Neutrophil-Mediated Diseases 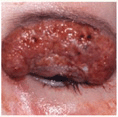
Epidemiology
Rare, prevalence unknown. All age groups affected with a peak between 40 and 60 years. Slight preponderance of females.
Etiology and Pathogenesis
Unknown. Although called pyoderma, it does not have a microbial etiology. PG is counted among the neutrophilic dermatoses because of the massive neutrophilic infiltrates within the skin.
Clinical Manifestation
Three Types. Acute. Acute onset with painful hemorrhagic pustule or painful nodule either de novo or after trauma. There is the phenomenon of pathergy, where a needle stick, insect bite, biopsy, or other minimal trauma can trigger a lesion. Chronic: slow progression with granulation and hyperkeratosis. Less painful. Bullous: true blisters often hemorrhagic and associated with hematologic disease.
Skin Lesions. Acute. Superficial hemorrhagic pustule surrounded by erythematous halo; very painful (Fig. 7-1). Breakdown occurs with ulcer formation, whereby ulcer borders are dusky-red or purple, irregular and raised, undermined, boggy with perforations that drain pus (Fig. 7-2). The base of the ulcer is purulent with hemorrhagic exudate, partially covered by necrotic eschar (Fig. 7-3), with or without granulation tissue. Pustules both at the advancing border and in the ulcer base; a halo of erythema spreads centrifugally at the advancing edge of the ulcer (Fig. 7-3). Chronic: lesions may slowly progress, grazing over large areas of the body and exhibiting massive granulation within the ulcer from the outset (Fig. 7-4) and crusting and even hyperkeratosis on the margins (Fig. 7-5). Lesions are usually solitary but may be multiple and form clusters that coalesce. Most common sites: lower extremities (Figs. 7-2 and 7-5) > buttocks > abdomen (Fig. 7-3) > face (Fig. 7-4). Healing of ulcers results in thin atrophic cribriform scars. Bullous: blisters from the outset, often hemorrhagic, followed by ulceration.
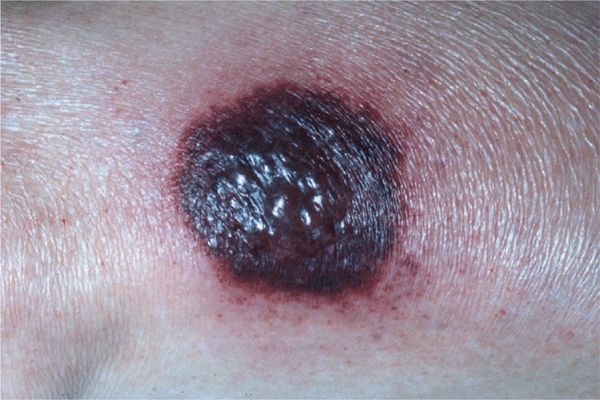
Figure 7-1. Pyoderma gangrenosum The initial lesion is a rapidly enlarging hemorrhagic nonfollicular pustule surrounded by an erythematous halo and is very painful.
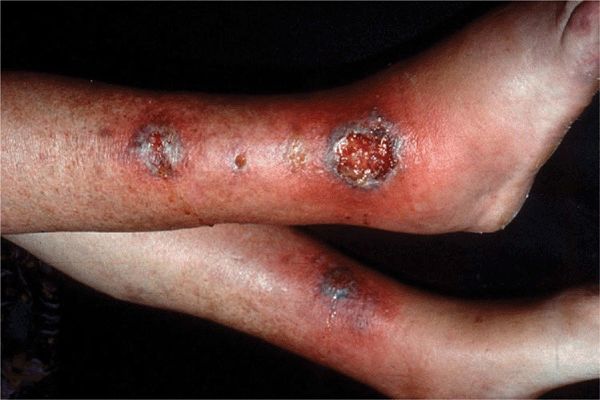
Figure 7-2. Pyoderma gangrenosum Lesions rapidly break down in the center and become boggy, hemorrhagic, and purulent ulcers. Note small abscesses at base of ulcer on left leg.
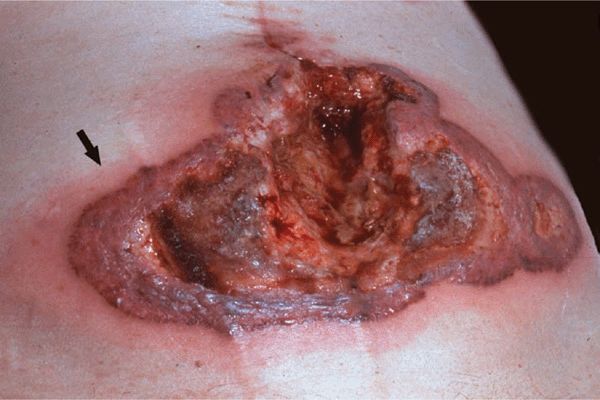
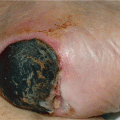
Figure 7-3. Pyoderma gangrenosum A very large ulcer with raised bullous undermined borders covered with hemorrhagic and fibrinous exudate. The arrow indicates erythema surrounding advancing borders of the lesion. When the bullae are opened, pus is drained. This lesion arose acutely and spread rapidly after laparatomy for an ovarian carcinoma.
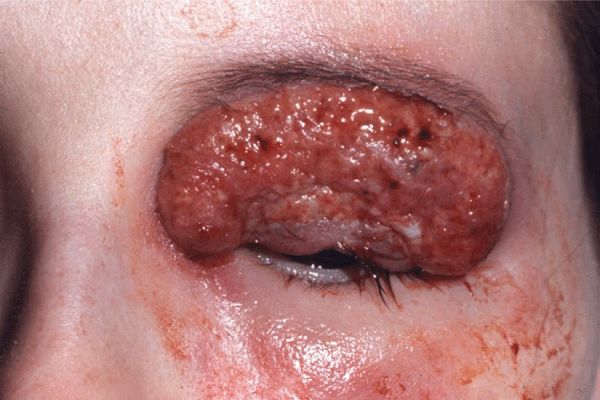
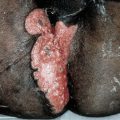
Figure 7-4. Pyoderma gangrenosum: chronic type The lesion involves the upper eyelid and represents an ulcer with elevated granulating base with multiple abscesses. The lesion later spread slowly to involve the temporal and zygomatic regions and eventually healed under systemic glucocorticoid treatment, leaving a thin cribriform scar that did not impair the function of the eyelid.
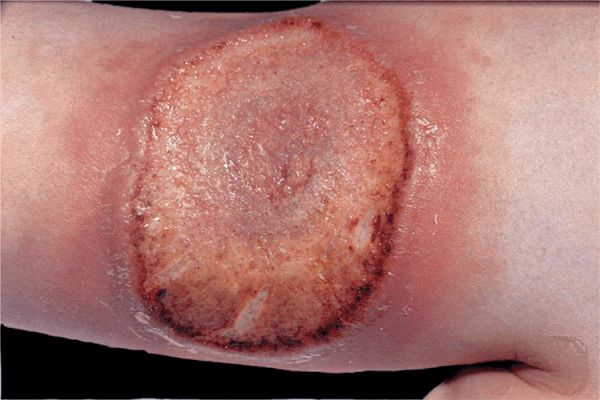
Figure 7-5. Pyoderma gangrenosum: chronic type This lesion, which appears like a plaque, spread only slowly but was also surrounded by an erythematous border. The lesion is crusted and hyperkeratotic and is less painful than the lesions in acute pyoderma gangrenosum.
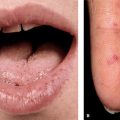
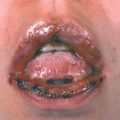
Mucous Membranes. Rarely, aphthous stomatitis–like lesions; massive ulceration of oral mucosa and conjunctivae.
General Examination
Patient may appear ill.
Associated Systemic Diseases
Up to 50% of cases occur without associated disease. Remainder of cases associated with arthritis, large- and small-bowel disease (Crohn disease, ulcerative colitis), diverticulosis (diverticulitis), paraproteinemia and myeloma, leukemia, active chronic hepatitis, Behçet syndrome (which is also a disease with pathergy).
Laboratory Examinations
There is no single diagnostic test.
ESR. Variably elevated.
Dermatopathology. Not diagnostic. Neutrophilic inflammation with abscess formation and necrosis.
Diagnosis and Differential Diagnosis
Clinical findings plus history and course; confirmed by compatible dermatopathology. Differential diagnosis: ecthyma and ecthyma gangrenosum, atypical mycobacterial infection, clostridial infection, deep mycoses, amebiasis, leishmaniasis, bromoderma, pemphigus veg-etans, stasis ulcers, Wegener granulomatosis.
Course and Prognosis
Untreated, course may last months to years, but spontaneous healing can occur. Ulceration may extend rapidly within a few days or slowly. Healing occurs centrally with peripheral extension. New ulcers may appear as older lesions resolve. Pathergy.
Management
With Associated Underlying Disease. Treat underlying disease.
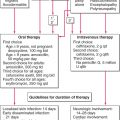
Systemic Treatment. High doses of oral glucocorticoids or IV glucocorticoid pulse therapy (1–2 g/d prednisolone) may be required. Sulfasalazine (particularly in cases associated with Crohn disease), sulfones, cyclosporine, and, more recently, infliximab, etanercept, adalimumab.
Topical. In singular small lesion, topical tacrolimus ointment or intralesional triamcinolone.
 ICD-10:L88
ICD-10:L88 
 PG is an idiopathic, either acute or chronic, severely debilitating skin disease.
PG is an idiopathic, either acute or chronic, severely debilitating skin disease. It is characterized by neutrophilic infiltration, destruction of tissue, and ulceration.
It is characterized by neutrophilic infiltration, destruction of tissue, and ulceration. It occurs most commonly in association with a systemic disease, especially arthritis, inflammatory bowel disease, hematologic dyscrasias, and malignancy, but may also occur alone.
It occurs most commonly in association with a systemic disease, especially arthritis, inflammatory bowel disease, hematologic dyscrasias, and malignancy, but may also occur alone. Characterized by the presence of painful, irregular, boggy, blue-red ulcers with undermined borders and purulent necrotic bases.
Characterized by the presence of painful, irregular, boggy, blue-red ulcers with undermined borders and purulent necrotic bases. There is no laboratory test that establishes the diagnosis.
There is no laboratory test that establishes the diagnosis. The mainstays of treatment are immunosuppressive or modulating agents.
The mainstays of treatment are immunosuppressive or modulating agents. Relapses occur in most patients and there is significant morbidity.
Relapses occur in most patients and there is significant morbidity.