Sarcoidal
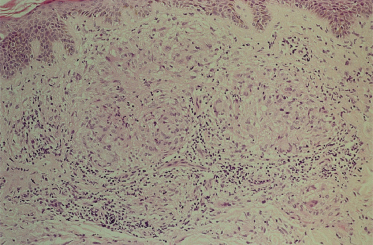
An uncommon pattern, seen in about 3% of cases [86] although relatively more common in localized than generalized granuloma annulare [89], is the formation of epithelioid nodules (Fig. 93.2). There is usually some degree of infiltrative change beyond such nodules. If present, eosinophils and central mucin can be helpful in distinguishing this pattern from sarcoidosis.
Fig. 93.2 Dermal granuloma annulare. Sarcoid-like accumulation of epithelioid cells with peripheral lymphocytes.
Courtesy of Professor J.W.B. Bradfield, Bristol Royal Infirmary.
Subcutaneous Granuloma Annulare
In subcutaneous granuloma annulare the areas of necrobiosis tend to be larger and may extend through the fat, and rarely into underlying structures such as muscle [93].
Vasculitis and Vascular Occlusion
Vasculitis with endothelial swelling, necrosis of the vessel wall, neutrophil debris and even occlusion is sometimes seen [67], perhaps more with the palisading granuloma pattern [86], but is not necessarily the earliest event and neutrophils may be present without vasculitis [69]. Deposition of amorphous material in the basement membrane region of capillaries is also seen, especially in generalized granuloma annulare, reminiscent of diabetic microangiopathy [89].
Elastic Tissue
Elastic tissue is reduced or absent in the necrobiotic areas, particularly in generalized granuloma annulare [94], and phagocytosed elastotic material can often be seen in individual histiocytes [95]. These changes can also occur in subcutaneous nodular granuloma annulare.
Epidermal and Follicular Perforation
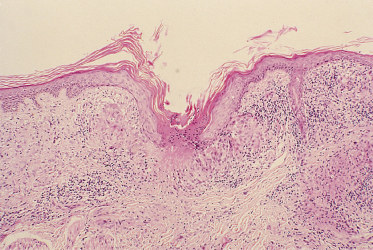
In most cases of granuloma annulare the epidermis is normal, although it may be thinned, particularly in the papular umbilicated type [96]. However, in perforating granuloma annulare, an underlying necrobiotic granuloma communicates to the surface through an epidermal defect [97] (Fig. 93.3). There is usually some epidermal hyperplasia at the edge of the perforation. A variant of this process is transfollicular perforation [98].
Fig. 93.3 Perforating granuloma annulare. Extrusion of necrobiotic material through a breach in the epidermis.
Courtesy of Professor J.W.B. Bradfield, Bristol Royal Infirmary.
Histochemistry
The mucin in granuloma annulare is colloidal iron positive, hyaluronidase labile, Alcian blue positive at pH 3.0 but negative at pH 0.4 and toluidine blue positive at pH 3.0 but not at pH 2.0. Abundant hydrolase and esterase activity is found, typical of a histiocytic infiltrate. Perhaps distinctive for granuloma annulare is possible staining for lysozyme, compared with necrobiosis lipoidica and rheumatoid nodule, which are negative [99]. There is evidence of both increased collagen production [100,101] and collagenase [102].
Immunocytochemistry
Necrobiotic areas are rich in fibrin. Immunoglobulin and C3 are sometimes but not regularly seen in vessel walls [67,86,103]. Immunoperoxidase techniques have shown activated T-lymphocytes with an excess of CD4+ helper/inducer cells and CD1a+ dendritic cells, i.e. Langerhans cell phenotype, in the perivascular and granulomatous infiltrates [82,104]. Interleukin 2-positive cells and IL-2 receptor-positive cells were also increased, as occurs in cell-mediated responses [82]. The histiocytes may be a locally derived, immunocytochemically distinct population [105].
Electron Microscopy
The ultrastructural details of collagen and elastic tissue degeneration, fibrin accumulation and multilayered basal lamina thickening around capillaries have been described [86,89,106]. A surprising finding in the endothelial cells has been the presence of Birbeck granule-like structures [107].
Clinical Features
Prevalence
Point prevalence in the community has never been determined. It has been stated that 0.1–0.4% of new patients (all ages) attending dermatologists have granuloma annulare [47]. Granuloma annulare can occur at any age but overall is most common in children and young adults [5]. Some clinical subtypes are, however, almost always reported in children: the subcutaneous ‘pseudo-rheumatoid nodule’ and the papular umbilicated type [96]. Generalized granuloma annulare occurs in children [108], but in a series of 100 patients only 8% were under the age of 20 years [52]. The reported female predominance for generalized granuloma annulare [52] probably does not apply in the paediatric age range.
Familial cases have been recorded (see above).
The uncommon variety, perforated granuloma annulare, may be more common in Hawaii than elsewhere [109], but there are no other reports to suggest a geographical or racial basis for differences in prevalence.
Seasonal fluctuation in granuloma annulare has been described, with lesions appearing on the elbows in spring and subsiding in October [110], but such changes have not been described in other patients.
Localized Granuloma Annulare
This is the most common form in children. Lesions are single or a few in number. The most easily recognizable pattern is a ring composed of smooth, firm papules, often coalescent with each other (Figs 93.4, 93.5). Papules may be skin coloured, red, violaceous or paler than surrounding normal skin, and can be made more visible by stretching the skin between the finger and thumb.
Isolated papules as well as ring-shaped configurations may be present, and sometimes the subcutaneous form (see below) may co-exist. The rings gradually enlarge but are usually less than 5 cm across. They may be multiple. Sometimes the papular component is not evident, the lesions presenting as purplish rings (Fig. 93.6). Rarely, they may be notably inflammatory and oedematous [16].
The skin surface is usually normal over localized granuloma annulare, although on exposed sites the stratum corneum can have a compacted shiny appearance.
The most common sites are the backs of the hands, fingers, tops of the feet, legs and forearms [5], although granuloma annulare has been reported on almost all body sites including the ear [111] and the eyelid [112].
Granuloma annulare has been recorded on the buccal mucous membrane [113], but this isolated report was in an adult with acquired immune deficiency syndrome (AIDS). Lesions are usually asymptomatic, but can be painful, especially on the hands and feet. Occasionally, the lesions itch.
Linear Granuloma Annulare
Granuloma annulare has been described in a Blaschkoid distribution, followed after 5 years by generalized lesions [114].
Generalized Granuloma Annulare
The individual lesion in generalized granuloma annulare is usually a small skin-coloured papule, although macules and nodules can occur, and the colour may be erythematous, yellowish or violaceous. There is no surface change. The distinctive annular configuration of lesions is only seen in about two-thirds of cases [52]. Sometimes lesions aggregate into reticulate and circinate patterns. Lesions are widespread, symmetrical and when non-annular tend to favour the trunk more than the limbs. In some cases, the disease occurs mainly on sun-exposed sites. Unusual variants (so far only described in adults) include diffuse swelling of the hands [115], sclerotic plaques [116] and sparing of vaccination sites [117,118]. The eruption may be disfiguring but is otherwise usually asymptomatic. If the lesions are stated to be painful or disabling but are evidently not so, the diagnoses of Munchausen syndrome by proxy or non-accidental injury should be considered [119].
It is impossible to say from the literature whether generalized granuloma annulare in children is significantly associated with diabetes and hyperlipidaemia as it may be in adults [52,118].
Subcutaneous Granuloma Annulare
This variant of granuloma annulare has been described under several synonyms including benign rheumatoid nodule, pseudo-rheumatoid nodule, isolated subcutaneous nodule, subcutaneous palisading granuloma and palisading granuloma nodosum [120]. It most commonly occurs in younger children and is rare beyond the second decade.
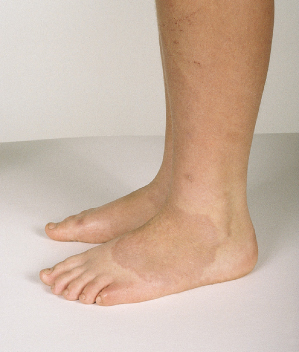
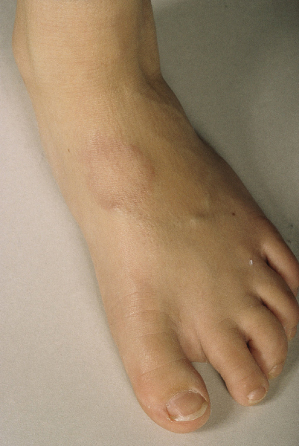
The lesion usually presents as a nodule or mass, which may be rapidly growing at presentation. It may be mobile but often appears to be fixed to underlying periosteum or muscle. Lesions are frequently multiple. The characteristic sites are the lower limb, especially the foot (Fig. 93.7) and pretibial area, hands, forearms and scalp [121–123]. The occiput is the most common location of the scalp to be affected. Subcutaneous GA around the eyes is well described [124] and can even extend beneath the periosteum [125]. The palms and soles are occasional sites [126]. Lesions are usually asymptomatic.
Typical localized granuloma annulare can occur elsewhere: in 25% in one series of 54 cases [10]. In most cases, subcutaneous granuloma annulare in children is not associated with any systemic disease [93,120–122] although with long-term follow-up small numbers of children do develop rheumatoid factor or even rheumatoid arthritis [127,128] and diabetes mellitus [129]. Whether these few cases are intrinsically different from the majority, in whom there is no systemic disease, remains to be established.
Imaging
Because of concerns regarding possible malignancy, imaging techniques have been useful in the evaluation of subcutaneous granuloma annulare. Ultrasound shows an ill-defined mass hypoechoic to the surrounding fat and a cystic or vascular lesion can usually be excluded [130]. On plain radiography the nodules are radiodense with no evidence of mineralization. Computed tomography (CT) shows a mass isodense with muscle, often with a stellar appearance [131]. Magnetic resonance imaging (MRI) [132–134] shows a mass with low signal intensity on both T1- and T2-weighted images, with homogeneous enhancement after intravenous gadolinium. There may be a peripheral high signal. There is no infiltration of muscle or bone.
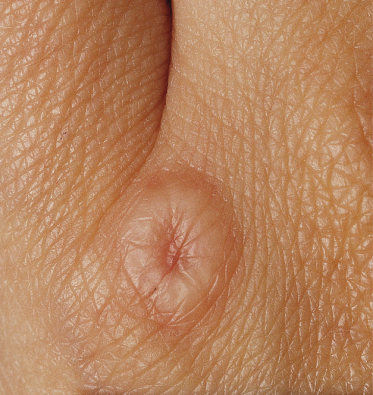
Perforating Granuloma Annulare and Papular Umbilicated Granuloma Annulare
There is probably a spectrum of change variously reported as perforating granuloma annulare [97] and papular umbilicated granuloma annulare [96], in which a breach in the epidermis with transepidermal elimination of necrobiotic connective tissue is sometimes but not always seen.
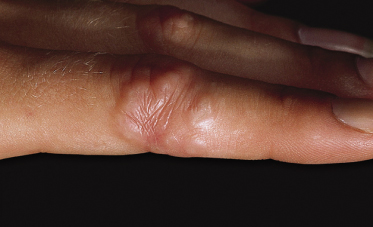
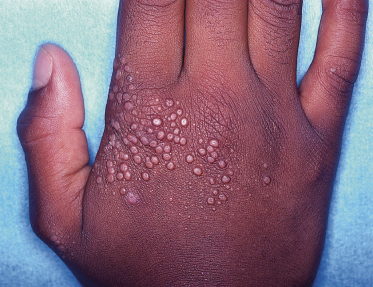
Lucky et al. [96] reported four cases of an eruption of asymptomatic papules symmetrically located on the dorsa of the hands and fingers in four boys. The papules were 1–4 mm in diameter, smooth, flesh coloured to hypopigmented, usually flat topped, but some with central depressions (Fig. 93.8). There were occasional typical localized granuloma annulare lesions. The histology of these cases showed no true perforation, although some of the other features associated with perforating granuloma annulare were minimally present.
Fig. 93.8 Discrete dermal papules, many are umbilicated.
Courtesy of Dr Anne W. Lucky, and the Archives of Dermatology.
In cases described as perforating granuloma annulare, umbilication of the papules is a feature, the depressed centre sometimes being associated with discharge of viscous or creamy material, or with scale or crust [97,135]. The localized form is typically over the backs of the hands and sides of the fingers and the condition can be generalized [47]. When widespread, the arms and legs are frequently involved [108]. The incidence of widespread perforating granuloma annulare may be higher in Hawaii than elsewhere.
Prognosis.
Granuloma annulare is ultimately a self-limiting condition, and only very rarely has it been associated with tissue destruction and scarring [52]. In a single case of granuloma annulare in a child, the condition was followed by mid-dermal elastolysis [136]. Localized granuloma annulare can last from months to more than 20 years, although it has been stated that 50% of cases clear spontaneously in 2 years [47]. About 40% of all patients, children and adults, may experience recurrent eruptions, usually at the same sites, but these tend to resolve more quickly than primary lesions [5].
Generalized granuloma annulare lasts on average 3–4 years but can last a decade or more [52]. Subcutaneous granuloma annulare lesions also tend to last months to several years, all resolving by the second decade [121].
Individual lesions of granuloma annulare have been observed to resolve after biopsy, although this phenomenon is rarely reported [137].
Differential Diagnosis.
Clinical appearances and a characteristic location will enable a diagnosis to be made in most cases of typical localized granuloma annulare. Occasionally, ring-shaped arrays of warts can be confused, but the surface is verrucous. Knuckle pads are flesh-coloured thickenings confined to knuckles. Tinea corporis will have a scaly periphery, and confirmation is easily made by microscopy and culture. Other asymmetrical or localized annular disorders that may occasionally mimic granuloma annulare include lichen planus, erythema annulare centrifugum, secondary syphilis [138], sarcoidosis and erythema elevatum diutinum. When in the form of plaques, granuloma annulare may be mimicked by follicular mucinosis, non-X histiocytosis, juvenile xanthogranuloma and xanthomas.
The differential diagnosis of generalized granuloma annulare includes lichen scrofulosorum, lichen nitidus, sarcoidosis, non-X histiocytosis, eruptive xanthoma, secondary syphilis, lipoid proteinosis and lymphoma. In adults, an additional consideration is the papular eruption of HIV infection [139], and this may also be true for children, although it does not seem to have been documented yet.
The differential diagnosis of generalized perforating granuloma annulare includes perforating collagenosis, molluscum contagiosum and lichen nitidus; sarcoidosis can resemble the papular umbilicated variant on the backs of the hands.
Prior to biopsy, there is a wide differential diagnosis for subcutaneous granuloma annulare including tumours, cysts, deep-seated infections, panniculitis and so on. Radiological techniques, especially MRI, can be helpful in some cases [140]. After biopsy, the nodules of juvenile rheumatoid nodule, lupus erythematosus, scleroderma, rheumatic fever and sarcoidosis may occasionally need to be excluded. Occasionally epithelioid sarcoma can mimic deep granuloma annulare, both clinically and histologically, but the tumour cells in the former stain for cytokeratins and the histiocytes in GA show positivity for CD68 [141].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree