Chapter 53 FUTURE PERSPECTIVES IN SKIN REJUVENATION BY FAT GRAFTING: A CLINICAL AND HISTOLOGIC DEMONSTRATION
This book has demonstrated that fat serves not only as a filler for correcting body contour, but it also plays an important role in tissue regeneration, improving function, as in the management of Dupuytren disease, velopharyngeal incompetence, vocal fold paralysis, scar remodeling, and other conditions and in treating tissue damage from radiotherapy, scleroderma, difficult wounds, reconstructing radiated breasts, and more.
For centuries adipose tissue has been considered a high-energy reservoir, typically involved in homeostasis because of its ability to bind large amounts of fluids, and with insulating properties designated to the maintenance of thermoregulation.
In 2000, 1 it was discovered that adipose tissue is the greatest source of adult mesenchymal stem cells and adipose-derived stem cells (ADSCs), which are capable of differentiating into other types of tissues such as bone, muscle, cartilage, muscle, nerve, and blood vessels. This confirmation has changed the attitude among previously skeptical surgeons regarding the benefits of fat grafting. The presence of the stromal vascular fraction (SVF) in the lipoaspirate, as well as progenitor cells, T cells, B cells, mast cells, and adipose tissue macrophages, and the repair and regenerative potential obtained from injections of the purified lipoaspirate, has led to significantly increased scientific interest in the applications for fat grafting.
Previously, closure of a skin defect was typically achieved by transferring a tissue excised from another area of the body using flaps or skin grafts. While this can produce an effective correction, it involves damaging an intact area to repair another. We think that in the not too distant future, structural fat grafting will play a primary role in reconstructive surgery, facilitating wound closure, improving scar contractures, reducing the postmastectomy pain syndrome, augmenting the breast, and other applications, with a minimally invasive type of approach that takes advantage of the regenerative potential offered by fat grafting.
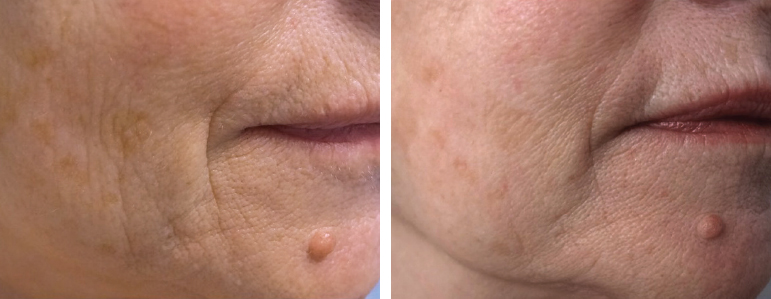
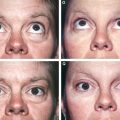
Note the antiaging effect after structural fat grafting in the subdermal layer in this patient, seen before and 1 year after fat grafting.
At this point a key consideration may arise. It has been definitively demonstrated that the regenerative potential of fat has the capability of not only correcting soft tissue defects, but also rejuvenating the skin. What are the most important activities related to this process: Adipose tissue regeneration? Modification of fibrosis? Enhancement of neovascularization? Anything else?
Material and Methods
To demonstrate the antiaging treatment of facial skin by fat graft and ADSCs, we undertook the following clinical study in patients who were candidates for facelift. 1 It was our goal to analyze the following:
The histologic and ultrastructural changes of the aged skin after the injection of fat or expanded MSCs (mesenchymal stem cells), with its stromal vascular fraction
The structural differences, by comparing specimens before and after injection of fat or expanded MSCs
The subcutaneous connective tissue, to establish whether this represents a good clinical model with which to study the related effects of the antiaging mechanism
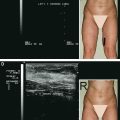
The study consisted of harvesting fat by liposuction (20 cc) and excising a piece of skin from the left preauricular area. This tissue specimen represented the baseline/control model. It was sent to the Human Anatomy Laboratory of the University of Verona (Italy) and to the Federal University of Rio de Janeiro (Brazil) for morphologic analysis by optical and electron microscopy.
The harvested fat was divided into two parts: part 1 was immediately injected in the left preauricular area, far from the wound of the previously harvested specimen, whereas part 2 was sent to the laboratory for the expansion of stem cells. After 5 weeks, the expanded cells were contralaterally injected in the preauricular area.
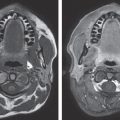
Three months after treatment with fat injection and with expanded MSCs, a second biopsy was taken concurrent with a facelift procedure. Control samples were compared with specimens obtained after treatment or with the expanded ADSCs. Surprisingly, the angiogenic effect was similar in both specimens, whether treated with fat and/or with MSCs.
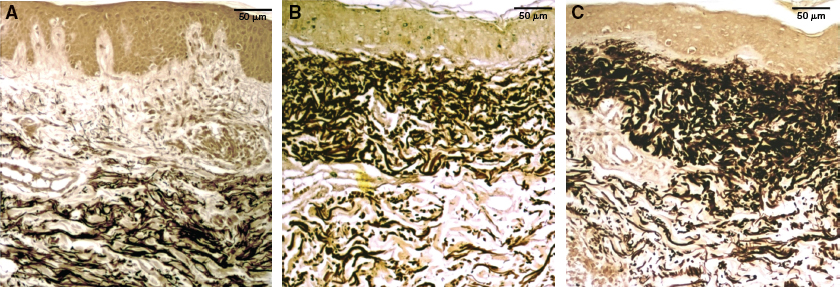
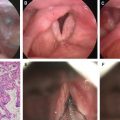
Orcein stained skin is shown before treatment (A), after treatment with expanded MSCs (B), and after treatment with fat and SVF (C). After both treatments, the increment of elastic fibers, stained in black and localized in the superficial layer of dermis, is detectable. In contrast, the elastic fibers are scarce in the deep layer of dermis.
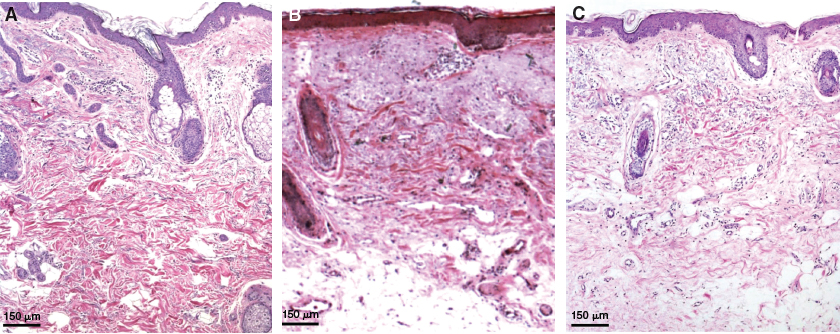
Hematoxylin and eosin (H&E) stained skin is shown before treatment (A), after treatment with expanded MSCs (B), and after treatment with fat and SVF (C). After both treatments, the presence of vessels can be seen in the area of dermohypodermic junction.
It is interesting to note that before treatment, skin showed evidence of elastosis, associated with a decrease in “new elastic fibers,” which has been termed the oxytalan fiber formation, whereas after treatment with expanded MSCs, a significant decrease in presence of elastosis was noticed, along with a significant increase in oxytalan fiber formation in the papillary dermis. In other terms, an important production of new elastic fibers was detectable at optical and electron microscopy. The same result was obtained after treatment with fat.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree