Key points
- •
Fifteen different dermal fillers.
- •
Contraindications.
- •
Correct injection techniques.
- •
Early complications due to technique.
- •
Late complications due to fillers.
- •
Treatment of complications.
Introduction
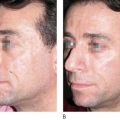
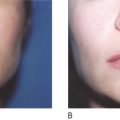
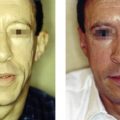
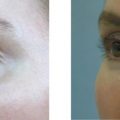
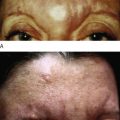
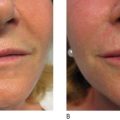
All fillers are associated with a risk of both early and late complications. Early side-effects like swelling, redness, and bruising occur after intra- or subdermal injections. The patient must be made aware of and accept these. Adverse events that last longer than 2 weeks can be due to technical shortcomings, e.g. too superficial an implantation of a long-lasting filler substance. Such adverse events can be treated with intradermal 5-fluorouracil, steroid injections, vascular lasers, or intense pulsed light (IPL), and later with dermabrasion or shaving. Late adverse events also include immunological phenomena such as late-onset allergy and non-allergic foreign body granulomas (FBG). Both react well to intralesional steroid injections, which often have to be repeated in order to establish the right dose. Surgical excisions remain the last option and are indicated for hard lumps in the lips and visible hard nodules or hard granuloma in the subcutaneous fat.
All injectable dermal fillers can cause complications. Late side-effects can be divided into those caused by insufficient training or technical errors during injection and those caused by immunologic (allergic as well as non-allergic) reactions to the injected substance. In the case of late, non-allergic reactions, the pathological substratum differs between injectables but can always be classified into one of three distinct forms of FBG ( ). The histological reaction is always similar ( ) and the trigger for this sudden stimulation of macrophages might be a systemic infection of the patient ( ).
Dermal fillers
Fluid silicone and bovine collagen, Artecoll® and Restylane® are used worldwide ( , ). The first of these, medical grade fluid silicone of 350 centistokes (cSt), was manufactured by Dow Corning Inc. from 1954–1992, but banned by the FDA in 1967 for cosmetic use ( ). A more viscous product Silikon® 1000 was approved for retinal reattachment from 1998 and used off-label as a dermal filler. Bovine collagen (Zyderm®, Zyplast®) was introduced in 1981 and 1983 and became the gold standard for injectables. Artecoll® has been distributed since 1994, and Restylane® started its triumphant advance in 1997. Since that time, a variety of fillers have been introduced, mainly to the European market. Radiesse® has been approved for facial bone augmentation since 2003 and for wrinkle treatment since 2007. Sculptra™ is approved for facial HIV-lipodystrophy but used ‘off-label’ for wrinkle treatment since 2005. The FDA approved Restylane® in 2003, Hylaform® in 2004, Captique™ in 2005, and Juvéderm® in 2006 for the treatment of facial wrinkles.
The clinical persistence of an injectable and its effect on wrinkles depends on its chemical structure, the amount used, and the depth at which the implant is injected ( Table 11.1 ). A thin strand applied beneath a constantly moving wrinkle on a human face is absorbed faster than a round depot beneath the skin on a rat forehead or a human forearm ( ). The carrier substance, whether quickly or slowly absorbed, may also play an important role in persistence. So far, none of the implants with the exception of silicone, polyacrylamide, and PMMA is palpable for longer than 9 months ( ), although some, like Juvéderm®, Radiesse® and Restylane® may be visible for up to 12 months. Radiesse® and Sculptra™ persist even longer, sometimes lasting up to 2–3 years.
| Brand name | Active ingredient | Mechanism of action | Bio-degradable | Persistence in tissue |
|---|---|---|---|---|
| Zyderm ® | Collagen | Volumizer | Yes | 4 months |
| Restylane ® | Hyal. acid | Volumizer | Yes | 6 months |
| ArteFill ® | PMMA | Stimulator | No | Permanent |
| Silikon ® 1000 | Silicone | Volumizer | No | Permanent |
| Radiesse ® | Ca apatite | Volumizer | Yes | 1 year |
| Sculptra ® | PLLA | Stimulator | Yes | 1 year |
| Autologous fat | Living fat | Volumizer | Yes/No | Unpredictable |
Although all filler substances, resorbable or non-resorbable, appear to be clinically and histologically safe, all may exhibit undesirable clinical side-effects, and host defense mechanisms react differently to the differing filler materials ( ). According to the histological reaction that fillers stimulate, they have been classified as ‘volumateurs’ with little cellular invasion, and ‘stimulateurs’ with strong cellular reactions ( ). Since the mechanism of late inflammation or granuloma formation is still unknown, early histological findings are not useful in predicting possible late reactions to filler substances. Such late complications can be confirmed only in rigorous long-term clinical studies, and in government-enforced reporting to a centralized independent Implant Registry.
In order to avoid or treat complications with dermal fillers, the knowledge of their composition, physiological tissue reactions, absorption time, and persistence is indispensible. Therefore, the fillers that are well-known and available worldwide are described below with respect to one or more of these characteristics.
Autologous fat grafts
- •
Liposculpture: with the patient’s own fat.
- •
Pre-adipocytes (Fidia Advanced Biopolymers, Padua, Italy): no clinical data yet.
- •
Stem cells from adipose tissue (Cytori, Inc., San Diego, CA): no clinical data yet.
Autologous fat is rarely permanent and its fate is unpredictable. There are convincing anecdotal cases published ( ) but no statistics are available on fat graft survival. The key to long-term survival of injected fat, i.e. the development of functional pre-adipocyte or stem cell cultures, has yet to be discovered. What happens to the surviving fat cells in the face if patients become obese is not well known or well documented.
Bovine collagen
- •
Zyderm ® I, II and Zyplast ® (Inamed Aesthetics, Santa Barbara, CA): FDA approved.
- •
Koken Atelocollagen ® (Koken, Tokyo, Japan)
Porcine collagen
- •
Permacol ® (Tissue Science Labs., Aldershot, UK).
- •
Fibroquel ® (Aspid, Mexico).
- •
Evolence ™ (ColBar LifeScience, Herzliya, Israel): The company claims that Evolence lasts for 1–2 years but this has still to be clinically proven.
Human collagen
- •
Cosmoderm ® , Cosmoplast ® (Inamed Aesthetics, Santa Barbara, CA): FDA approved.
- •
Isolagen ® (Isolagen Technologies, Houston, TX): collagen from patient’s own cultured fibroblasts, currently in clinical trials.
- •
Fascian ® (Fascia Biosystems, Beverly Hills, CA): strips from human fascia; FDA approved.
- •
Cymetra ® (Lifecell, Branchburg, NJ): injectable micro-particles from human skin; FDA approved.
So far, all collagen preparations disappear clinically within 4–6 months and are histologically absorbed between 3 and 9 months depending on the volume injected ( ). Cultured autologous fibroblasts (Isolagen) have yet to demonstrate their survival and effectiveness.
Hyaluronic acid gels
- •
Restylane ® : FDA approved; Perlane ® , Restylane Fineline ® , SubQ ™ , Macrolane ™ (Q-Med, Uppsala, Sweden and Medicis Aesthetics, Scottsdale, AZ) derived from Streptococcus equi .
- •
Hylaform ® (Inamed Aesthetics, Santa Barbara, CA); from rooster combs; Hylaform Plus™, Hylaform Fineline™: all FDA approved.
- •
Juvéderm ® 18, 24, 30 (Leaderm, Paris and Inamed Aesthetics, Santa Barbara, CA). From Streptoccocus equi ; FDA approved.
- •
Rofilan Hylan Gel™ (Rofil Medical International RMI, Breda, The Netherlands).
- •
AcHyal ™ (Tedec-Meiji Farma, Spain).
- •
Matridur ® (BioPolymer, Siershahn, Germany).
- •
Hyal-System ® (Merz Pharma, Frankfurt Germany): for two-dimensional augmentation.
- •
Puragen ™ , Prevell ™ (Mentor Corp., Santa Barbara, CA): contain lidocaine.
Natural fillers such as collagen and hyaluronic acids are broken down by enzymes, absorbed or phagocytosed slowly with minimal histological reaction. After further purification of Restylane® in 1999, its incidence of complications has been markedly reduced.
Polymethylmethacrylate (PMMA) microspheres
- •
Artecoll ® (Rofil Medical International (RMI), Breda, The Netherlands) consists of microspheres 30–42 µm in diameter, suspended in European bovine collagen.
- •
ArteFill ® (Artes Medical, San Diego, CA) consists of highly purified microspheres 30–50 µm in diameter, suspended in US bovine collagen: FDA approved.
- •
ArteSense ™ (European Medical Contract Manufacturer EMCM, Nijmegen, The Netherlands), similar to Artecoll, approved in Canada.
- •
MetaCrill ® (Nutricel Laboratorios, Rio de Janeiro, Brazil); PMMA microspheres 1–80 µm in diameter, with impurities similar to those of the former Arteplast, suspended in carboxygluconate gel, approved in Brazil.
- •
NewPlastic ® (Biomedical Comercio, Porto Alegre, Brazil), similar to MetaCrill, approved in Brazil.
- •
Precise ™ (Clinica Estetica, Tijuana, Mexico), similar to NewPlastic ® .
PMMA microspheres remain unchanged throughout the patient’s life but are encapsulated individually with connective tissue, macrophages, and sporadic giant cells. They provide scaffolds for continuously renewed connective tissue formation and vascularity ( ).
Silicone fluids
- •
Silikon 1000 ™ (Alcon Laboratories, Fort Worth, TX) is FDA-approved for retinal re-attachment since 1998.
- •
SilSkin ™ , 1000 cSt (Richard-James Development Corp., Peabody, MA) is currently in clinical trials for facial wrinkles but is not FDA approved.
- •
PMS 350 ™ (Vicomed, Germany) is fluid silicone of low viscosity (350 cSt) similar to the former Silicone 350 from Dow Corning.
Resorbable fluid fillers, such as fluid silicone ( , , ) and polyacrylamides dissipate slowly into the tissue, are clinically inconspicuous and cause little fibrosis. Large volumes, however, can dislocate in patients with loose connective tissue through muscle movement and gravity. They are considered ‘inert implants’ ( ).
Polyacrylamide gels
- •
Aquamid ® (Ferrosan AS, Copenhagen, Denmark) polyacrylamide gel 2.5% in water.
- •
Interfall ® (Interfall Ltd., Kiev, Ukraine).
- •
Bio-Alcamid ® (Polymekon, Milan, Italy); 4% polyacrylamide crosslinked with polyalkylimide.
- •
Outline ® (ProCytech, Bordeaux, France) is temporary and absorbed within 1–2 years.
- •
Amazing Gel ® (FuHua Ltd., ShenZhen, China).
- •
Formacryl ® (Bioform, Moscow).
- •
Argiform ® (Bioform, Moscow) contains silver ions as antibiotic.
Polyacrylamide gels are well tolerated ( ) and slowly absorbed by the body over many years. They either dissipate (Aquamid®) like fluid silicone or are kept in place (Bio-Alcamid®) by means of a fibrous capsule (endoprosthesis). The effect of polyacrylamide gels on wrinkles has not undergone sufficient clinical and scientific testing. Like silicone, polyacrylamide causes a high incidence of late complications if injected in large quantities ( ).
Other injectables
- •
Radiesse ® (Bioform Inc., San Matteo, CA); calcium-hydroxylapatite (constituent of bone and teeth) microspheres of 40 µm suspended in carboxymethylcellulose gel. When the cellulose is absorbed, the calcium microspheres often appear white beneath the vermilion or thin skin. It is a safe injectable, induces almost no foreign body reaction and is absorbed in 9–12 months ( ).
- •
Dermalive ® and Dermadeep ® (Dermatech, Paris). Hydroxyethylmethacrylate (HEMA) particles are suspended in hyaluronic acid. HEMA particles are packed after injection and absorbed and phagocytized within 1–2 years ( ). They cause the highest rate of granulomas ( ) and should only be used epiperiosteally if at all.
- •
New-Fill ® /Sculptra ™ (Sanofi-Aventis, Strasbourg and Dermik Aesthetics, Berwyn, PA) consists of microspheres from polylactic acid (1–50 µm) suspended in methylcellulose. New-Fill/Sculptra ™ appears to be safe and effective in larger quantities in facial defects like facial lipodystrophy or chin and malar augmentation. The microspheres induce an inflammatory response and foreign body reaction, and clinically disappear beneath wrinkles at 6–9 months ( ). Their ‘skin-thickening effect’ after injections into the residual subcutaneous fat in HIV patients with facial lipodystrophy is not yet understood, but persists for 2 years or longer.
- •
Matridex ® (BioPolymer, Siershahn, Germany) consists of dextran beads of 40 µm suspended in hyaluronic acid (after FDA approval, it will be distributed in the USA by AART, Reno, NV).
- •
Reviderm Intra ® (Rofil Medical Int., Breda, Holland) consists of dextran beads of 40 µm in diameter suspended in hyaluronic acid. Dextran microspheres induce a pronounced foreign body reaction and disappear within 6–9 months ( ).
- •
Evolution ® (ProCytech Labs., Bordeaux, France) consists of polyvinyl microspheres suspended in a rather fast absorbable polyacrylamide gel. The microspheres are well tolerated and permanent, while the gel diminishes clinically and histologically over 9 months ( ).
- •
Bion-Blue ® (Polymekon, Milan, Italy) is an 8% polyvinyl-alcohol (PVA) gel, which is absorbed quickly.
Avoiding complications
Patients who are contemplating a wrinkle treatment for the first time and are unsure about their options should try a collagen or hyaluronic acid. If patients are satisfied but do not want to repeat treatment every 6 to 12 months, they should consider a longer-lasting injectable like Sculptra™ or Radiesse®, or a permanent injectable like silicone or TG TMMP.
Physicians may reduce the risk of complications by selecting appropriate patients and by employing proper injection technique ( ). There are anecdotal reports that patients who have a tendency towards keloid or hypertophic scar formation, developed granuloma in both sites injected with dermal fillers. There are also reports of patients with sarcoidosis, who developed a similar histological pattern at injected sites. However, because of the small numbers of patients involved, a relationship between hypertrophic scarring or sarcoidosis and susceptibility to FBG cannot be established at this time.
Considerations
Thin skin
In general, thin skin of 0.4 mm in thickness, i.e., the eyelids and in cheeks that have many tiny wrinkles is a contraindication for all fillers. In such sites, laser resurfacing or a chemical peel is the treatment of choice.
Temporary treatment of lips before a permanent filler
Prior injections of collagen can cause scar formation beneath the vermilion border, which may lead to unevenness or asymmetries when a permanent filler is injected. These fine lumps and bumps can easily be corrected, preferably 3 months later, as long as the patient does not object to waiting for this period.
Laser treatment after dermal fillers
Most lasers cause a burn injury to the superficial dermis, which forces it to contract. All longer-lasting implants lie subdermally and are not affected by the laser rays or its induction of high temperature. Lasers exert heat well below the approximate melting point of silicone (600°C) and PMMA (125°C). Deep wrinkles, which will withstand laser treatment, can even be injected with a longer lasting filler directly before laser therapy; the concomitant swelling facilitates the effect of the laser.
Permanent makeup on top of injectables
Permanent make-up is delivered to the upper papillary dermis, while particulate fillers are delivered to the junction between the dermis and the subdermis, so there is no interference between these two agents. A mature ArteFill® implant, for example, behaves like a scar; it is a living tissue that can be tattooed, lasered, dermabraded, or peeled. Like a scar but unlike pure fillers (volumenizers) an ArteFill® implant heals by itself ( ).
Temporary filler on top of a permanent filler
To date, there is no report of any patient with an untoward reaction to a second filler implanted over another filler. Fear of inducing granuloma formation is therefore hypothetical at this time.
Temporary filler preceding a permanent filler
In Europe, thousands of patients received semi-permanent or permanent fillers after temporary fillers, and no interference between the two has been reported thus far.
Visibility of permanent implant as patients age
Although the thickness of the skin at the extremities decreases in old age, the facial skin thickens with age ( ). Therefore, permanent implants beneath the nasolabial folds will not become visible, even in patients in their nineties.
Touch-up injections
Most patients will require one to three touch-up injections. These should be performed 1–3 months after the first implantation unless there is a reason, such as unevenness, or asymmetry, to do it earlier. After 3 months, a permanent implant has assumed its final shape, and the wrinkle above it has been restored to the thickness of the surrounding skin.
Weather conditions
Two patients developed longer lasting swelling of their injected lips after driving a snow mobile all day in Northern Canada. Therefore, the lower face should be covered during cold weather sports such as skiing or mountain climbing, and during any other exposure to extreme cold.
Questionable contraindications
Autoimmune diseases and collagen
In the early nineties, some physicians and lawyers claimed a correlation between collagen injections and subsequent polymyositis and dermatomyositis in some patients. The FDA took this possibility very seriously but decided in 1995 that ‘a causal relationship between collagen injections and PM/DM or other connective tissue diseases listed, has not been established’.
Compatibility of different fillers
Several physicians inject Restylane® (or other collagen or hyaluronic acid fillers) intradermally, directly on top of the subdermal implant of a longer-lasting filler in the same session for treating glabellar frown lines, without any reported adverse events.
Diabetes
Since wound healing is normal in these patients, except for neurological foot ulcers, diabetes is not a contraindication to any filler.
HIV patients
The microspheres in some products, such as ArteFill®, stimulate simple granulation (scar tissue) formation similar to that associated with surgical or traumatic wounds. Immune deficiency and HAART are not contraindications.
Immuno-depressed patients
In general, wound healing is not delayed in these patients, since fibroblasts need an approximately 10-fold higher concentration of immunosuppressive therapy than immunocytes do to be affected. Therefore, immune depression is not necessarily a contraindication to any kind of filler.
Lupus
Systemic lupus is an autoimmune disease characterized by anti-DNA antibodies. The FDA has dismissed any correlation of collagen injections with autoimmune diseases. So far, systemic lupus is not a contraindication for dermal fillers.
Rheumatoid disease and fillers
Particles and microspheres stimulate granulation (scar tissue) formation as in surgical or traumatic wounds. Theoretically, collagen synthesis could be over-stimulated, but this does not occur in patients with rheumatoid diseases. If wound healing is normal, rheumatoid disease is not a contraindication for dermal fillers.
Scleroderma
Since wound healing is normal in scleroderma patients, dermal fillers are not a contraindication.
Sebaceous skin
Thick, oily skin is associated with fewer and later wrinkles. Patients with such skin are ideal candidates for two to three sessions of particulate fillers. However, during implantation, deep pores may be inadvertently hit, possibly causing a subsequent leak or pustule of the filler.
Skin types
In general, lighter skin types are more prone to allergic reactions than darker complexions. Problems with fillers, however, have only occurred in patients with extremely thin skin, where even subdermal injections can end up close to the epidermis.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree