Anatomy
An excellent knowledge of the entire anatomy of the lower trunk and extremities is essential for esthetic and reconstructive skin-tightening procedures. In addition to knowledge of the main perforating vessels, the course of important nerves is mandatory to avoid postoperative complications. Furthermore, the knowledge of Langer’s lines (relaxed skin tension lines) is crucial for the best possible scar development.
Skin
Abdominal skin and fat tend to become distributed in the lower abdomen with aging and pregnancy. Striae also become common, especially as a result of multiple pregnancies, resulting in a rupture and separation of dermal collagen with consequent skin thinning. Following postbariatric weight loss, patients have been shown to have damaged skin in recent studies evaluating the content and structure of collagen and elastin when compared to nonbariatric patients.
The skin of the abdomen has areas of increased adherence to the underlying fascia (“zones of adherence”) in the vertical midline area, and occasionally in a horizontal direction just superior to the umbilicus (supraumbilical skin fold), as well as in a horizontal direction above the anterior superior iliac crest.
Fascia
The abdominal subcutaneous tissue is divided by two layers of fascia: the superficial Camper’s fascia and the deep Scarpa’s fascia, a strong fibrous layer of connective tissue which is continuous with the fascia lata of the thigh.
Fat
The superficial fat layer has a more compact character with smaller lobules and a rich vascularization, while the deeper fat stains larger lobules with a more scattered pattern.
The Umbilicus
In most patients, the umbilicus is the most important landmark on the abdominal wall. It is normally situated in the midline, approximately 9–12 cm above the upper border of the mons pubis region. A round or ellipsoid shape may characterize it. The abdominal fascia in this region can present as weak with an increased incidence for hernias. The blood supply derives from branches of the subdermal plexus, from both deep inferior epigastric arteries, as well as a blood supply from the median umbilical ligament. In general, the umbilical stalk is blunted and dissociated from the surrounding fat tissue.
Musculoaponeurotic System
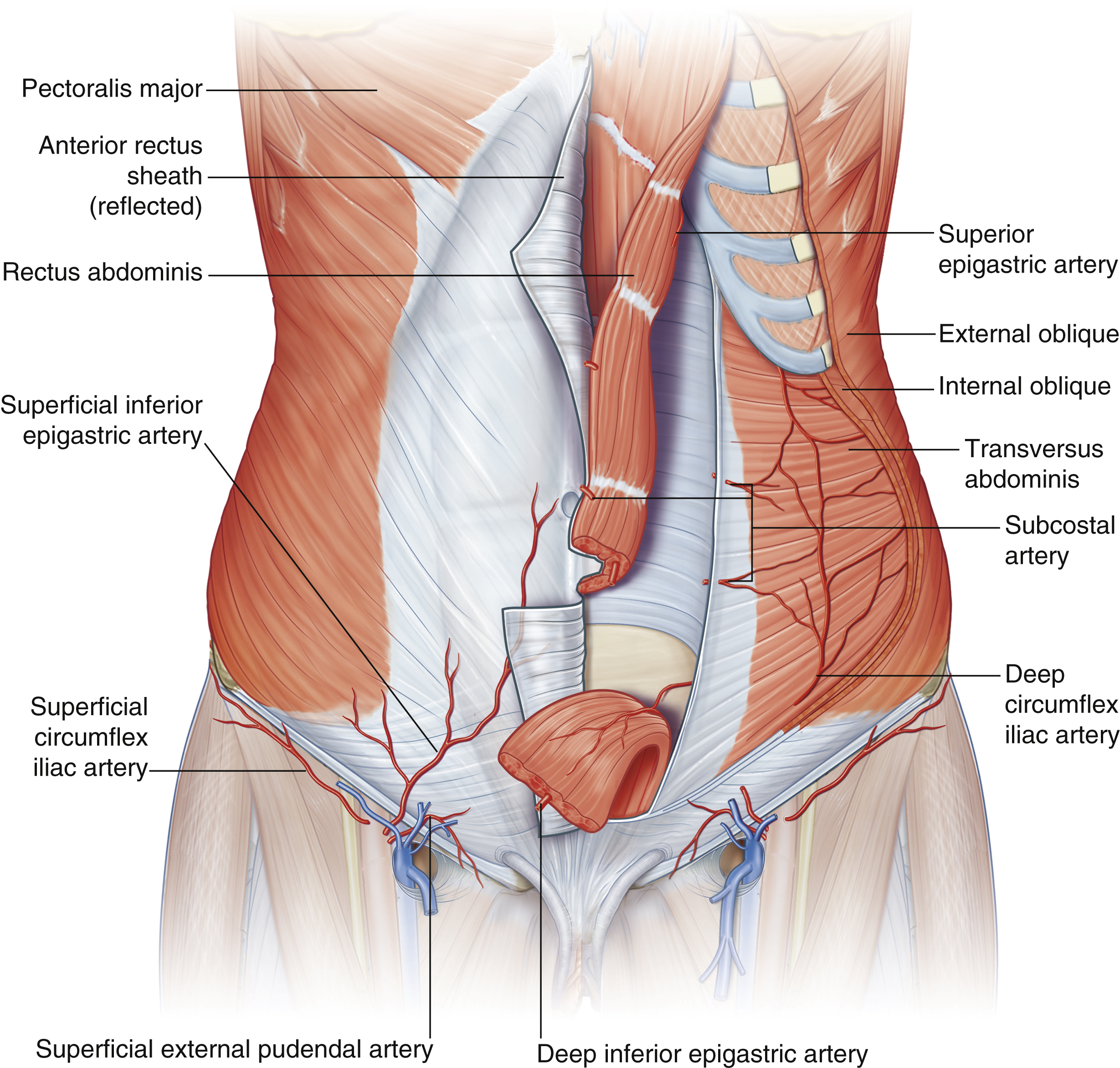
The abdominal musculature includes four paired muscles: the rectus abdominis, connected in the median linea alba, the external oblique and internal oblique, and the transversus abdominis muscle, which incorporate into the anterior and posterior rectus sheath at the linea semilunaris. The rectus abdominis muscles are enclosed by an anterior and posterior sheath, originating at the infracostal margin and attaching at the symphysis pubis. Above the arcuate line (situated approximately midway between umbilicus and pubic symphysis), the anterior rectus sheath is formed by the external oblique and internal oblique aponeurosis, whereas the posterior rectus sheath is formed by the internal oblique and transversus aponeurosis. Below the arcuate line, the posterior rectus sheath is absent, except for the transversus fascia and the peritoneum. At the inferior aspect of the rectus muscles, the pyramidalis muscles are present in 80%–90% of patients ( Fig. 71.1 ).
Lymphatic Drainage
The abdominal lymphatic system is divided into supraumbical drainage to the ipsilateral axillary lymph nodes and an infraumbilical drainage into the superficial inguinal lymph nodes. The lymph vessels in the infraumbilical area pass through the sub-Scarpal plane, emphasizing the importance of Scarpa’s fascia preservation in abdominal wall surgery.
Blood Supply
The blood supply to the abdominal wall is derived from numerous major arteries of the thorax and pelvic region; these communicate through many anastomotic interconnections. Two types of cutaneous blood supply are known: direct vessels that supply the skin directly and indirect perforating vessels that emerge from the deep fascia as terminal spent branches of arteries whose main purpose is to supply the muscles and other deep tissues. Moon and Taylor were able to demonstrate connections between the deep superior and deep inferior epigastric systems and their relationship to the cutaneous circulation.
A detailed knowledge of the arterial supply of the abdominal wall is crucial to abdominal wall surgery, especially in cases of prior abdominal wall surgery. Huger described different zones of the abdominal blood supply which should guide the surgeon in planning and performing a safe operation. Huger defined zone I of the abdominal wall as the area that is fed anteriorly by the vertically oriented deep epigastric arcade. Zone III was defined as the lateral aspect of the abdominal wall (flanks) that are fed by the six lateral intercostal and four lumbar arteries. The lower abdominal circulation is provided by the superficial epigastric, superficial external pudendal, and superficial circumflex iliac systems (zone II). A rich plexus between these systems allows collateral flow (see Fig. 71.1 , Fig. 71.2 ).
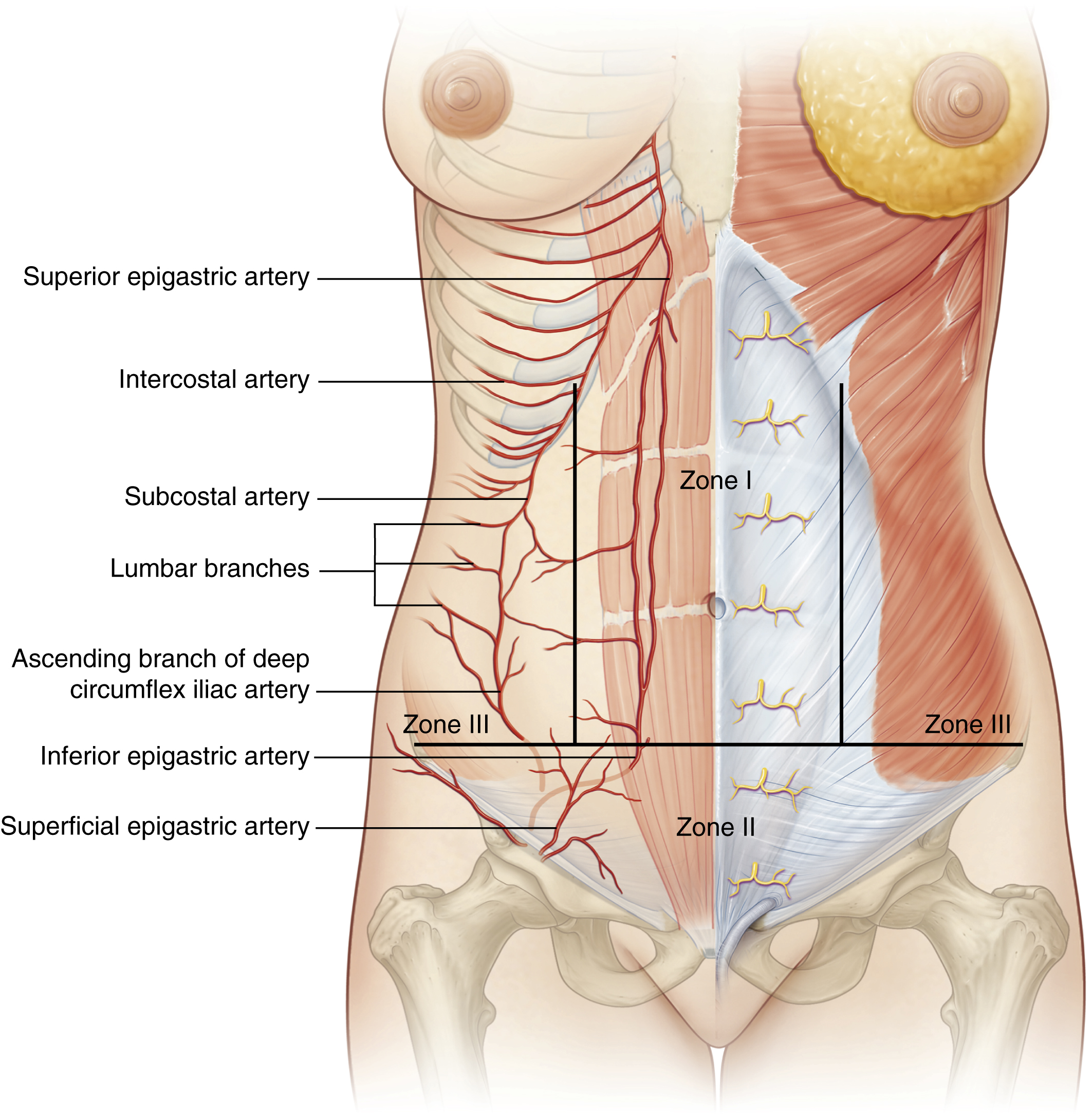
In standard abdominoplasty procedures, the blood supply to zone I and main parts of zone II is disrupted after flap mobilization, resulting in an abdominal flap perfusion mainly supplied by zone III. The lateral perforating branches from the lateral intercostals and lumbar arteries are essential for the remaining flap perfusion. Therefore, it is crucial to study any preoperative existing scar, such as subcostal cholecystectomy incisions (see Fig. 71.2 ).
Nerve Supply
The sensibility of the abdominal wall derives from the anterior and lateral cutaneous branches of the eight to twelfth intercostal nerves, which reach the skin and fascia by passing between the internal oblique and transversus abdominis muscles and finally through the rectus abdominis muscle. The lateral cutaneous branches penetrate the intercostal muscles in the midaxillary line, ending in the subcutaneous layer.
The motor branches of the rectus abdominis muscle derive from lateral branches of the fifth to twelfth intercostal nerves, which pass behind the rectus muscles and enter the muscles at the junction of the lateral third and medial two-thirds. The oblique and transversus abdominis muscle are innervated by branches from the lower thoracic and lumbar dorsal nerves ( Fig. 71.3 ).
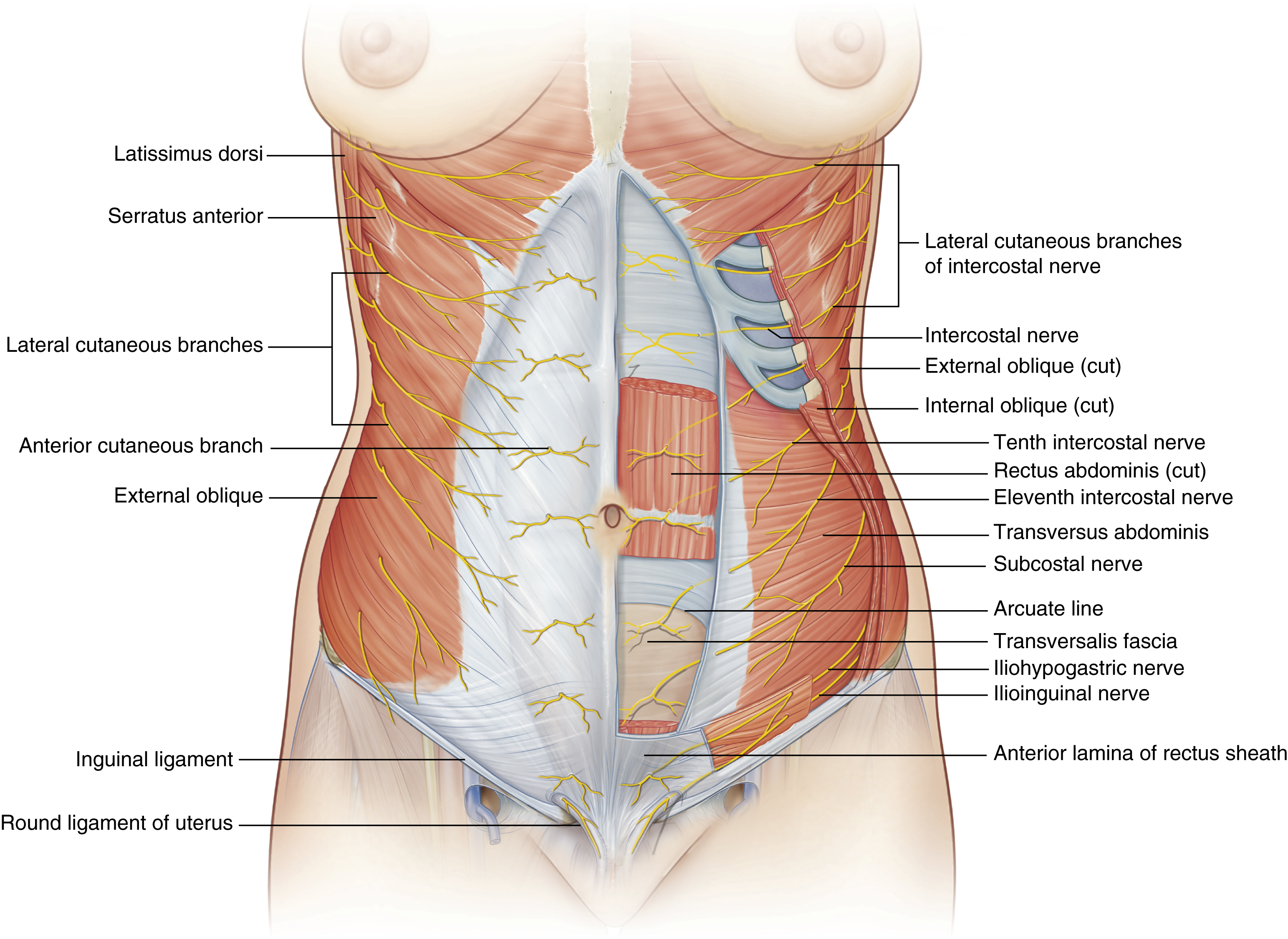
Peripheral nerves such as the iliohypogastric and ilioinguinal must be noted, as they may be injured in lateral transverse lower abdominal incisions, resulting in consistent loss of sensory in the area of the groin and medioventral thigh.
Anatomical Landmarks
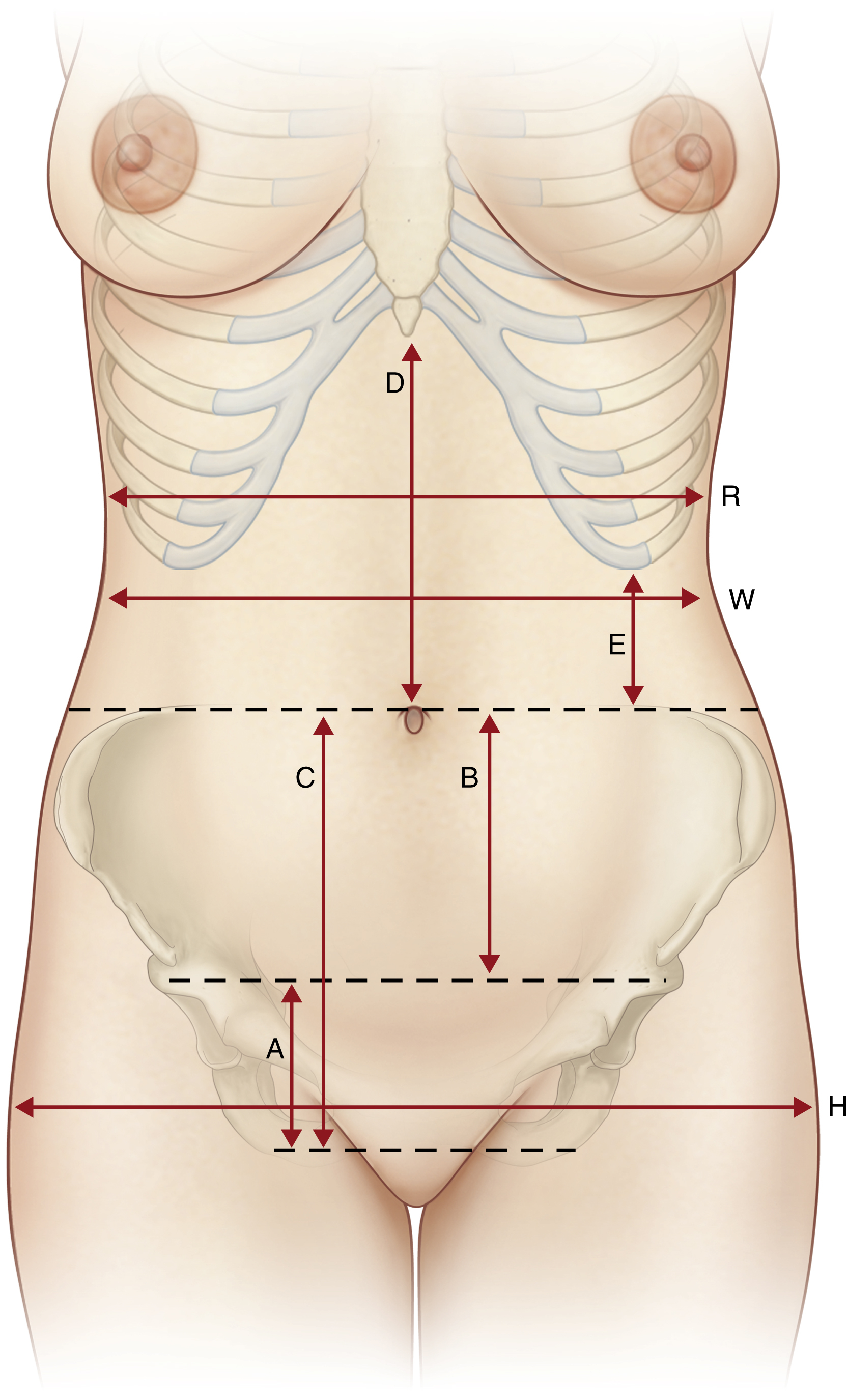
Normal abdominal anatomical proportions ( Fig. 71.4 ):
- •
The umbilicus is located in line with the most superior point of the iliac crest in 99% of patients.
- •
Distance between the top of mons and anterior valvar commissure ( A ): average height is 5–7 cm.
- •
Distance between umbilicus and top of mons ( A + B ): average height is 11–13 cm.
- •
Distance between umbilicus and top of anterior and vulvar commissure ( C = D ).
- •
Distance between the costal marginal and the iliac crest ( E ). The proportion of this distance to the width of the base of the rib cage ( R ) determines whether the patient is long-waisted or short-waisted. The normal proportion ( E : R ) is roughly 1:3 (long-waisted approaches 1:2, short-waisted approaches 1:3).
- •
The rib cage tapers inferiorly. A narrower lower rib cage relative to the width under the armpits helps to emphasize the waist by creating a subtle V.
- •
Hip width ( H ). A wider pelvis than rib cage emphasizes the waist; the waist is more defined when R < H.
- •
Natural waist ( W ) – the narrowest point of the torso. (Note that the umbilicus usually sits below the natural waist by about 1–4 cm.) Relative to the hips, this waist-to-hip ( W : H ) ratio in healthy women is roughly 0.72:1; in healthy men, it is roughly 0.83:1. Note that the natural contour of the healthy abdomen reveals a subtle epigastric sagittal depression transitioning to a mild infraumbilical convexity. A subtle vertical sulcus at the lateral rectus border, which is more distinct in a muscular person, may also be seen (see Fig. 71.4 ).
Esthetic Assessment
Abdominal Wall
The esthetic assessment of the abdominal wall includes:
- •
Regions of local adipose tissue and their thickness in centimeters
- •
Local adipose tissue in the upper and central abdominal region
- •
Regions of local skin excess
- •
Local skin excess in the upper and central abdominal region
- •
Presence of skin folds and their depths
- •
Areas of maximal looseness and adherence
- •
Local adipose tissue in the adjoining regions of the flanks, hips and breasts
- •
Local adipose tissue in the mons pubis region
- •
Skin laxity in the mons pubis region
- •
Any asymmetric aspects
- •
Any bulginess
- •
Any preexisting scars and their quality
- •
Presence and degree of striae.
Umbilicus
The esthetic assessment of the umbilicus includes:
- •
Shape and depth of the umbilical stalk
- •
Position of the umbilical basis on the abdominal wall (to be demonstrated to the patient)
- •
Height of umbilical descent
- •
Any existing umbilical herniation or adipose tumor
- •
Any existing eczema, hyperpigmentation or preexisting scars
- •
Any prior operation in the umbilical region has to be clarified, since impaired perfusion after dissection may occur in these cases.
Back, Thighs, and Buttocks
The esthetic assessment of the back, thigh, and buttocks includes:
- •
Regions of local adipose tissue and their thickness in centimeters in the back
- •
Mobility of the dorsal skin in the lower back region
- •
Local skin excess m the back region
- •
Presence of dorsal skin folds and their depth
- •
Local adipose tissue in the gluteal region
- •
Regions of local skin excess, measured by pinching in vertical distance in the gluteal and flank region
- •
Presence of gluteal skin folds and their depths
- •
Areas of maximal looseness and adherence
- •
Local adipose tissue in the anterior, posterior, lateral and inner thigh region
- •
Skin laxity in all thigh regions
- •
Presence of skin folds in the thigh region (e.g., inner thigh, distal anterior)
- •
Any asymmetric aspects
- •
Any bulginess
- •
Any preexisting scars and their quality
- •
Any existing eczema or hyperpigmentations
- •
Presence and degree of striae.
Patient Assessment
History
During the first consultation a review of the patient’s medical history is mandatory. We recommend a review of this prior to surgery, when it is performed with a delay from the first consultation and at least annually. The assessment of medical history includes the current weight, the ABSI (a body shape index) and body mass index (BMI), the weight history with weight fluctuations and constancy periods, the frequency of exercises, former bariatric procedures, nutritional disorders, medication, the number of pregnancies and children, history of cesarean section, abdominal surgeries and abdominal hernias, gastrointestinal, cardiac, and pulmonary history, a smoking history, and any existing coagulation disorder. Patients should be asked specifically about previous liposuction in the abdominal area, often overlooked by patients in past surgical history.
Physical Examination
Physical examination is part of every medical history assessment. It evaluates the entire region the patient is concerned about. An examination of the skin tissue and the different fat layers is performed by pinching and measuring the subcutaneous layer thickness. Skin quality with the presence of striae should be noted, clarifying with the patient that supraumbilical striae will not be resected in abdominoplasty procedures (except for fleur-de-lis procedures). In this context, it is helpful to handout of studies on skin quality in postbariatric patients who have demonstrated damage to collagen structures. ,
It is important to assess and measure the lower and upper abdominal pannus, documenting any existing eczema or consequent hyperpigmentation. The entire skin excess in the areas inferior to the lower abdominal fold, in the area of the lateral and upper abdomen, the waist, hips and thighs, as well as the lower chest, have to be included in the preoperative assessment, during upright standing, supine, as well as sitting positions. Any preexisting scars (subcostal, midline, horizontal) in the abdominal area have to be documented, since they can impair the blood supply. Furthermore, the status of the abdominal musculature should be assessed and any existing rectus diastasis, incisional, epigastric or umbilical hernia excluded. Supportive CT or MRI scans may be considered.
In this context, it is mandatory to evaluate intraabdominal pressure to avoid any postoperative pressure increase or abdominal compartment syndrome. In cases of elevated intraabdominal pressure, in the supine position, the abdominal wall elevates above the costal margin and the level of the iliac crest. Abdominoplasty procedures, especially with fascial reconstruction, have to be performed cautiously in such cases. In these cases, it is mandatory to wear a compression girdle for at least 8–12 weeks prior to surgery to improve and adapt the body to the postoperative situation and to prevent respiratory difficulties.
Documentation
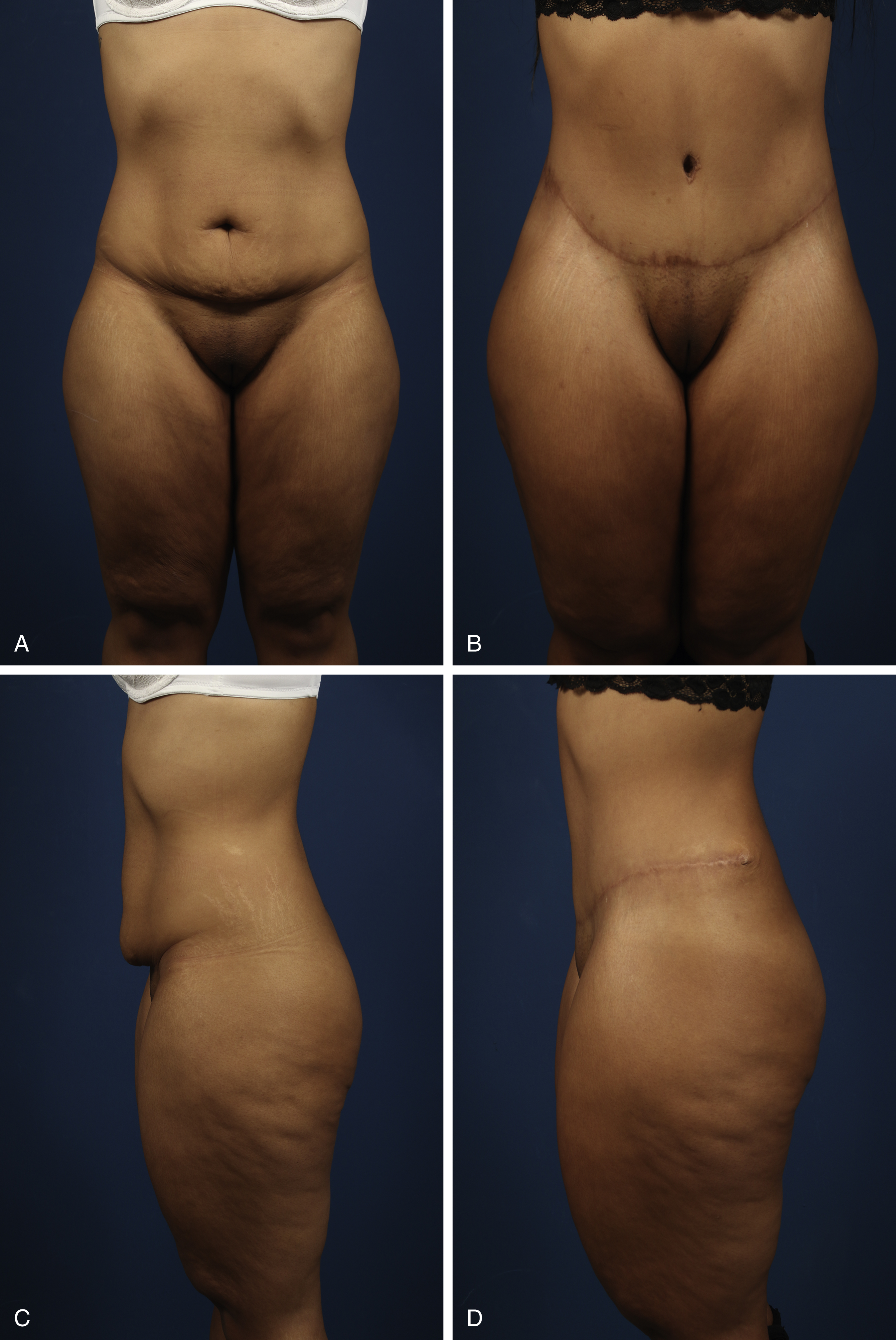
It is mandatory to ensure a complete medical photographic documentation pre- and postoperatively, consisting of different views (anterior, oblique, side, and posterior). Postoperative photo documentation should be made at 3, 9, and 12 months. In individual cases it is recommended to perform additional photo documentation of standard arm and thigh positions, tissue characteristics with relaxed and contracted muscles, the patient in sitting position to demonstrate redundant upper abdominal laxity and tissue excess, additional views with the patient holding up and pinching excess tissue in the specific region or bending forward to demonstrate skin excess in the upper abdominal region.
Informing the patients in detail about the operative procedure, alternative techniques, and the general and operation-related risks and benefits is an essential part of preoperative documentation. Besides standard and individualized consent forms, which have to be reviewed and signed by the patient at the earliest opportunity and at the latest 24 hours prior to the operation, we recommend an audiovisual demonstration for exact understanding. In general, we recommend informing every patient transparently about any and all possible complications. Moreover, patients have to be informed about their postoperative care, including their expected level of activity, and the limitations of the surgical result in cases of existing variables of bone structure, fat distribution, and any existing scars.
Esthetics
The preoperative esthetic status of the body region of concern has to be well documented in written and photographic format after a precise physical examination. For a classification of the different deformities, we found the Pittsburgh Rating Scale to be helpful for patient demonstration and selection of the best operative approach. However, we have experienced a wider indication for the combined technique of liposuction and excisional procedures in all body regions.
General
Patients are advised to stabilize their weight for at least 6–12 months preoperatively; any desired weight loss should be completed prior to the surgery. Smokers should stop smoking at least 6 weeks prior to surgery and continue for 6 weeks after surgery.
Where a postoperative blood transfusion is considered (e.g., body lifts), patients have to be informed preoperatively, as this requires a blood typing and informed consent and the possibility of an autologous blood transfusion should be discussed. Anticoagulant drugs and supplements must be avoided 14 days prior to surgery. In cases of a planned abdominal procedure, we advise patients to perform bowel purgation the night before surgery. In some cases, patients can be restricted to a fluid diet for 24 hours prior to surgery.
Patients have to be informed about the intraoperative procedures, including any change of position with the risks of postoperative complication, antithrombotic prophylaxis, urinary catheter, drains, and garment placement, as well as patient-controlled analgesia (PCA). Moreover, they have to be instructed about the postoperative course, regarding thromboembolism prevention (we administer dalteparin 5000 IU perioperatively and daily for at least 2 weeks), respiratory exercises, early mobilization, avoidance of high abdominal pressure maneuvers, the estimated time point for drain and/or suture removal, as well as the minimum time required off work and abstinence from exercise. Length of inpatient admission must be discussed with patients where surgery cannot be performed in an outpatient setting, Diabetes may be considered a relative contraindication to this procedure, especially in poorly controlled patients. Staging procedures may be necessary to improve patient safety and to improve outcomes. An inspection of the abdominal skin and umbilicus areas for local skin irritation during consultation, and immediately prior to the operation, is strongly advisable.
Prophylaxis for deep venous thrombosis (DVT) and pulmonary embolus (PE) is an essential consideration in all patients, especially in smokers and patients taking birth control medications or hormone replacement therapy. We inform patients that this specific risk will be decreased if hormonal therapy is discontinued 3–4 weeks prior to surgery and until at least 14 days after surgery.
In cases of an existing extended diastasis or hernia, the reconstruction of the fascia results in an increased intraabdominal pressure, which may be a source of respiratory difficulties. Therefore, we advise preoperative breathing exercises (utilizing an incentive spirometer) beginning 1–2 weeks prior to and continuing for 2 weeks after the surgery or, as described above, the application of a compression girdle for 8–12 weeks prior to surgery. A cold, dry cough or any kind of respiratory infections should lead to postponement of surgery, since fits of coughing may provoke a rupture of the fascial sutures with consequent secondary bleeding. , ,
Operative Principles and Approach
Various procedures are available with various indications as listed in Table 71.1 .
| Mini | Standard | HLT | Fleur-de-Lis | Bodylift | Reverse | |
|---|---|---|---|---|---|---|
| Lower abdomen | + | +++ | +++ | +++ | +++ | 0 |
| Periumbilical | (+) | ++ | ++ | +++ | ++ | (+) |
| Upper abdomen | 0 | ++ | ++ | +++ | ++ | +++ |
| Diastasis/hernia | (+) | ++ | ++ | +++ | ++ | (+) |
| Flanks/hips/thighs | 0 | (+) | + | ++ | +++ | 0 |
Liposuction
The indication for sole liposuction of the abdomen is seen very rarely. In patients with an abdominal contour impaired by an irregular and solely thickened abdominal fat layer, liposuction may improve the abdominal shape dramatically. Nevertheless, as soon as a patient highlights his or her frustration due to a laxity of skin, it will not be worthwhile to perform liposuction without simultaneous skin excision. Ideal cases for liposuction are patients with localized adipose tissue in the flank/hip region, the infra- and/or supraumbilical region. They can be optimally treated by liposuction under local anesthesia as an outpatient. For achievement of maximum outcomes, it could be reasonable to acquire one of the assisted liposuction techniques nowadays available (e.g., laser-, ultrasonic- or radiofrequency-assisted liposuction), which allow simultaneous skin tightening. It should be clarified with patients that such a procedure can result in a higher risk of complications if an abdominoplasty is performed afterwards.
In all cases of liposuction in the abdominal region it is mandatory to exclude any existing rectus diastasis or abdominal hernia. If required, diagnostics may include an ultrasonic scan, CT or MRI ( Fig. 71.5 ).
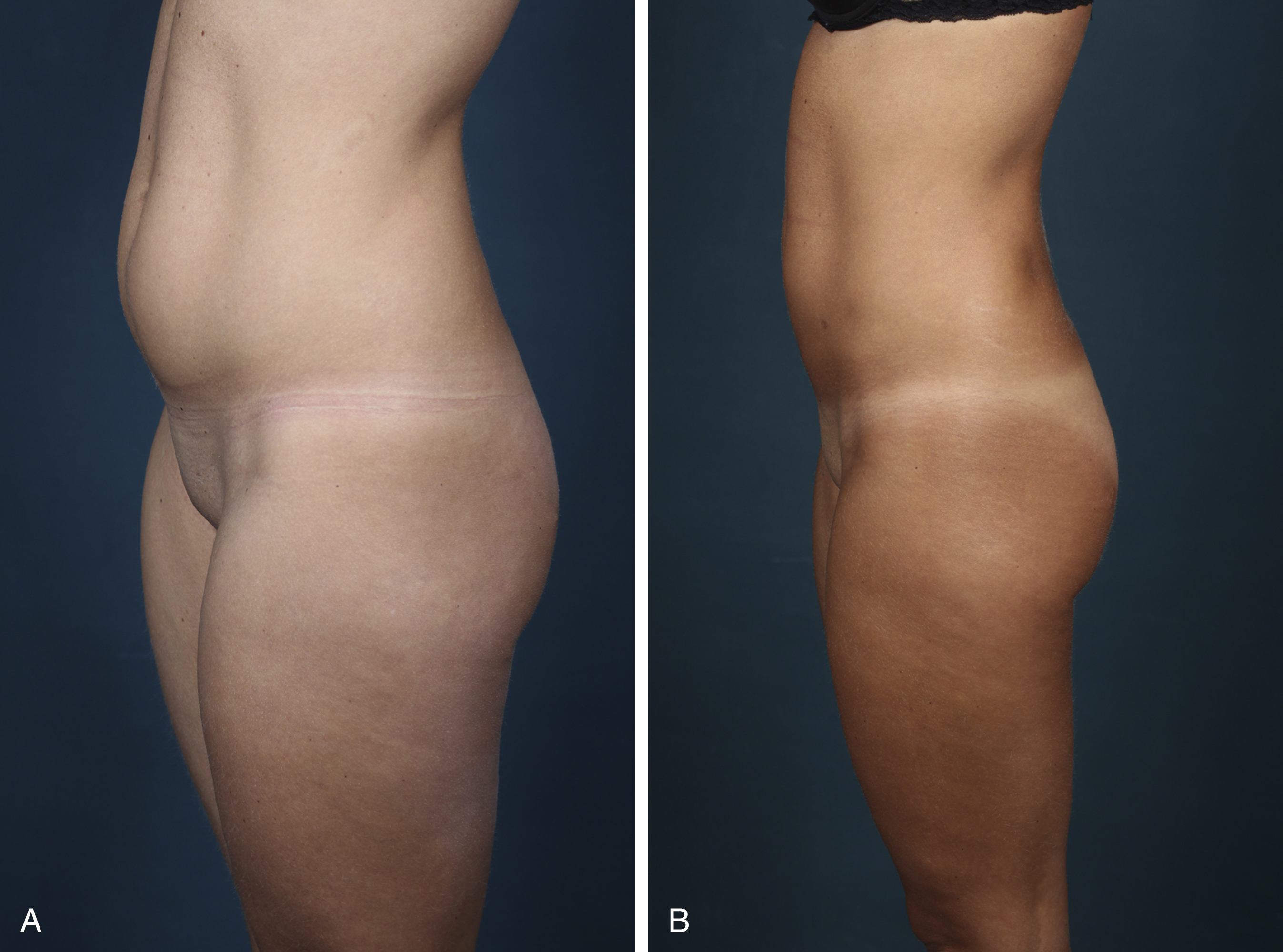
Any adjunctive liposuction of the abdominal wall should be performed at the beginning of the abdominoplasty procedure in order to sufficiently thin out the different layers, including the subfascial and, carefully, the epifascial layer. It is important to assess the relation of excess skin and fatty tissue, since in cases of extensive skin excess in the upper and midabdominal region a fleur-de-lis procedure may be indicated. In these cases, there is usually no necessity for liposuction in the abdominal region, since a maximal amount of abdominal tissue is resected.
Adjoining regions (e.g., the flanks and hips) may be treated by liposuction during the abdominoplasty procedure, preferably at the end of the operation. Infiltration of tumescence solution should be performed at the beginning of the procedure and liposuction can then be performed after a sufficient time of exposure during the abdominoplasty procedure. ,
Standard Abdominoplasty
The standard abdominoplasty is one of the most common procedures in plastic surgery. It enables the simultaneous treatment of the upper abdomen, periumbilical area, and lower abdomen, with optimally concealable scars.
Traditional abdominoplasty procedures involved wide mobilization of the abdominal wall up to the costal arch in order to ensure a tension-free wound closure. Multiple studies have since demonstrated that circulatory disturbance of the abdominal skin flap is the result of extensive undermining and destruction of the lateral perforators of Huger’s zone III. In modern abdominoplasty, undermining cranially to the umbilicus is mainly performed in the midline area anterior to the linea alba and both rectus muscles, including the zones of adhesion described by Lockwood and specified by Aly. The lateral abdominal flap may be securely released by additional liposuction or the Lockwood dissector for discontinuous undermining, preserving the lateral perforators and the lateral attachment to the rectus abdominus muscles.
The standard abdominoplasty is indicated in patients that typically demonstrate a localized and diet-resistant adiposity of the abdominal wall in combination with coexisting slack and atonic skin, such as patients after multiple pregnancies, patients with weakness of the connective tissue or patients after weight loss ( Fig. 71.6 ).