nerve.
The lymphatic drainage of the lip has a certain direction; firstly the lymphatic fluid of the lower lip is drained into the lymph nodes in front of the facial blood vessel on the surface of the mandible and the level I lymph nodes and then is drained into level II and III lymph nodes; therefore, the level IV and V lymph node metastases are very rarely seen in the patients with lip cancers. The hematogenous distant organ metastases are rarely seen in the patients with lip cancers [3, 4].
2 Repair Method
2.1 V-Shaped Resection of the Lip
2.1.1 Indications
The patients who have lip benign tumors and small and limited lip cancers with a diameter of less than 2 cm or a resection range of no more than one third of the whole lip, which have not invaded the corner of the mouth, can undergo V-shaped resection in most cases.
2.1.2 The Surgical Procedure
- 1.
The routine disinfection and sterile draping are carried out, and the methylene blue is used to draw out the range of the tissues to be removed. The benign tumors can be removed along the incision line drawn at 2 mm from the margin of the tumor; if the cancer is confirmed, the resection should be performed at 0.5–1 cm from the margin of the cancer.
- 2.
The lip clips or fingers are used to pinch the lips on both sides of the incision to reduce the bleeding. The incision line should be V shaped or W shaped, the surgical knife should be at right angle with the skin on the labial surface, the full-thickness skin incision is made, and the lip artery is ligated.
- 3.
After mass resection, 0–1 silk thread is used to suture the mucous layer and muscular layer, and 5–0 silk thread is used to suture the wound margin of the skin. In order to get good results in the lip shape, at first, a suture in the lip prolabium should be accurately performed. When the suture is performed, if the lip tissue has a greater tension, the assistant incisions can be made in the transitional parts at both sides.
- 4.
The wound is covered with dressing, which is removed after 24 h.
2.1.3 Precautions
- 1.
Keep the wound dry and clean. If there is food or escharosis in wound, the wound can be cleaned and treated with 3% hydrogen peroxide solution or 75% alcohol.
- 2.
When the needle pus or surface infection occurs, it may be appropriate to take out some stitches, and the gromwell oil is smeared onto the local area.
- 3.
The antibiotics are applied for 3–4 days.
- 4.
The stitches are taken out after 5–7 days.
2.2 Lip Resection
2.2.1 Indications
It is applicable to the precancerous lesions of the lip, such as leukoplakia of the lip.
2.2.2 The Surgical Procedure
- 1.
The incision of the whole lip is made along the lip vermilion border.
- 2.
The tissue forceps are used to lift the tissues to perform the stealth separation to the underneath of the inner lip mucosa, and the lesion area is totally removed.
- 3.
The inner lip mucosal tissue is migrated forward to be close to the skin margin, and then the interrupted suture is carried out with silk thread.
2.2.3 Precautions
They are the same as the V-shaped lip resection.
2.3 Cross Lip Flap Transfer
The cross lip flap transfer is also known as Abbe-Estlander operation.
2.3.1 Indications
If the lip cancer involves a range of more than 2 cm, after cancer removal, the defect range reaches up to the half of the transverse diameter of the lip; the patient can be treated with this method (this procedure is applicable to the lesions which are located at the middle and outer one third of the upper and lower lips). The skin flap can be designed into a variety of shapes, such as triangles, rectangles, and squares. It is appropriate that the donor site can be directly closed and sutured. The width of lip flap in the donor site is half of the width of the contralateral lip defect.
2.3.2 Surgical Procedures
If the defect is located in the middle of the lip, an additional incision can also be made firstly in one side of the lower lip adjacent to the corner of the mouth, and the lip flap is transferred to the middle part to repair the defect; then the upper lip tissue adjacent to the corner of the mouth is transferred into the lateral lower lip defect and is sutured (Figs. 5.1 and 5.2). This method not only ensures that there is enough tissue to repair the defect in the middle part of the lower lip but also avoids the transfer of the tissue in the middle part of the upper lip, which has the disadvantage of causing damage to the shape of the upper lip and philtrum. The elongation of the oral fissure should be performed at 3–4 weeks after the lip flap is transferred to achieve bilateral symmetry
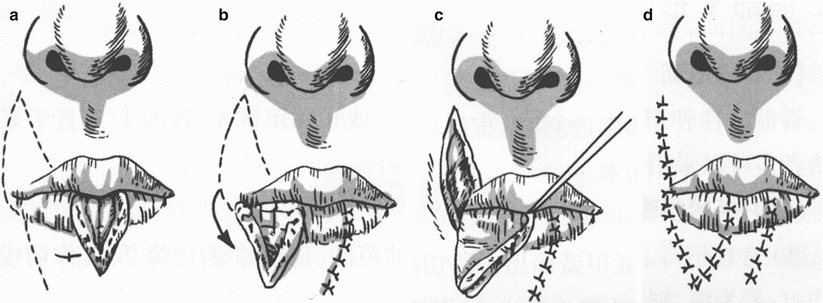
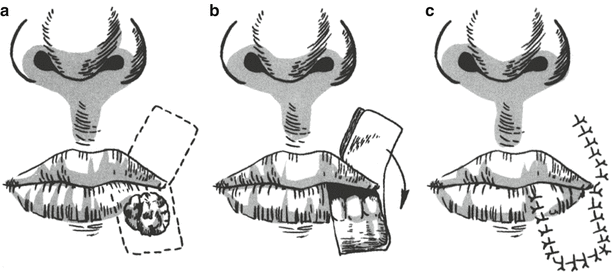

Fig. 5.1
The transfer of cross lip flap to repair the tissue defect in the middle part of the lower lip. (a) The defect and incision design. (b) The lower lip flap is transferred to the middle part and is sutured. (c) The upper lip flap is transferred downward. (d) After suture

Fig. 5.2
The transfer of cross lip flap to repair the tissue defect after tumor resection in the lower lip. (a) Incision design. (b) The lesion in the lower lip was removed, and the upper lip was transferred downward. (c) After suture
2.4 The Nasolabial Flap Combined with the Vermilion (Mucosa) Sliding Flap or Tongue Flap for Defect Repair After Resection of Lower Lip Cancer
2.4.1 Indications
The lip cancer involves a wider range, the defect range after resection can reach from more than three fourths of the transverse diameter of the lip to the whole lip, and the method is applicable for the upper and lower lip defects.
2.4.2 The Anatomy of the Nasolabial Flap
The nasolabial flap has been used for a long term due to the advantages that it is adjacent to the location of the lip and has a similar color and texture as well as a rich blood supply, and its donor site is relatively hidden. After a piece of the skin of 2–3 cm is harvested in this area, the incision can be closed and sutured directly. The nasolabial flap has a rich blood supply, which comes from multi-sources. There is the inner canthus artery in the upper part, the facial artery in the lower part, the superior labial artery in the inner side, and the transverse facial artery in the outer side. The branches of these blood vessels anastomose each other to form a dense vascular network within the skin and subcutaneous area, which has laid a good vascular basis for the nasolabial flap. The pedicle of the nasolabial flap can be designed at one of the sites such as the inner, outer, upper, and lower sites, and the flap can be designed into the random pattern skin flap and the subcutaneous island pedicle flap.
2.4.3 The Surgical Procedure
- 1.
The routine disinfection and sterile draping are carried out.
- 2.
The vermilion tissue is preserved as far as possible on the premise of ensuring adequate safe incisal margin, and the range for skin flap harvesting is marked according to the size of the defect after tumor resection. The medial incision of the nasolabial flap should be anastomosed with the nasolabial fold wrinkle. The skin, subcutaneous tissue, and mimetic muscles are incised open layer by layer according to the marker line to form the nasolabial flap pedicled with the facial artery and vein, and the donor site of nasolabial flap is closed and sutured directly. A tunnel between the donor site and the defect site is made; then the skin flap is passed through the tunnel to repair the defect site; finally the bilateral vermilion sliding flaps and the mucosal sliding flap are used to repair the vermilion defect according to the size of the vermilion defect.
- 3.
If the area of the vermilion defect is larger, the tongue flap with a pedicle in the front part can be designed to repair the vermilion defect. Incise from the tip of the tongue and extend the incision toward the both sides along the margin of the tongue to reach the superficial layer of the tongue muscle, the incision length is consistent with the length of vermilion defect, and then a 1.5 cm of sharp dissection is performed toward the direction of the tongue root along the superficial layer of the tongue muscle to form the tongue flap; the lower margin of the tongue incision is sutured with the wound margin in the pedicle of the skin flap. The pedicle of the tongue flap is preserved, and the pedicle is cut off at 2 weeks after surgery (Fig. 5.3).
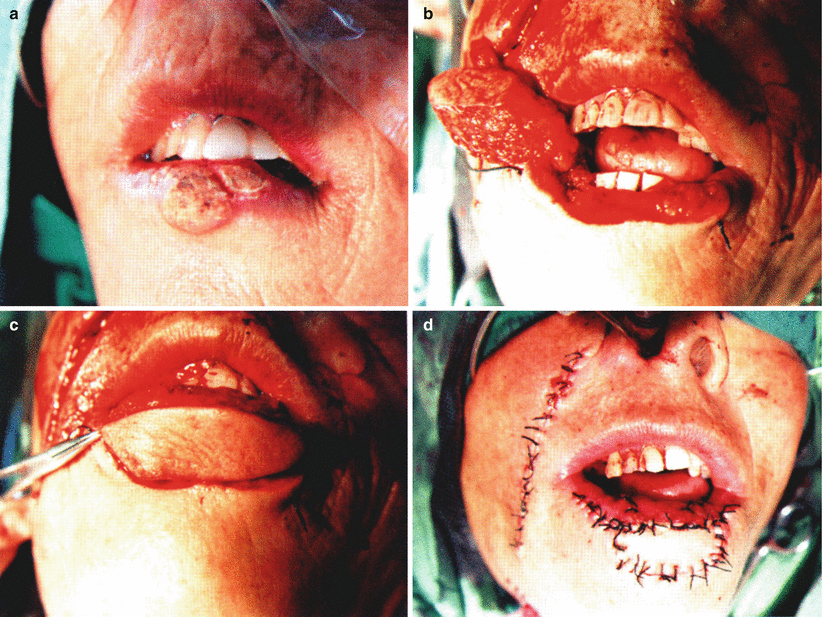
Fig. 5.3
Defect repair after resection of lower lip cancer (the nasolabial flap is passed through the tunnel to repair the lower lip; the lip mucosal sliding flap is used to repair vermilion defect). (a) Preoperative situation, the range of the lower lip cancer is more than the three fourths of the transverse diameter of the lip. (b) The lower lip defect after tumor resection. (c) The nasolabial flap is passed through the tunnel to repair the lower lip defect. (d) The lip mucosal sliding flap is used to repair the vermilion defect
2.5 Elongation of the Oral Fissure
2.5.1 Indications
The microstomia deformity occurs due to the fact that the normal shape of the corner of the mouth is damaged by the lip surgery. At this time, the elongation of the oral fissure can be performed, in order to make both corners of the mouth symmetrical. Generally, the elongation of the oral fissure is performed at more than 3 weeks after the healing of incision in one-stage operation.
2.5.2 Surgical Procedures
- 1.
The routine disinfection and sterile draping are carried out. Generally in the corner of the mouth, the triangle incision of appropriate length and size is made toward the outside skin and extending along the vermilion border. The unilateral elongation of the oral fissure is performed taking the healthy side as the standard (Fig. 5.4a); if there exist bilateral small mouth deformities, it is needed to determine the new location of the corner of the mouth. Generally a vertical line is drawn downward from the pupil or the point of intersection of inner and middle one third of the palpebral fissure, and then a horizontal line is drawn outward from the oral fissure; the point of intersection of two lines is the location of the corner of the mouth; two connecting lines are made from this point, respectively, toward the upper and lower vermilion borders to form a triangle.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree