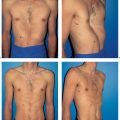
7 Reconstruction of the Nipple–Areola Complex
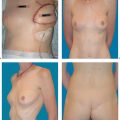
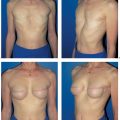
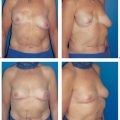
The final step in breast reconstruction is to recreate the nipple–areola complex (NAC). Although many patients initially think that this step is unnecessary, it is only after reconstruction of the nipple and areola that the breast takes on a natural appearance.
Reconstruction of the nipple–areola complex should only proceed once the patient and surgeon are satisfied with the shape and volume of the reconstructed breast. It is virtually impossible to re-correct nipple position.
The shape and position of the new nipple are partly determined by the appearance of the opposite breast. In principle at least, the correct nipple position is at the highest point of the breast mound. However, usually there is slight asymmetry between the reconstructed breast and the “normal” one, and often a compromise has to be made between the actual measurements and the visual appearance. Since some degree of asymmetry also occurs naturally, this is usually readily accepted by the patient. Using the nipple position on the contralateral breast as a guide is always preferable to basing the new nipple site on measurements alone.
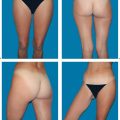
The challenging part of nipple–areola reconstruction is to recreate the most natural-looking nipple possible with stable nipple projection. This is best achieved by taking a nipple graft from the contralateral breast. In autologous tissue reconstruction, excess flap tissue can also provide an excellent basis for recreating a nipple from the skin and underlying fat. This technique is less successful if the breast skin is tight, as is often the case after implant reconstruction.
Areolar tattooing has considerably simplified the reconstruction of the nipple–areola complex. A good alternative is a full-thickness skin graft—from the medial thigh, for example. Horizontal mastectomy scars in particular are difficult to conceal by tattooing, but can be covered extremely well by a skin graft.
Nipple Reconstruction Techniques
Nipple Grafting from the Contralateral Breast
If the contralateral nipple has sufficient projection, it is cut in half horizontally, and after de-epithelialization of the recipient site, it is sutured into the correct position using simple interrupted sutures. The donor-site defect can be closed primarily or can remain open to allow re-epithelialization to occur from the lactiferous ducts.
Patients are often wary of this procedure, fearing loss of nipple sensation and wishing to avoid surgery on the “healthy” breast. Both of these concerns can be allayed. Firstly, it is not possible for sensory disturbance to be cause by a transverse incision of the nipple; and secondly, there is only minimal scarring after reepithelialization and wound closure.
This technique is still the best option for re-creating a natural-appearing nipple ( Fig. 7.3 ).
Intraoperative harvesting of a portion of the ipsilateral nipple is an alternative to using a graft from the contralateral nipple. Intraoperative histopathological diagnosis is mandatory, but it should be noted that even then, there is still a risk of transferring cancer cells.
Local Flaps
A number of local flap techniques have been described. We have found the modified star flap based on the method of Askenazi and Hartrampf to be an excellent option for nipple reconstruction after autologous tissue transfer—for instance, in latissimus dorsi or transverse rectus abdominis muscle/deep inferior epigastric perforator (TRAM/DIEP) flap reconstruction of the breast. The advantage of this procedure is that it does not require an additional skin graft for coverage of the donor site. Instead, the areola is created by tattooing.
Depending on the amount of excess skin available after breast reconstruction, a smaller or larger flap can be cut. Normally, the width of the flap base is drawn according to the width of the opposite nipple ( Fig. 7.1 ). The width of the flap wing should generally not exceed 1.5 cm, as it will otherwise limit natural breast ptosis. The flap length should not exceed that of the planned areola. The flap wing is typically 2 cm in length. After closure of the donor site, the nipple is reconstructed from the small, star-shaped flap. Additional details are provided in the accompanying figures.
We no longer use the skate flap for nipple reconstruction, as it requires a skin graft to cover the defect.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree