Introduction
Female cosmetic genital surgery (FGCS), sometimes referred to as vaginal rejuvenation, is an umbrella term encompassing multiple plastic surgery procedures that are quite distinct from one another but are often used in combination to achieve a certain vulval appearance. The procedures are performed across several surgical specialties, including urology, gynaecology and plastic surgery. Numerous FGCS techniques are on offer and surgeons may also adapt standard techniques to better suit differences in genital anatomy and satisfy patient requests. Most procedures are operations to alter the external genital appearance, although procedures to tighten the vagina may also be requested and can be performed at the same time. Labiaplasty is the most frequently performed operation on the external genitalia and has become synonymous with cosmetic surgery of the female genitalia. It would be impossible to describe all FGCS procedures in a single chapter. This chapter focuses on labiaplasty techniques.
Normal female genital anatomy is described in detail elsewhere (Chapter 2 by Crouch, this volume). Although there is a wide variation in the normal width of the labia minora and, to some extent, the labia majora, patients who express concerns to surgeons usually complain that the labia minora are too large. Surgeons often describe this as ‘labial hypertrophy’, although this has not been well defined and may well describe normally sized labia. There is no underlying medical cause for labial hypertrophy. Women requesting surgery usually desire a prepubescent aesthetic. The labia majora of young females tend to be fuller and smoother and nearly approximate in the midline just in front of the clitoris to form the intervulvar commissure on the standing position. To achieve this aesthetic, which is associated with younger age, the labia minora are reduced sufficiently to be hidden behind the symmetrical labia majora, giving the vulva a smoother, ‘clamshell’ appearance without unwanted tissue [1] (Figure 5.1a and b). Some patients will express concerns about their clitoral hood in addition to labial concerns. They may complain about unwanted skin folds of the clitoral hood as well as any perceived wrinkling and/or protrusion. There is a wide age range for patients requesting labiaplasty, with reports in the literature ranging from 16 to 68 years [2]. Only a few articles report preoperative width, but where it is recorded the average width measured from midline to the lateral edge of the labia minora ranges from 2.7 to 5 cm. Because of the wide variation in perineal anatomy and the high incidence of asymmetry, meeting the patient’s cosmetic goals can be challenging. A thorough assessment is therefore crucial, even if it involves several consultations.
Before the Operation
Physical examination of the patient has two purposes:
To exclude any underlying pathology which may be causing or exacerbating vulval symptoms
To assess specific vulval concerns and plan appropriate cosmetic genital surgery
Physical Examination to Exclude Underlying Pathology
In a small proportion of cases there will be a medical cause for perceived labial enlargement, and a careful medical examination of the genitals is essential. It is important to exclude rare causes, such as androgenic hormones, either exogenous or as a result of a virilising medical condition, and sensitivity to topical oestrogen. Stretching or weight attachment of the labia for sexual enhancement or as female genital mutilation will lengthen the labia. Dermatitis (which can be secondary to urinary incontinence) and vulvar lymphedema (swelling either post cancer radiation or as a primary disease) must be excluded. It is important to evaluate genital skin health and note conditions such as lichen sclerosus (irregular silver plaques) and herpes simplex lesions (grouped vesicles/blisters).Symptoms such as urinary tract and vaginal infections, urinary incontinence and prolapse may exacerbate labial discomfort, and in some cases referral to a urogynaecologist may be indicated.
Fat loss associated with age, menopause and weight loss can result in flattening of the mons pubis and the labia majora. This can create a perception of excess labia majora skin. Palpation of the clitoris is important to rule out clitoral enlargement as the cause of the prominent appearance of the clitoral hood. Any current or previous medical or psychological problems must be documented and investigated appropriately. Smoking is thought to have a detrimental impact on labial healing after surgery and smoking cessation advice should be offered. It is useful to ask about other lifestyle factors that are potentially implicated in labial health such as hygiene.
Physical Examination to Plan Surgery
Once any underlying pathology is ruled out, the second part of the physical examination is to decide if surgery is indicated and, if so, which technique is most likely to meet expectations. The contour changes of the labia and any vaginal tears resulting from childbirth or injuries should be recorded. Physical examination of the vulva should assess the extent of both vertical and horizontal skin excess and the presence of asymmetry. The amount of subcutaneous fat is evaluated and the skin checked for elasticity and signs of atrophy. The overall pattern of skin and fat distribution in the labia should be noted as well as the presence and extent of any varicosities (prominent veins). The presence and shape of clitoral hood folds and the condition of the hymen or its remnants should be noted. The examination should be performed both in the supine and standing positions.
Preoperative photographs in both the standing and lithotomy positions are usually taken for all cosmetic perineal procedures. Patients frequently do not look at themselves carefully with a mirror in lithotomy position (lying down with legs apart) before the operation, as they are primarily concerned with the standing view. However, postoperatively, they may then notice pre-existing irregularities for the first time.
The decision to proceed with labia minor and /or labia majora surgery is primarily guided by the extent of the patient’s desire to change. It is best that the patient demonstrates a clear understanding of the limitations of labia minora and majora contouring to avoid postoperative disappointment. The risks and benefits for each method should be discussed with patients and the technique used should be based on patient anatomy and patient preference weighted with the desired appearance outcome.
Agreeing on the Goals of Surgery
While the most frequently expressed goal for patients seeking labiaplasty is simply to make the labia minora smaller and/or eliminate significant asymmetry, surgery is often more complex than simple excision. Surgeons see the goal of labiaplasty as aligning as far as possible the patient’s existing external genital to the most desirable appearance in our contemporary world. This aesthetic is based on a differently balanced relationship between the labia minora, clitoral hood and the labia majora. To achieve this balance, the surgeon must address this three-dimensional problem with a series of steps that involve reducing the excess skin and redistributing the fat tissue in a three-dimensional fashion. Clitoral hood contour and clitoral hood ptosis (drooping) may pose a significant challenge and contribute to a ‘top heavy’ appearance. Reducing clitoral hood folds and skin advancement flaps (moving small sections of skin to a different position in the vulva) may be employed to avoid this outcome. It is essential to maintain the neurovascular (blood and nerve) supply to the skin and to preserve the vaginal introitus (entrance) as well as achieving an optimal color/texture match.
For patients who have experienced deflation of the volume of the labia majora due to either weight loss or natural ageing, revolumising of the area using fat transfer techniques can create fuller shaped outer labia. It may be combined with minor skin reduction of the labia major and radio frequency skin tightening. Pubic mound contour should be kept in mind when planning labia majora augmentation to avoid a mismatch. It is often useful to combine lipocontouring (using ultrasound to reduce localized fat) of the pubic mound to achieve the desired vulva aesthetic.
Finally, it is important to clarify whether the patient is seeking surgery for purely aesthetic or functional reasons or with the hope of enhancing sexual satisfaction. An inquiry as to the status of sexual function among women seeking surgery is therefore necessary. It is important to ensure that the patients understand that surgery of the vulval area is not meant to improve a person’s sex life. Informed consent for elective procedures such as labiaplasty and other FGCS procedures should always include a detailed exploration with the patient of the option of no intervention; a ‘cool-off’ period is crucial [3].
Current Surgical Techniques
The history and clinical outcomes of labiaplasty are described in Chapter 6 by Michala and Chapter 4 by Rodriguez (this volume). Since the inception of labiaplasty into the plastic surgery literature by Hodgkinson and Hait in 1984 [4], there have been multiple new technique introductions and modifications. Surgical techniques that have been reported in the literature since that article was published include de-epithelialisation, direct excision, W-shaped resection, wedge resection, composite reduction, Z-plasty and laser labiaplasty [5]. Each labiaplasty technique offers its own advantages and disadvantages. Unfortunately, in the literature to date there is an absence of comparative analysis of the reported labiaplasty techniques to establish criteria for operative planning.
In general the term labiaplasty refers to reduction of the size of the labia minora. Less commonly, however, labia majora reduction is sometimes performed. Conversely, on occasion reduction of the labia minor may be combined with techniques such as fat injection to plump up the labia majora to achieve a more youthful genital contour. There are several main surgical approaches to labiaplasty. Each approach has its own advantages and disadvantages. Surgeons may use a combination of techniques or modify a technique depending on the final outcome which they and the patient hope to achieve.
Labiaplasty of the Labia Minora
The following are broad descriptions of the types of surgical techniques which may be used in labiaplasty of the labia minora.
Labia Minora Excision (Resection, Trim)
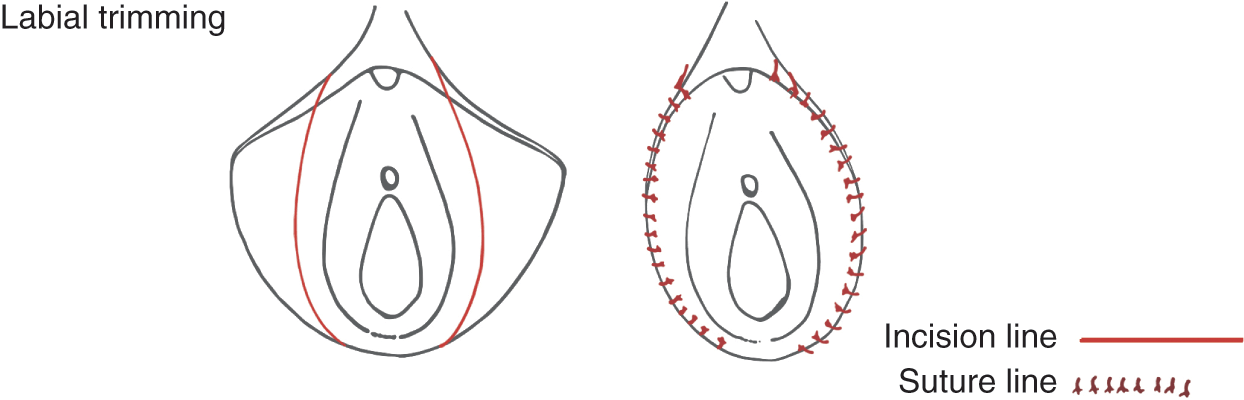
The labia minora can be directly excised by trimming a strip of skin from the lateral aspect (outside edge) of each labia [6] (Figure 5.2a). This procedure is the most straightforward technique and is probably more commonly performed by gynaecologists than cosmetic plastic surgeons. Direct labial excision provides a simple way for the excision of excess tissue, as requested by many patients. This technique, however, removes the natural contour, colour and texture of the free edge of the labia minora. It places a suture line at the free edge of the labia minora, which may lead to visible scar formation (Figure 5.2b). A ‘dog-ear’ (a corner of skin which is more prominent) can be formed at the edge of the incision nearest to the clitoris and can look unsightly. Sensation may, in theory, be affected by scar formation along the border of the labia minora, although neither of these statements regarding scar formation has been validated in any study thus far.
Figure 5.2 Labial trimming. (a) Surgical incisions. (b) Suture line.
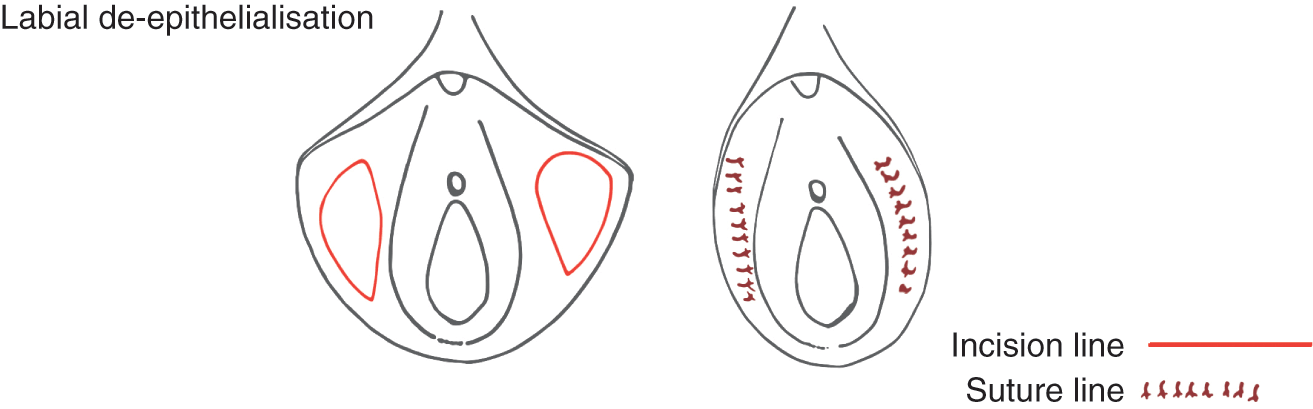
De-epitheliasation
In de-epithelialisation techniques, an oval area of skin on the central and lateral (outside) edges of the labial minora is identified and marked. The overlying skin (epithelium) is removed while preserving the underlying tissues. The skin edges of this area are then stitched together (Figure 5.3a). The advantages of this type of surgery are that it preserves the natural outside border of the labia minora and the neurovascular (blood and nerve) supply [7]. In all studies of the de-epithelialisation technique, complications are few. However, this technique may not work as well in patients with wider labia, as it may not reduce enough tissue bulk. The scar is in the middle of the labia (Figure 5.3b) and may leave the centre of each labia with an uneven appearance.