and Emir Q. Haxhija2
(1)
Department of Plastic Surgery and Burns, Institute for Mother and Child Health Care of Republic Serbia, University of Belgrade, New Belgrade, Serbia
(2)
Department of Pediatric and Adolescent Surgery, Medical University Graz, Graz, Austria
Keywords
Cleft lip and palateChildrenTreatment7.1 Introduction
Cleft lip and palate are the most common congenital craniofacial anomalies [1, 2]. Cleft lip (CL), cleft palate (CP), and cleft lip and palate (CLP) constitute a heterogenous group of birth defects with multifactorial origin [1]. Cleft care requires closely allied reconstructive and cosmetic principles, applied by a plastic surgeon as a member of a collaborative multidisciplinary team [3–8]. Major advances in the care of children born with CLP occurred in the last three decades, and there is a tendency for cleft care centralization [4].
7.2 Embryology
Primary palate develops from 4 to 8 gestational weeks (GW) and secondary palate develops from 5 to 12 GW [2, 9, 10]. Although they often occur together, they have different embryonic origins [2, 6, 7, 11]. Medial nasal, lateral nasal, and maxillary processes are involved in the formation of primary palate, and any failure of fusion will give a rise to the cleft of the lip, alveolus, and hard palate to the incisive foramen on one or both sides [6, 9–11]. The secondary palate develops from the paired lateral palatine processes [2, 10, 11]. This shelf-like mesodermal projections are fused together from anterior to posterior, after the tongue is moved inferiorly [7, 11]. If the shelves do not fuse (as a result of defective growth, failure to rise above the tongue, or there is a rupture after fusion), cleft palate occurs [2, 7].
7.3 Cleft Anatomy
Normal lip anatomy is a reconstructive goal [6]. The lip surface is divided into cutaneous, dry vermilion, and vet vermilion part, and superior to the upper lip in central position is the nose with philtrum lying between these two [6, 10, 12]. Deep to the skin is the orbicularis oris muscle (OOM) which is striated and it encircles the mouth [6, 10]. The palate consists of anterior bony (hard) palate covered with mucoperiosteal lining, and posterior muscular (soft) palate, with foramen incisivum that delimits primary from secondary palate [6, 11, 13]. Soft palate muscles (m. levator veli palatini and m. tensor veli palatini as most important) are involved in speech, swallowing, and hearing [6, 11, 13–15].
In unilateral CL, lip is short on medial side, philtral column is flattened, and vermilion is narrow [10, 12]. On lateral side vermilion border and red line converge as they approach to cleft, with the deficiency of OOM and misdirection to the alar base and columella [5, 6, 10, 12, 13]. The nasal floor, alveolus, and palate can also be involved [10, 12].
In bilateral CL, the prolabium and premaxilla remain entirely separated from the lateral lip and maxillary arch elements [1, 5, 6, 13]. The cutaneous roll of prolabium is of poor quality, the height of vermilion is inadequate, labial sulcus is shallow, there is lack of OOM, and the lateral elements are similar to lateral elements of unilateral cleft [1, 13].
Unilateral complete CLP is characterized by direct communication between the entire length of the nasal passage and oropharynx (there is a full thickeness palatal defect of nasal mucosa, bony palate, velar musculature, and oral mucosa), and the nasal septum is deviated and buckled toward the cleft side (in bilateral cleft palate vomer remains free of attachments to the palatal shelves) [1, 11, 13]. Isolated cleft palate can occur as an opening in the posterior soft palate to a cleft extending up to the incisive foramen, and in submucous cleft palate, there is underlying levator palatine muscle discontinuity with triad of symptoms midline clear zone (zona pellucida), bifid uvula, and a palpable notch in the posterior hard palate [1, 11].
7.4 Epidemiology
The overall incidence of CLP is 1/700 [2, 4, 6, 8, 15]. Isolated cleft palate has an overall incidence of 0.4–0.5 per 1000 live births [1, 2, 4, 16]. The most common diagnosis is CL/P, followed by isolated cleft palate and then isolated cleft lip [2, 6]. Unilateral clefts are nine times as common as bilateral clefts, the left side is more often involved than right side, and the majority of bilateral and unilateral cleft lips are associated with a cleft palate [1, 2, 6]. Males are predominant in the CL/P population and females in isolated CP [2, 6].
7.5 Etiology
Both environmental (phenytoin, thalidomide, retinoic acid, maternal cigarette smoking, alcohol use) and genetic factors are involved in the genesis of cleft lip and palate [1, 2, 6, 15]. Gender differences (palate develops 1 week later in males), low socioeconomic status, parents’ age, as well as maternal obesity play a role in clefting [1, 2, 6].
Clefts are classified as non-syndromic (without other physical or developmental anomalies, and known teratogenic exposures) and syndromic [2, 15, 16]. Isolated CP is most commonly a part of the syndromes compared to all cleft types (in 50% of all cases) [1, 2, 6].
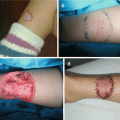
There are more than 350 Mendelian disorders associated with CLP (Van der Woude, Treacher-Collins, Waardenburg, Apert’s, Stickler’s, Carey-Fineman-Ziter, velocardiofacial syndrome, Pierre Robin sequence, etc.) (Fig. 7.1) [1, 2, 6, 10, 11].


Fig. 7.1
Syndromic cleft palate: (a) Pierre Robin syndrome; (b) Van der Woude syndrome (lower lip pits); (c) Möbius syndrome; (d) Apert’s syndrome
7.6 Diagnosis
Prenatal diagnosis of CL by ultrasound (US) is possible in more than 70% of cases [17, 18]. This is very important to establish because the birth of a child with cleft is a very large stress for unprepared parents, and it allows early preparation of the family [4, 8, 16–18]. The mean gestational age at detection of CL reported by some authors is 25.5 weeks [6].
Neonatologist or pediatrician has to be available at the time of the delivery (patients with clefts are in most cases already seen by pediatricians after the delivery and sent to the surgeon) [6, 8]. After cleft evaluation, complete examination of the oral cavity and entire body has to be performed (to exclude associated anomalies) [1, 8]. Instructions and assistance should be given to the parents regarding the feeding issues [8]. After birth, genetic counseling for the parents may be beneficial, and the child with CL and/or CP should be sent to regional cleft center [1, 3, 4, 8]. Parents are usually very upset and even angry with plethora of questions regarding etiology, care, and surgical treatment of their child [4, 6].
7.7 Surgical Evaluation and Classification
Clefts are typically divided into four groups: cleft of primary palate (unilateral, bilateral, total, or subtotal), cleft of secondary palate (total, subtotal, and submucosal), cleft of primary and secondary palate (unilateral, bilateral, total, or subtotal), and rare facial cleft [1, 6, 16].
Kernahan proposed a system to classify cleft lip and palate with the incisive foramen as central landmark and Y-shaped diagram (upper limbs represent primary palate and lower limb represent hard and soft palate) [1, 10, 16]. This classification is modified by adding numbers for more precise description [17]. Otto Kriens proposed a system that used letters to present components [1, 10]. The acronym LAHSHAL denotes the bilateral anatomy of the lip (L), alveolus (A), hard (H), and soft (S) palates, by convention from right to left [1, 10, 16]. Small letters represent incomplete clefts of the structure, and a period denotes no cleft [1, 10]. Clefts also can be recorded by letter codes (R, right; L, left; P, primary; S, secondary; C, complete, I, incomplete) [16].
There are several types of unilateral CL: unilateral incomplete clefts have in common an intact nasal sill, or Simonart band, and unilateral complete clefts are characterized by disruption of the lip, nostril sill, and alveolus (complete primary palate), and there is a group of unilateral CL named lesser-form clefts with three anatomical categories (minor-form, microform, mini-microform clefts) (Fig. 7.2a–e) [1, 10, 16, 19].
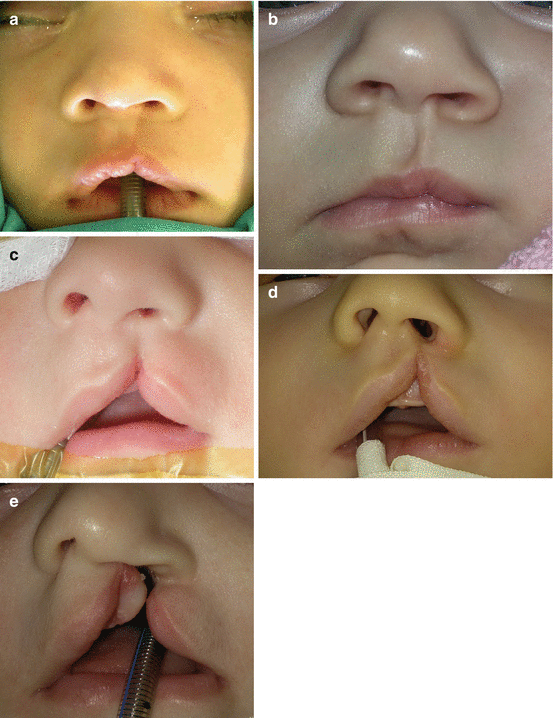

Fig. 7.2
Different types of unilateral cleft lip: (a) microform cleft lip; (b) mini-microform cleft lip; (c) minor form cleft lip; (d) unilateral incomplete cleft lip; (e) unilateral complete cleft lip
In incomplete bilateral primary clefts, there is a near-normal nose, a normally positioned premaxilla, and clefts involving only the lip, and in complete bilateral primary cleft, the protruding premaxilla with lateral palatal shelves is collapsed toward the midline (Fig. 7.3a–c) [1, 5].
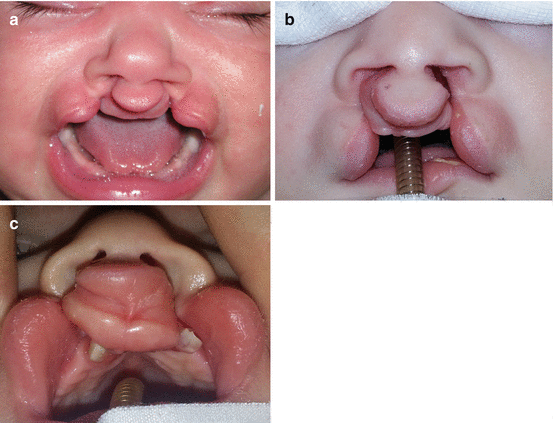

Fig. 7.3
Bilateral cleft lip: (a) incomplete bilateral cleft lip; (b) complete bilateral cleft lip; (c) complete isolated bilateral cleft of primary palate
Unilateral complete clefts are characterized by disruption of the lip, nostril sill, and alveolus, hard and soft palates [1, 10]. Small group of patient with complete unilateral or bilateral CLP has nasolabiomaxillary hypoplasia and orbital hypertelorism, and they are named binderoid CLP [20].
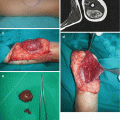
Isolated cleft palate can be unilateral, bilateral, and medial (total or subtotal) (Fig. 7.4a, b) [1, 7, 11]. Pierre Robin sequence includes micrognathia, glossoptosis, and airway obstruction, typically associated with wide U-shaped cleft palate in up to 73–90% of cases (Fig. 7.5) [11, 21]. Patients with submucous cleft palate are in generally asymptomatic, although approximately 15% will develop velopharyngeal insufficiency (VPI) (Fig. 7.6) [1, 6, 11].
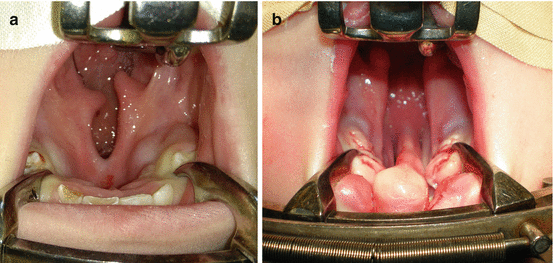
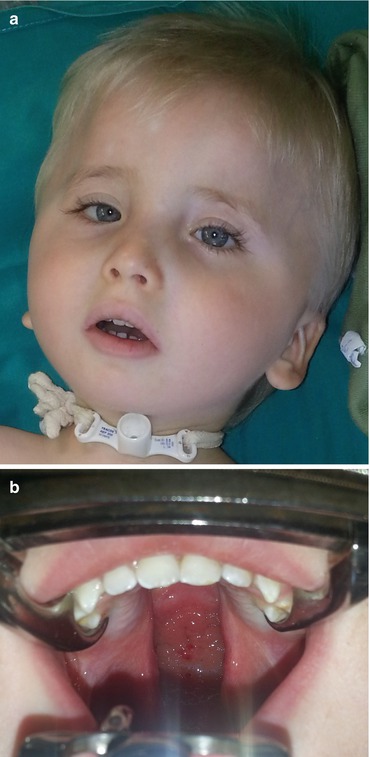
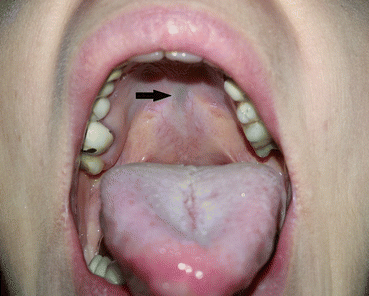

Fig. 7.4
Cleft palate types: (a) incomplete cleft palate; (b) complete cleft palate

Fig. 7.5
Pierre Robin syndrome: (a) tracheostomy performed because of airway problems; (b) cleft palate of the same child

Fig. 7.6
Submucosal cleft palate (zona pellucida)
7.8 Treatment of Cleft Patients
Goals of treatment for patients with clefts include generally: feeding counseling, surgical treatment, hearing and speech evaluation, orthodontic treatment, and additional surgical treatment [1, 8, 11, 13, 18].
7.8.1 Feeding
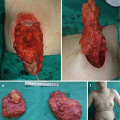
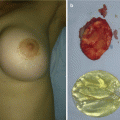
Most infants with CP are unable to breast feed because they cannot generate intraoral vacuum, and food may reflux into the nasal passage (Fig. 7.7) [7, 8, 11]. There are proper feeding techniques with the upright position (30°–45°) with special devices, bottles, and nipples (with enlarged hole) made to make low resistance to flow [7, 11]. When surgery on palate is performed and the palate is closed, there is no need for special feeding methods [11].
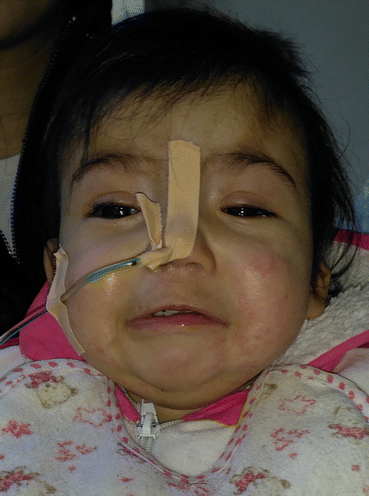

Fig. 7.7
Nasogastric feeding tube left in place by child’s mother for 10 months without any visit to a hospital or outpatient clinic (low socioeconomic status)
7.8.2 Presurgical Nasoalveolar Molding
Presurgical infant orthopedics (PSIO) is classified as passive which include using of alveolar molding plate (Liu’s and Grayson’s method) and active (Latham pinned coaxial screw appliance) which requires a surgical procedure to introduce the device and to remove it [1, 6, 7, 10, 13, 16, 22]. Gingivoperiosteoplasty (GPP) is a procedure used for correction of the cleft alveolar segments at the time of cleft lip repair [5, 13]. There are concerns about influences of PSIO and GPP on maxillary growth [1, 10, 22]. Lip adhesion can also reduce the gap of alveolar segments by 60% [6, 10, 16, 22].
Objectives of presurgical nasal and alveolar molding (PNAM) are active molding and repositioning of the nasal cartilages and alveolar processes and lengthening of the deficient columella [1, 5, 10, 22]. PNAM is applied both to the patients with unilateral and bilateral clefts in most cases during 6 weeks after birth [1, 22].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree