Advantage of flaps for secondary burn reconstruction
Hypertrophic scars/scar contractures (HS/SC) result from dermal inflammation. During wound healing, inflammation is necessary to accelerate collagen production and angiogenesis. However, this inflammation is prolonged by several local and systemic factors. The most important local factor is tension. Cyclical cutaneous tension increases vascular permeability and results in prolonged inflammation, which is one of the main causes of HS/SC formation. ,
Systemic factors can also significantly impact scarring. Asians and African patients tend to be more prone to HS/SC than Western/European tissue types because of the potential for prolonged inflammation. Moreover, high blood pressure (hypertension) and estrogen are risk factors of HS/SC. , Flaps should be the primary choice for reconstruction for these patients compared with skin grafts in those undergoing secondary burn reconstruction.
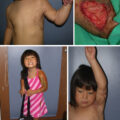
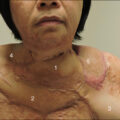
Various flaps are useful for releasing burn scar contractures. Because flaps have subcutaneous tissues that can expand naturally after surgery, they are not prone to postsurgical HS/SC. By contrast, skin grafts do not expand, meaning skin grafting tends to generate secondary contractures that result in circular HS/SC around the grafted skin ( Fig. 52.1 ). When used for burn scar contractures, flaps should preferably have skin paddles to help release contractures effectively ( Fig. 52.2 ). The postoperative extensibility of the flap should be considered when determining which flap design is optimal for the individual patient. With regard to skin-pedicled flaps, local flaps should be the primary choice. If the area of reconstruction is large, large local flaps with supercharged vessels can be designed. If, for various reasons, adjacent skin cannot be used as a flap donor site, free flaps should be selected. In this case, more than small free flaps are needed to prevent HS/SC because free flaps are always island flaps and cannot expand effectively. Thus for deep scar contractures, the order in which flap choice should be considered is first a skin-pedicled local flap, then a supercharged skin-pedicled flap, and finally a free flap. For specific areas of reconstruction, prelaminated and prefabricated flaps can be very useful and can provide excellent opportunities and options for reconstruction, especially in places such as the face. This chapter discusses options in burn reconstruction, specifically the supercharged flaps, free flaps, and prelaminated flaps using microsurgery.
Scars and grafted skin are difficult to expand after surgery; thus inflammation continues on the peripheral area. This will be a cause of hypertrophic scars/scar contractures.
Our previous study showed that skin-pedicled flaps could be extended more after surgery than island flaps. Thus a skin-pedicled flap should be used primarily.
Supercharged flaps
A thin flap should be employed when considering using a flap for contour-sensitive areas such as the anterior neck. In this case, a few points should be considered. First, if the thin flap is too large, ischemia or congestion could arise in the periphery. To enhance flap survival, the flap pedicle should be dissected as little as possible and carefully manipulated. Such efforts can result in sizable flaps for large areas of reconstruction ( Fig. 52.3 A). However, peripheral ischemia can also be overcome by anastomosing a perforating branch to the flap periphery, creating a supercharged flap with stable blood circulation (see Fig. 52.3 B).
(A) A male in his 60s with the anterior neck contracture reconstructed by a large 19-cm × 6-cm skin-pedicled flap. To promote flap survival, we did not elevate the flap pedicle more than necessary and then manipulated the flap very carefully. The flap survived fully, and the contracture was effectively released after 6 months. (B) If we attach supercharged vessels on the periphery of the flaps, blood circulation becomes strong, and peripheral congestion can be prevented.
The anterior neck poses complex reconstructive challenges because it connects the head to the body, and its skin must accommodate multidirectional and complex mobility. The skin, especially the dermis, must be very thin. Extensive scar contractures in this region often include the face, chin, and chest. In addition to severely restricting neck mobility, such contractures are often associated with shoulder stiffness and lower lip ectropion.
Flaps can be harvested from the anterior chest and the posterior torso for anterior neck reconstruction. For flaps harvested from the anterior chest, the pectoral intercostal perforators, the internal thoracic perforators, and the lateral thoracic perforators can be easily attached to skin-pedicled flaps ( Fig. 52.4 A–C). If we harvest a skin-pedicled flap from the dorsal area, many perforators are also available, including the circumflex scapular vessels, the superficial cervical artery perforators (trapezius muscle perforators of transverse cervical vessels), and the dorsal intercostal perforators including the latissimus dorsi paraspinal perforators ( Fig. 52.5 ). Which of these flaps is most suitable for individual patients depends on the size of the perforator and the geometry and size of the flap to be transferred.
(A) According to the selection of supercharged vessels, long and large flaps can be harvested on the chest wall. Internal mammary artery perforators (IMAPs) can be found and used. (B) A male in his 20s with the anterior neck contracture reconstructed by a large 22-cm × 7-cm skin-pedicled flap. The second IMAP was attached to the flap and anastomosed with the facial artery and veins. The flap survived fully, and the contracture was effectively released. (C) The flap maintained its release after 18 months. (D) A male in his 70s with the anterior neck contracture reconstructed by a large 28-cm × 6-cm skin-pedicled flap. The second and seventh IMAPs were attached to the flap, and only the second IMAPs were anastomosed with the facial artery and veins. The flap survived fully, and the contracture was effectively released. (E) The flap maintained its release after 3 years.
(A) According to the selection of supercharged vessels, long and large flaps can be harvested on the dorsum. Circumflex scapular vessels and dorsal intercostal perforators can be found stable and used. (B) A female in her 30s with the anterior neck contracture reconstructed by a large 35-cm × 19-cm skin-pedicled flap. The circumflex scapular vessels and the seventh dorsal intercostal perforators were attached to the flap, and both were anastomosed with the facial vessels and transverse cervical vessels, respectively. The flap survived fully, and the contracture was effectively released. (C) The circumflex scapular vessels and the seventh dorsal intercostal perforators are attached to the flap and anastomosed with the facial vessels and transverse cervical vessels, respectively. (D) The flap release and inset can be seen here after 3 months. (E) The flap release and inset can be seen here after 4 years.
Regarding recipient sites, the facial artery, the transverse cervical artery, the suprathyroid artery, and the superficial temporal artery can be used for anastomosis with supercharged vessels. If the pedicle length is short and does not reach the recipient’s vessels, it can be rotated and anastomosed ( Fig. 52.6 ).