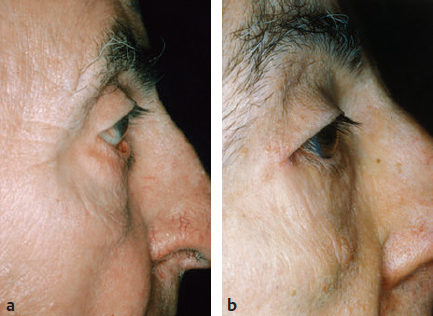
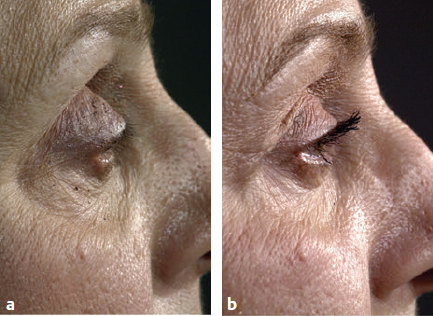
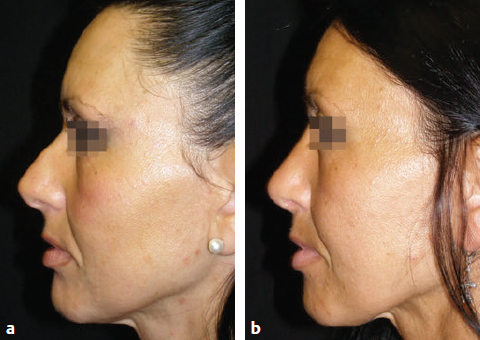
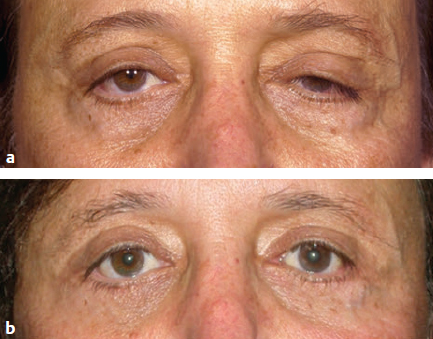
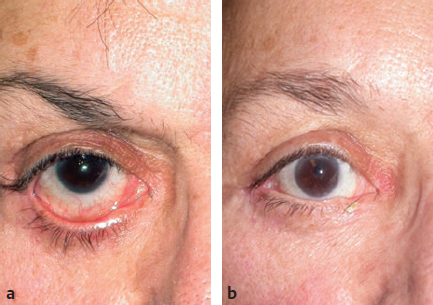
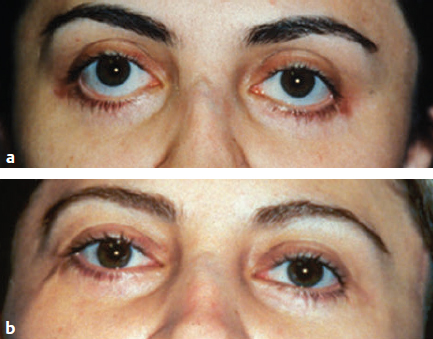
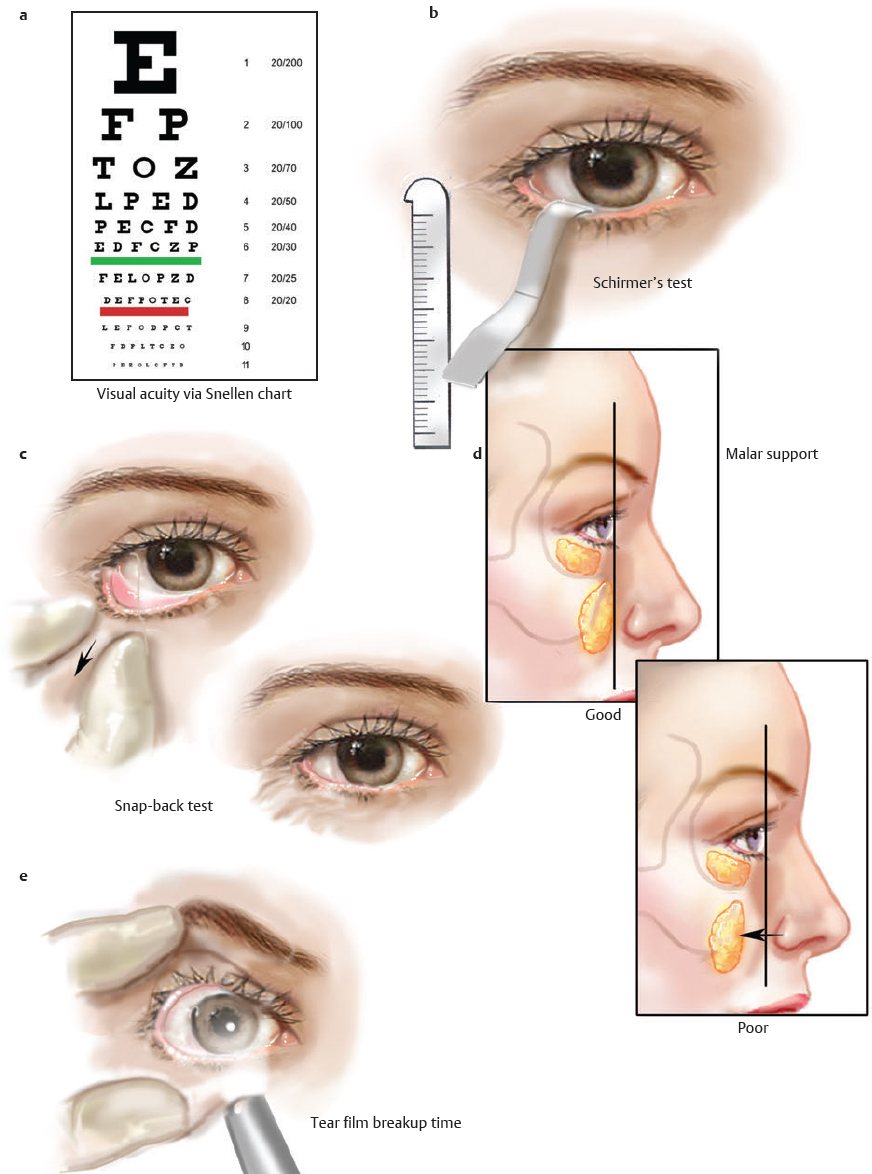
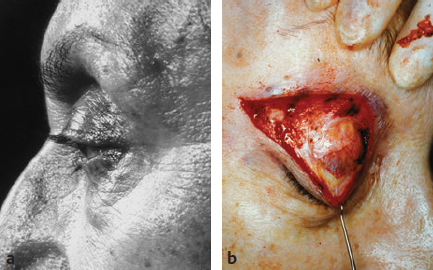
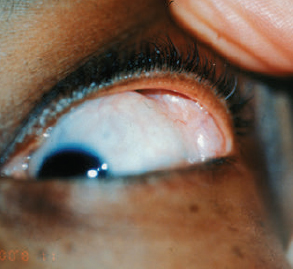
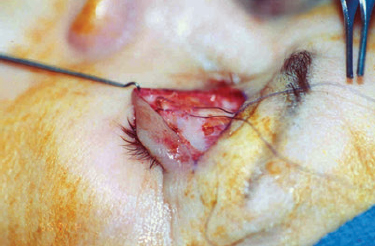
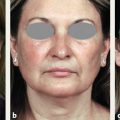
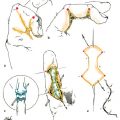
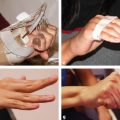
CHAPTER The demand for blepharoplasty (cosmetic eyelid surgery) continues to rise annually in the United States; according to the American Society of Plastic Surgery, 206,509 blepharoplasties were performed in 2014.1 The frequency of this procedure has predictably coincided with an increased number of early and late complications. Complications are inevitable, but surgeons must be able to recognize postoperative complications and guide appropriate management. Most important, complications can be significantly minimized with a detailed understanding of the surgical anatomy, focused history and physical examination, patient education and informed consent, and a refined surgical approach. This chapter discusses the spectrum of complications seen with blepharoplasty, preventive solutions, and treatment options.2–4 The skin of the eyelid is the thinnest in the body and has minimal subcutaneous fat. As patients age, the periorbital skin has decreased type I collagen synthesis and increased dermal collagenase activity. With time, these metabolic shifts lead to thinning, folding, and wrinkling of the eyelid skin.2–10 The orbicularis oculi is the sphincter of the eyelid. This muscle is adherent to the overlying skin and comprises three parts: orbital, palpebral, and lacrimal. The outer, orbital portion attaches medially to the medial canthal tendon, the nasal part of the frontal bone, and along the inferomedial orbital margin. Laterally, the orbital portion continues around the orbit and attaches to the lateral canthus. The palpebral portion of the orbicularis oculi, the middle segment, has pretarsal and preseptal segments. Medially, the preseptal segment of the palpebral portion of the orbicularis oculi has the anterior head, which becomes the anterior crus of the medial canthal tendon and inserts into the frontal process of the maxilla, and the posterior head, which inserts into the posterior lacrimal crest (Horner’s muscle). Laterally, the preseptal fibers of the palpebral portion of the orbicularis oculi coalesce with the lateral palpebral ligament to form the lateral palpebral raphe. The small, inner portion of orbicularis oculi, the lacrimal segment, interdigitates with the medial palpebral ligament. This portion of the orbicularis oculi arises from the orbital surface of the lacrimal bone, passes behind the lacrimal sac, and divides into two slips, upper and lower, which are inserted into the superior and inferior tarsi, medial to the puncta lacrimalia.2–10 The three segments of the orbicularis oculi have distinct functions. The orbital portion of the orbicularis oculi tightly closes the eye. Contraction of the pretarsal and preseptal portions of the palpebral orbicularis oculi primarily closes the eyelid. The lacrimal portion transposes the lacrimal canals medially to receive tears and compresses the lacrimal sac.2–10 The orbicularis oculi is anchored by well-defined ligamentous attachments. Medially, the orbicularis oculi attaches directly to the inferior orbital rim. Laterally, the orbital retaining ligament bridges the fascia of the orbicularis oculi to the periosteum of the orbital rim. At the lateral canthus, the orbital retaining ligament merges with the lateral orbital thickening, a triangular condensation of the superficial and deep orbicularis oculi that extends across the frontal process of the zygoma onto the deep temporalis fascia. Release of the orbital retaining ligament and lateral orbital thickening allows untethered redraping of the eyelid.2–10 With age, the orbicularis oculi muscles relax, and the ligamentous attachments attenuate. This transformation results in progressive eyelid ptosis. Malar ptosis compounds this eyelid ptosis, forming a malar crescent or festoon over the malar eminence with an aged appearance. In addition, the pigment of the orbicularis oculi becomes more apparent over the thinning skin.2–10 Fig. 22.1 (a) This patient had ectropion and lower lid retraction with malar ptosis after a lower lid blepharoplasty by a referring plastic surgeon. (b) Correction of the ectropion and lower lid contraction with a tarsal strip canthoplasty. This patient elected not to correct the malar ptosis. Fig. 22.1a demonstrates a patient with ectropion and lower lid retraction with malar ptosis after a lower lid blepharoplasty by a referring plastic surgeon. Fig. 22.1b demonstrates the correction of the ectropion and lower lid contraction with a tarsal strip canthoplasty that I (H.M.S.) performed. Of note, the patient elected not to correct the malar ptosis. The tarsal plates, composed of dense fibrous tissue, are located directly above the lid margins and contribute to the integrity and support of each eyelid. Each tarsus measures approximately 29 mm long and 1 mm thick. The semilunar, superior tarsus measures 10 mm centrally and narrows medially and laterally. Conversely, the rectangular, inferior tarsus measures 3.5 to 5 mm centrally. The medial and lateral ends of the tarsi are attached to the orbital rims by the medial and lateral palpebral ligaments. Each tarsus contains approximately 25 sebaceous meibomian glands, which secrete meibum, an oily substance that prevents evaporation of tear film.2–10 The orbital septum has dense fibroelastic tissue and forms the anterior boundary of the orbital contents. On the upper eyelid, the orbital septum inserts 10 to 15 mm above the superior tarsal border and joins the levator aponeurosis. On the lower eyelid, the orbital septum joins the capsulopalpebral fascia 5 mm below the tarsal border. In addition, inferiorly, the orbital septum fixates to the rim of the orbital periosteum and forms the arcus marginalis.2–10 The upper eyelid has two distinct intraorbital fat compartments, medial and central, divided by the superior oblique. The medial fat pad is lighter and firmer than the central fat pad. In addition, the medial fat pad encompasses the infratrochlear nerve and the terminal branch of the ophthalmic artery. Of note, the lacrimal gland occupies the lateral compartment.2–10 The lower eyelid has three distinct fat compartments: the medial, central, and lateral fat pads. The inferior oblique separates the medial and central fat pads. The central and lateral fat pads are separated by the arcuate expansion, a fascial band extending from the capsulopalpebral fascia to the inferolateral orbital rim.2–10 Of note, the interconnecting septae of the intraorbital fat link the extraconal (outside the muscle cone) and intraconal (within the muscle cone) spaces. Therefore traction on fat just posterior to the orbital septum can produce forces in any of these spaces and accounts for the small but definitive risk of orbital hemorrhage and even blindness when addressing anterior orbital fat in surgical procedures.2–10 The preseptal, or extraorbital, fat represents retro-orbicularis oculi fat and may accumulate outside the orbital rim on the inferior lateral brow and upper malar areas.2–10 The levator palpebrae muscle is the upper eyelid retractor and originates from the lesser wing of the sphenoid, extending anteriorly along the superior orbit. The levator condenses approximately 14 to 20 mm above the superior border of the tarsus into Whitnall’s ligament. Anterior to Whitnall’s ligament, the levator forms a bilamellar aponeurosis that joins with the septum to insert into the tarsus. A lateral horn divides the lacrimal gland into the palpebral and orbital lobes and contributes to the lateral retinaculum. A medial horn inserts into the lacrimal crest. The posterior lamella of the levator aponeurosis contains Mueller’s muscle.2–10 The capsulopalpebral fascia forms the lower eyelid retractors. This fibroelastic tissue originates from the inferior oblique muscle, fuses into Lockwood’s ligament, and inserts approximately 5 mm below the inferior tarsus.2–10 The lateral canthus partitions into an anterior and posterior leaflet. The anterior leaflet inserts onto the orbital rim periosteum, and the posterior leaflet inserts onto the lateral orbital tubercle (Whitnall’s), approximately 3 mm behind the orbital rim. The lateral canthus lies approximately 6 mm below the lacrimal gland fossa and is the culmination of the lateral canthal retinaculum, which consists of the following: • Lateral horn of the levator palpebrae superioris • Preseptal and pretarsal orbicularis oculi • Lockwood’s ligament • Check ligament of the lateral rectus muscle Of note, all key elements of the lateral retinaculum need to be addressed before mobilizing the lateral canthus for any repositioning or tightening procedures. The most anatomically ideal and aesthetically pleasing position of the lateral canthal tendon is 10 to 15 degrees above the medial canthal tendon.2–10 Fig. 22.2a demonstrates a patient with lateral canthal effacement and displacement after three blepharoplasties by a referring plastic surgeon. In addition, this patient has levator dehiscence and ptosis of the upper lid and ectropion of the lower lid. Fig. 22.2b demonstrates the correction of the lateral canthus, lid ptosis, and ectropion with levator advancement and a canthoplasty that I (H.M.S.) performed. Fig. 22.2 (a) This patient had lateral canthal effacement and displacement after three blepharoplasties by a referring plastic surgeon. In addition, he had levator dehiscence and ptosis of the upper lid and ectropion of the lower lid. (b) After correction of the lateral canthus, lid ptosis, and ectropion with levator advancement and a canthoplasty. The medial canthal tendon inserts into the bony orbit with three leaflets: anterior and posterior horizontal leaflets and a vertical leaflet. The medial canthal tendon is the culmination of the medial canthal retinaculum, the confluence of the deep head of the pretarsal orbicularis, the orbital septum, the medial end of Lockwood’s ligament, the medial horn of the levator aponeurosis, the check ligaments of the medial rectus muscle, and Whitnall’s ligament. Of note, the upper, lower, and common lacrimal canaliculi are closely approximated to the medial canthal retinaculum, and care should be taken to preserve their integrity when altering its position2–10 (Fig. 22.3). Summary Box Unfavorable Results and Complications Associated with Blepharoplasty • Visual loss secondary to hemorrhage • Perforation of the globe during anesthesia • Damage to the extraocular muscle • Damage to the cornea • Wound dehiscence • Lower eyelid malposition • Upper eyelid malposition (ptosis) • Loss of lashes • Dryness • Infection • Incisional scarring • Excessive upper lid fat resection • Inappropriate lower lid fat resection A detailed history and physical examination may not only differentiate an ideal surgical approach but also elucidate the patient’s desires. The preoperative consultation should dismantle any preconceived notions of blepharoplasty and educate the patient on the appropriate surgical steps based on the patient’s aesthetic aspirations, clinical history, and eyelid morphology. Together, the surgeon and patient should develop a mutual understanding that the surgical approach will be selected based on not only patient preference but also the tissue characteristics. The patient must understand the limitations of his or her eyelid topography. The surgeon and patient can review patient images and physical attributes to determine the ideal clinical course. This educational approach and informed consent has proven to enhance patient satisfaction and overall aesthetic outcomes.2–4,11–15 Fig. 22.3 (a) An oblique cross-section of the right orbit and adnexa. (b) A lateral cross-section of the right orbit and adnexa. Note the relationship of the levator, the superior rectus, the inferior oblique, and rectus muscles. Also, note the preaponeurotic fat pad superiorly and the postseptal fat pad (precapsulopalpebral) inferiorly. Before the physical examination, the surgeon should take a detailed history. The consultation should include a general medical history and a detailed ocular history, including a description of dry eyes or ophthalmic lubricants, corrective lenses, thyroid disease, previous refractive surgery, recurrent acute or chronic blepharitis, and any other ocular or periocular conditions. A detailed history may suggest various procedures for the patient. For example, a patient with a history of dry eyes and corrective lenses will certainly demand greater tear production and tolerate less evaporative loss than a patient without those underlying issues. Alternatively, chronic blepharitis or recurrent herpes zoster may be exacerbated by eyelid surgery, and prophylactic antibiotic or antiviral therapy may be warranted before surgical intervention. The most important aspect of obtaining a good history is to tailor the surgical procedure to the individual patient; this approach will minimize risks and maximize the cosmetic and therapeutic aspects of any procedure.2–4,11–15 The aesthetic desires of the patient must be discussed and determined; I (H.M.S.) prefer having the patient describe his or her complaints while looking in a mirror. In addition, reviewing static and dynamic eyelid and facial photographs from multiple views may identify abnormalities, delineate patient wishes, and enhance the consultation.2–4,11–15 A detailed physical examination is essential to determining the ideal surgical approach. The initial examination should note any gross anatomic abnormalities and normal structures; in addition, the proper anatomic position and relationship of the upper and lower lids should be identified. The upper lid should divide the width of the iris in half. The lower lid should lie above or abut the corneoscleral junction; the upper and lower lids should have a smooth sweeping arch or contour. The highest point or maximal arch of the upper lid should lie at the most medial aspect of the pupillary aperture. Inflammatory changes and crusting along the eyelid margins or within the eyelashes indicate blepharitis. A clear glistening corneal surface, sclera, and conjunctiva without injection indicate adequate coverage, lid excursion, and appropriate wetting of the ocular surface. Eyelid folds should be symmetrical; the fold height varies according to the patient’s sex and race. The patient’s superior sulcus should be examined, including the level of concavity or convexity and its relationship to eyelid movement.2–4,11–15 Fig. 22.4a demonstrates a patient with upper eyelid ptosis after four blepharoplasties by a referring plastic surgeon. Fig. 22.4b demonstrates the correction of the lid ptosis with levator advancement and a canthoplasty that I (H.M.S.) performed. Fig. 22.4 (a) This patient had upper eyelid ptosis after four blepharoplasties by a referring plastic surgeon. (b) After correction of the lid ptosis with levator advancement and a canthoplasty. Eyelid margin abnormalities (ectropion or entropion) and whether they change with the blinking cycle should be determined. For example, patients with involutional entropion will usually present with lax lower eyelids, scleral show, and sometimes a tendency toward ectropion until they are asked to close their eye forcibly. Almost immediately, the lower eyelid of these patients will briskly roll inward against the globe with forced blinking.2–4,11–15 Fig. 22.5a demonstrates a patient with chemosis, scleral show, and lid retraction after a blepharoplasty by a referring plastic surgeon. Fig. 22.5b demonstrates the correction with a canthoplasty and a palatal graft that I (H.M.S.) performed. Furthermore, baseline visual acuity should be documented with a Snellen chart; the right and left eye should be assessed with and without corrective lenses. Commonly, patients complain about visual acuity changes postoperatively; as such, a baseline should be documented presurgically. Of note, astigmatism in a selective meridian can be alleviated or induced by surgery, and an ophthalmologist referral may be warranted before surgical intervention.2–4,11–15 Next, extraocular motion and pupillary function should be assessed, with asymmetries being most notable. Normal facial animation and a pupillary light and accommodation response should identify appropriate innervation.2–4,11–15 Fig. 22.5 (a) This patient had chemosis, scleral show, and lid retraction after a blepharoplasty by a referring plastic surgeon. (b) After correction with a canthoplasty and a palatal graft. Fig. 22.6 (a) This patient had chemosis, scleral show, and lid retraction after a blepharoplasty by a referring plastic surgeon. (b) After correction with a canthoplasty and a palatal graft. Subsequently, tonicity of the lower eyelid should be measured. The lower eyelid is gently pulled down and distracted away from the globe and then allowed to retract back into its regular anatomic position. Delays or asymmetries in the rate or position of the lower lid snap-back should be recorded. A youthful and intact lower eyelid should position itself against the globe and revert to an appropriate height within 1 second of distraction. I (H.M.S) grade snap-back as weak, moderate, or brisk; anything but a brisk snap-back requires increased intrinsic support or minimized extrinsic distraction forces.2–4,11–15 In addition, the periorbital anatomy should be evaluated, specifically the presence or absence of zygomatic or malar support. Patients whose malar eminence lies posterior to their cornea have poor lower lid support and are prone to malposition. In patients with lower eyelid malposition (scleral show), the surgeon should digitally elevate the lower eyelid and tighten while concomitantly visualizing the tension created on the suborbital soft tissues. This manual suspension may guide appropriate surgical intervention. In addition, the surgeon should try to assess which lamella (anterior, middle, posterior) is deficient. This differentiation will assist in planning complementary procedures to the canthopexy such as cheek or midface suspension, interposition grafts, skin grafts, or external flaps.2–4,11–15 Fig. 22.6a demonstrates a patient with chemosis, scleral show, and lid retraction after a blepharoplasty by a referring plastic surgeon. Fig. 22.6b demonstrates the correction with a canthoplasty and a palatal graft that I (H.M.S.) performed. All patients should be assessed for baseline tear production with Schirmer’s test using topical anesthesia and pre-cut standardized No. 41 filter paper strips. This assessment should take place in a dark room to prevent the effect of ambient light on tear production. Patients can be subdivided into three categories: low tear producers (0–9 mm), moderate tear producers (10–20 mm), or high tear producers (21–30 mm). Of note, very high tear producers may have obstruction of the nasolacrimal system and may present with a spectrum of complaints including epiphora, recurrent medial canthal swelling, and/or mucopurulent discharge.2–4,11–15 In addition to tear production and tear quality, the ability of tears to withstand evaporation or breakup should be assessed; a simple test can be performed that measures film breakup time. Fluorescein is introduced onto a topically anesthetized eye, and after the patient blinks to disperse the agent, the eyelids are then held apart and the uniform tear film is visualized over the corneal surface through a cobalt blue filter. The period between holding the patient’s eyes open and deterioration of the tear layer (tear film breakup) should be longer than 20 seconds. Of note, because of the multifactorial etiology of tear quality, this test may have low yield.2–4,11–15 After a detailed history and physical examination, the surgeon should identify the problem and tailor the surgical procedure according to the specific patient’s findings. There are almost no contraindications to surgery in the periocular region but rather definitive historical and physical signs that dictate the ideal surgical approach for an individual patient.2–4,11–15 Fig. 22.7 outlines key components of the preoperative physical examination before an upper and lower eyelid blepharoplasty.3,16 The morphology of the upper eyelid can be differentiated into four different categories: 1. Occidental 2. Deep set 3. Baggy 4. Asian The normal youthful Occidental upper eyelid has levator extensions inserting into the skin surface to define a lid fold that averages 6 to 8 mm above the lid margin. The orbital septum coalesces with the levator aponeurosis, creating the fat-containing aponeurotic space. The position of the levator-skin linkage and the anterior-posterior relationship of the preaponeurotic fat determine the lid fold height and degree of sulcus concavity or convexity. In the deep-set eyelid or in the case of levator dehiscence from the tarsal plate, the upper lid crease is displaced superiorly, measuring 8 to 13 mm from the lid margin. The orbital septum and preaponeurotic fat linked to the levator are displaced superiorly and posteriorly. These anatomic changes create a lid crease; a deep superior sulcus; and, in the case of levator dehiscence, eyelid ptosis.2–4,17–23 Fig. 22.8a demonstrates a patient with levator dehiscence and overresection of fat after a blepharoplasty by a referring plastic surgeon. Fig. 22.8b identifies the levator dehiscence intraoperatively. Fig. 22.7 Key components of the preoperative examination for an upper and lower lid blepharoplasty. (a) A basic Snellen chart should be used before surgery with all patients undergoing eyelid procedures to document their baseline visual acuity. (b) Schirmer’s test strips measure baseline tear production. (c) A lower lid snap-back test. (d) The relationship of the anterior globe vector to the midfacial skeletal support in a youthful face and malar support. (e) A Bell’s reflex test with a normal result. (a From Codner MA, McCord, CD Jr. Eyelid and Periorbital Surgery. 2nd ed. New York: Thieme Medical; 2016.) Fig. 22.8 (a) This patient had levator dehiscence and overresection of fat after a blepharoplasty by a referring plastic surgeon. (b) The levator dehiscence of the same patient. Fig. 22.9 A herniated lacrimal gland after an upper lid blepharoplasty by a referring plastic surgeon. In the aging or baggy eyelid, the septum becomes attenuated and stretches. The preaponeurotic fat attachments loosen, and this attenuation allows orbital fat to prolapse forward and slide over the levator into an anterior and inferior position. The net result is an inferior displacement of the levator skin attachments and a low and anterior position of the preaponeurotic fat pad. Clinically, this transposition results in a low lid crease that is only a few millimeters from the lid margin and may not be visible because of the overhanging lid. The youthful Asian eyelid anatomically resembles the baggy or senescent upper lid with a low levator skin zone of adhesion and an inferiorly, anteriorly located preaponeurotic fat. The characteristic, but variable, low eyelid crease and convex upper eyelid sulcus are classic.2–4,17–23 The four anatomic variations in the upper eyelid displayed by different ethnic groups and the changes associated with senescence within each group allow for a convergence of anatomy. Many of these ethnic differences are erased by aging or attenuation of structures, allowing for a unified lid concept. Before an upper lid blepharoplasty, the upper eyelid topography should be categorized with a tailored approach to treat the pathology.2–4,17–23 In planning and executing the upper lid blepharoplasty, the surgeon must first determine the endogenous lid crease or the height at which to create a new lid crease (if different from the existing crease). Of note, a new lid crease would require supratarsal fixation. The level of the lid crease serves as the lower limb of the blepharoplasty incision and the height of supratarsal fixation, if indicated. The width or extent of skin excision is determined by pinching the lid skin between forceps and using slight lash line eversion as the end point. This superior mark will determine the location for the superior limb of the skin incision.2–4,17–23 Concurrently, the extent of lateral eyebrow ptosis and the amount of lateral upper eyelid hooding should be determined. The degree of lateral hooding will dictate the lateral extent of the incision. In general, incisions that extend beyond the orbital rim are not well tolerated. The upper and lower limbs typically have unequal lengths to eliminate dog-ears and must be exaggerated as when widening the lateral skin excision. Sometimes, a balance must be made between the extent of lateral hooding and maintaining the incision lines within the confines of the orbital rim. Of note, if the lateral extent of the incision becomes excessive, then a lateral brow suspension should be entertained. In addition, an enlarged or herniated lacrimal gland can also produce fullness of the lateral portion of the upper eyelid. The lacrimal gland can be resuspended or plicated; excision of the gland is discouraged because of the risk of dry eye syndrome.2–4,17–23 Fig. 22.9 demonstrates a herniated lacrimal gland after an upper lid blepharoplasty by a referring plastic surgeon. In practice, the upper lid blepharoplasty can be efficiently performed using a few technical manipulations consistent with the anatomy. Digital traction and light pressure by the surgeon or assistant allow smooth, quick incisions. Slightly more pressure must be exerted on the scalpel laterally as the skin thickens. The skin may be elevated with the orbicularis muscle with a needle-tipped, insulated cautery; resection can be optimized by transposing the myocutaneous flap superonasally while providing digital traction laterally. The orbital septum may be stabbed or widely incised, exposing the preaponeurotic space. The underlying levator aponeurosis is protected by opening the septum as cephalad as possible, because the levator and septum diverge as one moves superiorly.2–4,17–23 Fat will prolapse spontaneously or with light digital pressure. The medial fat is whiter and lies medial to the superior oblique muscle. The central or preaponeurotic fat is darker and less fibrous. Care should be taken not to overly resect fat when using digital pressure techniques. Excessive traction and manipulation of fat could cause a deep orbital hemorrhage and should therefore be avoided. Closure may then be performed; I (H.M.S.) prefer 6–0 nylon interrupted sutures laterally and 5–0 nylon intracuticular sutures medially.2–4,17–23 Once the upper lid skin is incised or excised, the levator may be modified (shortened or lengthened) by various interventions, including plicating the levator muscle alone, removing a strip and apposing the cut ends, or plicating and removing the excess levator above the suture line.2–4,17–23 Fig. 22.10 demonstrates intraoperative levator advancement sutures. The skin edges may also be incorporated in these modifications to accentuate or move the lid crease (supratarsal fixation). These changes may be performed alone or in combination and may be used freely with the standard upper lid blepharoplasty. Fig. 22.11 outlines the planning and execution of an upper eyelid blepharoplasty.3
22
Blepharoplasty
Anatomy
Skin
Orbicularis Oculi
Tarsal Plates
Septum
Postseptal (Intraorbital) Fat
Preseptal (Extraorbital) Fat
Upper Eyelid Retractors
Lower Eyelid Retractors
Lateral Canthus
Medial Canthus
Avoiding Unfavorable Results and Complications in Blepharoplasty
Patient Evaluation
Medical History
Physical Examination
Upper Lid Blepharoplasty
Plastic Surgery Key
Fastest Plastic Surgery & Dermatology Insight Engine