and Emir Q. Haxhija2
(1)
Department of Plastic Surgery and Burns, Institute for Mother and Child Health Care of Republic Serbia, University of Belgrade, New Belgrade, Serbia
(2)
Department of Pediatric and Adolescent Surgery, Medical University Graz, Graz, Austria
Keywords
BreastCongenital deformitiesChildren5.1 Introduction
Breast anomalies in pediatric population are common and they can have a significant psychological effect on teenage and adolescent girls (especially during breast development) [1–5]. Mammary pathology is very often a reason for consultation in medical practice [3]. The spectrum of breast disorders in pediatric population is different from that in adults, with significant physiological impact on patients and parents [1, 3–5]. Even most of pediatric breast lesions are benign, we have to think about malignancies [1, 2, 5, 6]. There is lack of comprehensive categorization of these abnormalities [1, 2].
5.2 Embryology
Breast development begins during the sixth week of gestation [1, 5, 7]. The breast originates from the ectoderm, along the milk line from the primitive axilla to the primitive groin [1, 5, 7–9]. By the tenth week, the upper and lower part of ridge disappears and the normal breast develops on the anterolateral chest wall [1, 7, 9]. The areola develops at the fifth month of gestation [7]. The average age of female thelarche (when the breast growth begins) is approximately 11 years of age (range from 8 to 15 years) [5, 8, 9]. Typically, breast growth is complete between 16 and 18 years [7, 9].
5.3 Anatomy
The glandular tissue of the breast (with significant amount of adipose tissue) is fixed in place by the superficial fascial system [10, 11]. The Cooper’s ligaments provide interconnections between the deep and superficial fascial layers [4, 10, 11]. The breast overlies the anterolateral thorax principally the second through sixth ribs, with the nipple areola complex as the primary landmark of the breast [1, 4, 10, 11].
5.4 Diagnosis
Evaluation of breast-related symptoms in children begins with a thorough history (regarding menstrual history for adolescent and family history of similar problems, and other breast diseases) and physical examination [12, 13]. During physical examination (which is performed with maximal care) besides the breast evaluation, any pre-existing asymmetries, spinal curvature, or chest wall deformities should be recognized and noted [10, 12, 13]. Breast sonography is generally the primary imaging modality used in pediatric population [1, 5, 6, 12]. Magnetic resonance imaging (MRI) of the breast is rarely used in children, likewise open biopsy and fine needle aspiration biopsy (FNAB), while mammography has practically no use in pediatric patients [5, 6, 12, 13].
5.5 Classification
There is no adequate categorization of breast abnormalities in pediatric population [1, 2]. Breast anomalies can be roughly classified into four groups: hyperplasia, hypoplasia, asymmetry, and deformation [1, 2, 7, 9].
5.5.1 Breast Hyperplasia
There are several possible causes of breast hyperplasia in pediatric population such as premature thelarche, juvenile hypertrophy-macromasty, polythelia, polymasty, benign tumors (fibroadenoma, vascular anomalies), malignant tumors (breast carcinoma, phyllodes tumor, metastatic disease), non-tumorous masses (cysts, galactocele), and gynecomasty (Figs. 5.1, 5.2, 5.3) [2, 6, 13].
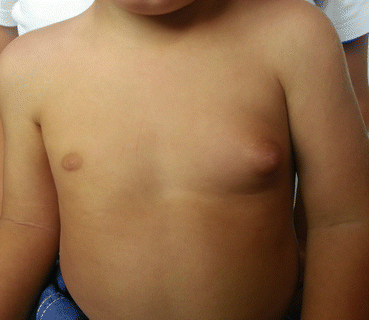
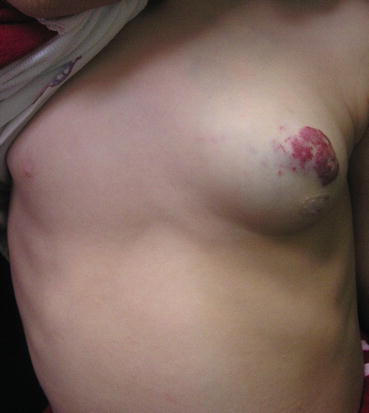
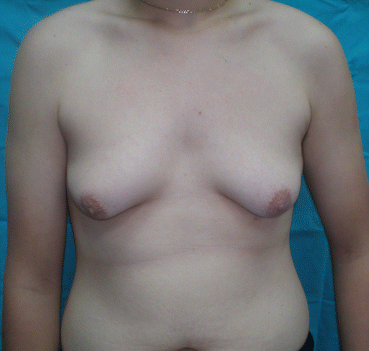

Fig. 5.1
Galactocele of the left breast

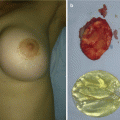
Fig. 5.2
Hemangioma of the left breast

Fig. 5.3
Clinical appearance of bilateral gynecomastia
5.5.1.1 Premature Thelarche and Precocious Puberty
Premature thelarche presents as enlargement of one or both breasts from 6 months to 9 years of age and it occurs without other evidence of precocious puberty [4, 6]. Precocious puberty implies premature breast development in association with other secondary sex characteristics (only 18% of girls with premature thelarche develops precocious puberty) [4, 6, 14]. For premature thelarche, biopsy is contraindicated since it is a benign and self-limited condition, and reevaluation is indicated every 6–12 months [6, 14].
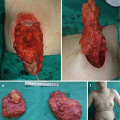
5.5.1.2 Gigantomastia (Virginal Hypertrophy)
Virginal hypertrophy is massive enlargement of breast with patients generally aged 11–16 years when the growth begins [1–4]. It is an uncommon primary condition with high sensitivity to estrogens as possible etiological factor [1]. Excessively large breast in a teenager can cause physical problem, such as pain and skin maceration, along with a psychological problem [15, 16]. Treatment of virginal hypertrophy is surgical (in most cases breast reduction with free nipple grafts, or mastectomy), with adjunct medical therapy (medroxyprogesterone, dydrogesterone, tamoxifen) to prevent regrowth after reduction mammoplasty [1, 3, 4, 13]. Psychologist and psychiatrist consultations are also needed [1]. Reduction mammaplasty is rarely performed in pediatric population (with similar indication as in adults) [10, 13, 15–21]. Surgery should be delayed, whenever it is possible, until the end of puberty because of continued breast growth [1, 2, 4, 7, 15, 21]. There are two important decisions in breast reduction surgery: choice of incision and choice of pedicle type, and breast amputation with free nipple graft remains as an alternative to breast reduction with nipple-bearing pedicle [15–21].
Mammary ptosis is a rare entity in pediatric population. The Regnault classification system for mammary ptosis describes mild, moderate, severe, and pseudoptosis according to the relative positions of the nipple and the inframammary fold [10, 16, 18, 22]. Mastopexy is a procedure designed to elevate breast tissue and the nipple areola complex to correct breast ptosis with several techniques involved (inverted-T mastopexy, concentric mastopexy procedures, periareolar “round-block” mastopexy, and vertical-incision mastopexy) used with different success and frequently combined with breast augmentation [16, 18, 22].
5.5.1.3 Polymastia
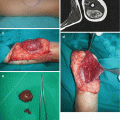
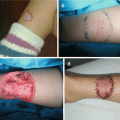
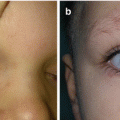
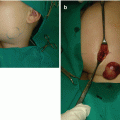
Polymastia is the presence of the supernumerary breast, usually manifested at puberty when hormonal influence started with an incidence of 1–2% of all live births [1–4, 9]. It is typically located along the primitive milk line (most commonly in the axilla) (Fig. 5.4a–d) [1, 4, 7]. When it is located outside of the mammary line, it is called ectopic mamma (Fig. 5.5a–c) [1, 3]. Since it is a subject to the same pathology as normally located breast tissue, complete resection is recommended [1–4].
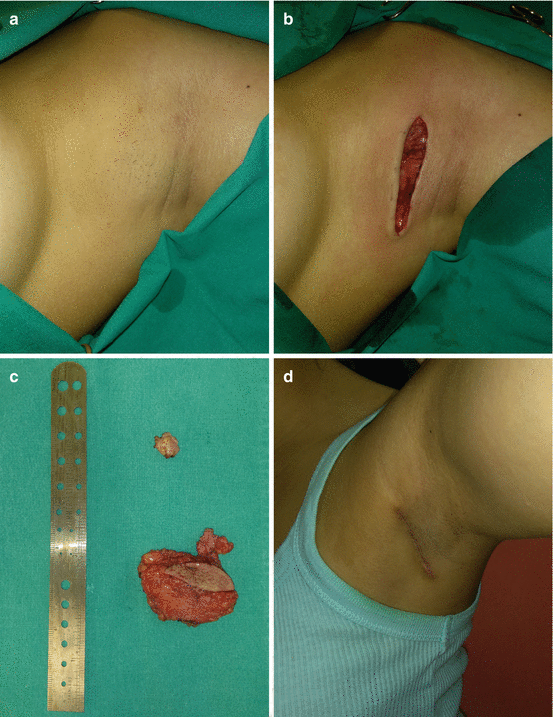
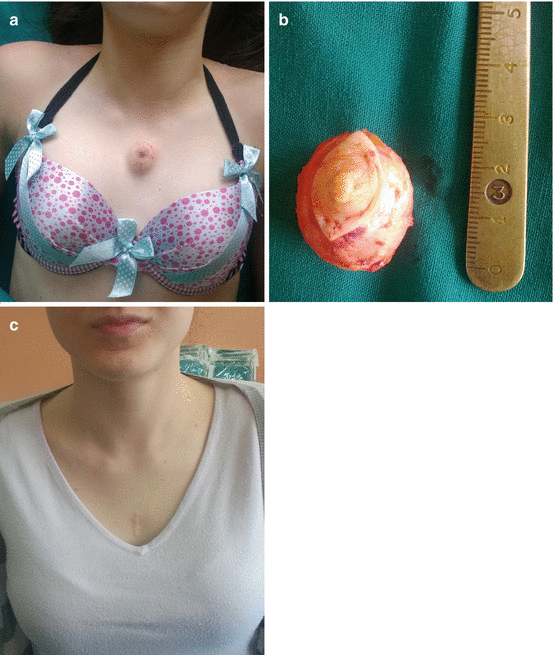

