Abstract
Carpal fractures and dislocations are rare injuries, with injury to the scaphoid comprising the majority. Evaluation of patients with suspected carpal injuries begins with thorough history taking as well as detailed physical diagnosis. To correctly diagnose and treat injuries of the carpus a comprehensive understanding of the unique anatomical features, complex interactions between the bones and ligaments, and specific radiological assessments is required. For timely and proper treatment the evaluator must always have a high index of suspicion for these injuries.
7 Carpal Fractures and Dislocations
I. Scaphoid
A. Background
Most common carpal fracture (60%).
Demographics: Young men 15 to 25 years of age.
Risk factors include college football players, military personal, and low socioeconomic class.
Mechanism
Fall onto hyperextended wrist (>95 degrees extension).
Excessive stress at scaphoid waist.
B. Presentation
1. Physical Examination
Tenderness at anatomic snuff box, longitudinal thumb compression, scaphoid tubercle, painful ulnar deviation, and decreased grip strength.
Snuff box tenderness has high sensitivity but low specificity.
Combination of maneuvers is recommended to increase specificity and sensitivity
C. Evaluation
1. Imaging
Radiographs
Standard series (four views): Posteroanterior (PA), lateral, and oblique hand radiographs; scaphoid view radiograph; PA wrist with ulnar deviation (only about 64% sensitive).
If negative on imaging, commonly treated with 2 weeks of thumb spica cast immobilization followed by repeat radiograph.
Overtreat five out of six patients with suspected injuries.
Will miss 9% of scaphoid fractures.
Computed tomography (CT)
Sensitivity = 0.71
Specificity = 0.99
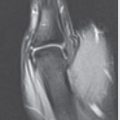
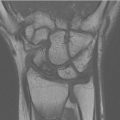
Magnetic resonance imaging (MRI)
Most utilized advanced imaging in North America
Sensitivity= 0.88
Specificity= 0.99
Bone scintigraphy
Highest diagnostic accuracy
Sensitivity= 0.99
Specificity = 0.86
Highest radiation exposure
Diagnostic delay of 72 hours
D. Classification
Many classification systems available, all with varying limitations and clinical utility.
At least 13 based on fracture location/orientation/stability/displacement.
Limitation of classifications
Many rely on radiographs with limited sensitivity and potential underestimation of displacement.
Poor intraobserver reliability.
Most have poor prediction of fracture union.
Specific classifications
Herbert
Stable: Tubercle fractures and incomplete waist fractures.
Unstable: Complete distal oblique fractures, complete waist fractures, proximal pole fractures, and transscaphoid perilunate fracture-dislocations.
Mayo
Location: Distal tubercle, distal intra-articular surface, distal third, waist, and proximal pole.
Rousse
Orientation: Transverse, horizontal oblique, and vertical oblique (highest rates of nonunion and increased shear stress).
E. Management
Treatment algorithms must be personalized and depend on many variables:
Fracture location.
Fracture displacement.
Patient-specific factors.
1. Nondisplaced Scaphoid Waist
Nonoperative: Short arm cast with or without thumb immobilization for 6 weeks. Then obtain CTscan of wrist. IfCTscan demonstrates healing, transition to wrist brace for another 4 to 6 weeks.
Union expected from 2 to 3 months.
Operative
Percutaneous treatment
Recent literature has shown faster time to union with lower complication rate than nonoperative management.
Variables affecting patient’s decision-making for operative versus nonoperative management are out-of-pocket cost and surgical apprehension.
2. Proximal Pole Fractures and Unstable Scaphoid Fractures
Operative management generally recommended
Unstable fractures are defined by over 1 mm of displacement, comminution, associated perilunate fracture-dislocation, intra-scaphoid angle ofover 35 degrees, scapholunate angle of over 60 degrees, or radiolunate angle of over 15 degrees.
Goals ofoperative fixation
Rigid fixation for primary bone healing.
Approaches for operative fixation
A meta-analysis comparing volar and dorsal approaches for acute scaphoid fractures showed no difference in union rates, functional outcomes, or pain.
Volar approach: It divides the radial extrinsic carpal ligaments. It may result in scaphotrapeziotrapezoid (STT) arthritis. There is an increased rate of ulnar deviation with the volar approach, but this is of uncertain clinical significance.
Dorsal approach: It provides more consistent central screw position, but places the scaphoid blood supply and extensor tendons at risk.
Percutaneous.
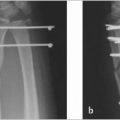
3. Methods of Fixation
Cannulated Herbert screw
Benefits: Improved union rate, improved return to work, and improved functional outcomes.
Technique
Screws should be within the central one-third axis of the scaphoid utilizing the longest screw possible that is ideally perpendicular to the fracture.
Central placement with longer screws will provide greater stiffness, a reduction of forces at the fracture site, and a reduction in time to union.
Anatomic studies show safe screw lengths of 27 mm in men and 23 mm in women.
Arthroscopic-assisted reduction can assist in determining screw length by providing direct visual joint visualization.
Other
K-wires, staples, plate fixation.
Plate fixation may be indicated in osteoporotic fractures.
F. Complications
1. Most Common
Delayed union (time to union >6 months).
Nonunion
Delayed diagnosis and treatment increases the risk for nonunion and may occur in 5 to 25% ofcases.
Post-traumatic arthritis.
Malunion
Amadio et al (1989) reported patients with lateral intrascaphoid angle ofover 45 degrees had unsatisfactory outcomes in 73%ofcases and post-traumatic arthritis in 54%compared to 17% unsatisfactory outcomes without malunion.
Tendon rupture.
Complex regional pain syndrome (CRPS).
Osteonecrosis
Osteonecrosis is seen in 13 to 50%ofscaphoid fractures with higher rates seen in proximal pole fractures.
Prominent hardware.
2. Complication Differences between Nonoperative and Operative Management
In a recent systematic review of minimally and nondisplaced scaphoid fractures, there was no significant difference between operative treatment (14%) and nonoperative treatment (7%) in terms ofcomplications.
The most common complications in the operative group were delayed union, nonunion, and hardware-related complications.
The most common complications in nonoperative group consisted of predominantly delayed union and nonunion complications.
Malunion occurs in both operatively and nonoperatively treated scaphoid fractures where the distal fragment flexes and the proximal fragment extends resulting in a humpback deformity.
II. Perilunate Instability
A. Background
Perilunate dislocations and fracture-dislocations encompass a wide spectrum of injuries and typically result from high energy trauma.
Pure ligamentous perilunate dislocations are referred to as lesser arc injuries while greater arc injuries involve fractures most frequently of the scaphoid.
Mayfield et al (1980) described progressive perilunate instability in four stages:
Stage 1: Hyperextension of the carpal row with failure of the scapholunate ligament as the scaphoid extends beyond the limits of the lunate.
Stage 2: Dorsal dislocation of the scaphoid and distal carpal row from the lunate (perilunate dislocation).
Stage 3: The third stage occurs with continued hyperextension that now results in the fracture of the triquetrum or rupture of the lunotriquetral ligaments as the triquetrum extends.
Stage 4: Results from an intact radioscaphocapitate (RSC) ligament pushing the capitate proximally with the lunate then dislocating.
Herzberg et al (1993) further subclassified lunate dislocations based on lunate rotation:
Worsening results were seen with increasing lunate rotation and were attributed to higher energy mechanisms with increased ligament injury and soft tissue interposition.
B. Presentation
Relatively limited physical examination findings beyond pain, decreased wrist range of motion, and possibly carpal tunnel related symptoms.
Diagnosis requires a high index of suspicion following high energy wrist trauma.
C. Evaluation
Radiographs
PA, lateral, and oblique wrist:
Perilunate dislocation will show disruption of Gilula’s lines with a loss of carpal height.
Lateral view may show dislocation of the capitate or lunate.
D. Classification
As described by Mayfield et al (1980) and Herzberg et al (1993).
E. Management
1. Initial Management
Reduction of any carpal dislocation
Usually requires complete muscular relaxation, axial traction, and recreation of initial injury mechanism followed by reduction.
Dorsal dislocation: Thumb should be placed volarly to prevent conversion to a volar lunate dislocation.
Prompt surgical management
Nonoperative management is not advised: Persistent carpal instability, pain, weakness, and delayed surgical management result in worse outcomes.
2. Methods of Surgical Management
Approaches:
Dorsal midline with or without volar component:
Arthroscopy can be useful; further diagnose ligamentous injuries, assess chondral injuries, and assist with reduction.
Specific injury patterns and their management
Greater arch injuries: Reduction of fracture typically required; usually scaphoid; 95% of fractures will be in middle third; amenable to cannulated screw, but may require bone grafting if comminuted.
Ligamentous injuries: Scapholunate interosseous ligament (SLIL)—suture anchor with Kirschner wire (K-wire); lunotriquetral interosseous ligament (LTIL)—suture anchor with K-wire.
3. Outcomes
Studies on long-term outcomes for perilunate instability are limited to case series with varying methods of treatment.
In a study by Krief E et al (2015) on perilunate dislocations with minimum 18 years follow-up, 70% ofpatients developed radiographic arthritis.
Clinical and functional outcomes did not correlate with radiographic arthritis.
There was also a loss of ROM of wrist with an average arc of 90 degrees (35-140 degrees).
III. Triquetrum
A. Background
Triquetral fractures are uncommon, but after scaphoid fractures, they are the second most common isolated carpal fractures.
Up to 15% ofcarpal fractures.
Mechanism
Typically result from a fall onto an outstretched hand with wrist in dorsiflexion and ulnar in deviation.
Ligament avulsion fractures: Both intrinsic and extrinsic ligaments attach to triquetrum; thus many different ligaments are implicated. Volar avulsions are typically avulsions of the palmar ulnar triquetral or the lunotriquetral ligament.
Direct compression: Compression against ulnar styloid or hamate.
B. Presentation
Focal tenderness on the dorsum of the triquetrum after a fall.
C. Evaluation
1. Radiographs
PA, lateral, and oblique radiographs of the hand.
45 degrees pronated oblique view
Will view the triquetrum on profile
Can be especially helpful with dorsal fractures.
Radial deviation
May be useful for volar avulsion fractures.
2. CT
Has seen increased usage for fracture characterization and diagnosis confirmation.
D. Management
1. Nonoperative
Dorsal chip fractures
Cast immobilization for 4 to 6 weeks at the most; rich vascular supply; low rate of complications.
Volar avulsions
Mainstayoftreatment involves management ofpotential carpal instability through cast immobilization and not the avulsion itself.
2. Operative
Specific indications are sparse in the literature and clouded by other associated injuries.
Determined based on the presence of associated injuries as well as degree of fracture displacement.
Typically reserved for triquetral body fractures:
Herbert compression screw.
K-wires.
Some associated triangular fibrocartilage complex tears have been associated with dorsal triquetral fractures, and are potentially amenable to repair if patient notes persistent ulnar sided pain after bony healing has occurred.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree