Key Term
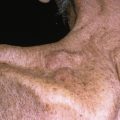
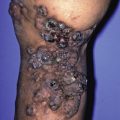
Erythema chronicum migrans
Annular and targetoid lesions are distinct clinical configurations that include many common disorders, such as dermatophyte infections, granuloma annulare, various reactive conditions, and even serious diseases (e.g., Lyme disease, leprosy).
Without Scale
- •
Actinic granuloma
- •
Borderline leprosy (can have scale)
- •
Erythema annulare centrifugum (see below)
- •
Erythema chronicum migrans
- •
Erythema multiforme
- •
Erythema marginatum
- •
Granuloma annulare
- •
Necrobiosis lipoidica
- •
Neonatal lupus erythematosus (can have scale)
- •
Subacute lupus erythematosus
With Scale
- •
Erythema annulare centrifugum (see above)
- •
Pityriasis rosea
- •
Seborrheic dermatitis (seborrhea petaloides)
- •
Tinea corporis, tinea cruris, tinea faciei
- •
Tuberculoid leprosy
Important History Questions
How long have the lesions been present?
This question is useful in distinguishing among disorders that are typically acute, such as erythema migrans and erythema multiforme, and conditions that tend to be chronic, such as granuloma annulare, tuberculoid leprosy, and necrobiosis lipoidica.
Have you had a similar rash in the past?
Erythema multiforme, for example, tends to occur as repetitive episodes.
What medications do you take?
A medication history is important because erythema multiforme and erythema annulare centrifugum may be drug induced.
Where have you lived?
Leprosy is endemic to much of the world, including, in the United States, Texas and Louisiana.
Where have you been recently?
Travel to an area of the country where Lyme disease is endemic is important (see box).
Have you been camping outdoors or with animals?
Lyme disease is caused by a tick bite, and it is also useful to inquire directly about insect and arthropod bites.
Are you diabetic?
Necrobiosis lipoidica diabeticorum and, to a slightly lesser extent, granuloma annulare are both associated with diabetes.
Important Physical Findings
Do the lesions demonstrate scale?
This is an important clinical feature because dermatophyte infections and erythema annulare centrifugum typically demonstrate scale, whereas granuloma annulare, erythema marginatum, and erythema migrans typically lack appreciable scale.
What is the distribution of the lesions?
Distribution is important because some diseases have a characteristic pattern. For example, necrobiosis lipoidica usually affects the pretibial surface, whereas erythema multiforme often involves distal acral skin. Symmetric distribution may also be more characteristic of a systemic reactive condition. Also, some diseases, such as actinic granuloma and neonatal lupus erythematosus, may be photodistributed.
Are there any mucosal lesions?
The presence of mucosal lesions (e.g., ocular, oral, genital) is an important finding in erythema multiforme.
 Tinea Corporis, Tinea Faciei, and Tinea Cruris
Tinea Corporis, Tinea Faciei, and Tinea Cruris
ICD10 codes B35.4, B35.6
FUNGAL INFECTION
Introduction
When dermatophytes affect glabrous skin, such as the face, groin, and trunk, annular lesions often result—hence, the common name, “ringworm.” Dermatophyte infections are usually acquired from other humans but may also be acquired from other animals and from the soil. The three species most often associated with cutaneous infections in humans include Trichophyton rubrum, Trichophyton mentagrophytes, and Epidermophyton floccosum . Outbreaks may be seen among people in close contact, such as wrestling teams (tinea corporis gladiatorum) prisoners or persons who are institutionalized.
Clinical Features
- •
The primary lesion in dermatophyte infections is an erythematous annular plaque that is nearly always scaly ( Figs. 16.1 and 16.2 ), particularly at the peripheral edge. The amount of scale is variable.
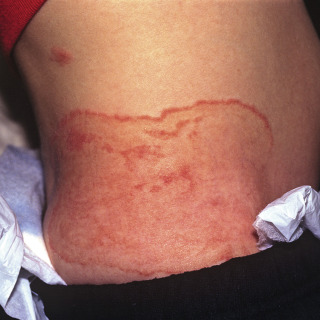
Fig. 16.1
Patient with tinea corporis, with highly inflammatory annular lesions. Note that a very early lesion is not yet annulare.
(From the William Weston Collection, Aurora, CO.)
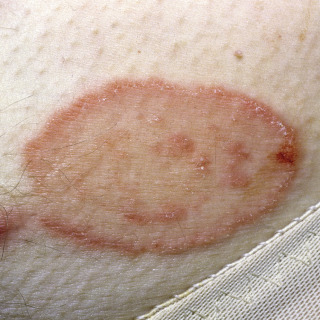
Fig. 16.2
Close-up of a lesion of tinea corporis. Note the trailing scale. The blood is the result of overzealous scraping for a potassium hydroxide (KOH) preparation.
- •
Rarely, concentric annular lesions may resemble a topographic map.
- •
In tinea cruris (so-called jock itch), the lesions typically involve the inguinal crease and characteristically spare the scrotum ( Fig. 16.3 ).
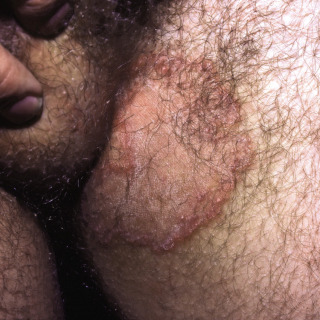
Fig. 16.3
Patient with classic case of tinea cruris, with an annular edge. Note that the scrotum is spared.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
- •
A subset of patients may also demonstrate follicular lesions, especially if a topical corticosteroid has been used by the patient, causing localized immunosuppression.
- •
In rare cases, the peripheral edge may be pustular, or bullae may form ( Fig. 16.4 ).
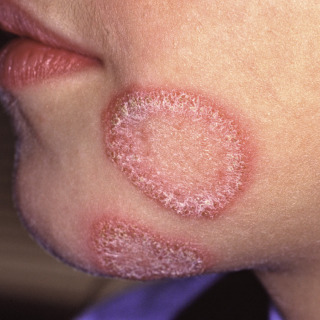
Fig. 16.4
Patient with tinea faciei presenting as annular lesions with marked induration and scale to the point that papulosquamous disease, such as psoriasis, is in the clinical differential diagnosis.
Diagnosis
- •
In many cases, the diagnosis may be strongly suspected on clinical grounds, but it is important to remember that even skilled dermatologists may mistake erythema annulare centrifugum, granuloma annulare, and even tuberculoid leprosy, for a dermatophyte infection.
- •
A potassium hydroxide (KOH) preparation, taken from the active edge of the lesion and examined by skilled persons, is diagnostic (see Chapter 2 ).
- •
A culture of scrapings from the active edge may also be diagnostic.
- •
The diagnosis may also be made by a skin biopsy, although clearly it is prudent not to perform a biopsy unless necessary. Also, a pathologist may miss the organism without use of special stains, so it is important for clinicians to indicate suspicion of a fungal infection on submission.
Treatment
- •
First-line treatment of uncomplicated dermatophyte infections of glabrous skin includes topical allylamines, such as terbinafine cream 1%, available over the counter, applied bid to affected areas for 1 week beyond any visible infection. This usually takes 2 to 3 weeks.
- •
Near-equivalence is seen with topical azoles (e.g., clotrimazole, miconazole) and ciclopirox olamine.
- •
Systemic therapy should be considered for patients with extensive or follicular involvement. Typically, oral terbinafine (250 mg/day for 7–14 days) or itraconazole (100–200 mg/day for 7–14 days) is used in these cases.
- •
Tinea infections among athletes may require evaluation of the entire team to prevent or mitigate a larger outbreak. Most cases are acquired by skin-to-skin contact, although rare cases may be acquired from fomites (e.g., wrestling mats). Fomites (e.g., headgear, padding) should be cleaned and not shared.
- •
Infected teams should be treated with oral medications, if possible, until the outbreak has been controlled.
Lyme Disease
ICD10 code L92.0
BACTERIAL INFECTION
Pathogenesis
Lyme disease is a tickborne systemic infection caused by the spirochete, Borrelia burgdorferi. The most common vectors in the United States are the deer tick (Ixodes scapularis) and, in the western United States, the black-legged tick (Ixodes pacificus). Although adults and nymphs may transmit the disease, the nymphs are more often the source of infection. Lyme disease has been reported in nearly every state, but a travel history is often involved (see box, above) outside of the East Coast, West Coast, or Great Lakes areas. Because of increased outdoor exposure during the summer months, children are affected more often than adults.
Clinical Features
- •
In many cases, history of a tick bite cannot be elicited.
- •
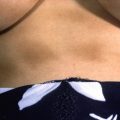
Skin lesions appear between 3 and 30 days after tick attachment, with an average of 9 days.
- •
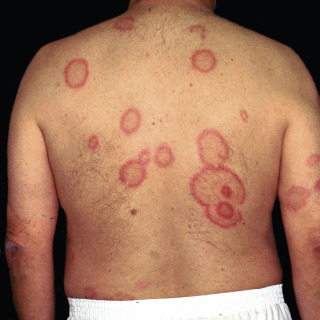
The primary lesion is an annular ring of erythema, with variable induration (erythema chronicum migrans), which expands at a rate of 1 to 2 cm/day and may reach up to 60 cm in greatest diameter ( Fig. 16.5 ).
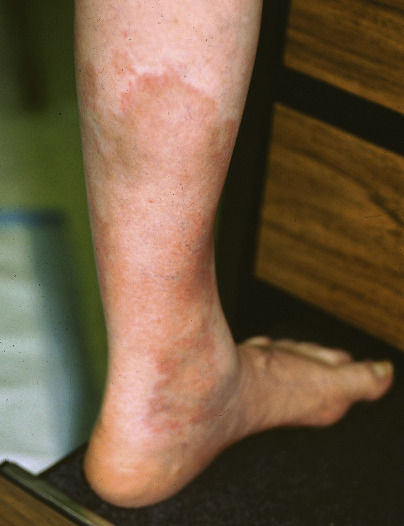
Fig. 16.5
Patient with large, irregular, annular lesion of the lower leg, with a small secondary lesion at the superior pole.
(From the William Weston Collection, Aurora, CO.)
- •
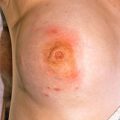
A small central papule that represents the tick bite may (or may not) be observed, which may give the appearance of a bull’s eye ( Fig. 16.6 ).
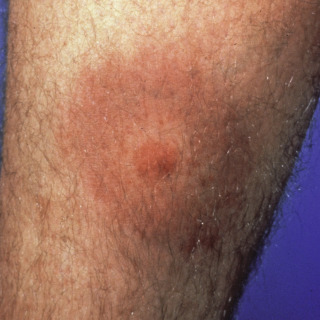
Fig. 16.6
Patient with annular lesion with central bull’s eye that represents the site of the tick attachment.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
- •
Lesions may be pruritic.
- •
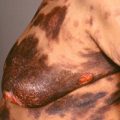
The primary lesion lasts up to 4 weeks and may become hemorrhagic ( Fig. 16.7 ).
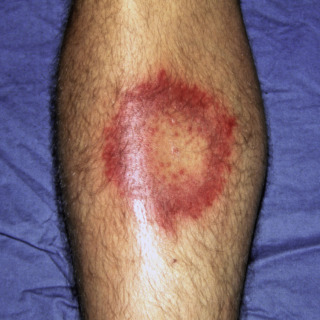
Fig. 16.7
Patient with hemorrhagic annular variant of erythema chronicum migrans.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
- •
Some patients may get one or more secondary smaller annular lesions (from spirochetemia).
- •
Associated constitutional findings include fever, lymphadenopathy, headache, and malaise.
Diagnosis
- •
An erythematous annular lesion after travel to a highly endemic area should raise suspicion of erythema migrans.
- •
Punch biopsy of a skin lesion for culture (modified Barbour-Stoenner-Kelly medium) is the only diagnostic test and is positive in about 75% of cases within 4 weeks. This technique is not widely available.
- •
Serologic screening tests include the enzyme-linked immunosorbent assay (ELISA), but immunoglobulin M (IgM) titers become positive after 30 days, and IgG titers become positive between 45 and 60 days; this is not the period in which the rash is observed.
- •
A 4- to 6-mm punch biopsy can manifest features that are consistent with but not only diagnostic of erythema migrans. In about one-third of cases, special stains may demonstrate the spirochete.
Treatment
- •
Prophylactic treatment of tick bites is controversial, but, at present, it is reasonable to treat patients in endemic areas with a single dose of doxycycline (200 mg) within 72 hours of a tick bite.
- •
Adults with suspected or documented erythema migrans are treated with doxycycline (100 mg PO bid for 14–21 days), amoxicillin (500 mg PO tid for 14–21 days), or cefuroxime axetil (500 mg bid for 14–21 days). Doxycycline is also effective against human granulocytic ehrlichiosis, which is a co-infection seen in about 10% of Lyme disease cases.
- •
Children with suspected or documented erythema migrans may be treated with doxycycline (100 mg PO bid for 14–21 days) if older than 9 years, amoxicillin (30–50 mg/kg per day for 14–21 days), erythromycin (30 mg/kg per day for 14–21 days), or phenoxymethylpenicillin (25–50 mg/kg per day for 14–21 days).
Clinical Course
Untreated erythema chronicum migrans can result in disseminated disease that may involve other organ systems.
Erythema Annulare Centrifugum
ICD10 code L53.1
INTERNAL DISORDER
Pathogenesis
Erythema annulare centrifugum (EAC), like urticaria or erythema multiforme, is a reactive condition that can result from multiple immunologic stimuli or other systemic perturbations of homeostasis, even conditions such as pregnancy. The precise immunologic mechanism whereby it develops is not well understood.
- •
Infections
- •
Candidiasis
- •
Dermatophyte infections
- •
Viral infections (molluscum contagiosum, herpes zoster)
- •
- •
Infestations
- •
Ascariasis
- •
Phthirus pubis
- •
- •
Medications
- •
Amitriptyline
- •
Ampicillin
- •
Antimalarials
- •
Cimetidine
- •
Finasteride
- •
Gold
- •
Hydrochlorothiazide
- •
Nonsteroidal antiinflammatory drugs (NSAIDs)
- •
Piroxicam
- •
Thiacetazone
- •
- •
Foods
- •
Blue cheese ( Penicillium )
- •
- •
Internal malignancies
- •
Pregnancy
Clinical Features
- •
No predilection exists regarding gender, race, or age.
- •
Multiple lesions are usually present.
- •
Superficial variants of EAC present as annular or polycyclic lesions, with an erythematous edge and trailing scale, which extend in centrifugal fashion ( Figs. 16.8 to 16.10 ).