Fig. 5.4
Polymastia: (a) lesion in the left axillary region; (b) intraoperative view; (c) excised lesion; (d) 1 month after excision

Fig. 5.5
Ectopic breast at sternal region: (a) preoperative appearance; (b) excised lesion; (c) postoperative hypertrophic scar at sternal region
5.5.1.4 Polythelia
Polythelia (supernumerary nipple) is a benign, most commonly encountered pediatric breast anomaly [1, 2, 4, 7, 9]. The incidence is 1–3%, and there is a male predominance [1, 7, 9]. It results from the failure of mammary ridge to regress in utero, but it can be located out of the mammary ridge also [1, 13]. If it is associated with polymastia, it is generally recognized at birth, and as a sole entity, polythelia is often unrecognized until the puberty (often misdiagnosis for nevi) [1]. Associated renal anomalies should be evaluated (physical exam, urinalysis, and renal ultrasound (US)) [1, 2, 4]. Excision is mostly because of surgery (Fig. 5.6a, b) [1, 2, 4, 7].
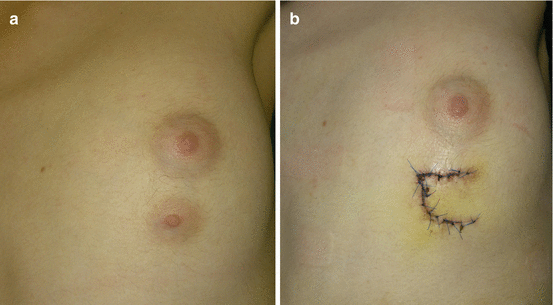

Fig. 5.6
Polythelia: (a) left female breast polythelia; (b) excision and reconstruction with local flap
5.5.2 Breast Masses
In neonatal and prepubertal period, there is often a palpable breast mass, in one or both breasts, in either sex, that typically resolves spontaneously in a few months [4]. Benign breast masses include fibroadenoma, phyllodes tumors, and fibrocystic disease (non-tumorous mass) [4, 13]. Adolescent breasts are typically fibrous with small lumps and cysts present through the breast [3, 13]. Biopsy of the prepubertal breasts is rarely indicated [4]. Firm support, analgesics, and reassurance are treatment options [3, 13]. Simple fibroadenoma is the most common breast lesion in adolescent females (91% of solid breast masses in girls under 19 years) (Fig. 5.7a, b) [4, 6, 13]. It is benign, nontender mass that grows as the result of tissue hypersensitivity to normal levels of gonadal hormones [1, 7, 9]. In 75% common fibroadenoma is presented as single lesion, the diagnosis is made by physical examination and ultrasound (US), and most of them can be observed safely [4, 13]. For patients with giant fibroadenoma (greater than 5 cm in size), complex fibroadenomas, positive family history, or associated proliferative disease, excision is recommended (increased risk of breast Ca) [2, 3, 6, 7, 9, 13]. Vascular anomalies, if located in the breast, can cause breast hypertrophy (they can be ruled out with US and MRI) [4, 6].
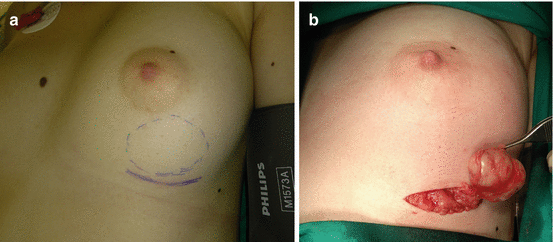

Fig. 5.7




Left breast fibroadenoma: (a) preoperative view; (b) complete excision of the tumor
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree