Introduction
Already described in Roman times and in the Middle Ages, and rediscovered by the Swiss dermatologist Robert Muller, ambulatory phlebectomy (AP) is a safe and effective surgical technique that enables the removal of incompetent saphenous veins (except the saphenofemoral and in most cases the saphenopopliteal junctions), their major tributaries, perforators, and reticular veins, including the feeding veins of telangiectasias, or even blue telangiectasias. Ambulatory phlebectomy may also be used in varicophlebitis and superficial phlebitis, or for veins in other locations, for instance dilated periorbital, temporal or frontal venous networks, as well as venous dilatation of the abdomen, arms or dorsum of the hands.
AP is indicated in almost all patients, including the elderly. Most of the procedures are performed in truly ambulatory patients, but the technique may also be used in conjunction with other surgical procedures in ambulatory or stationary patients.
The goal of ambulatory phlebectomy is to secure definitive treatment of the varicose veins, once the underlying cause of reflux has been treated and eliminated. In some cases, the goal may be only partial or short-term improvement. Examples include avulsion of a single painful varicose vein in a young mother unwilling or unable to consider more extensive treatment, or in an elderly patient, removal of a single symptomatic varicose segment or of a feeding vein causing a leg ulcer.
The Problem Being Treated
This chapter will clarify how to select patients who may benefit from AP and how to safely and effectively perform the procedure. However, AP cannot be learned solely from a textbook, and being able to perform the procedure independently requires observing an experienced phlebologist treat different kinds of varicose veins as he or she carefully explains the successive steps of infusing anesthesia, operating and bandaging.
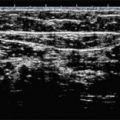
Every patient should be carefully interviewed and examined, with the examination including at least a continuous wave Doppler, but preferably duplex ultrasound (DUS), before selection of the most appropriate procedure ( Box 8.1 ). Side-transillumination (episcopy) is a useful tool for detecting reticular varicose veins and feeding veins associated with overlying telangiectasias.
- •
Patient interview
- •
Clinical examination while the patient is in the supine position
- •
Episcopy (side-transillumination)
- •
Doppler or duplex ultrasound
Patient Selection
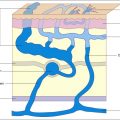
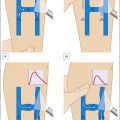
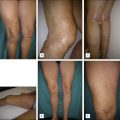
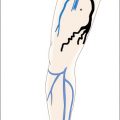
Patients of all ages may be treated with AP. All types of primary or secondary varicose veins (saphenous, reticular, perineal, telangiectatic, veins and perforators corresponding to classes C1–C6 of the clinical, etiologic, anatomic, pathophysiologic classification (CEAP)) may be removed by AP ( Boxes 8.2 , 8.3 ; Figs 8.1–8.3 ). Further special indications are discussed at the end of this chapter.
C 0 No visible or palpable signs of venous disease
C 1 Telangiectasias or reticular veins
C 2 Varicose veins; distinguished from reticular veins by a diameter of 3 mm or more
C 3 Edema
C 4 Changes in skin and subcutaneous tissue secondary to chronic venous disorders (CVD)
C 4a Pigmentation or eczema
C 4b Lipodermatosclerosis or atrophie blanche
C 5 Healed venous ulcer
C 6 Active venous ulcer
- •
Saphenous and saphenous tributaries
- •
Varicose veins of the lateral aspects of the leg
- •
Reticular varicose veins
- •
Perineal varicose veins
- •
Veins of the dorsal aspect of the foot
- •
Varicose pearls
- •
Perforators (with some limits)
Phlebectomy of an isolated portion of a saphenous vein should not be conducted if the termination is insufficient. Phlebectomy of the perforators is to be envisaged with caution. The results are good if the hook is used to remove the medial perforators of the thigh and small perforators of the lateral surface of the legs. The results are mediocre with respect to the medial perforators of the lower leg
Other indications
- •
Curettage of telangiectasias
Other esthetic indications
- •
Facial, palpebral and arm veins, etc.
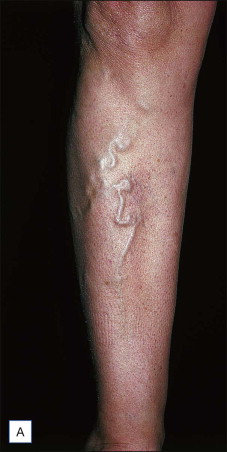
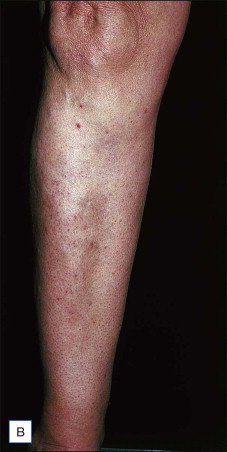
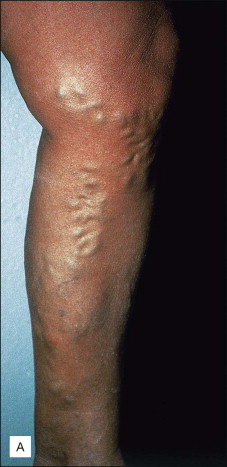
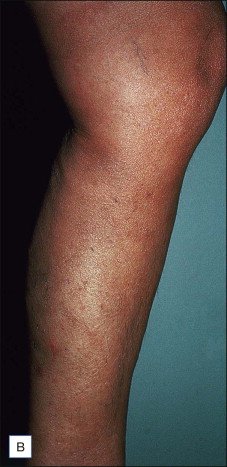
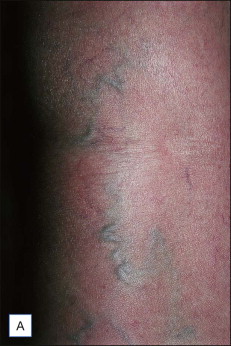
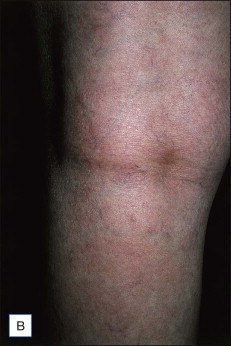
Regional venous networks particularly appropriate for ambulatory phlebectomy include accessory saphenous veins of the thigh, groin pudendal (perineal) veins, reticular varicose veins (popliteal fossa, lateral thigh and leg, as described by Albanese), veins of the ankles, and the dorsal venous network of the foot.
While most procedures are performed in ambulatory patients, the technique may also be used in conjunction with other surgical procedures such as high ligations (crossectomy), stripping of incompetent saphenous veins and endovenous ablation (laser or radiofrequency) in ambulatory or stationary patients.
Contraindications are rare or relative: critical arterial ischemia, infections, allergy to local anesthetics, bed-ridden status, and impaired blood clotting or immunity. AP is usually not performed during pregnancy or immediately postpartum, as varicose veins frequently regress spontaneously.
Expected Benefits
Since Muller’s first writings in 1966, AP has been considered a very effective and economical technique that affords outstanding cosmetic results.
Long-term results tend to be excellent as long as the most proximal source of reflux is eliminated, however evidence-based objective data confirming this widely accepted conclusion continue to be sparse. A single randomized, controlled trial by de has recently been published and found excellent long-term results of AP and verified its superiority to sclerotherapy for treatment of the anterior thigh accessory great saphenous vein. A recent extensive study demonstrates satisfying long-term results of phlebectomy, even with conservation of a refluxing saphenous vein ( ).
Improvement in anesthetic technique with the advent of tumescence has resulted in greatly reduced pre- and postoperative pain as well as complications. As AP is usually performed in the friendly environment of an office rather than in the operating room, it is mostly experienced as ‘quite comfortable’ by patients.
The technique is safe, as noted by several publications that have reviewed reported complications of AP. The side effects of this procedure will be discussed later.
It should be noted that in order to obtain good results and prevent recurrences, AP must only be performed when it is indicated. When this procedure is selected, it must consist of removal of all segments of varicose veins, including feeding perforators, to prevent relapses or unsightly complications, such as telangiectatic matting.
AP is an easy and inexpensive procedure to perform. A skilled practitioner may remove an extensive array of varicose veins in a short period of time, generally lasting 20–90 minutes, with both legs being operated upon in a single session. A simple, streamlined operative approach by a well-trained practitioner is much more effective and economical than ‘high-tech’ new modalities.
Sclerotherapy may initially appear to be even easier to perform and more economical than AP, but for veins larger than superficial telangiectasias, the number of sessions required and the high rate of recurrence exclude this option ( Box 8.4 ).
These indications are debatable. The choice of the method depends first on the skill of the practitioner and local traditions.
- •
Sclerotherapy: telangiectasias and reticular varicose veins
- •
Ultrasound-guided sclerotherapy: intrafascial varicose networks, including the small saphenous veins
- •
Ambulatory phlebectomy: from reticular to large, epifascial varicose veins
Overview of Treatment Strategy
•
Treatment approach and major determinants
Major treatment modalities in phlebology include compression therapy, sclerotherapy, AP, endovenous ablation, surgery, and laser treatment. Each technique has its own indications and advantages, although there are some areas of overlap.
For most indications, the procedure most similar to AP is sclerotherapy. Sclerotherapy is principally indicated in the treatment of telangiectasias and reticular varicose veins. New modalities, such as foam sclerotherapy and ultrasound-guided sclerotherapy, afford excellent results in the treatment of intrafascial varicose networks, including post-operative relapse, the small saphenous veins, or saphenous and accessory saphenous veins of the thigh.
AP is superior to sclerotherapy in the treatment of medium to large, epifascial varicose veins. With AP, there are fewer recurrences, and no risks of inadvertent intra-arterial injection, skin necrosis (due to extravasation of sclerosant or unpredictable arteriovenous anastomosis injection), or residual hyperpigmentation.
Patient Interviews
Elicitation of patient histories is discussed in a previous chapter. Recording of structured case histories permits appropriate weighting of the various symptoms and venous risk factors, and improved estimation of prognosis.
The physician must be especially receptive to the patient’s complaints and expectations, as postoperative patient disappointment is often less a matter of technical failure than the result of unrealistic patient expectations that were unchallenged prior to treatment.
Careful analysis of the patient’s history and symptoms may enable the physician to differentiate venous problems from arterial lesions, nerve root irritation syndrome, osteoarticular or muscle-tendon disease, and more generalized diseases such as fibromyalgia. Some symptoms, such as muscle cramps and restless legs, are not very specific. Treatment of varicose veins is unlikely to result in the resolution of these symptoms, and the patient should be made aware of this.
The prognosis and likely evolution of chronic venous disease in each particular patient should also be discussed. Depending on the predominant type of varicose veins, the severity of the disorder, and presence of specific risk factors, patients may be likely to encounter different clinical courses in the future.
Clinical Examination
This is an essential part of the treatment, as good AP results depend on the accuracy of the diagnosis and of a thorough evaluation of the exact origin and extent of the varicose veins. Clinical examination should be supplemented by Doppler and/or duplex ultrasound, as described in Chapter 3 ( Box 8.1 ).
Treatment Techniques
•
Equipment
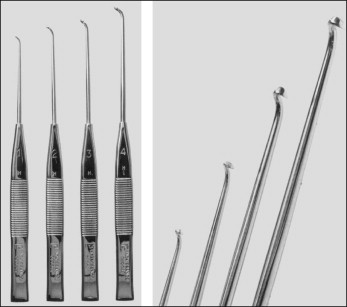
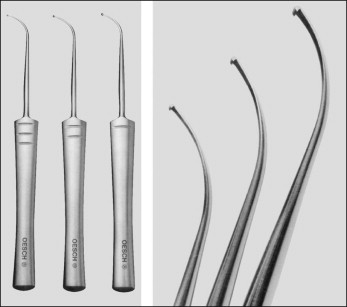
Only a few surgical instruments and forms of equipment are required ( Box 8.5 ) for AP. Among the types of hooks that have been marketed for vein grasping and extraction are the Müller, Oesch, Ramelet, Tretbar, and Varady ( Figs 8.4–8.7 ).
- •
Local buffered anesthetic, normal saline or Ringer’s solution
- •
Resuscitation equipment, indispensable during any procedure
- •
Sterile gloves and mask
- •
Disinfectant (not removing the marking stain of the course of varicose veins)
- •
No. 11 straight blade scalpel
- •
18 gauge needle
- •
Phlebectomy hooks
- •
Mosquito forceps
- •
Sterile pads
- •
Dressing materials
- •
Elastic bandages

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree