Cutaneous Viral Infections
Jessica Kaffenberger
Richard H. Flowers
Barrett J. Zlotoff
Mark R. Wick
Viral diseases of the skin are relatively common in children and are more varied in nature than that seen in adults. The current widespread practice of early vaccination in pediatrics has markedly decreased the number of active viral infections, when compared with historical data. However, many children are still affected by them yearly on an international scale. This chapter outlines the spectrum of cutaneous viral infections in early life, along with possible associated complications.
HERPES SIMPLEX VIRUS
Definition and Epidemiology
Herpes simplex virus (HSV) is a part of the herpesvirus family that includes herpes simplex virus-1 (HSV-1), herpes simplex virus-2 (HSV-2), varicella-zoster virus, cytomegalovirus, Epstein-Barr virus, and human herpesviruses and 6-8.1 HSV causes a vesicular rash that periodically flares throughout the patient’s life.
HSV-1, a ubiquitous virus, is typically transmitted during childhood via nonsexual contact. It predominantly affects the oral mucosa, pharynx, and lips. HSV-2 is primarily linked with sexual transmission and affects the genital tract; however, in the United States, HSV-1 is becoming an increasingly prevalent cause of genital herpes.2 In neonates, HSV-2 can be acquired via vertical transmission from the mother to child during passage through the birth canal.3
Between 2005 and 2010, HSV-1 seroprevalence was 30% between ages 14 and 19, 50% by age 20 to 29, and 62% by ages 30 and 39. (4) Between the same years, HSV-2 had a seroprevalence of 1.2% between the ages of 14 and 19, 10% by age 20 to 29, and 19% by ages 30 to 39.4
Etiology
Herpesvirus family consists of large, enveloped, double-stranded DNA viruses. HSV-1 and 2 serotypes have a similar DNA sequence but carry different envelope proteins.1
HSV-1 and 2 proliferate intracellularly after entering the skin or the mucous membranes, resulting in a vesicular eruption. The primary episode in most immunocompetent hosts will clear after a few weeks; however, the virus will travel in a retrograde manner along axons to neuronal cell bodies. Here, the virus will establish a life-long latent infection. The trigeminal and sacral ganglia are the primary sites of HSV1 and HSV2 latency.1,5 At periodic times, the virus reenters the lytic phase, travels back to the skin or mucous membranes, and creates another vesicular outbreak.6 The recurrences may be spontaneous or a result of numerous triggers, including stress, sunlight, heat, cold, menstruation, fevers, trauma, or immunosuppression.7
Clinical Presentation
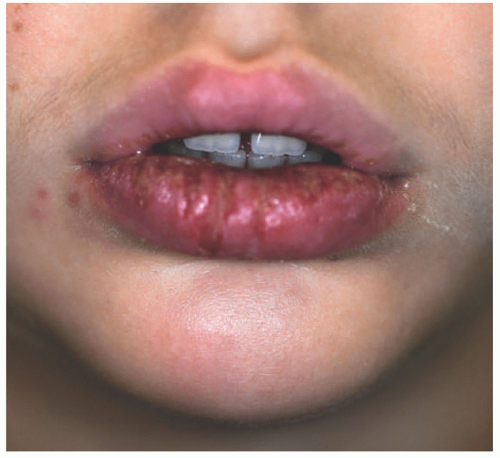
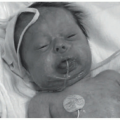
The classic lesions of HSV-1 and 2 are grouped vesicles on an erythematous base (Figure 19-1). The sensations of burning, numbness, or pain often precede the vesicular outbreak. Although often asymptomatic, initial exposure to HSV-1 can result in primary gingivostomatitis and most commonly occurs in young children between 1 and 5 years old.1 This primary infection can be widespread, with lesions occurring both intraorally and periorally on the lips, cheeks, and chin (Figure 19-2).1,3,8 Children are often unable to swallow because of the pain and are at risk of dehydration.
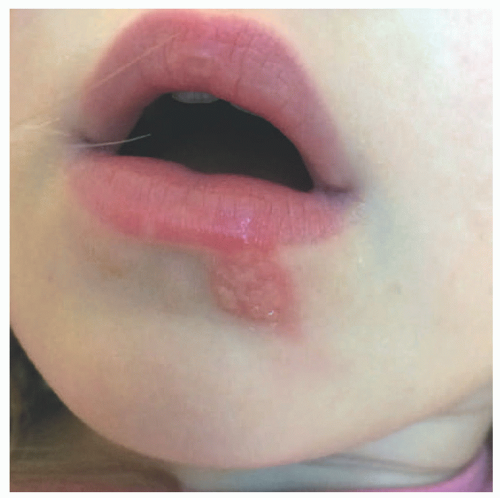
Associated fevers and lymphadenopathy may also be present. Severe cases of herpetic gingivostomatitis often warrant hospitalization where hydration and pain control can be provided. Recurrences of HSV-1 are generally less severe than the primary infection and present as the classic “cold sore” (Figure 19-3).3
Associated fevers and lymphadenopathy may also be present. Severe cases of herpetic gingivostomatitis often warrant hospitalization where hydration and pain control can be provided. Recurrences of HSV-1 are generally less severe than the primary infection and present as the classic “cold sore” (Figure 19-3).3
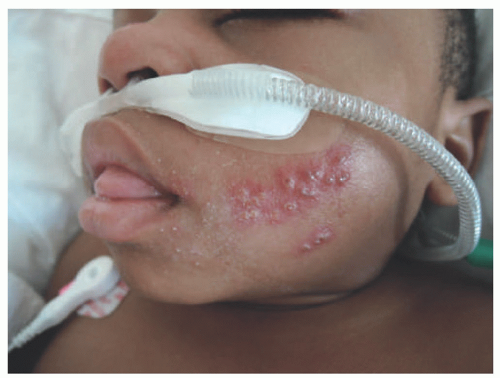 FIGURE 19-1. Grouped vesicles and vesiculopustules on an erythematous base in neonatal herpes simplex virus infection. |
Primary HSV-1 can also affect the eye and is a leading cause of corneal blindness in the United States.9 Patients often have concurrent primary oral HSV infection or a prior history of oral HSV.1 Clinical signs include conjunctivitis, edema, erythema, and erosions of the cornea. Patients often experience severe pain, photophobia, and eye watering. Urgent ophthalmologic evaluation is essential.1
Neonates are also susceptible to HSV, and the virus can be transmitted in utero, peripartum, or postpartum. Around 95% of neonatal HSV infections are acquired during the peri- or postpartum periods with the greatest risk of transmission from a mother with a primary genital HSV infection at or near the time of delivery. Neonatal HSV most commonly affects the mouth, skin, or eyes, yet rarely can lead to central nervous system (CNS) or disseminated disease.10
HSV-2 is primarily responsible for genital tract disease. Like HSV-1, most primary HSV-2 infections are subclinical and are, therefore, unnoticed.11 However, if symptomatic, primary HSV-2 typically affects the vulva, labia, vagina, perineum, penis, or urethra. Cervical lesions in females are also common in primary infections. Widespread vesicles rupture, leaving painful erosions and ulcers.1
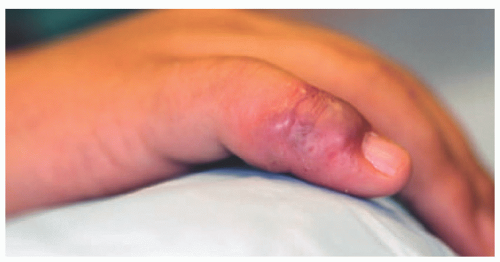
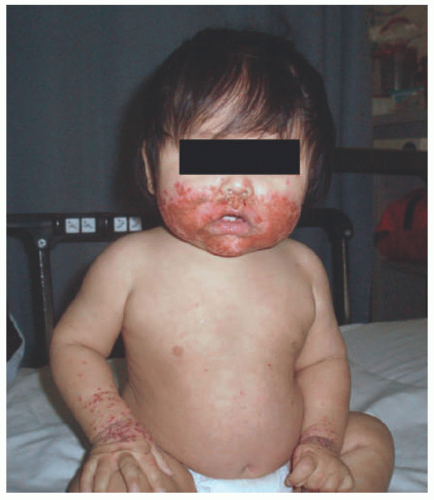
Children are more prone to cutaneous HSV than adults, with one study citing that 60% of children who visited an academic dermatology center for HSV had no labial or mucosal involvement.8 Cutaneous HSV can occur in any location, but there are several distinct subtypes that are often seen in children. In neonates, HSV can infect traumatic wound from scalp electrodes and prevent healing of scalp erosions.12 Herpetic whitlow is a distinct form of HSV involving the distal phalanx (Figure 19-4). Herpes gladiatorum refers to widespread HSV1 inoculation through abraded skin from sports such as wrestling or rugby. Finally, eczema herpeticum, also known as Kaposi’s varicelliform eruption, is a widespread HSV infection of the impaired skin of patients with atopic dermatitis (Figure 19-5) or other condition causing an impaired skin barrier.1
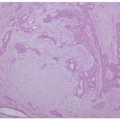
Histologic Findings & Differential Diagnosis
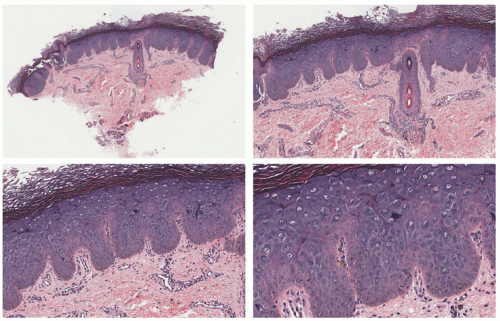
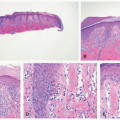
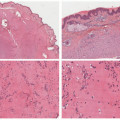
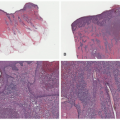
HSV dermatitis begins as an intraepidermal process, proceeding to the formation of subepidermal blisters. Infected keratinocytes in the epidermis and hair follicles undergo “ballooning” degeneration and acantholysis, and they may form multinucleated cells. Nuclei often have a “gun-metal gray” color, with margination and homogenization of chromatin (Figure 19-6). At least some contain eosinophilic viral inclusions, surrounded by clear halos. As the lesions age, the keratinocytes become intensely eosinophilic and the cited nuclear changes tend to disappear. Dermal inflammation is variable in quantity and constituency; it may include a mixture of mononuclear cells and neutrophils, and, in rare cases, lymphoid cells in the infiltrate are numerous and cytologically atypical (Figure 19-7). Indeed, on many occasions, a rich CD30-positive infiltrate is seen. Vasculitic changes are also very frequent in the biopsies. The presence of inflammation of the sebaceous glands attached to the hair follicles can also point toward the diagnosis of HSV infection.13,14,15,16,17,18,19 Immunostains for HSV-1 or HSV-2 are positive in active skin lesions. As mentioned earlier, the microscopic changes of erythema multiforme may develop subsequently.16
CAPSULE SUMMARY
HERPES SIMPLEX VIRUS INFECTION
Up to 62% of people are infected by HSV by age 40. The DNA virus remains latent in neural ganglia. HSV infection causes a vesicular painful eruption on an erythematous base and may cause “eczema herpeticum” in atopic patients. The histopathology of the infection shows intraepidermal vesicles and subepidermal blisters, with “ballooning” degeneration and acantholysis of keratinocytes. The nuclei of infected cells show margination and homogenization of chromatin, and intranuclear viral inclusions are surrounded by a halo. Inflammation is variable, but may simulate lymphoma in some cases.
VARICELLA-ZOSTER VIRUS
Definition and Epidemiology
Varicella-zoster virus (VZV) is a part of the herpesvirus family that includes HSV-1, HSV-2, VZV, cytomegalovirus, Epstein-Barr virus, and human herpesviruses 6 and 8.1 Acute infection with VZV causes a widespread vesicular eruption called varicella, also frequently known as chickenpox. The reactivation of VZV that is latent in the sensory nerve ganglia causes herpes zoster (HZ), often known as shingles. The terms “shingles” and “zoster” derive from the Latin and Greek words for “girdle”, referring to the girdle-like dermatomal distribution of recurrent VZV infections.
VZV is predominately transmitted via air droplets, but can also be spread by direct contact with lesions. VZV is extremely contagious when spread in an airborne fashion. Prior to vaccine development, studies report that 60% to 100% of susceptible household contacts would develop a clinically evident infection.20 VZV’s incidence has dramatically decreased after the development of a varicella vaccine that has been available in the United States since 1995.21,22 One dose of varicella vaccine was reported to be 80% to 85% effective in preventing varicella.23 Although excellent, this was not sufficient to prevent community outbreak, and a two-dose varicella vaccine was approved for children in June 2006.21 A 2017 meta-analysis found the incidence of breakthrough varicella to be 2.2 cases per 1,000 person years in healthy children after two doses of the vaccine, as against 8.5 cases per 1,000 person years for those who received one dose.22
Herpes zoster, which is caused by the reactivation of VZV, has also seen a decline after the institution of the varicella vaccine, and its prevalence has been reported to be 79% lower among vaccinated than among unvaccinated children. Wildtype virus causes over half of HZ cases in children who have been vaccinated. Skin-to-skin contact with fluid from HZ vesicles can transmit VZV to susceptible individuals.24
Etiology
Herpes virus family consists of large, enveloped, double-stranded DNA viruses. When transmitted via respiratory droplets, the virus disseminates hematogenously, causing a systemic infection. The virus then invades the capillary endothelial cells in order to invade the epidermis and cause cutaneous lesions. Once the primary infection resolves, VZV travels in a retrograde fashion back to the dorsal root ganglia where it establishes latency. The reactivation of VZV can occur years after primary infection, and usually presents in a dermatomal distribution as HZ. Like HSV, reactivation can be spontaneous or occur because of stress, sunlight, heat, cold, menstruation, fevers, trauma, or immunosuppression.25
Clinical Presentation
VZV is usually preceded by a prodrome of fever, malaise, and myalgia. Following this prodrome, vesicles surrounded by a rim of erythema, colloquially described as “dewdrops on a rose petal”, erupt on the scalp and face and then spread to the trunk and extremities (Figure 19-8). Vesicles quickly form pustules or crusts and then heal within 7 to 10 days. The presence of lesions in numerous stages of development is a hallmark of varicella in contrast to smallpox, which presents with all lesions in the same stage of development.25
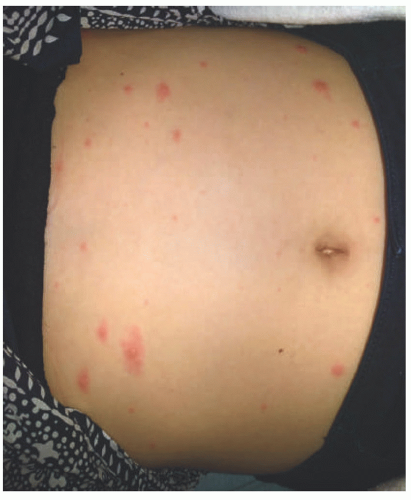 FIGURE 19-8. Vesicles on an erythematous base in the “dew drops on a rose petal” pattern found in primary varicella-zoster virus infection, commonly known as “chicken pox.” |
Maternal VZV during the first 20 weeks of pregnancy can put the fetus at risk for developing congenital varicella syndrome, which is characterized by multisystem abnormalities, including ocular abnormalities, low birth weight, brain abnormalities, cutaneous scarring, and hypoplastic limbs.26 Transplacental transmission can also cause outbreaks within the first 10 to 12 days of life.27
Like VZV and HSV, HZ is characterized by vesicles on an erythematous base. HZ is classically confined to a dermatomal distribution (Figure 19-9), with more than 50% of cases exhibiting a thoracic distribution. Vesicles usually appear proximally and then spread distally along the affected dermatome.28 HZ is often preceded by and then accompanied by severe hyperesthesia, pain, and tenderness. After the cutaneous lesions resolve, some patients develop postherpetic neuralgia, which manifests as recurrent sharp, “lightening-like” pain, and paresthesia in the previously affected areas. Fortunately, in otherwise healthy children, postherpetic neuralgia is very rare.29
Histologic Findings
The microscopic features of skin lesions in shingles and PV are largely superimposable on those of HSV. All of those disorders feature the presence of distinctive multinucleated cells in cytologic scrape preparations of unroofed blisters (Tzanck smears) (Figure 19-10). Inflammation is least prominent in the early lesions of primary varicella, compared with those of HSV and shingles. Immunostains for VZV are positive in the infected keratinocytes of both primary varicella and shingles.
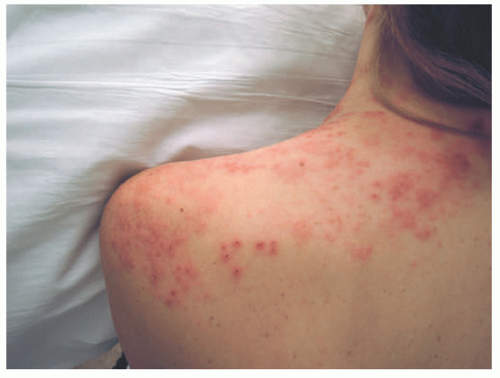 FIGURE 19-9. Punched-out erosions, vesicles, and erythematous-eroded plaques in a dermatomal distribution in recurrent varicellazoster infection, commonly known as “shingles.” |
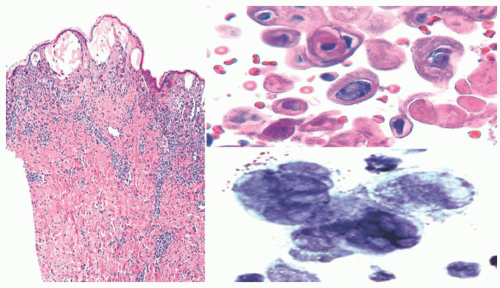 FIGURE 19-10. This example of varicella-zoster virus dermatitis shows findings that are comparable to those seen in Figure 19-6, including intraepidermal vesicles with reticular degeneration (left panel), marginated nuclear chromatin, and intranuclear inclusions (top right). A Tzanck smear from one of the vesicles demonstrates the multinucleated lesional cells, as seen with a Papanicolaou stain. |
CAPSULE SUMMARY
VARICELLA-ZOSTER VIRUS INFECTION
Infection by VZV occurs by airborne spread as well as by contact with lesions from infected individuals. Maternal transmission can result in dermatomal scar-type presentation with systemic sequela. There has been a decreased incidence since the development of an effective vaccine, but the infection can still occur in vaccinated children. VZV is a DNA virus that remains latent in neural ganglia; chickenpox in children can be followed by “shingles” in adolescence or adulthood, sometimes with multiple episodes. Postinfectious neuralgia may follow shingles, but this is rare in children. The clinical and histologic features of VZV lesions are superimposable to those of HSV.
WARTS
Definition and Epidemiology
Warts (verrucae) are caused by human papillomaviruses (HPV) that infect the epithelial tissues of the skin and mucous membranes. HPV is a ubiquitous virus with over 200 distinct HPV genotypes currently characterized.30,31 Some subtypes of HPV, especially HPV-16 and 18, are classified as high risk and can incite changes leading to numerous malignancies; to cite an example, cervical cancer.31
Verruca vulgaris, also known as common warts, are most commonly associated with HPV types 1, 2, 27, 57, with type 1 most commonly occurring in children under 12 years old.32 Verruca plana (flat warts) are primarily associated with HPV types 3, 10.33 Palmar-plantar (myrmecial) verruca are most commonly associated with HPV type 1, but types 2, 27, and 57 are also seen.32,33,34 Condyloma (genital warts) are associated predominately with HPV subtypes 6 and 11.35 Verruca are transmitted via skin-to-skin contact or from fomites on warm, wet areas such as public pools or showers.33 Common warts have a prevalence of up to 25% in schoolchildren and often go untreated.36 However, even without treatment, most common warts will spontaneously regress.31
Condyloma acuminata (CA) is one of the most common sexually transmitted diseases in adolescents and adults. The prevalence of this condition in infants and children remains poorly studied. A female predominance has been reported.37 Condyloma in children should always warrant at least a consideration of sexual abuse. However, autoinoculation or heteroinoculation from mothers, siblings, or caretakers are frequently responsible for transmission.34,38 After a thorough investigation, one study indicated that only 3 of 131 patients were ruled suspicious for sexual abuse.38 The older the child the more likely sexual abuse is a cause. Vertical transmission from maternal birth canal is most likely for those under 2 years. Abuse is rare for those under 4 years; for 4 to 8-year-olds, it is still rare but more of a consideration, and in the 8 or older age group, abuse is 12 times more likely than in the 4 and under age group.39
Etiology
HPVs are small, nonenveloped, circular, double-stranded DNA viruses. The virus infects the basal cells of the stratified epithelium.31 In order for the HPV to reach the basal layer, it is likely that microabrasions in the skin serve as a portal of entry for the virus. HPV utilizes numerous mechanisms to avoid inciting an immune response. The virus does not cause cell death, which would trigger inflammation and a subsequent immune response. Instead, the infected cell is shed during the natural turnover of keratinocytes. Additionally, HPV downregulates interferon gene expression, thereby preventing a robust immune response.40
Clinical Presentation
Verruca Vulgaris
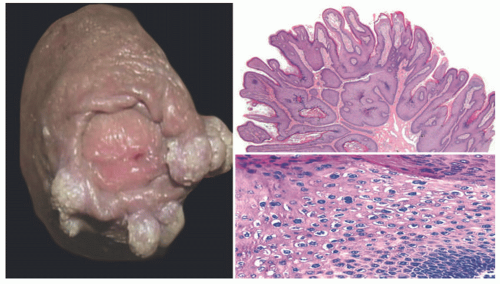
Verruca vulgaris are most commonly flesh-colored, pink, or light brown papules with a verrucal (rough) surface. They may be dome-shaped, hyperkeratotic, exophytic, or filiform and often affect the dorsal hands (Figure 19-11) or periungal areas, but can also be seen on the face and extremities. 33,34 Upon close examination, verruca vulgara often have black puncta that reflect thrombosed capillaries. A linear formation created by autoinoculation secondary to scratching or a ringed appearance (Figure 19-12) following aggressive topical therapies are examples of koebnerization of the disease.
Verruca Plana
Verruca plana are flesh-colored, pink, or light brown flat-topped papules. Unlike verruca vulgaris, verruca plana are smooth and are usually small with a diameter under 5 mm.33 Verruca plana koebnerize easily and are commonly found on the dorsal hands, arms, face, or legs.
Palmoplantar Verrucae
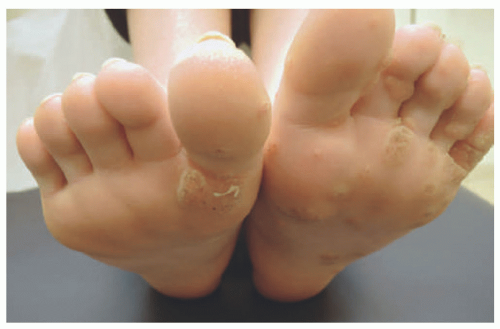
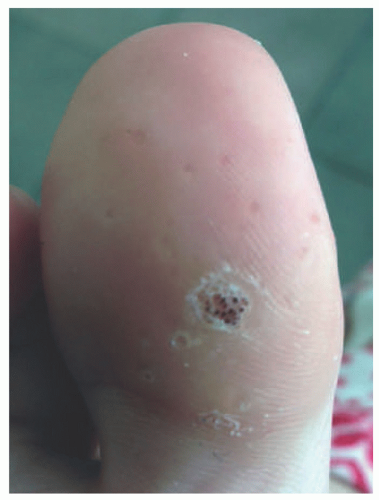
Palmar and plantar verrucae are thick, hyperkeratotic papules or plaques found on the palms or soles. These warts are often on pressure points of the foot and therefore can cause significant discomfort (Figure 19-13).33 The thick keratotic plug is often surrounded by a hyperkeratotic rim, and removal of the plug leaves a central depression behind.33 The presence of thrombosed capillaries is helpful to distinguish these warts from corns or calluses (Figure 19-14).34
Condyloma Acuminata
These are pink, soft, exophytic papules most commonly found perianally in children.38 Lesions can also occur on the penis, scrotum, and vulva. Multiple lesions are usually present, and these lesions can coalesce into large, exophytic plaques. Small lesions are frequently asymptomatic; however, these large plaques are easily irritated, resulting in pain and bleeding.33
Histologic Findings
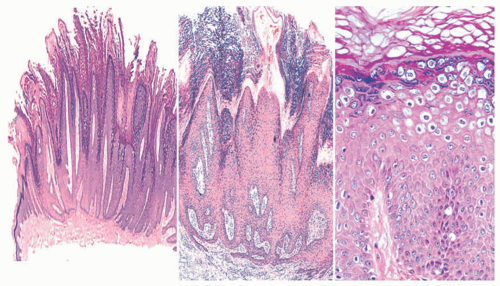
Histologically, verruca vulgaris (VV) shows epidermal hyperkeratosis and parakeratosis. The second of those changes often assumes the appearance of peaked columns (“peaking parakeratosis”). Other typical changes include hypergranulosis with a clumping of cytoplasmic keratohyaline; papillomatosis with lengthening of the rete ridges; hypervascularity of the upper dermis; and bowing of the peripheral rete in the lesion, toward its center. The last of those changes may ultimately cause fusion of the rete ridges, producing a flat lesional base. Evidence of intranuclear viral replication includes perinuclear halos in infected keratinocytes (“koilocytes”), with possible binucleation, as well as crenation and hyperchromasia of the nuclei or homogenization of chromatin (Figure 19-15).
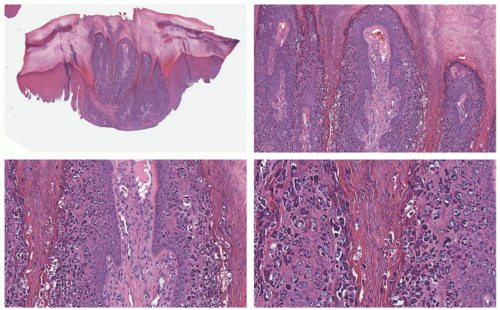
Ordinary and myrmecial plantar warts have different appearances. The first of those lesional groups shows exophytic, papillomatous epidermal growth with koilocyte formation and prominent cytoplasmic keratohyaline granules. In myrmecial verrucae, one sees endophytic epidermal growth, with large eosinophilic granules in the cytoplasm and nuclei of infected keratinocytes. Cellular vacuolization is also common (Figure 19-16).41,42,43,44
Microscopically, CA show epidermal papillomatosis, often yielding frond-like profiles or a more blunted “roller-coaster” surface configuration (Figure 19-17). Variable parakeratosis is apparent, along with possible epidermal koilocytosis and nuclear crenation. Another peculiarity of CA is that they may virtually perfectly imitate the histologic appearance of extragenital seborrheic keratoses, with interlocking bars of bland epidermal epithelium that are punctuated by keratinous “horn cysts.”45
CAPSULE SUMMARY
HUMAN PAPILLOMAVIRUS INFECTION
Over 200 DNA viral HPV genotypes belong to this category. They are transmitted by skin to skin or fomite to skin transfer. HPV does not cause cell death; virus is shed during keratinocyte turnover. Multiple clinical forms like verruca vulgaris, verruca plana, palmoplantar verruca, and condyloma acuminatum exist. The histologic features of HPV infection include epidermal papillomatosis, clumping of keratinocyte keratohyaline, bowing of peripheral rete to a central focal point, and koilocytosis.
EPIDERMODYSPLASIA VERRUCIFORMIS
Definition and Epidemiology
Epidermodysplasia verruciformis (EV) is a rare autosomal recessive genodermatosis that predisposes patients to widespread infections with specific HPV subtypes, most commonly HPV 5 and 8.
EV was first described by Lewandowksy and Lutz in 1922.46 Reports first mapped the disease to several consanguineous EV families.47 However, since this time, genetic cases of EV have been documented worldwide. The disease likely carries genetic heterogeneity, with only 75% of the affected individuals carrying the known inactivating mutations of EVER1/TMC6 (transmembrane channel-like) and EVER2/TMC8.48,49,50
In 2009, the term “acquired EV” (AEV) was adopted to describe an EV-like syndrome that developed in immunosuppressed patients.51
Etiology
EV is a genodermatosis caused by mutations in two adjacent genes, EVER1/TMC6 and EVER2/TMC8.47 EVER genes encode endoplasmic reticulum transmembrane proteins that are important in ion transport and signal transduction.47,48 It is proposed that TMC6 and TMC8 provide resistance to HPV by regulating intracellular zinc and by increasing tumor necrosis factor-alpha.50
At least 20 HPV subtypes have been found in EV patients. The most common subtypes are HPV 5 and 8, both of which are associated with malignant transformation.48
AEV has been described in patients with defective cell-mediated immunity such as infection (HIV), non-Hodgkin lymphoma, leprosy, or medications. This entity is very
rare, with several scientists suggesting that affected patients have an unknown genetic susceptibility to EV infections.50
rare, with several scientists suggesting that affected patients have an unknown genetic susceptibility to EV infections.50
Clinical Presentation
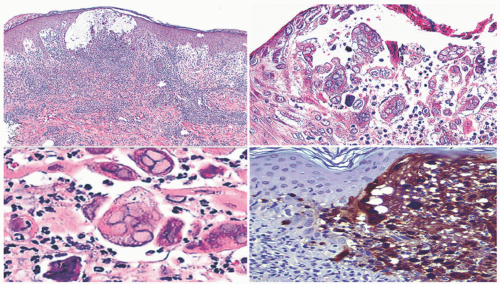
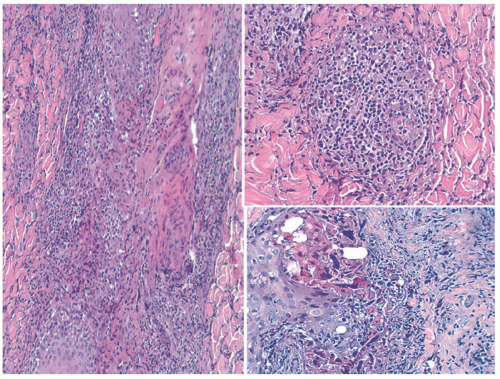
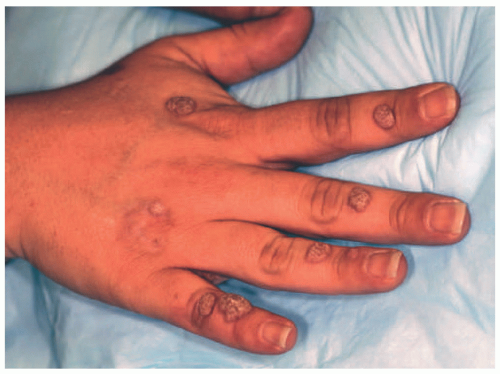
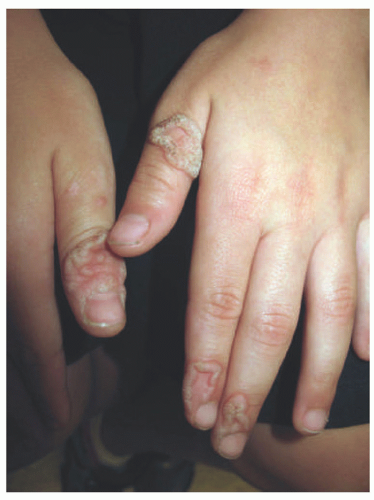
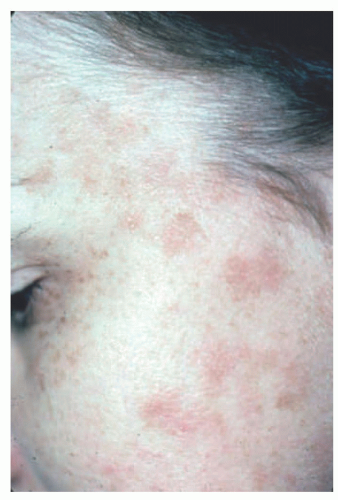
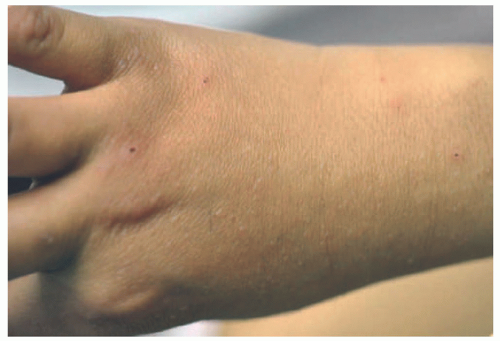
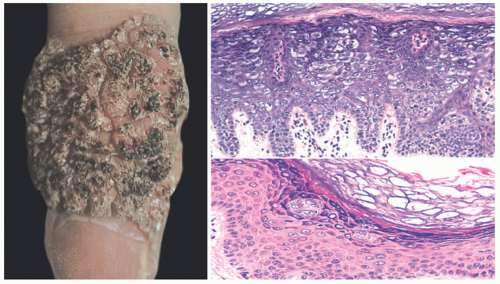
EV skin lesions begin in early childhood and are often characterized by slightly scaly, reddish-brown papules and patches that resemble pityriasis versicolor (Figure 19-18). Lesions can also resemble flat warts and usually start on the dorsal hands (Figure 19-19) and forehead and then spread to the arms, legs, neck, and trunk, with particular involvement of the gluteal cleft area (Figure 19-20). The buttocks and other non-sun-exposed skin are an unusual site for flat warts outside of EDV. Mucosal membranes are spared. Lesions are refractory to treatment.50 Malignant transformation, most commonly to squamous cell carcinoma, occurs in 30% to 70% of patients by early adulthood. Carcinomas are predominantly found in sun-exposed areas, suggesting a role of UV irradiation in malignant transformation.48,50,52
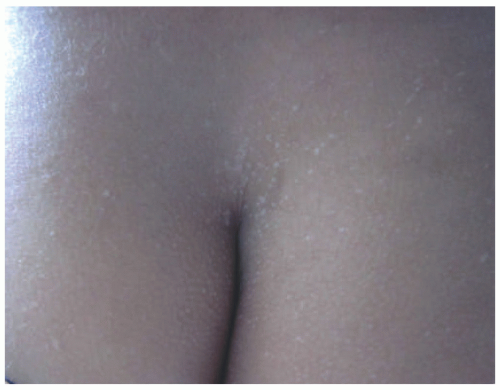 FIGURE 19-20. Thin, flat wart-like papules in gluteal cleft, an unusual site for flat warts but common in epidermodysplasia verruciformis. |
Clinically, AEV resembles EV. It has been reported in patients of all ages and in both sexes equally.51
Histologic Findings
Histologic findings in EV differ somewhat from those associated with ordinary VV or CA. The biopsies of EV show viral changes over a relatively broad expanse of epidermis, or multiple “islands” thereof in the surface epithelium. One sees enlarged keratinocytes in the upper epidermis; these often have blue-gray cytoplasm and may also demonstrate koilocytosis. Hypergranulosis is commonly present, but, in some cases, it affects only small islands of keratinocytes that are scattered throughout the upper epidermis (Figures 19-21 and 19-22).53,54,55,56,57
CAPSULE SUMMARY
EPIDERMODYSPLASIA VERRUCIFORMIS
EV is an autosomal recessive genodermatosis that predisposes to infection with specific HPV types—usually 5 and 8. Mutations in 2 adjacent genes—EVER1/TMC6 and EVER2/TMC8 on chromosome 17 can be seen. “Acquired” EV is associated with defective cellular immunity, as seen in infection with human immunodeficiency virus, non-Hodgkin lymphoma, and patients undergoing intense chemotherapy. Clinically, the lesions appear in early childhood as scaly red-brown papules
and patches, which multiply in number and involve the neck, extremities, and trunk, mimicking tinea versicolor in some cases. There is no mucosal involvement. Squamous cell carcinoma complicates EV in 3% to 70% of cases, usually on sun-exposed skin. The biopsies of EV show changes associated with HPV infection over a broad expanse of epidermis or multiple islands of infected cells in the surface epithelium.
and patches, which multiply in number and involve the neck, extremities, and trunk, mimicking tinea versicolor in some cases. There is no mucosal involvement. Squamous cell carcinoma complicates EV in 3% to 70% of cases, usually on sun-exposed skin. The biopsies of EV show changes associated with HPV infection over a broad expanse of epidermis or multiple islands of infected cells in the surface epithelium.
CYTOMEGALOVIRUS
Definition and Epidemiology
Cytomegalovirus (CMV) or human herpes virus-5 is a ubiquitous double-stranded DNA virus. It is an opportunist infection in the setting of immunosuppression especially in transplant and AIDS patients. CMV is a very common infection, with 70% to 90% of individuals being infected worldwide. CMV is the most common congenital infection, affecting up
to 2% of newborns58 and 0.7% of newborns in the United States.59 Infection is asymptomatic in up to 90% of neonates.60
to 2% of newborns58 and 0.7% of newborns in the United States.59 Infection is asymptomatic in up to 90% of neonates.60
Etiology
CMV is transmitted via urine, saliva, sexual fluids, and breast milk. Blood transfusions may also transmit CMV. Transmission from mother to fetus/infant may occur via the placenta, during delivery via cervical secretions and postnatally via breast milk or saliva. Transmission rates are higher in women with primary CMV infection versus women with reactivation. 60 Following primary infection, CMV establishes life-long latency within the host. Periodic reactivation may result in viral shedding; reinfection is not uncommon with other viral strains. Systemic infection may occur in neonates and in immunosuppressed populations.58
Clinical Presentation
Symptomatic manifestations in neonates are similar to other TORCH infections (toxoplasmosis, syphilis, rubella, CMV, herpes simplex). The liver, spleen, gastrointestinal tract, and CNS are prominently affected, with the later classically resulting in deafness, encephalitis, and intracranial calcifications. Severe neurologic damage, sensorineural hearing loss, and permanent developmental delay may occur, even in asymptomatic individuals. Cutaneous manifestations include jaundice, purpura, and a “blueberry muffin” appearance.61 The latter describes dark blue-red papules and nodules representing extramedullary erythropoiesis. Cutaneous vesicles may rarely occur.62
Aside from congenital infection, CMV-associated disease occurs most commonly in adults and children with immunodeficiency where it may manifest infection of the retina, CNS, lungs, and gastrointestinal tract. This occurs characteristically in the setting of HIV/AIDS but also in immunocompromised patients with hematologic malignancy or postorgan transplantation. The most common cutaneous manifestation in this setting is sharply demarcated anogenital ulcerations, but lesions may be extragenital in children. These ulcers are often coinfected with HSV in patients with AIDS, but not in patients who are immunocompromised from other etiologies.63,64 A diaper dermatitis-like presentation in a child with disseminated CMV has been described.65 Gianotti-Crosti syndrome in children may result from CMV.66 CMV can cause a heterophil-antibodynegative mononucleosis-like syndrome (fevers, myalgias, abnormal liver function tests, atypical lymphocytosis) with a “rubelliform” rash in adolescents/young women.61,67 A small-vessel vasculitis with livedo-like changes was reported in this setting.68 Scleredema-like changes in an infant with CMV pneumonia has been reported as well.69 A variety of other nonspecific lesions, including purpuric papules and plaques, exanthems, crusted papules, vesiculobullae and prurigo nodularis-like lesions, have been reported, although predominantly in adults.70
Histologic Findings
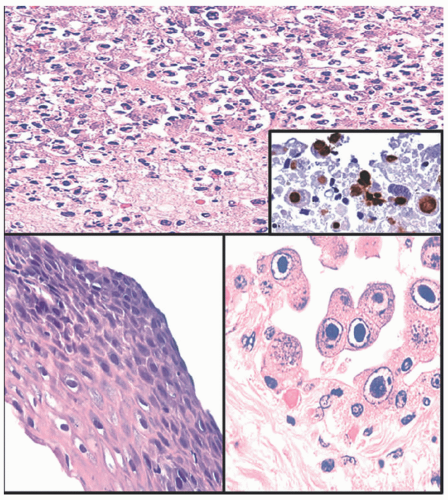
In the skin, CMV can actively proliferate in vascular endothelium, the epidermis, or dermal appendages. Cutaneous biopsies show possible ulceration and mixed acute and chronic inflammation in the corium. CMV-infected cells often contain characteristic large, eosinophilic nuclear inclusions surrounded by a halo (Figure 19-23). They are easily visible by routine microscopy, but may be accentuated with immunostains for CMV-early antigen or in situ hybridization for CMV DNA.71,72,73,74
CAPSULE SUMMARY
CYTOMEGALOVIRUS INFECTION
CMV is synonymous with human herpesvirus-5. Congenital CMV infection can cause purpura and “blueberry muffin” lesions in the skin of babies. CMV causes an opportunistic infection in immunocompromised hosts. Clinically, there are sharply demarcated cutaneous ulcers in diaper area, and other locations may be CMV-infected in immunodeficient individuals. The virus is transmitted by contact with bodily secretions. Adolescents may develop CMV-related illness resembling infectious mononucleosis. Histologically, CMV infects vascular endothelium, epidermal keratinocytes, and dermal appendageal epithelium, with possible ulceration. Infected cells contain large intranuclear eosinophilic viral inclusions, surrounded by halos.
EPSTEIN-BARR VIRUS
Definition and Epidemiology
Epstein-Barr virus (EBV) or human herpes virus-4 is a double-stranded DNA virus. It is a very common human pathogen resulting in a wide range of clinical manifestations particularly in the pediatric population.
EBV infection is ubiquitous, with prevalence reaching 95% in adults worldwide.75 The incidence by age varies in different countries; in the United States for example, approximately 50% of the population have seroconverted by age 5. In developing countries, children acquire the infection earlier, with universal seroconversion occurring by age 3 to 4. By adulthood, the vast majority of individuals regardless of socioeconomic status or nationality would have seroconverted.76
Etiology
EBV infection is transmitted through bodily fluids, primarily oral secretions but also blood transfusions, genital secretions, and breast milk.77 The virus infects the oropharynx and then targets circulating B-lymphocytes via the binding of CD21. Following acute infection, EBV establishes latency
within the B-cells. It escapes immune recognition by limiting viral gene expression. In the presence of compromised cell-mediated immunity, B-cells become immortalized and may lead to EBV-induced malignancy. Cell-mediated immunity is protective against primary infection, but an internal reactivation of the virus leads to periodic viral shedding.78
within the B-cells. It escapes immune recognition by limiting viral gene expression. In the presence of compromised cell-mediated immunity, B-cells become immortalized and may lead to EBV-induced malignancy. Cell-mediated immunity is protective against primary infection, but an internal reactivation of the virus leads to periodic viral shedding.78
Clinical Presentation
EBV is associated with a variety of mucocutaneous manifestations in children, including nonspecific exanthem, infectious mononucleosis, Gianotti-Crosti syndrome, non-sexually-related acute genital ulcers, oral hairy leukoplakia, and hydroa vacciniforme (HV), in addition to a host of neoplastic and lymphoproliferative diseases. Nonspecific manifestations including erythema multiforme, acute urticarial, and leukocytoclastic vasculitis, have also been described.
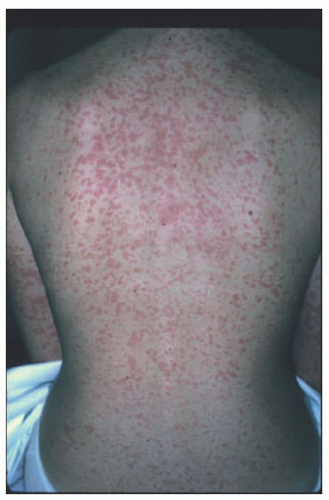
Infants and young children infected with EBV will develop a mild nonspecific febrile illness, if symptoms occur at all. Adolescents and young adults generally develop infectious mononucleosis. The classic triad of fever, lymphadenopathy, and pharyngitis occur in approximately half of patients.78 Fatigue and malaise linger. Patients may also have splenomegaly (leading to feared splenic rupture), hepatomegaly, hemolytic anemia, myocarditis, or CNS disease. The cutaneous manifestations of infectious mononucleosis include palatal petechiae, genital ulcers, jaundice, and a transient pink exanthematous rash. Bilateral upper eyelid edema (Hoagland sign) is an early manifestation.79 Up to 90% to 100% of patients with infectious mononucleosis who are given ampicillin will develop a diffuse morbilliform eruption (Figure 19-24),80,81 but a recent study suggested that the number may be closer to 30%. This rash has been described in the setting of EBV to a variety of antibiotics, including amoxicillin, penicillin, tetracycline, and macrolides.82
Gianotti-Crosti syndrome or papular acrodermatitis of childhood is a distinct eruption of monomorphic edematous papules or papulovesicles (Figure 19-25) on the extensor extremities, cheeks, and buttocks, most often occurring in children younger than 4 years old. Although originally described secondary to hepatitis B infection and also linked to a variety of viral and bacterial infections, the majority of cases are linked to primary EBV infection. The rash generally resolves within 2 to 4 weeks.83
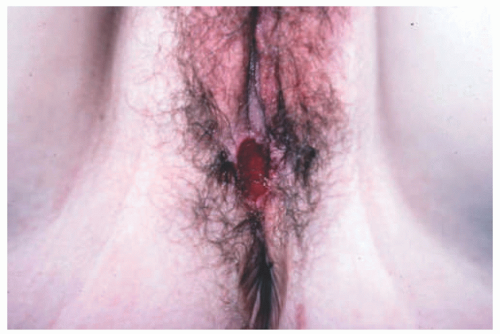
Non-sexually-related acute genital ulcers, or Lipschütz ulcers, are painful genital ulcers often occurring on the labia
minora of adolescent females. They are described as purple-red ulcers with ragged edges (Figure 19-26).77 They are not sexually transmitted and are often associated with systemic symptoms and a history of aphthosis.84 EBV is the most commonly associated infection, although often no etiology is found.85
minora of adolescent females. They are described as purple-red ulcers with ragged edges (Figure 19-26).77 They are not sexually transmitted and are often associated with systemic symptoms and a history of aphthosis.84 EBV is the most commonly associated infection, although often no etiology is found.85
Oral hairy leukoplakia (OHL) is a benign EBV-associated mucosal disease. It is most commonly associated with HIV, but is seen in a variety of immunosuppressive states as well. OHL often presents as white plaques on the lateral tongue with a corrugated surface. The plaques cannot be scraped off, unlike oral candidiasis. OHL is generally asymptomatic but can cause burning, soreness, or taste changes. The appearance of OHL is similar in adults and children, but the incidence of clinical disease may be much less frequent in children.86 Unlike in adults, OHL in children with HIV has not been shown to have predictive value for progression to AIDS.87
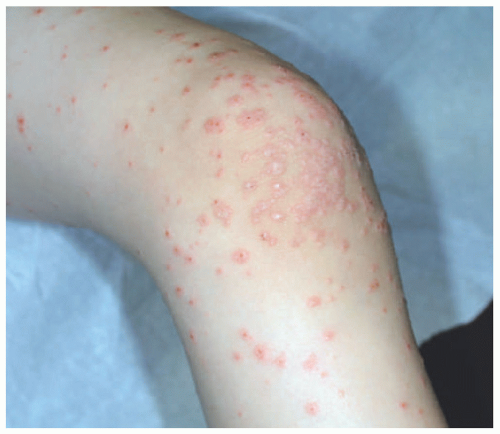 FIGURE 19-25. Juicy, pink papules on extensor surfaces with concentration over elbows in Gianotti-Crosti syndrome. Similar papules occur in high number over knees, buttocks, and cheeks. |
Typical HV is a rare generally self-limited photosensitizing disorder of childhood, associated with EBV infection. HV features painful recurrent papulovesicles on the sun-exposed areas of the cheeks, nose, ears, and dorsal hands/arms that heal with pox-like scars (Figure 19-27). Severe ulcerating lesions are seen in atypical HV, which features less
photosensitivity. This disease could sometimes progress to an HV-like lymphoma, a cutaneous T- or NK-cell lymphoma. The most recent update in the WHO classification has changed the terminology of HV to HV-lymphoproliferative disorder. These children and adolescents may develop fever, lymphadenopathy, and hepatosplenomegaly. Children may develop hypersensitivity to mosquito bites (Figure 19-28), with erythema, bullae, and ulceration as well as systemic symptoms. Underlying chronic active EBV infection as well as NK/T-cell leukemia and lymphoma are associated.77
photosensitivity. This disease could sometimes progress to an HV-like lymphoma, a cutaneous T- or NK-cell lymphoma. The most recent update in the WHO classification has changed the terminology of HV to HV-lymphoproliferative disorder. These children and adolescents may develop fever, lymphadenopathy, and hepatosplenomegaly. Children may develop hypersensitivity to mosquito bites (Figure 19-28), with erythema, bullae, and ulceration as well as systemic symptoms. Underlying chronic active EBV infection as well as NK/T-cell leukemia and lymphoma are associated.77
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree