Fig. 32.1
Postoperative photos of a failed flap in which necrosis was observed after arterial trombosis. Right upper corner photo is just after perfusion and the left is after 7 days
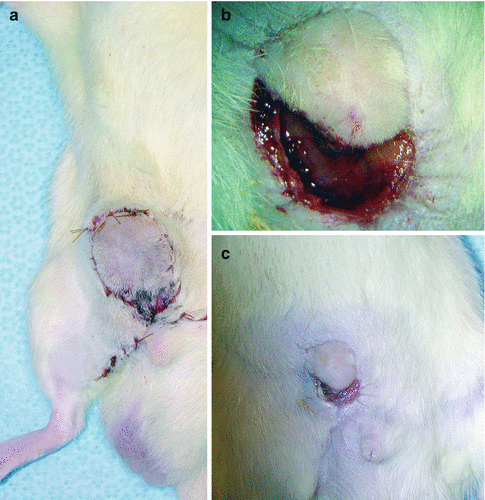
Fig. 32.2
(a) Photo of the first successful flap 1 week after transplantation, (b) 3 weeks and (c) 4 weeks sequentially please note the contraction over time. The flap contracted from 2.5 cm diameter to aproximately 1 cm
According to the histological examinations, failed flaps revealed remarkable endothelial and interstitial oedema, including intravascular thrombi. Survived flaps in which streptokinase was used could be able to withstand endothelial oedema and perfusion persisted leading to clearence of the interstitial oedema (Fig. 32.3). We also found that successful flaps prominently contracted after the first week (Figs. 32.1 and 32.2).
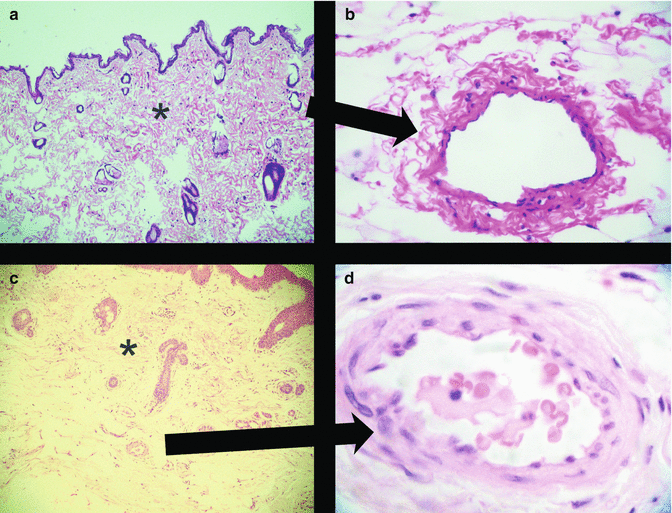

Fig. 32.3
(a) ×50, H&E stained microphotograph of successful flap skin biopsy on day 1 postoperatively, please note the restored interstitial appearence (asterisk) after clearence of oedema fluid. (b) ×400 H&E stained microphotograph of successful flap skin biopsy on day 1 postoperatively showing healthy endothelium. (c) ×50, H&E stained microphotograph of failed flap skin biopsy on hour 1 postoperatively, please note interstitial appearence (asterisk) with marked oedema fluid. (d) ×400 H&E stained microphotograph of failed flap skin biopsy on hour 1 postoperatively postoperatively showing endothelial oedema and intravascular trombus formation
We had performed one case of preliminary study in which we had cryopreserved cremaster flap of an isogenic rat for 1 week in −196° with DMSO perfusion through external iliac artery and thawed using sucrose perfusion including heparin and streptokinase administration. After thawing we have transplanted the cryopreserved cremaster muscle flap to the groin region of the recipient rat via anastomosis to the femoral artery and vein (Fig. 32.4). After spreading to the intravital microscope observation chamber we have noticed the patent perfusion through main branches using optical doppler but it was impossible to visualize the microcirculatory functions in capillary bed and postcapillary venules because of the remarkable oedema.
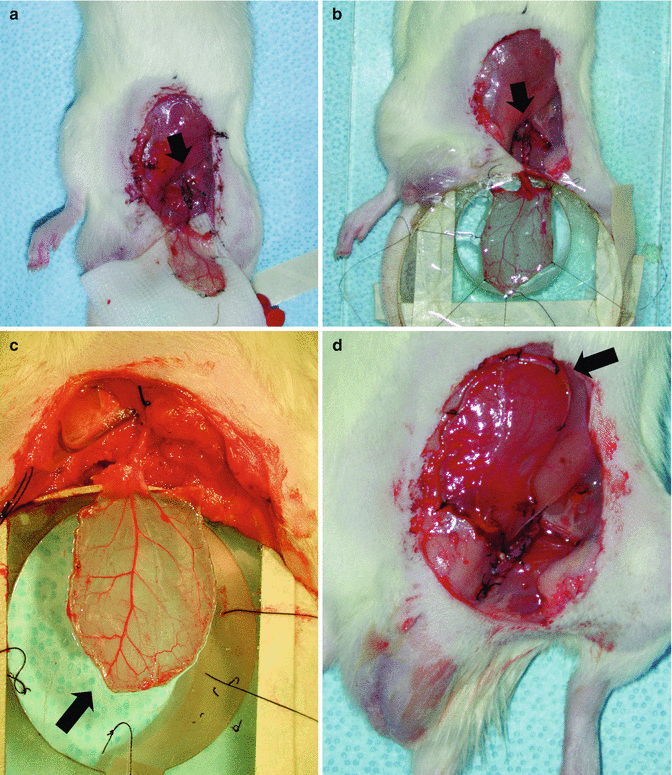

Fig. 32.4
Photos of cryopreserved and thawed isogenic cremaster muscle flap transplanted to femoral vasculature. (a) After perfusion. (b) Mounted to the intravital observation chamber (arrows in photos a, b depict vascular anastomosis site). (c, d) The flap released from the chamber after failed microscopy session because of remarkable interstitial oedema. Please note the thickened flap because of oedema (arrows)
Conclusion
Cryobiology is an exciting and promising field of medical and surgical research. For plastic surgery speciality, safe cryopreservation of vascularized composite tissue is a challenging task. Use of more sophisticated cryoprotective solutions and better cooling and thawing process seem to be the key issues for success. According to our experience anticoagulant and thrombolytic treatment combination was essential in prevention of pedicle thrombosis. Curiously we have observed exagerated flap contraction after the first week. This may be attributed to undercover microscopical tissue injury or a new phenomena.
Further studies on cryoprotectant perfusion, more refined freezing and thawing protocols are needed in order to achieve dependable cryopreservation protocols for storage of vascularized composite tissues for reconstructive purposes.
References
1.
Mobjerg N, et al. Survival in extreme environments – on the current knowledge of adaptations in tardigrades. Acta Physiol (Oxf). 2011;202(3):409–20.CrossRef
2.
3.
Salai M, Brosh T, Keller N, Perelman M, Dudkiewitz I. The effects of prolonged cryopreservation on the biomechanical properties of bone allografts: a microbiological, histological and mechanical study. Cell Tissue Bank. 2000;1:4.
4.
5.
6.
Bakhach J. Xenotransplantation of cryopreserved composite organs on the rabbit. Organogenesis. 2009;5(3):127–33.PubMedCentral




Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








