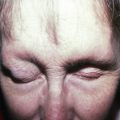
The evaluation of lymphoid neoplasms typically requires clinicopathological correlation, and classification often requires panels of immunostains. This section of the atlas will focus on the clinical appearance of cutaneous lymphomas that should prompt the physician to perform a biopsy. The distribution and morphology of the lesion are also helpful in classification of the neoplasm to ensure optimal therapy.
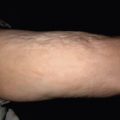
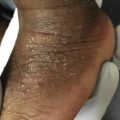
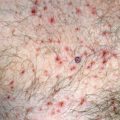
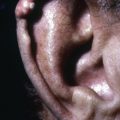
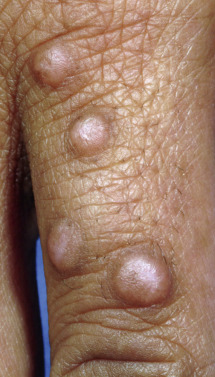
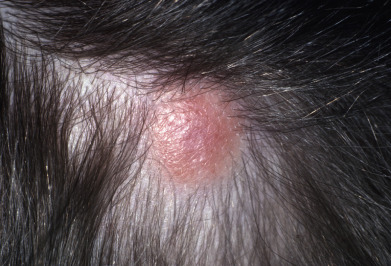
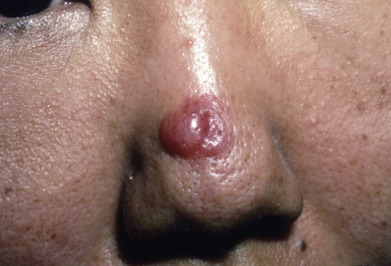
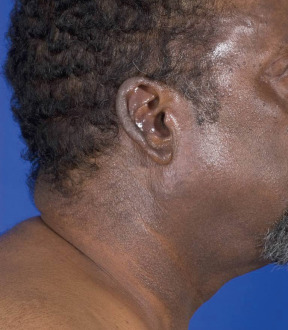
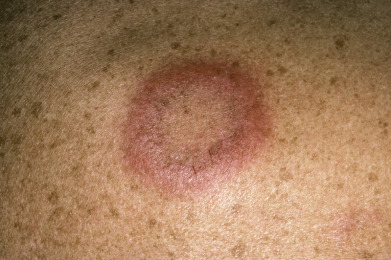
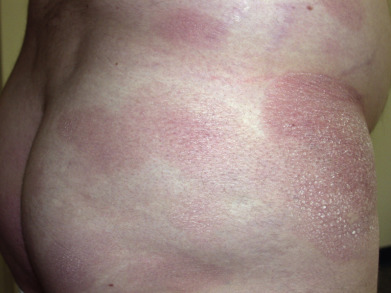
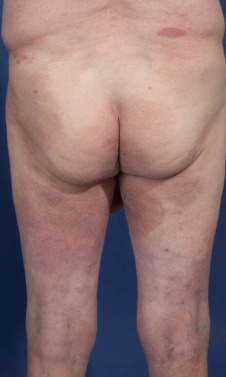
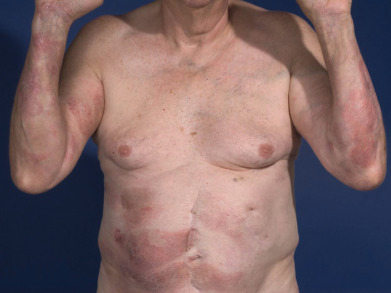
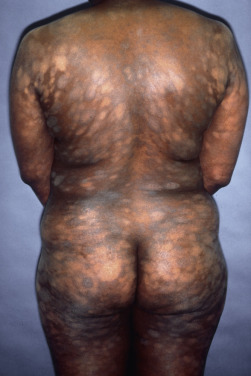
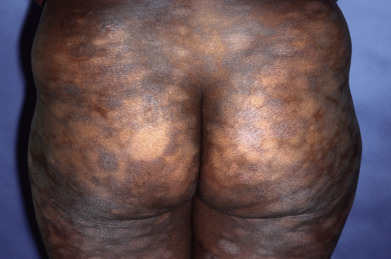
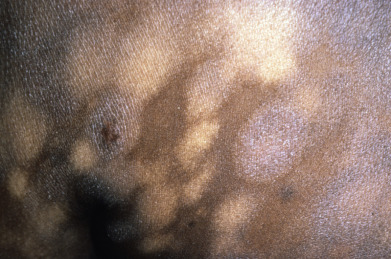
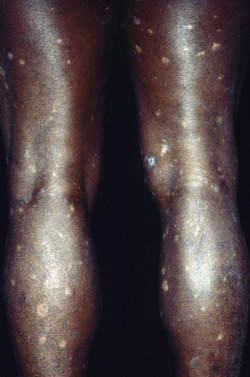
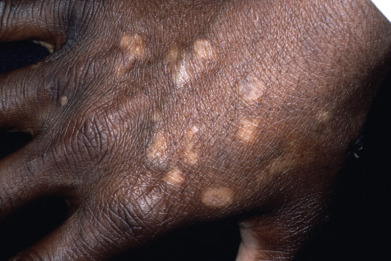
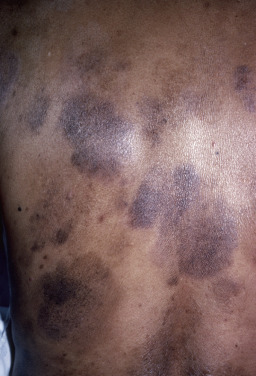
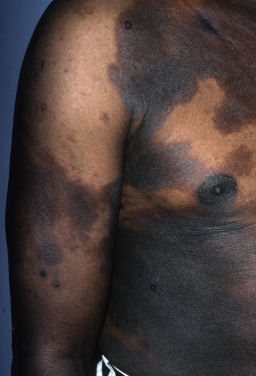
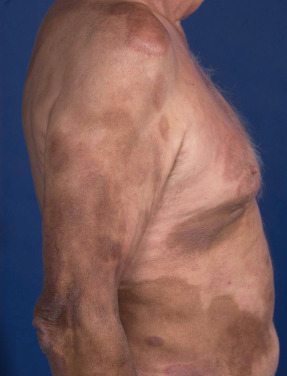
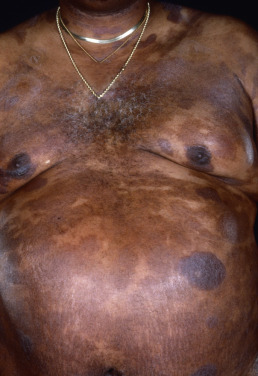
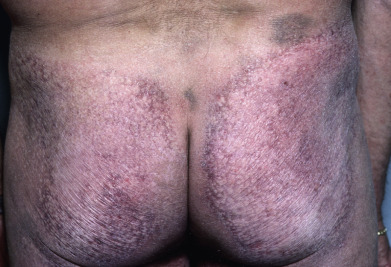
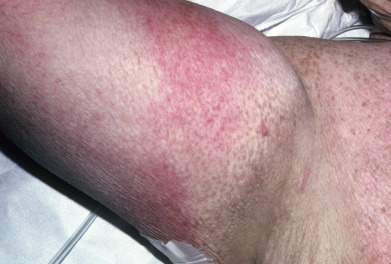
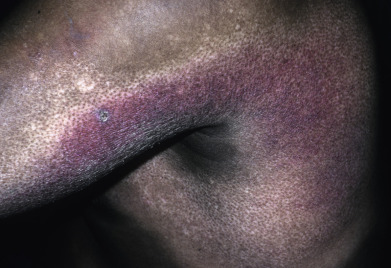
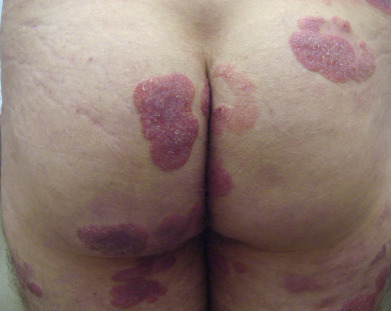
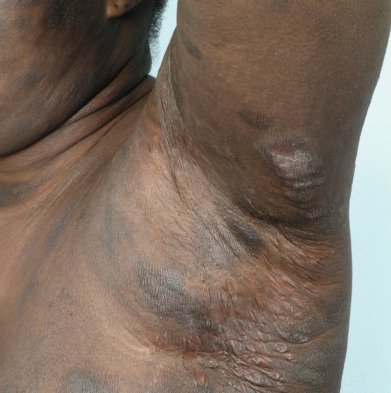
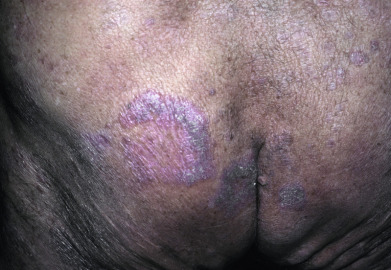
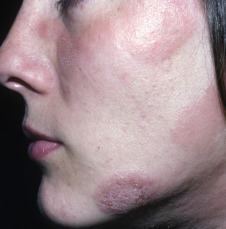
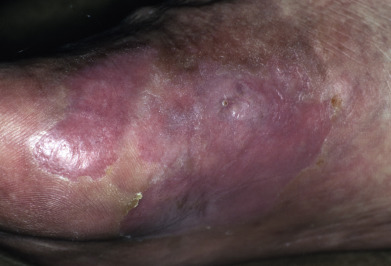
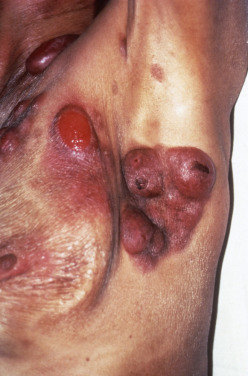
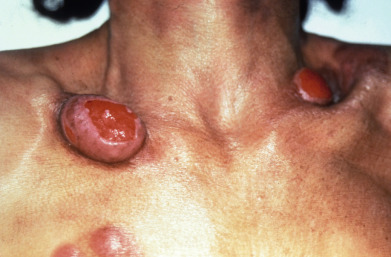
Mycosis fungoides commonly involve the trunk, buttocks, and proximal extremities. The lesions tend to be larger than 5 cm in diameter with a poikilodermatous appearance (mottled, hyperpigmentation and hypopigmentation, atrophy, and telangiectasia). B-cell lymphomas commonly present as plum-colored nodules with a smooth, shiny surface. Discrete nodules on the head and neck, trunk, or proximal extremities; arcuate lesions and nodules on the trunk; taught, shiny nodules on the lower extremities; and multinodular lesions on the legs are all seen in the wide variety of lymphoid neoplasms in this chapter. The lesions of lymphomatoid papulosis are often papulonecrotic, erupt in crops, and resolve spontaneously. Leukemias and myelomas often appear as skin-colored to purple papules and nodules, at times with accompanying hemorrhage into the lesions. This portion of the atlas will focus on the cutaneous manifestations of lymphoid proliferations.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree