11Combination Reconstruction
Abstract
Reconstructive surgery blends the knowledge of proper techniques, a framework of when these techniques should be used, execution, foresight of the healing process, as well as vision, creativity, and the art in medicine. Planning out a proper reconstruction involves evaluating the defect, cosmetic subunits involved, tissue properties (thickness, actinic damage, appearance of pores, presence or absence of hair), anatomic landmarks and danger zones, tissue reservoir, and free margins. With experience and proper evaluation of tumors and patient selection, a potential defect and reconstructive options may be planned prior to surgery. The majority of this book has focused on an algorithm and framework for reconstruction; however, large defects, defects involving multiple subunits, and multiple defects in the same patient may require a combination of reconstructive techniques and creativity.
This chapter focuses on using reconstructive techniques like combinations of primary closures, full-thickness skin grafts and Burow’s grafts, and flaps to reconstruct large or difficult, multisubunit defects and multiple defects on patients on the same surgical day. Keys to the evaluation and management of these defects are discussed, and pearls on how to best execute these reconstructions are highlighted. A case-based approach is used to illustrate these concepts. The “Combo-Z” flap is introduced to close two defects in close proximity using a combination of flap movements. The “West by East-West” flap combination is also introduced for large or multi-subunit nasal defects including the tip, supratip, and nasal sidewall. Mastering these key principles allows for a comfort level and confidence in approaching any defect(s) and broadening the reconstructive armamentarium of early career and seasoned surgeons.
Keywords: Combination reconstruction, multiple defects, flap, graft, subunit reconstruction
Capsule Summary and Pearls
Pearls for combination reconstruction:
•Reconstruction may confirm tissue tumor clearance.
–Removing a standing tissue cone at the edge of previous positivity or inflammation.
–Taking a deeper base to help clear tumor stroma or inflammation.
•Combinations of flaps, grafts, linear repairs, and second intention healing allow for preservation of cosmetic subunits and decreasing tension of improperly designed reconstructions.
–Periocular full-thickness skin graft (FTSG) to avoid ectropion or eyelid tension.
–FTSG after cheek advancement flap for large nasal sidewall defects (see Fig. 11.5a–c).
–Second intention healing or mucosal advancement flap for mucosal lip combined with reconstruction of the cutaneous lip defect (see Fig. 11.11a–c).
•Determine if one reconstructive option may repair multiple defects while sparing normal tissue.
–Consider the “Combo-Z” flap (see Fig. 11.15a, b).
•Repair larger of multiple defects first (see Fig. 11.9a–e).
–See how tissue moves when larger defect is repaired.
–Determine the direction and repair type of remaining adjacent tissue.
–Alternating orientations of primary repairs avoids tissue pull in the same direction.
•Determine if a planned repair may remove or reorient previously displeasing scars or lesions.
–Make sure to obtain informed consent, and discuss the removal of adjacent lesions prior to doing so.
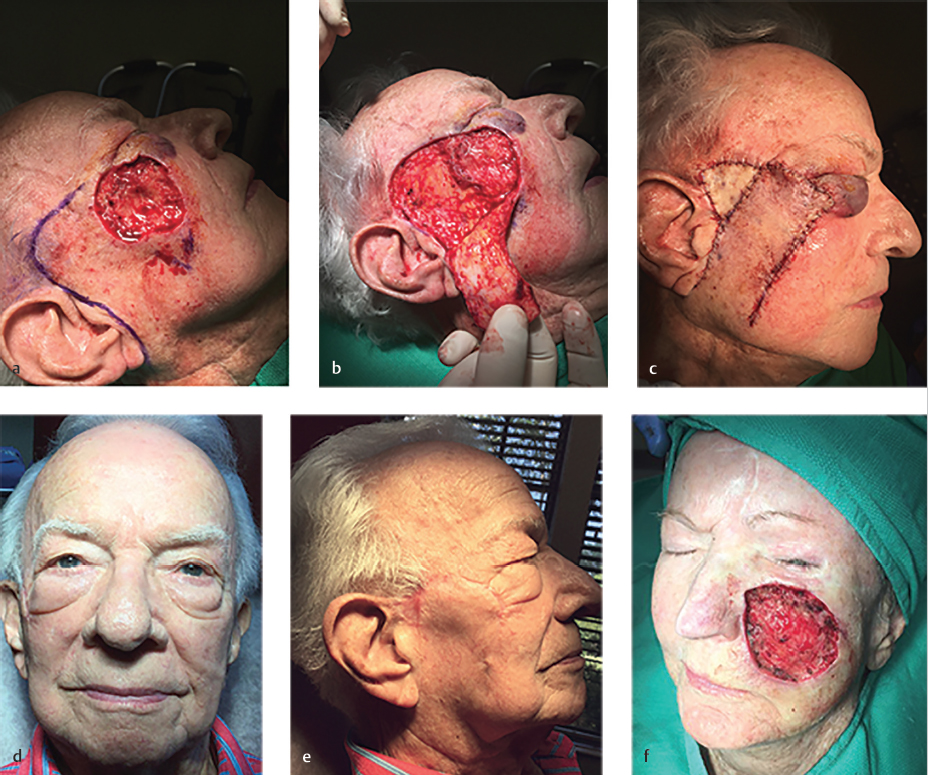
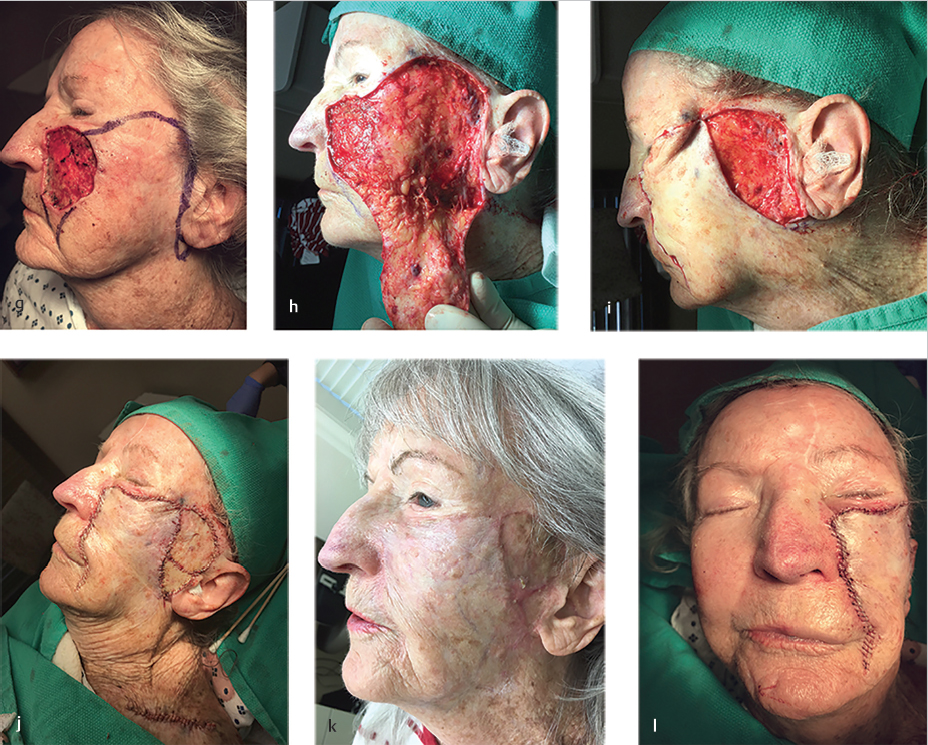
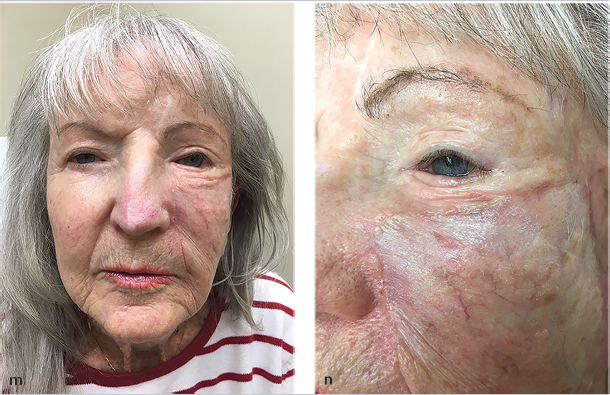
•Consider using another flap or “back-graft” to close a secondary or tertiary defect (see Fig. 11.2a–n; Fig. 11.7a–c).
–FTSG or O-T advancement flap for a secondary defect created by a forehead flap.
•Keep standing tissue cones or any excised tissue (may be used as Burow’s grafts).
•Don’t repair an area from which a graft may be taken until you determine the size of the graft needed (see Fig. 11.2c, j; Fig. 11.15f, g).
•Determine the direction of where a standing tissue cone is best removed.
–Extending a longer incision inferiorly on a cheek or preauricular area may help prevent pucker.
–Allows for reaching a tissue reservoir.
•Determine donor site properties for proper tissue match.
–Hair-bearing versus non-hair-bearing area.
○Forehead flap, cheek advancement flap, cheek rotation flap, FTSG.
–Actinic damage and pore density (preauricular vs. retroauricular vs. conchal bowl):
○Conchal bowl pore density matches the distal nose and alae.
○Retroauricular sulcus skin has less actinic damage than preauricular.
○Thin retroauricular sulcus tissue matches superficial helical or canthal defects.
○Non-hair-bearing preauricular skin matches the actinic damage and thickness of the nasal dorsum or sidewall.
–Supraclavicular skin and the inner upper arm allow for large reservoirs of free tissue.
○Supraclavicular skin typically has more actinic damage than inner arm.
•When harvesting an FTSG, trim tissue to the desired depth accounting for atrophy and metabolic demand.
–Even mild sloughing after incomplete FTSG thinning may allow a better long-term outcome than extensive immediate thinning causing a “skeletonized” appearance of the nose.
–Dermabrasion, intralesional corticosteroids, serial excisions, or scar revision can be done at a later time to improve aesthetic outcome.
•Suturing considerations.
–Create extra eversion when sewing from flap to flap (see Fig. 11.9d).
–Consider pulley sutures for key tight areas that can later be removed or left.
–Epidermal (top) pulley sutures may be used to bring adjacent tissue together over an FTSG allowing basting of the FTSG and gradual guiding contraction of the adjacent tissues (tie-over sutures) (see Fig. 11.17c, d).
–“Set in” graft or flap to surrounding tissue or base, respectively, to account for pincushioning.
○Sew from graft or flap to surrounding tissue.
○Take a more superficial bite of graft or flap and a deeper bite of the target tissue.
○Exiting the needle at the base farther from the graft allows for a better inset of the graft (especially for FTSG of the nasal ala).
11.1 Introduction
Patients with cutaneous malignancies often have multiple lesions requiring treatment. Single-site surgery is most common; however, the following reasons may lead to treatment of several tumors in a single day: patient preference, difficulty traveling for treatment, and multiple tumors in one cosmetic subunit or anatomic area which would encroach on a potential reconstruction. Treating more than one tumor at a surgical visit allows “cleaning up” the tumor burden on a patient analogous to field therapy treating actinic keratoses. To spare normal tissue, a combination reconstruction or using one reconstruction for multiple defects may be chosen.1,2,3
Inaccurate estimation of tissue laxity and reservoir can hinder a planned reconstruction and create aesthetically or functionally unsuitable results. This is often seen when overestimating the mobility of inherently tight forehead tissue, working in a scar, or approaching a free margin. Sometimes, a well-designed flap fails to close the defect. Even seasoned surgeons have elevated a large flap and realized it just won’t reach. In these cases, a comfort level with combination reconstructive techniques may improve outcomes.
11.2 Combination of Primary and Graft Reconstruction
As primary or linear repairs are commonly used reconstructive options, they should be the first reconstructive consideration after second intention. While the 3:1 length-to-width ratio of elliptical excisions with 30-degree angles of the standing tissue cones is frequently used, certain anatomic sites allow for lengthening or shortening of this ratio and widening or “cheating” the vertex angle of the standing tissue cones. For example, the hairless triangle of the lip, the medial canthus, and the back often allows for shortening of the excision and widening the vertex angle. However, ellipses on the nasal dorsum and columella, the scalp, the vermilion lip, and the helical rim are often extended past the 3:1 ratio, with angles that are even more acute, in order to lengthen the incision over a curved surface for a smooth transition and avoid a pucker.
In combination reconstruction, this extension of an ellipse allows for harvesting a graft without creating a new incision. Burow’s grafts are full-thickness skin grafts (FTSG) obtained from adjacent tissue from a standing cone of a primary repair, allowing for a better color, thickness, and texture match when used for adjacent tissue reconstruction.4–7 Traditionally, they are used on the nasal dorsum or tip with the proximal nose closed primarily providing the grafted tissue distally.8,9 However, they can be used in almost any location. In addition, FTSG from other locations can be used in combination with primary repairs.
The key points of using Burow’s grafts or FTSG in combination with primary reconstructions are:
1.Determine the appropriate tissue properties for the graft site.
2.Determine if the reservoir available in the standing tissue cone is sufficient for the defect after accounting for partial closure of the defect with a primary reconstruction.
3.If a unilateral or bilateral Burow’s grafts do not allow for sufficient tissue, FTSG may be harvested from a matching tissue reservoir (retroauricular, preauricular, conchal bowl, supraclavicular, inner arm, and femoral canal) depending on the amount of tissue needed.
4.Don’t discard tissue until the reconstruction is finished.
5.Don’t harvest the graft until you determine the area needed to be grafted.
6.Extend the primary repair from which a Burow’s graft may be harvested where an extended incision may best heal (inferior curvature of the cheek as opposed to zygoma, proximal nasal dorsum as opposed to distal nose).8,9
7.Consider tissue match (thickness, color, texture, hair density, pore density).
8.Suturing from graft to the surrounding base and “setting in” the graft helps limit pincushioning.
Anatomic examples will be discussed in the following text.
11.2.1 Arm/Hand
The dorsal hand or large forearm defects are great for FTSG/primary repair combinations. While granulation, purse string repairs, single arm rotation flaps, O-Z double rotation flaps, and the “Mercedes” flap are used in these locations, Burow’s grafts offer an acceptable reconstruction, especially on tight and often atrophic skin.10 If the defect is too large to use a Burow’s graft without significant tension, it may be prudent to repair much of the defect primarily and use a supraclavicular or axillary upper arm FTSG to close the remaining part of the defect.
11.2.2 Temple
Horizontally and vertically oriented primary repairs, rotation flaps, and advancement flaps are typically used to reconstruct the temple. While FTSG of the forehead often lead to an atrophic appearance, Burow’s grafts of the temple and lateral suprabrow offer an acceptable repair option (Fig. 11.1a–c).
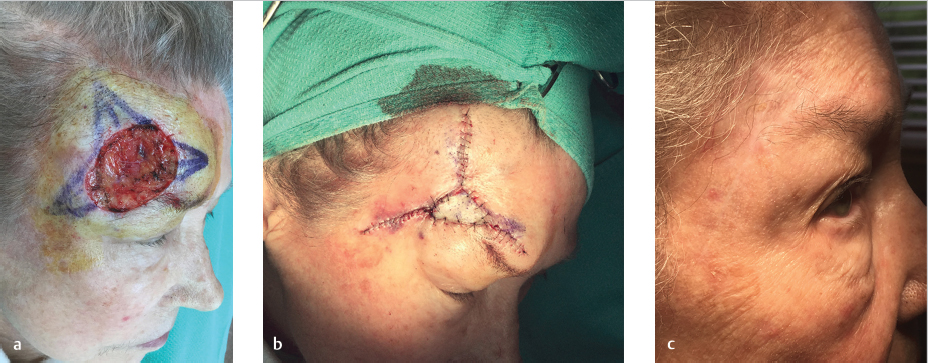
Fig. 11.1 Combinations of full-thickness skin graft (FTSG) and primary linear repairs of the forehead/temple. (a) Defect involving the lateral eyebrow, lateral forehead, and lower temple. (b) Burow’s graft and primary repairs bilaterally and superiorly causing slight elevation of the brow. This is often called a “Mercedes” flap when a Burow’s graft isn’t used. The brow elevation settles back to baseline within weeks to months of the repair. (c) Four-month follow-up with settling of the eyebrow and continued fading of the FTSG.
11.2.3 Cheek
11.3 Combination of Flap and Graft Reconstruction
As we approach defects with regard to subunits involved and wound tension, a flap may be the reconstructive choice. If the flap is unable to appropriately repair the entire defect, a graft may be used in combination. Donor sites for grafts are discussed in other chapters and earlier in this chapter. Below are some specific examples of flap and graft combination reconstruction.
11.3.1 Lateral Infraocular Cheek
The bilobed transposition and rotation flaps, such as the Mustarde cheek rotation flap, are used to close large infraocular defects. However, this cheek rotation flap is difficult to execute with the goal of avoiding any tension on the lower eyelid and preventing an ectropion. Keys to this flap include oversizing the flap (especially in the temple area), tacking the flap superolaterally from the lateral canthus with sutures to the taught temporal skin in the vertical vector or the orbital rim, and tacking the anterior edge of the flap in a horizontal direction to the medial portion of the defect or the nasal sidewall in order to avoid tension to the eyelid itself. However, if the cheek defect is large and too lateral to allow the secondary defect of the flap to be sewn out, other modifications must be made (Fig. 11.2a). Even with a maximum amount of tissue rotated starting immediately preauricularly and stretching superiorly to the lateral temple, the secondary defect may be too large. An FTSG may be taken out inferiorly from the flap standing tissue cone and purposely sized to close the secondary defect. The keys to the flap are similar to those previously discussed; however, an inferior tissue cone should not be removed until the secondary defect is maximally closed without giving too much pull to the flap or the lower eyelid. Subsequently, a template may be made of the remaining secondary defect and used to outline the area of the inferior standing tissue cone (Fig. 11.2b). This can then be sewn in to close the secondary defect without greatly changing the tissue vectors of the flap (Fig. 11.2c–e). In the case of medial or extremely large defects, a wider rotational arc maximizing the preauricular cheek availability and additional FTSGs may be needed (Fig. 11.2f–n).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree