Introduction
“Do I look normal down there?” This is a question asked by women that many nurses and midwives are all too familiar with. Nurses who work in cervical screening, sexual health and specialist gynaecology clinics have ample opportunities to assist women and girls to explore their genital appearance concerns, to offer reassurances, to signpost to women-centred resources and to offer appropriate advice and triaging. This is also true of the midwives for whom genital examination of women is routine.
In this chapter, we begin by critiquing nursing and midwifery training for not adequately addressing female body distress in general, not least because the professions are themselves staffed mainly by women who are subjected to the same social pressures as the female patients. We will provide a range of clinical scenarios whereby nurses and midwives can offer women useful input. Although we make references to ‘women’ and ‘girls’ in this chapter, we acknowledge that not all people with female-typical genitals identify as such.
Limitations of Nursing and Midwifery Education
In recent years, there has been a shift in nursing and midwifery education away from hospital-based clinical training to an academic degree–based model in the UK [1]. According to UK’s Nursing and Midwifery Council standards for pre-registration nursing education, all nurses and midwives must possess a broad knowledge of the structure and functions of the human body [2]. However, there is significant variability in how this broad brief is translated by training programmes that are governed by the Higher Education Institutes (HEI). Research shows that practitioners lack confidence in explaining the bio-scientific rationale for their clinical practice [1]. When it comes to gynaecology, the coverage is generally thin and invariably limited to reproductive physiology, with very little information on genital anatomy. For midwives, the female anatomy is covered in greater detail, but not to the extent that they can confidently address women’s concerns about genital appearance and function.
Nurses and midwives have fought long and hard for the professional autonomy that they currently enjoy. In many countries, practitioners are granted prescribing rights. In the UK nurse prescribing is well established, with more than 54,000 nurse and midwife prescribers in 2012 [3]. Many more independently offer specialist clinics in acute and community hospitals. They provide independent services in sexual health, family planning, birth injury, female genital mutilation and paediatric and adolescent gynaecology, to name a few. The pressure to acquire bio-scientific knowledge for effective professional practice has increased. However, in all of these specialties, there are implicit and explicit requirements for nursing and midwifery professionals to offer patient-centred or whole-person care [4]. As such, they need to be skilled at detecting emotional concerns. It is important for professional training decision makers to ensure that a balance between bio-scientific education and consultation training is achieved in nursing and midwifery training.
Currently, there are 285,893 nurses and health visitors and 21,596 midwives (whole-time equivalent) registered in the UK [5], of whom 89% are female and 11% are male [6]. Women working in these professions are subjected to the same social pressures on gendered appearances, functions and roles as the women for whom they provide care. A thorough education on female genital anatomy and functions should be seen as much as training for the professional as it is a health education intervention for the woman. While we discuss how nurses and midwives can assist other women, we must also reflect on how social pressures on female appearances may have shaped our own personal preferences and responses to patient and client concerns. If women in the general population are getting their information from the media, in what way are female nurses and midwives different? If we fail to question ourselves, our ignorance will continue to remain in the blind spot, and unhelpful and unprofessional anecdotes pertaining to women seeking information and reassurance being told to have their genitals ‘tidied up’ will surface time and again. The opportunity for empathic reflections and reassurances is repeatedly lost.
A Life Course Understanding of Female Genital Anatomy
Girls and women at any age can feel deeply distressed about their genitals, regardless of how they may appear. The reasons for seeking surgery are variable. Some feel that aspects of their lifestyle are restricted by the inner labia protruding beyond the outer labia (e.g., they find wearing tight clothes and swimsuits uncomfortable or embarrassing). However, research shows that there are no differences in labial dimensions between women who seek labiaplasty and those who do not [7]. Very few men are known to have their genital mass surgically reduced in order to feel more comfortable riding a bicycle or a horse. Therefore female genital distress is gendered. Psychologists have pointed out that even small sensations in a body part can be experienced as intolerable due to their emotional valence.
Throughout the lifespan, the female genitalia change considerably in size, shape and colouration. Our collective failure to recognise and value diversity in body and sexuality is a blessing to the FGCS industry, which in turn keeps us in ignorance. As we present a life course understanding for nurses and midwives in this section, we offer case vignettes to demonstrate good practice.
Puberty
Prepubertal girls generally have smaller inner labia which are often not visible without close inspection. In response to pubertal hormonal changes, the inner labia and the clitoris become much more noticeable. This is entirely normal. During this developmental process, one side can start growing first and both sides usually even out after a while. However, perfect symmetry does not always ensue. This too is normal. The lack of education on vulval structure and appearance diversity combined with popular but biased representations can leave some girls and often their mothers feeling unsure.
Case Study 14.1
A Teenage Girl Seeks Labiaplasty with Parental Support
Hannah is 16 years old. Accompanied by her mother, Hannah meets with her general practitioner (GP) to ask if she can have her inner labia made smaller. In the electronic notes “normal” and “floods of tears” are mentioned. The GP is non-committal and makes an appointment for Hannah and her mother to meet with the practice nurse. Accompanied by her mother, Hannah comes for her appointment. She looks embarrassed and signals to her mother to begin the conversation with the nurse. Her mother says: “I’m worried about my daughter. She gets really upset about how she looks down below … She showed me it. It [the inner labia] doesn’t look right. I don’t remember that. She wants to have the surgery and I think that will really help.” The nurse verifies this with Hannah, who continues the conversation by stating quietly but vehemently how much she hates the way her inner labia look and feel. When asked how she would like her vulva to look, Hannah states that her inner labia should not be showing and that by “leaking” out of the outer labia, they rub together and cause soreness. Hannah’s mother further adds that Hannah has always been a healthy and happy child without any emotional problems. She says Hannah is not vain and is never bothered about how she looks, but that it is “not right” that her labia are “hanging down.” Both daughter and mother want to emphasise that they are not considering surgery “at a whim” and that Hannah has been unhappy about her labia for several years. In Boxes 14.1 and 14.2, we explore potential ways of approaching the conversation with mother and daughter.
Box 14.1 Example Responses and Comments
| Responses | Comments |
|---|---|
| “The doctor thinks you’re normal, Hannah. It’s how you feel though, I understand that. I see lots of girls with poor body image these days. But surgery is not always the answer. I’m happy to talk to you about why you are absolutely normal. What do you think, mum? Or is Hannah not better off seeing our counsellor?” | The content of the message is not wrong. However, the empathy is hollow. It dismisses the young person’s very real concerns, making it difficult for her to work with you. |
| “Wait a while and see how you feel. I understand surgery is a day case. It is available privately if you can’t get it for free. Obviously if you continue to be bothered by this and you think it can really help you, then no one can stop you.” | Here, before any alternative views are explored, the nurse normalises surgery which is invasive and irrevocable but does not address any biomedical concerns. |
Box 14.2 Outline of a More Helpful Consultation
| Steps | Additional Notes |
|---|---|
| Welcome both and praise the mother for being supportive of her daughter. Always inform young people of their right to privacy and confidentiality. Check with Hannah if she would like her mother to stay in the room. If so, mention that you might still ask her mother to leave the room for part of the consultation if Hannah were willing. This will provide you time to provide a confidential space where the young person can disclose any sensitive information which may embarrass them in front of their parents, such as having been sexually active. Try and build rapport with the daughter and the mother. Manage expectations by asking what they have in mind by way of an outcome of the consultation. If support for surgery is mentioned, discuss that this may not ensue but that you are committed to helping them explore a range of options. | The nurse should demonstrate her recognition of the sensitivity of the situation and reassure Hannah and her mother, both vulnerable to shame, that their feelings are valid and they are right to seek help. The nurse’s professionalism will help to gain Hannah and her mother’s confidence and trust. |
| Invite Hannah to tell you about her concerns in her own words, e.g., “Tell me about your worries … ” If Hannah is willing, encourage her to elaborate, e.g., “Can you say a bit more … ?” . Acknowledge that her feelings are real, e.g., “Your distress is real. There’s no right or wrong in our feelings. Many girls tell me they feel unhappy about their body. Before we discuss how to approach your concerns, it’s important we talk more.” Ask Hannah about her life in general – to place the problem in context and to get to know Hannah better. | The health concerns of the young person and her parent should be properly acknowledged. Note whether the young person appears to be withdrawn or anxious and explore current coping strategies which may be positive (e.g., talk to friends about her feelings) or negative (e.g., self-harm/alcohol misuse). As well as that, explore any family (e.g., parents not getting on) and peer problems (e.g., bullying). |
| Ask Hannah what kind of information she has used, e.g., has she viewed the web pages of cosmetic surgery companies and their ‘before-and-after’ picture galleries? This could be a talking point before looking at resources which show a range of genital diversity. | An internet survey suggests that 16- to 24-year-olds are more likely to seek health information and advice online than from health professionals [8]. |
| Seek permission before offering Hannah and her mother some images on vulval appearance diversity such as the Labia Library [9], e.g., “Would it be ok if we look together at some images of ‘normal’? And then you can tell me what you think.” | Recent studies have shown that many adult women have limited knowledge of the different parts of the vulva, their function and genital diversity [10]. |
| Make a further appointment for a follow-up discussion. |
Notes on Educational Intervention
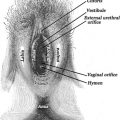
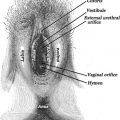
As you acknowledge feelings using the patient’s own words, you can also reframe denigrating wording by offering positive or neutral vocabularies (e.g., ‘sensitive tissue’ instead of ‘extra skin’). You can do this implicitly or explicitly: “Psychologists tell us that the way we talk to ourselves can affect how we feel. I would like to suggest that we try to avoid words that make a situation seem worse than it actually is.” Furthermore, always use correct terms for the different parts of the genitalia and never refer to the vulva as the vagina. For example: “This is the clitoris. It’s made up of the glans which is usually hidden by the clitoral hood. The glans is very sensitive so the hood keeps it protected from rubbing. The glans gets a bit bigger during sexual arousal because of the extra blood flow. The only function of the clitoris is sexual pleasure.”
Here is another example of how to communiate to patients: “You’ve got two sets of labia, the inside and the outside ones. The so called inner labia, despite its name, is visible for most women and, for some women, one side more so than the other. They usually look a little wrinkly after puberty and sometimes even before, because they are soft and stretchy. They have an important job to do – to protect your vaginal opening and experts say nowadays they contribute to sexual pleasure.”
As a third example of how to give information: “It is normal for the outer labia (lips) to grow bigger and for the clitoris to become more prominent. What a shame no one talks about these normal changes during puberty and later, causing so many girls and even older women to worry.”
Notes on Genital Examination
Hannah should not be examined again unless you are especially confident and skilled in performing genital examinations [11]. The most likely outcome of another examination is that you will, like Hannah’s GP, see a normal vulva. However, it may be an opportunity for Hannah to pinpoint the exact area that she is worried about. You can also teach Hannah about the different parts of the vulva on an examination couch using a mirror so she can see her own genitals. Alternatively, you can use images from online resources such as the Labia Library [8]. It is best practice to ask Hannah how she would like to do this.
The examination must be discussed first and consent obtained, including whether the mother is to be present. A chaperone should also be available. Ensure that enough time is allocated and that you are not disturbed halfway through. Have all materials at hand (e.g., lubrication and swabs if needed).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree