Abstract
Dermatologic, oncological, and aesthetic surgery require an intimate knowledge of the bony structures, muscles, vessels, and nerves of the head and neck. They also require an understanding of their relationship to each other, as well as the tissue planes and supporting structures in which they reside. Preservation of function and appearance is the definitive goal of surgical intervention and depends upon the intimate familiarity of the structural and functional anatomy. Awareness of the constant evolution in our understanding and variations of anatomic knowledge require continued vigilance to remain proficient.
Keywords
regional anatomy, anatomic variation, retaining ligaments, fat compartments, skeletal aging
Introduction
A working knowledge of anatomy is essential to perform any of the myriad of procedures in dermatologic surgery. Most surgical skills, even the basic ones, such as scar orientation and level of undermining, are predicated on a basic command of anatomy. More complicated tasks, such as nerve block anesthesia, designing tissue flaps and grafts for advanced repair of surgical defects, and the placement of botulinum toxin and fillers, require an even more intimate understanding. Without an in-depth working understanding of the pertinent anatomy, there is a real potential for the surgeon to cause damage by cutting into a vital structure or to be so insecure as to not progress in one’s acquisition of sophisticated surgical skills.
Surface Landmarks and Surface Anatomy
Being a keen observer of the surface anatomy of the face enables the surgeon to assess the patient for the vagaries of aging, to identify the reservoirs of redundant skin available for repairs, and to identify optimal placement of scars. It also allows the surgeon to project and visualize the course or location of the deeper vital structures onto the surface.
Masseter Muscle and Midpupillary Line
The masseter muscle is a good starting point. It is the large muscle of mastication that occupies the lateral portion of the cheek below the zygomatic arch ( Fig. 1.1 ). The parotid gland rests on this muscle. At its anterior border on a line drawn from the tragus to the middle of the upper cutaneous lip, the parotid duct can be identified as it dips inward, piercing the buccinator muscle to open into the mouth at the level of the second upper molar. Also, at the jaw line, just at the anterior border of the lower masseter muscle, the facial artery and vein enter onto the face. Pulsation of the artery is often possible at this location. The superficial temporalis artery pulse can be felt just anterior to the ear at its superior attachment. Just beyond this, it splits into superior and parietal branches.
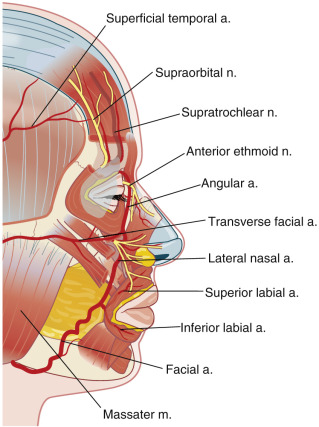
The midpupillary line is identified with the patient sitting up and gazing straight ahead. Three important openings in the skull can be located. The superior orbital foramen is located at the superior orbital rim, often palpable as a notch along the rim. Through it exits the important supraorbital neurovascular complex. Similarly, the infraorbital foramen, about 1 cm below the inferior orbital rim, contains the infraorbital neurovascular artery, vein, and sensory nerve. Finally, the mental foramen, located in the alveolar bone of the mandible in the midpupillary line and just below the canine tooth, contains the mental artery, vein, and nerve. All three foramena may be somewhat medial to the midpupillary line. The exact location of all three of these orifices is important when performing respective nerve blocks of the sensory nerves exiting them.
Relaxed Skin Tension Lines
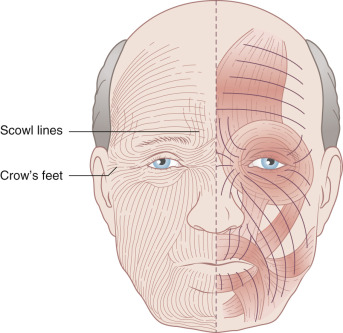
The lines and wrinkles that develop with age and sun exposure become an easily recognizable road map of the face. These wrinkles and creases, first noted as hyperanimation smile lines or frown (scowl) lines, may become permanently etched as elastic tissue degenerates and becomes ineffective in resisting the pull of the underlying muscles of facial expression. These are referred to as the relaxed skin tension lines (RSTLs; Fig. 1.2 ) and run perpendicular to the exertion of the mimetic muscles below. These lines are often the best choice for the placement of elective scar lines on the face. When they are readily apparent, no problem is posed in designing scar orientation. In younger people, having them animate by grimacing, wrinkling the forehead, smiling, or puckering will usually expose the RSTLs sufficiently to make the correct choice. Similarly, pinching the skin from various directions will also reveal the flow of the RSTLs. Scars not oriented within or parallel to the RSTLs are generally more noticeable, as they do not go with “flow” of the region. This is especially apparent when the patient is smiling or going through some other active form of dynamic emotional expression.
Cosmetic Units and Junction Lines
One of the major conceptual advances over the past decade or so in reconstructive and aesthetic surgery is the refinement and widespread acceptance of the junction lines and cosmetic (aesthetic) units of the face ( Fig. 1.3 ). Cosmetic unit junction lines are the lines on the face at the borders of the cosmetic units. They include the well-defined melo-labial fold that separates the cheek from the lip, the mental-labial crease that divides the chin from the cutaneous lower lip, the hairline, and the jaw line. More subtle junction lines separate the cheek from the nose (nasofacial) and lower eyelid from the cheek. The nose has several subunits defined by the alar groove, the dorsal crests, and the nasofacial line. Collectively these are the outlines that caricaturists use along with exaggerated features (broad forehead, wide-set eyes, protruding nose) to rapidly define an individual’s countenance and personality. They are also the best location for camouflaging scars. Since lines and shadows are anticipated in these areas, scars tend to visually disappear when placed within them. Conversely, scars crossing junction lines stand out as noticeable.
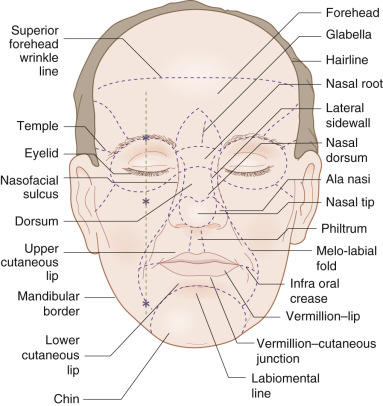
Cosmetic units are the areas cordoned off by the junction lines. They share common characteristics of skin color and texture, pore size, elasticity, thickness, presence or absence of hair, and shading. The cheek, temple, chin, and eyelids are their own well-defined units, whereas the nose, cheek, and ear are subdivided into smaller units. The nose in particular has been defined to include the root, dorsum, lateral side walls, paired alae nasi, soft triangles, columella, and tip.
Several useful principles of closure have been derived from the conceptualization scheme noted previously. These include:
- ▪
Scars should be oriented within junction lines or within or parallel to the RSTLs.
- ▪
Closures should be confined to a single cosmetic unit when possible.
- ▪
When closure is not possible within a single cosmetic unit, skin should be recruited from adjacent units and scar lines oriented so they lie within the intervening junction lines and within or parallel to the RSTLs.
- ▪
When a defect involves several cosmetic units, consider repairing each unit individually.
- ▪
When most of a cosmetic unit or subunit is missing, consider sacrificing the remaining portion and replace the entire unit.
Free Margins: Concept of Tension Vector of Closure
Another important concept when performing facial surgery is that of the free margins—the eyebrows, eyelids, lips, and nostril rims. These structures are extremely important, as they offer little resistance to the forces of wound closure and can be easily distorted by excess tension. This can occur from the immediate direct exertion of tension by a side-to-side closure or the delayed application of tension as a second intention healing wound or split-thickness graft site contracts. The resulting asymmetries can be both cosmetically unsettling and functionally disabling. Ectropion of the lower lid can lead to permanent visual problems, while eclabion and lack of a proper oral seal can cause problems with phonation, eating, and drinking, in addition to being aesthetically unpleasing.
Tension vectors of closure can be favorably manipulated by one of several techniques:
- ▪
Offset bias suturing: Each suture is skewed a bit from its anticipated placement 90 degrees to the long axis. The cumulative effect is to favorably alter the tension vector the requisite number of degrees to avoid pulling the free margin in question out of position.
- ▪
Flaps: Tissue rearrangement is designed so the tension vector is favorably disposed and avoids pulling on free margins.
- ▪
Suspension or anchoring suture: Instead of directing buried suture toward the free margin, a suture is placed from the undersurface of the closure down to and anchored to the underlying periosteum or perichondrium of the area. All tension is then directed downward toward these strong, unyielding structures, and away from the eyelid or eyebrow at risk of being distorted.
- ▪
Full-thickness skin graft: Placement of a full-thickness graft prevents wound contraction and the development of a tension vector of closure in any direction.
Concavities and Convexities: Implications for Second Intention Healing
The face is not a flat structure. Rather, it is composed of undulating well-defined elevations and depressions that need to be taken into consideration when planning closures. Scar lines that traverse from convexity to concavity may contract in an unbecoming manner and may require preplanning with an S-plasty configuration for appropriate closure. However, the major effect of whether an area is flat, concave, or convex determines how well defects resolve when allowed to heal by second intention. Although the size and depth of the defect have some impact on the final healing, defects on concave surfaces such as the temple, the medial canthus, and the alar groove do well, whereas defects on convex surfaces such as the malar eminence, the tip of the nose, and the chin generally heal poorly with webbed or elevated scars. Defects on flat surfaces, such as the forehead or cheek, typically respond somewhere in between.
The Aging Face
With time, predictable wrinkles and sagging take place. This is compounded by changes related to overexposure to ultraviolet radiation in sunlight. Up until 30 years of age, people do not have wrinkles at rest (Glogau I). The RSTLs first appear as hyperanimation lines perpendicular to the pull of the underlying muscles of facial expression (Glogau II). Crow’s feet lines and small crinkles under the eyes when smiling are often the first to become noticeable. With time, the elastic tissue and collagen fascicles that traverse the subcutaneous fat compartment and bind the muscles of facial expression to undersurface of the dermis degenerate and the RSTLs become permanently etched on the face (Glogau III). If the patient has significant photo-damage with deposition of solar elastosis within the papillary dermis, the lines become even more prominent, usually with a pronounced roadmap of lines all over the face (Glogau IV).
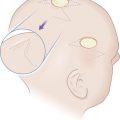
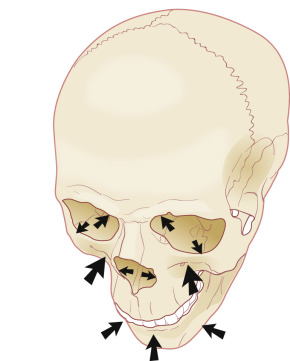
Aging has a profound effect upon the facial skeleton, the greatest on the bones of dental origin, the maxilla and mandible. These recede in their anterior projection and height beginning at a relatively early age. Regression of the orbital rim creates inferolateral and superomedial enlargement of the orbit causing loss of support for the periorbital soft tissues ( Fig. 1.4 ). Enlargement of the piriform aperture deepens the nasolabial groove, and these changes, previously attributed to gravity, create laxity of restraining fascial tissues and a generalized sagging of the skin that manifests as brow ptosis, dermatochalasis of the upper eyelids, hollowing under the eyes, vertical lines in the preauricular area, deepened melo-labial folds, rhytids of the perioral area, and pronounced jowls. These areas of redundant and excess, along with the temple and the glabella, constitute the reservoirs of skin available for recruitment for tissue rearrangements.
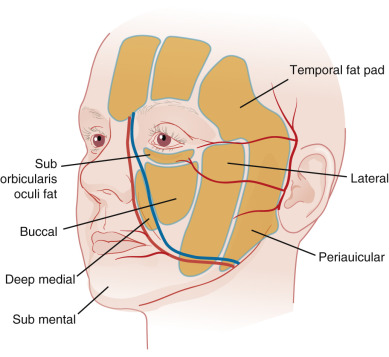
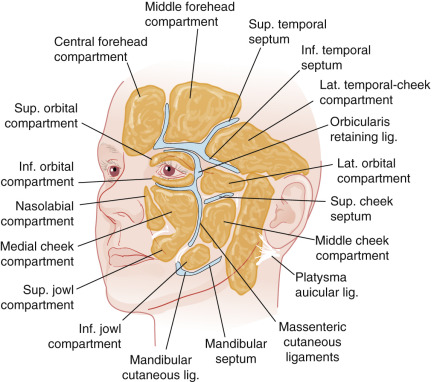
Generalized lipodystrophy of subcutaneous fat and specific resorption of the facial fat compartments and particularly the buccal fat pad ( Figs. 1.5 and 1.6 ) leads to a volume depletion of the face, resulting in a sunken appearance of the cheeks and a hollowing of the temples. What used to be thought of as a simple act of gravity creating a sagging face is now known to be a much more complicated interaction of fat atrophy, bone resorption, dynamic musculature, and changes in collagen and elastin.
Damage also results in splotchy hyperpigmentation and hypopigmentation; vascular changes in the form of telangiectasia of the cheeks and poikiloderma of the neck and rims of the ears; and the signature damage of ultraviolet radiation, the deposition of solar elastotic material in the papillary dermis, giving the skin a yellowish, thickened, and leathery appearance.
An accurate assessment of the aging face is important not only in correctly judging where there is available skin for recruitment in tumor defect repair but also for determining which cosmetic procedure is most applicable for any particular patient. An upper lid blepharoplasty may only compound severe brow ptosis if that condition is not also addressed. Similarly, it is important to recognize if a resurfacing (ablative laser, chemical peel, etc.), revolumizing (fillers), or tissue tightening procedure (radiofrequency, ultrasounds, etc.) would offer a particular patient the greatest benefit.
The Musculoaponeurotic System
Introduction
Humans communicate by use of the muscles of facial expression (the mimetic muscles). By use of this silent mode of interacting, human discourse is enriched by nuance and subtlety. Shades of annoyance, reverie, indifference, skepticism, sarcasm, and so on are molded onto the spoken word.
Muscles of facial expression are unique in that they are the only muscles to insert into the skin. They do so via fibrous septae that connect the superior portion of the muscle to the undersurface of the dermis and are part of the branching network of fibers known as the retinacular cutis. This is part of a larger complex system of fibrous septa in the subcutaneous layer of the face that connect to the retaining ligaments and contribute to the septa that create the fat compartments of the face. They also insert or interdigitate with the other mimetic muscles. So while the frontalis muscle wrinkles the forehead and raises the eyebrow, it helps open the eye widely by partially inserting into the upper fibers of the orbicularis oculi muscle ( Fig. 1.7 ).
Innervation of the muscles is exclusively by branches of the facial or cranial nerve VII. This occurs at the lateral undersurface of the muscle. The muscles are most effective and concentrated in the midplane of the face and exert their major effect around the two major orifices of the face—the eyes and the mouth.
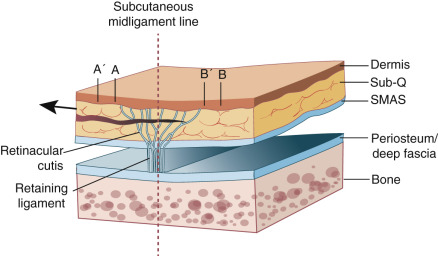
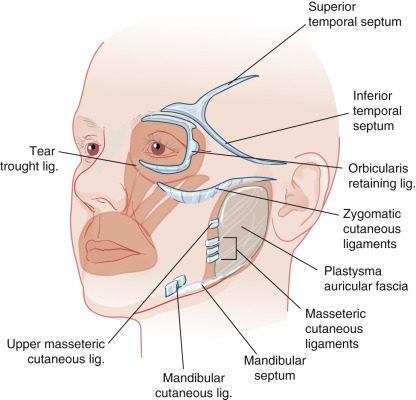
The aponeurotic component is made up of retaining ligaments that are strong and deep fibrous attachments that originate from the periosteum or deep fascia and travel perpendicularly through the facial layers to insert in the dermis ( Figs. 1.8 and 1.9 ). These ligaments act as anchor points, retaining and stabilizing the skin and superficial fascia (superficial musculoaponeurotic system [SMAS]) to the underlying deep fascia and skeleton. They tend to be more laterally displaced on the face in the SMAS of the cheek and the superficial temporalis fascia of the temple, which has a superior temporal septum and an inferior temporal septum. The orbicular retaining ligament surrounds the orbit connecting medially to the tear trough ligament ( Fig. 1.10 ). The other major components of the aponeurotic system are the zygomatic cutaneous, masseteric, and mandibular ligaments, and the galea aponeurotica is spread over the expanse of the skull, connecting the anteriorly displaced frontalis muscle with the occipitalis muscle of the neck. These ligaments and fascial components restrict cutaneous mobility and may be necessary to surgically disrupt in order to mobilize tissue for closures. It is also important to recognize that these retaining ligaments often share intimate relationships with branches of the facial nerve, so knowledge of their anatomic relationship is essential to avoid nerve damage during dissection.