CHAPTER 38 Local Flaps and Vascularized Lymph Node Transfer
KEY POINTS
The thoracodorsal artery perforator (TDAP) flap and vascularized lymph node transfer (VLNT) are harvested simultaneously with the patient in the decubitus position.
Great care must be taken to preserve the potential recipient vessels in the axilla and lateral chest during the dissection of the TDAP.
If no suitable recipient vessels are found, the TDAP pedicle may be used in an end-to-side anastomosis.
Preoperative magnetic resonance angiography or computed tomography angiography is helpful but unnecessary to confirm the viability of the TDAP pedicle.
The treatment for breast cancer can include a wide variety of surgical options, including lumpectomy, partial mastectomy, mastectomy, and any degree of axillary lymph node sampling. These procedures can result in both functional and cosmetic deformities requiring reconstruction. There are various options for autologous breast reconstruction, which are tailored to the specific defect. Reconstruction of the axilla may be indicated if the patient develops lymphedema of the upper extremity, which occurs in up to 42% of patients after lymphatic dissection during surgery for breast cancer. 1 The vascularized lymph node transfer (VLNT) is an effective way to treat postoperative lymphedema by reconstructing damaged lymphatic anatomy. 2 – 4 VLNT is a microsurgical free tissue transfer that transplants healthy lymph nodes to the area where lymph nodes have been either removed or traumatized. For patients who have lymphedema and need breast reconstruction, these two reconstructive operations can be combined. Microsurgical (free flap) autologous breast reconstruction with simultaneous lymph node transfer as part of the breast flap has been described. 2
In this chapter I will describe the use of local pedicled perforator flaps for partial breast reconstruction combined with VLNT for axillary reconstruction. Two case examples show how the lateral thoracic flap, specifically the thoracodorsal artery perforator (TDAP), can be combined with simultaneous VLNT to reconstruct two different breast deformities in patients who also have lymphedema.
Mastectomy of the Right Breast With a Failed Expander
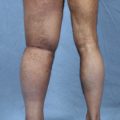
This 49-year-old woman had hypertension, depression, and obesity (BMI 39.6). She underwent a modified radical mastectomy and axillary lymph node dissection of the right breast for breast cancer, and a submuscular expander was placed for reconstruction. The expander leaked and was never expanded. She presented for right breast reconstruction and also had right arm lymphedema. Her symptoms included right arm swelling (Fig. 38-1, A).
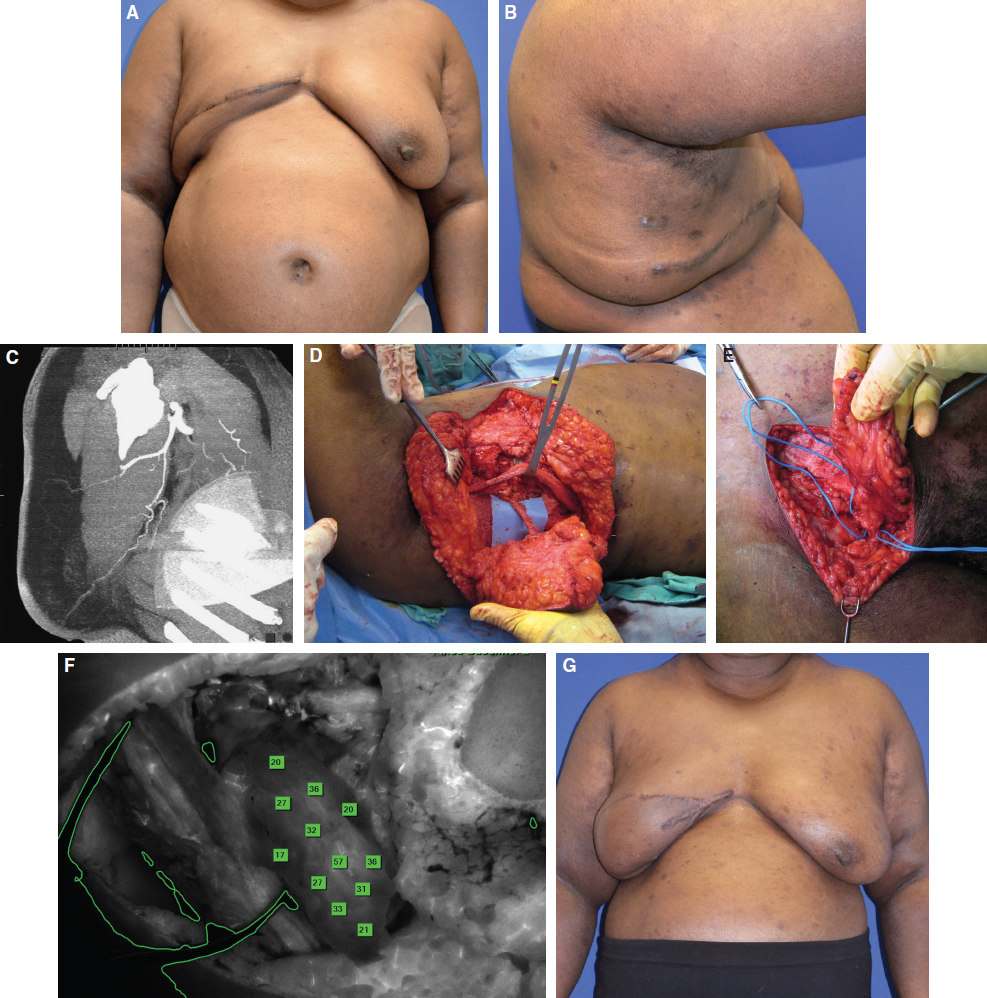
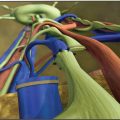
Her anatomy was suitable for autologous reconstruction with a lateral thoracic pedicled perforator flap because of the extended dog-ear on her chest from her previous mastectomy. This created an excess of lateral thoracic tissue that could be used for breast reconstruction (Fig. 38-1, B). A CT angiogram was obtained to evaluate the perfusion of the thoracic tissue, and a large TDAP was identified supplying this tissue (Fig. 38-1, C).
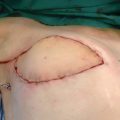
The patient underwent a TDAP total breast reconstruction with simultaneous VLNT (Fig. 38-1, D). The VLNT was harvested from the patient’s lower abdomen, just cephalad to the right inguinal ligament (Fig. 38-1, E), and was transferred to the right axilla. The recipient vessels were branches of the TDAP pedicle.
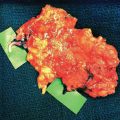
SPY indocyanine green intraoperative angiography was used to confirm the perfusion of the lymphatic tissue (Fig. 38-1, F). The patient did well after surgery. Her symptoms improved, and she had a reduction in forearm circumference (Fig. 38-1, G).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree