Chapter 25 STRUCTURAL FAT GRAFTING IN THE NOSE
The idea of adjusting facial proportion by infiltration of the subcutaneous tissues has been entertained since the earliest days of modern aesthetic surgery. The injection of paraffin and Vaseline for altering the contours of the nose was extremely popular 100 years ago. In 1911 Fredrick Kolle 1 created a detailed classification of deformities of the nose for the purpose of systematizing subcutaneous injections of paraffin or Vaseline. As the injection of paraffin fell out of favor because of the associated complications, aesthetic surgeons continued using the technique to inject other substances, such as rubber and gutta percha. In the 1970s surgeons injected silicone into the nose, but difficulties eventually developed. More recently, temporary fillers such as hyaluronic acid and hydroxylapatite have also been used.
Aesthetic and Topographic Considerations
AGING
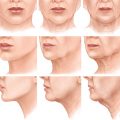
The aging nose loses fullness in the glabella and nasion more than in any other location. As this area atrophies, the remaining parts of the nose become relatively larger. Therefore the tip appears larger with the atrophy of the upper nose and tip. As this happens, the tip may also appear to plunge.
SHAPE
A frequent sequela of rhinoplasty surgery is an open roof in which the cartilaginous and bony parts of the nose have been repositioned so that they are no longer continuous. This leaves open roofs that are palpable and often even visible through the thin skin of the nasal dorsum. Deformation of the cartilage or bone occurs in other situations after rhinoplasties. The skin of the nose in some patients is so thin that irregularities can be amazingly visible, so that many malpositioned subcutaneous structures are painfully visible after nasal surgery.
Indications
The most obvious and simplest use of structural fat grafting to the nose is to fill in irregularities and divots. Placing a thin layer subcutaneously provides support for the skin and can disguise visible irregularities of the cartilage and bone. Concentrating the fat grafts into defined areas can improve the line of light reflection on the dorsum or subtly change the proportion of one part of the nose to another part. The structural application of fat grafts can improve alar notching or close an open roof. Finally, structural fat placed in the nasal valve may act like a spreader graft to relieve nasal airway obstruction. But fat grafting to the nose does much more than fill defects. It not only provides soft tissue coverage of the bony and cartilaginous framework under the skin, but it also thickens the skin of the nose and transforms it to healthier, more elastic skin.
Material and Methods
TECHNICAL GUIDELINES
Anesthesia
Anesthesia is obtained in most cases with local infiltration of 0.5% lidocaine with 1:100,000 epinephrine and sedation. Epinephrine is always useful for causing vasoconstriction and thereby decreasing the possibility of intravascular emboli.
Incisions
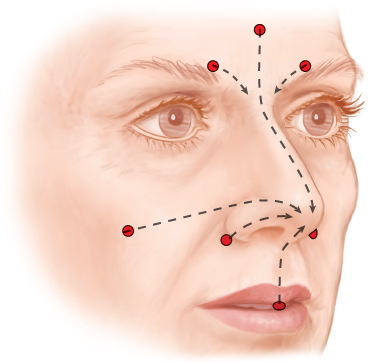
Incisions are usually made in the central forehead, medial eyebrows, cheek, or alar base and through the central lip.
Cannulas
Harvesting is performed using Coleman cannulas, as described in Chapter 1. Infiltration into the nose is performed mainly with Coleman style III cannulas. The flat tip of the style III cannula or mini-cannula helps push through the frequently encountered fibrous tissues of the nose, especially a nose that has scarring from a previous operation. Although I use straight cannulas most often, curved cannulas help navigate the curvature of the nasion and glabella as well as facilitating different approaches to the alae. I use mini-cannulas in most nose cases, as I have in the periorbital region. Finally, I find intradermal infiltration of fat with a sharp needle sometimes helpful. However, the injection of fat or fillers in the nose must be approached with great caution to avoid intravascular emboli.
Level of Infiltration
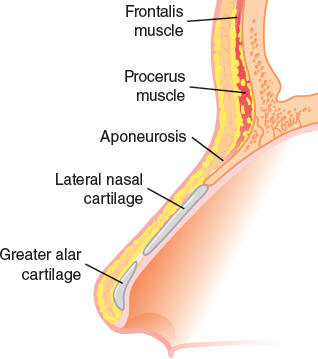
Fat is layered from the periosteum/perichondrium to the intradermal level.
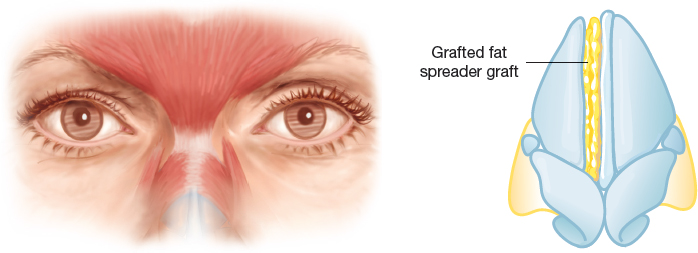
In particular, a significant layer of grafted fat can be placed into the muscles of the upper nose, nasion, and glabella. Occasionally fat can even be placed posterior to the cartilage to help expand the nasal valve, as a “spreader graft.”
Volume Ranges
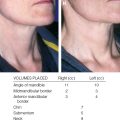
The volume placed varies widely, depending on the defect, but can be as little as 0.4 cc in the alar rim to as much as 9 cc in a saddle-nose deformity.
TECHNIQUE
The key to placement of fat into the nose is meticulous placement in every layer available: intradermal, subcutaneous, and intramuscular; into fibrous tissues; and above and even below the perichondrium and periosteum.
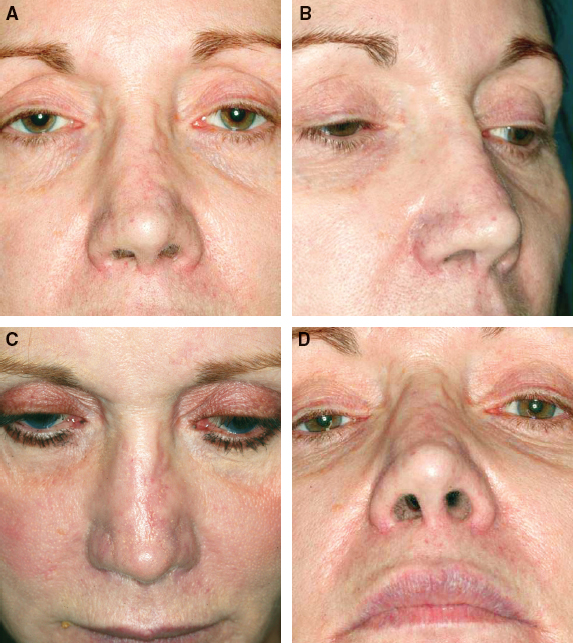
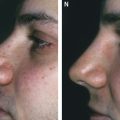
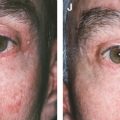
This patient had undergone at least 12 previous nasal procedures, including placement and removal of Gore-Tex, numerous ear cartilage grafts, and not only autologous but also homologous rib cartilage grafts. In spite of the many procedures with well-known and respected plastic surgeons, she was left with a marked irregular nasal surface which was easily visible through the thin skin of her nose.
Drawings/Blueprints

This patient primarily wanted to increase the projection of her nasal tip, but she understood that this was difficult to accomplish with fat grafting. She also wanted the nasal dorsum straightened more, with placement of more tissue down the center of the dorsum to obtain a more central light reflection. She also specifically wanted to have still less alar notching and more columellar show.
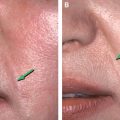
The goals reflected in the blueprints, developed during earlier consultations, were then transferred to her nose using colored markers immediately preoperatively. The red marks indicate the incision sites; the green marks indicate a planned structural change in the area; blue marks indicate planned intradermal placement of fat as well as subcutaneous placement; and orange marks are used to delineate the limits of placement (no fat is usually placed in the areas marked with orange).
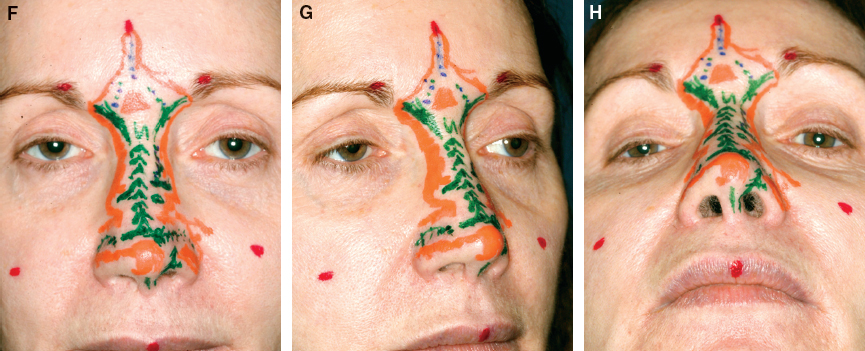
The plan was primarily to create soft tissue coverage to disguise the many irregularities left from her previous procedures, especially the cartilage grafts. In the glabella the focus was on rejuvenation, calling for placement of subtle amounts over the entire area, from orange markings to orange markings, plus some placement directly into the skin of the frown lines (blue). Incision sites were marked in red in her forehead, medial eyebrow, anterior malar cheeks, and vermilion in the middle of the upper lip.
Placement
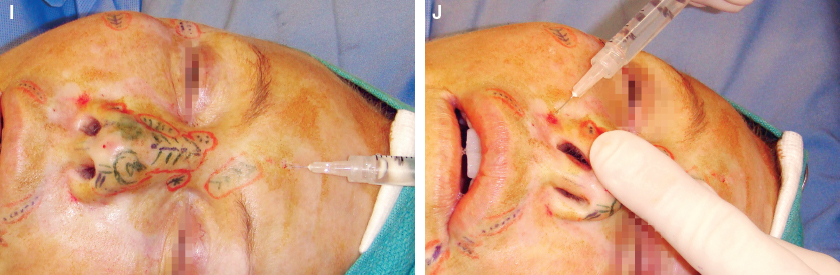
In another patient with a similar presentation, infiltration is shown with a 30-gauge needle into the incision sites, followed by infiltration of the local solution into the entire nose with a type III Coleman cannula.
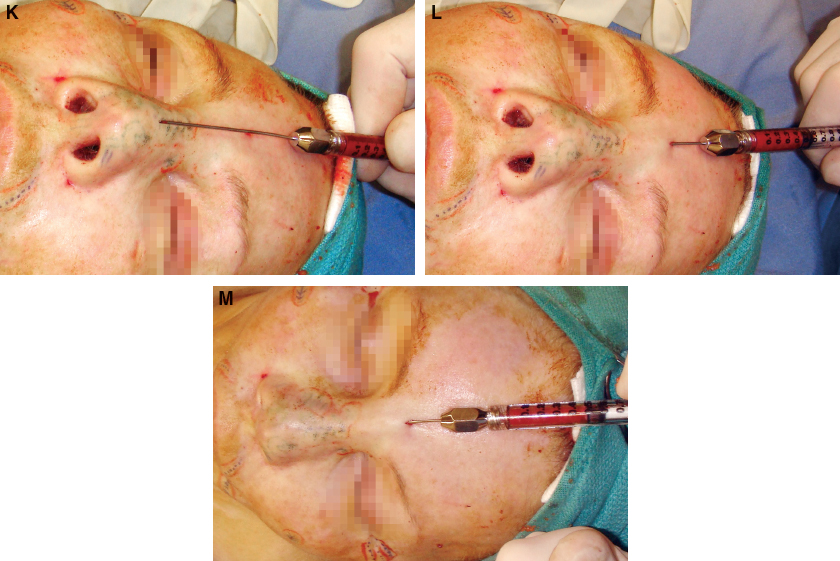
The dorsum is approached first with a curved Coleman cannula through the forehead incision. The fat in this case was layered, beginning against the periosteum/perichondrium, and was gradually brought through the layers to the immediate subdermal layer.
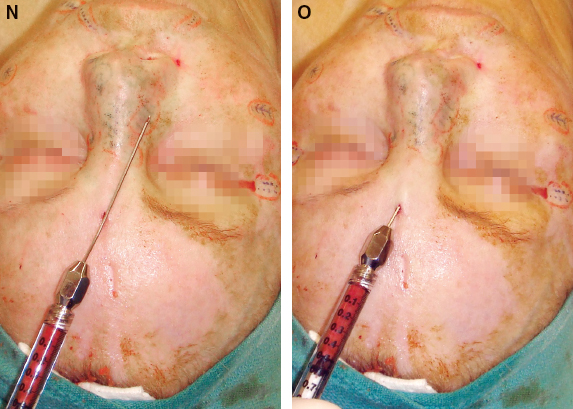
Fatty tissue was then layered in a similar fashion into the right lateral nose deficiency through the same forehead incision.
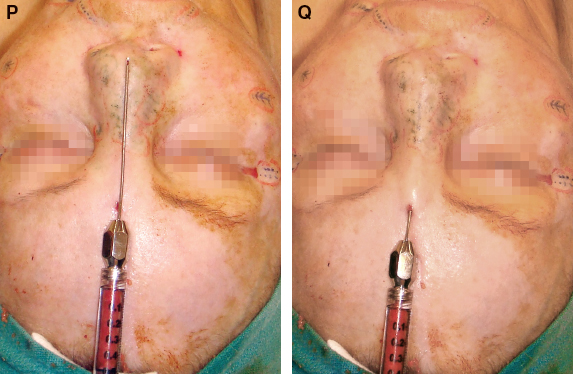
The tip was approached through the same incision to provide the first direction for layering into the tip to try to increase tip projection.
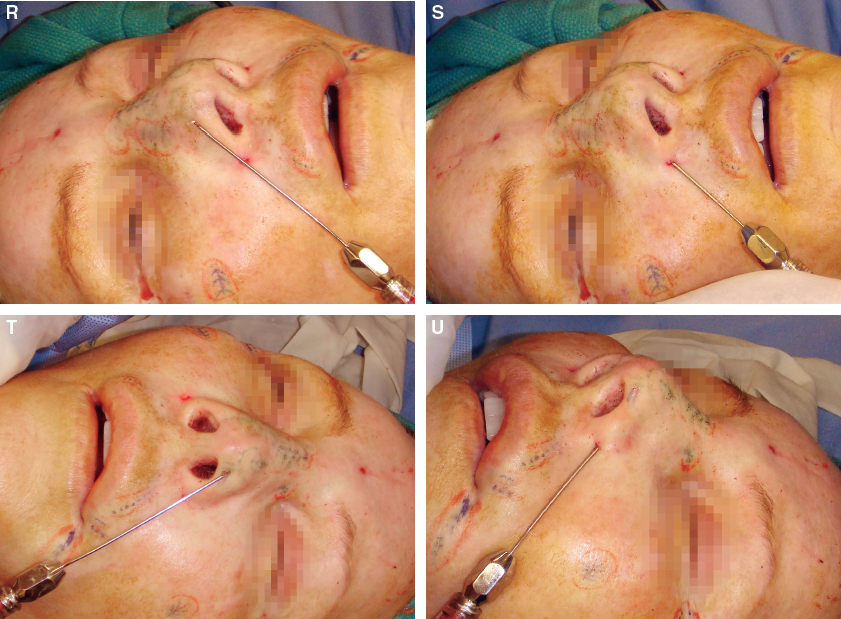
From the alar base, tissue was layered for structural support into the area of the alar notching. This structural approach should start at the alar rim through the middle alae. From this approach, further augmentation of the nasal tip can be attained to increase tip projection.
The right lateral nasal deficiency that was approached from the forehead now could be approached from the alar base. Adding a second direction of placement is always advised when possible.
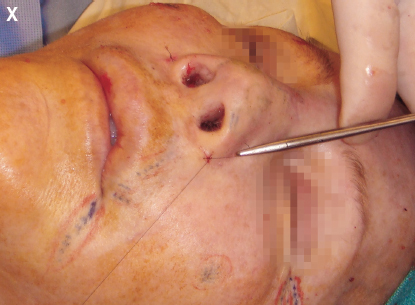
Before proceeding with another direction of placement into the nose, the incisions already made should be closed to prevent leakage of the fat out the incision sites.
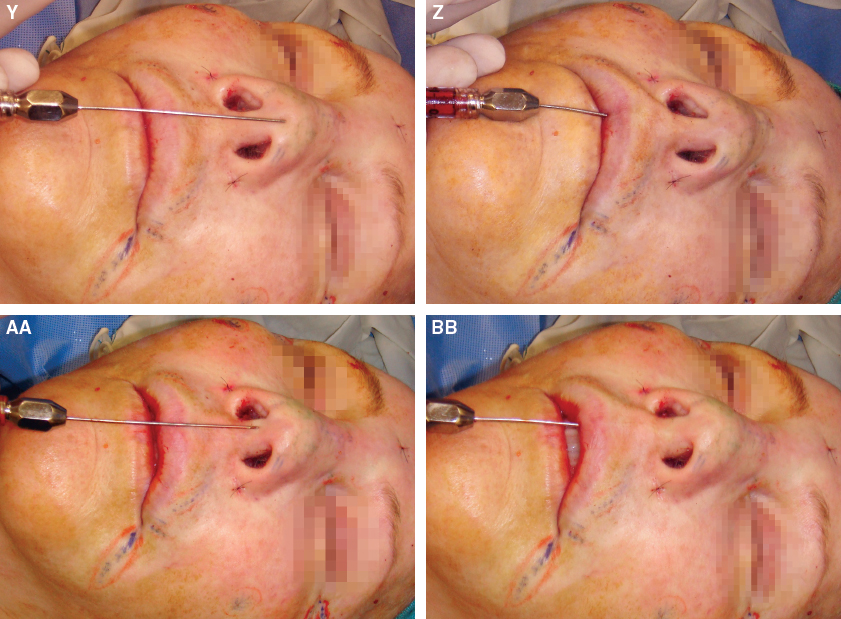
An incision was made in the vermilion of the lip to access the tip from another direction and to allow placement into the columella to increase columellar show.
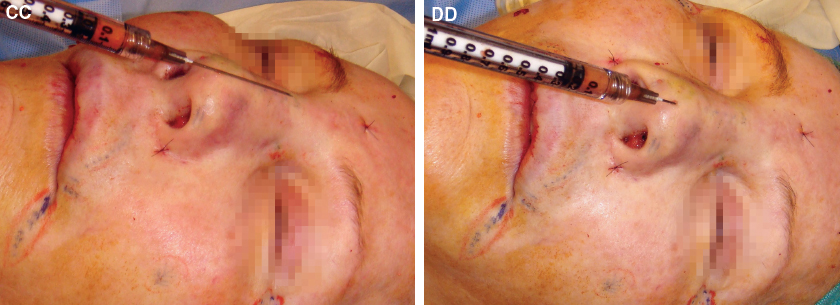
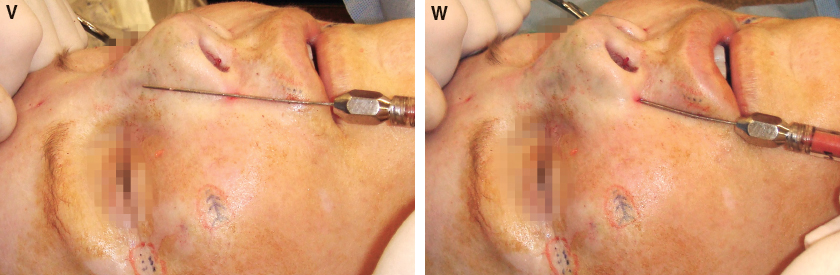
Intradermal injections into the central dorsum can sharpen the straight line of reflected light and add extra dorsal projection and maybe even tip projection.
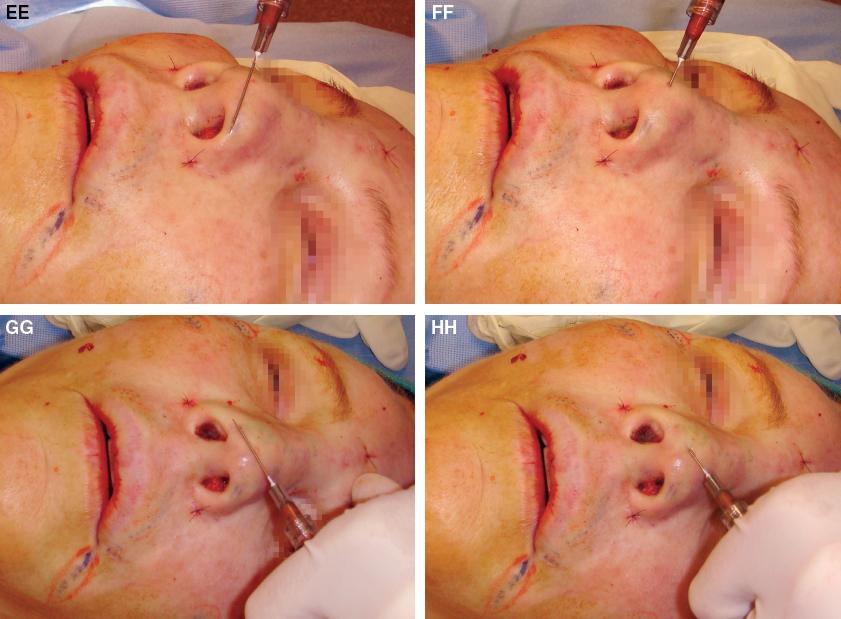
Further support in the alar rim can be created by supplementing the subcutaneous placement with intradermal injection from a different direction. The surgeon should avoid injection into the deeper structures with a sharp needle to avoid intravascular cannulation of arteries.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree