Case 57 Peripheral Nerve Injury
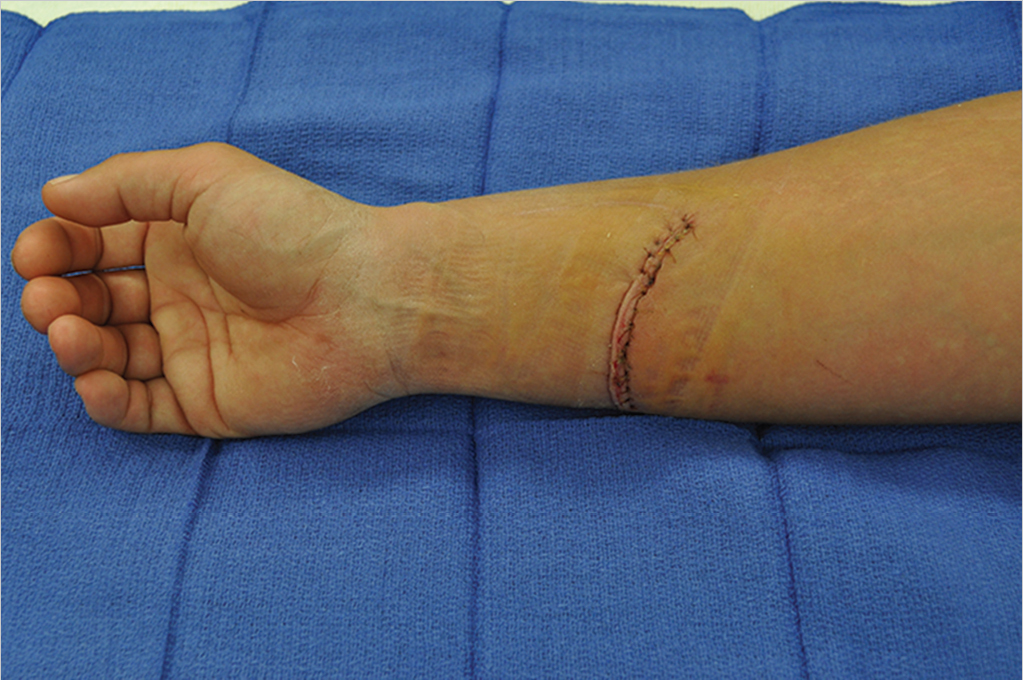
57.1 Description
Laceration repair over the volar aspect of the mid-forearm with decreased sensation to the median nerve distribution
Concerning for sharp injury to the median nerve
57.2 Work-Up
57.2.1 History
Mechanism of injury: Closed versus open
Closed injuries: Best treated initially with observation to distinguish between neuropraxia and true neurotmesis
Open injuries with nerve deficits: One must assume there is a nerve transection, requiring operative exploration and repair
Time since injury
Early repair of injured nerve is associated with improved recovery
Any additional or associated injuries and limitation in motion
Significant bleeding at the time of injury
Hand dominance, occupation, smoking history, and comorbidities
57.2.2 Physical Examination
Assess for associated lacerations, scars, presence of open injury, and viability of soft tissue coverage
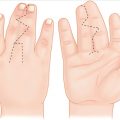
Complete sensory examination, including two-point discrimination of ulnar, median, and radial nerves; assess motor nerve function in a controlled manner
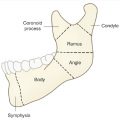
Median nerve at this level innervates the flexor pollicis brevis, opponens pollicis, abductor pollicis brevis, and radial two lumbricals (index and long)
Ask patient to oppose thumb or flex at metacarpophalangeal (MCP) joints of index and long fingers
Ulnar nerve innervates the hypothenar musculature and interossei (abduct and adduct fingers, assess for clawing, Wartenberg’s sign, Froment’s sign)
Vasomotor paralysis is a subtle yet reliable sign of early nerve injury; the skin in the area of the affected nerve is often warm and dry
Tinel’s sign: May help in identifying the site and level of injury, as well as the presence of neuroma or neuroma-in-continuity
Palpation and Doppler evaluation of ulnar and radial arteries
Examine tenodesis and cascade
Independently examine wrist flexors and finger flexors
57.2.3 Pertinent Imaging or Diagnostic Studies
Standard three-view x-rays should be obtained to assess for fracture or foreign body
For a closed injury, electrodiagnostic studies at 3 months may be helpful in ascertaining prognosis of nerve recovery
Fibrillation: Indicate some degree of motor injury
Motor unit potentials (MUPs): Indicate recovery
57.3 Patient Counseling
Nerve recovery after closed or open injury takes time. Axonal regeneration occurs at a rate of approximately 1 mm/day.
Recovery time can be estimated by measuring the distance from the site of injury to the distal target.
Nerve recovery after repair is unpredictable. Successful functional recovery after peripheral nerve repair has been reported to be between 50 and 80%, depending on the nerve and the location of injury.
57.4 Treatment
Indications for operative exploration of a nerve
Paralysis/sensory deficits of a major nerve after an open wound
Paralysis/sensory deficits affecting a nerve after a nearby iatrogenic surgery
A nerve lesion associated with arterial injury
A nerve lesion associated with a fracture or dislocation requiring open reduction and internal fixation (e.g., radial nerve exploration after open humeral fracture)
Deterioration/failure of recovery of a closed nerve injury while under observation
Exploration for other injuries (i.e., tendon lacerations)
Initial treatment plan should be based on type (open vs. closed) and chronicity of nerve injury
Muscle denervation begins to take place soon after nerve injury and the potential for reinnervation decreases as time passes (approximately 1% per week)
The time needed for nerve regeneration (1 mm/day) should be weighed against the potential for muscle reinnervation when considering nerve repair
All patients will benefit from hand therapy to maintain passive range of motion, manage pain, edema, and other problems associated with the inciting injury
57.4.1 Acute Open Injuries with Nerve Dysfunction
Require nerve exploration: Must assume the nerve was transected
The prognosis of nerve recovery is directly related to the interval between injury and nerve repair; clean injuries to motor nerves are best treated within a few days
Local contamination should be considered when considering nerve repair; nerve repair should be delayed until the wound bed is clean
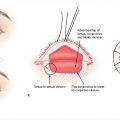
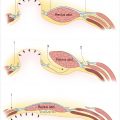
Direct repair or repair with an interposition graft is appropriate
Nerve transfers and babysitter procedures can be considered in high (proximal) motor nerve injuries
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree