Fig. 38.1
Live bone marrow cells are shown in histological sections of fresh cadaveric mandibles of rats (hematoxylin and eosin stain, ×300)
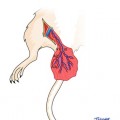
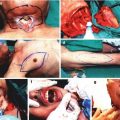
For this purpose, and to demonstrate potential of the vascular pedicle of the rat mandible, studies were performed on five fresh cadaver rats. First, the pedicle of the hemimandible was isolated. We found that when the inferior alveolar artery, which is the first branch of the internal maxillary artery, is protected, the hemimandible could be incorporated to the flap as a vascularized bone (Fig. 38.2). Further investigation in fresh rat cadavers showed that the entire composite flap could be harvested based on the common carotid artery and jugular vein. Barium sulfate (3 mL, BioTrace, Bryan Corp., Woburn, MA) injection into the pedicle of harvested flaps enabled the vascularity of the bone to be visualized. Following preliminary studies, we determined that heterotopic transfer of the hemiface/mandible/tongue flap to the inguinal region would be more appropriate.
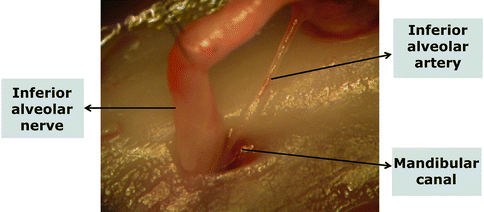

Fig. 38.2
The mandibular canal, inferior alveolar nerve, and the inferior alveolar artery are seen in the mandible of a fresh cadaveric rat under the microscope
Isotransplantation Studies of the Composite Hemiface/Mandible/Tongue Transplantation Model
Surgical Technique
After completion of preliminary anatomical studies, ten isogenic hemiface/mandible/ tongue flap transplantations were performed between Lewis (LEW) rats. As previously defined, a midline vertical incision was made in the hemiface flap. Following the midline vertical incision, the submandibular gland and sternocleidomastoid muscles were excised, and the common carotid artery and external jugular vein were revealed. Then, to obtain a better view of the external carotid artery and its branches, the digastric muscle, the omohyoid muscle, and the great horn of the hyoid bone were excised. A tracheostomy was performed to provide a safe airway. The mandible was divided into two parts at the symphysis to reach the base of the mouth and tongue. The right lingual artery pedicle was ligated, and the tongue was incorporated into the flap based on the left lingual artery pedicle. Thus, the left facial artery, superficial temporal artery, posterior auricular artery, the lingual artery, and the internal maxillary artery were preserved and incorporated into the flap.
In the occipital area, the dissection was conducted under the temporal muscle plane toward the zygomatic arch. The zygomatic arch was removed, and an orbital exenteration was performed. The external ear canal was separated from the osteocartilaginous junction, and the external ear was incorporated into the flap. One of the most difficult procedures was the dissection of vascular structures in front of the bulla. In the bulla, the side branches of the internal maxillary vein were cauterized and ligated, and the internal maxillary vein was preserved. Another difficult procedure involved the dissection of the temporomandibular joint capsule, which continued toward the base of the skull. Because there are vascular structures with large diameters in both areas of the base of the skull base, bleeding caused by carelessness and haste may cause the death of the donor rats and, thus, may render the harvesting of the flap impossible. In here, the vascular pedicle of the mandible, and the inferior alveolar artery, which is the first branch of the internal maxillary artery, were preserved.
At the level of the upper gingivobuccal sulcus, the oral mucosa was incised and dissected from the maxilla. Finally, the common carotid artery and the external jugular vein were included as a vascular pedicle, and the composite flap was harvested (Fig. 38.3a, b). The flap was transferred into the recipients’ inguinal region, and an end-to-end anastomosis was performed to the femoral artery and vein.
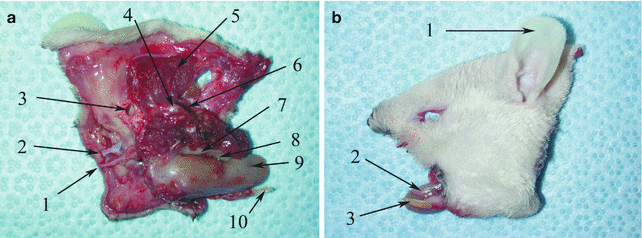

Fig. 38.3
Detailed view of the structures included in the hemiface/mandible/tongue flap harvested from isogenic Lewis rats. (a) The appearance from the inner side. 1 common carotid artery, 2 external jugular vein, 3 external auricular meatus, 4 mandibular condyle, 5 split temporalis muscle, 6 split masseter muscle, 7 oral mucosa, 8 hemimandible and teeth, 9 teeth, 10 madibular tooth. (b) The view from the outside. 1 external ear, 2 tongue, 3 mandibular tooth
The viability of the tissues constituting the flap was observed on day 45 post-transplantation. In the follow-up period, it was observed that the mandibular teeth grew and, thus, the duration of the follow-up was shortened so as to not disturb the recipient.
Histological Evaluation
Histological evaluations were made on day 100 post-transplantation in two euthanized hemiface/mandible/tongue recipients. Histological sections taken from the mandible showed the presence of live bone marrow cells. The integrity and viability of the tongue structures were observed in histologic sections. Histology of the tooth demonstrated the integrity of the tooth component of the composite flap. Skin biopsy from the composite hemiface/mandible/tongue flap on day 100 post-transplantation showed a normal epidermis and dermis, in other words, a grade 0 rejection reaction.
Radiological Evaluation
The integrity and viability of the mandibular bone (hemimandible) and mandibular teeth were observed in plain X-rays and computed tomography (CT) scans taken on the 100th day post-transplantation.
Allotransplantation Studies of the Composite Hemiface/Mandible/Tongue Transplantation Model
In the second part of the study, semi-allogenic transplantation was performed between Lewis-Brown-Norway (LBN, RT11+n) and Lewis (LEW, RT11) rats.
Surgical Technique
The previously defined skin incisions were completed, and the hemiface/mandible/tongue flap, based on the common carotid artery and external jugular vein, was harvested from the semi-allogeneic LBN donor rats (Fig. 38.4a, b). The harvested composite flaps were transferred to the inguinal region of the recipients (Fig. 38.5).
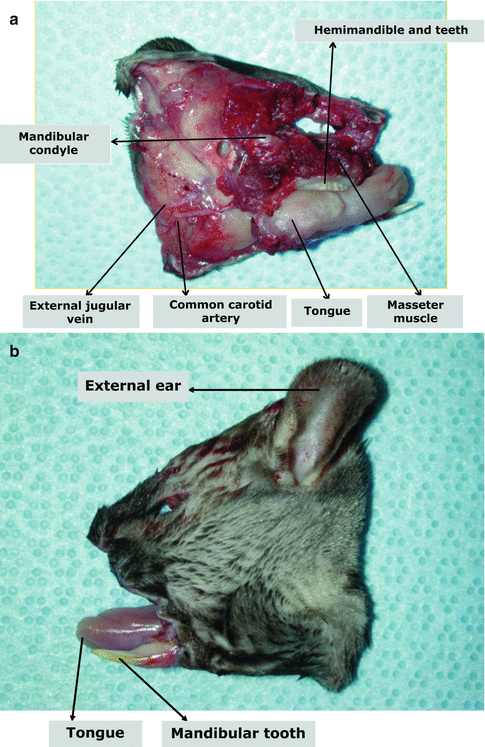
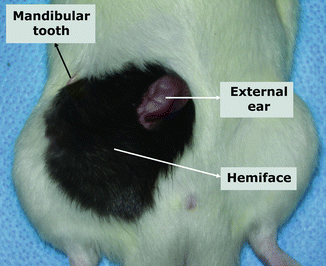

Fig. 38.4
Detailed view of the structures included in the hemiface/mandible/tongue flap harvested from semi-allogeneic Lewis Brown Norway rats. (a) The appearance from the inner side. (b) The appearance from the outside

Fig. 38.5
Appearance of a semi-allogeneic transplant 63 days after transplantation
Immunosuppressive Treatment Protocol
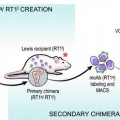
Allotransplant recipients were divided into two groups, a treatment group and a control group (rejection group). The treatment protocol was conducted as follows. In the first week, cyclosporin A (CsA) monotherapy was administered at 16 mg/kg/day. Then, the dose of CsA was reduced every week to one-half that of the previous week. In the fourth week, the dose of CsA was fixed at 2 mg/kg/day and maintained at this level thereafter. All subjects were monitored on a daily basis, and flap viability was assessed by CT and angiography. During the observation period, the chimerism level of the donor-specific antigen MHC class I (RT1n) in the peripheral blood of the Lewis recipients was evaluated by three-color flow cytometric analysis. Additionally, the presence of donor-derived cells in the recipients’ lymphoid organs and bone marrow compartments was assessed by immunohistochemistry.
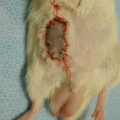
In the control group, rejection began 5–7 days after transplantation. In the treatment group, there were no signs of rejection, and, furthermore, the viability of all components of the composite tissue allograft was observed during examination on the 45th postoperative day (Fig. 38.6). The mandibular teeth in the allotransplants were growing, and, thus, there was a need to shorten the follow-up time so as to not disturb the recipients. In this group, allografts survived without any signs of rejection up to 385 days, and, at that time, the animals were sacrificed due to old age, without signs of rejection (Fig. 38.7).
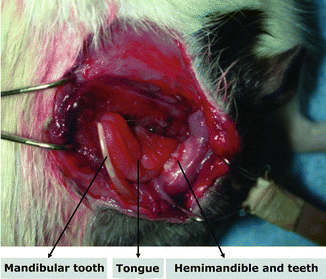





Fig. 38.6
The viability of all components of semi-allogeneic composite tissue allografts was seen 45 days after transplantation
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree