64 Nipple–Areolar Reconstruction
Summary
This chapter reviews the commonly accepted techniques for nipple reconstruction following mastectomy. Local and distant donor tissue options are covered with a detailed section on tattooing and the newer 3D techniques.
Key Topics
Determining nipple–areolar position.
Nipple reconstruction techniques:
C–V flap and modified C–V flap with dermal shelf.
Fishtail flap.
Skate flap and modified skate flap without areolar grafting.
Contralateral nipple-sharing.
Salvage full-thickness grafts.
Areolar reconstruction techniques:
Tattoo alone.
Nonspecific tissue grafting with tattoo.
Upper inner thigh graft.
Bilateral nipple–areolar reconstruction.
Key Teaching Points
Nipple-sharing is preferred if the patient has a donor nipple to share.
Local flaps work well on thick latissimus flap skin, moderately well on abdominal skin flaps and relatively poorly in thin, expanded skin.
Thin skin flaps may need augmentation with acellular dermal grafts in order to provide projection.
Siting the nipple reconstruction in the correct position is critical to a successful outcome.
All local flap-based nipple reconstructions will shrink with time.
Tattoos will fade and will often need revision after 1 to 2 years.
If skin flaps are used in thin-skinned patients, meticulous closure should be performed to ensure that implant exposure does not occur.
Observations
Much of the creativity and artistry of breast reconstruction involves applying the finishing touches to perfect and naturalize the restored breast mound and its surrounding structures. Meticulous attention to detail and careful surgical manipulation are requisite. There are no absolute patterns to serve as a model; treatment of each patient is individualized in accordance with her particular desires, tissue availability, and anatomical configuration.
As our ability to create a more realistic breast mound has improved in recent years, our patients have also become more demanding in their aesthetic expectations. The nipple–areola represents the ultimate finishing touch, transforming the reconstructed mound into a breast. When breast reconstruction is done correctly and the nipple–areolar reconstruction is attractive, the overall result is pleasing and natural. When the underlying breast reconstruction becomes deformed by capsular contracture or is displaced as it settles, the position, size, and shape of the nipple–areola may change unpredictably, deteriorating until it becomes aesthetically unacceptable.
64.1 Determining Nipple–Areolar Position
The position of the nipple on the breast mound can profoundly affect the appearance of symmetry. A well-shaped breast mound with an eccentrically placed nipple will appear distorted and asymmetrical. In addition, unilateral breast reconstructions have a tendency to become asymmetrical over time, which affects nipple–areolar positioning, particularly when the opposite breast is soft, mobile, and ptotic.
Technical Pearl
The reconstructed breast typically lacks mobility and does not elevate readily. Thus, it is a challenge to position the reconstructed nipple–areola so that it looks correct with and without a brassiere.
A patient may have a reconstructed nipple forming a symmetrical, equilateral triangle with the opposite nipple and sternal notch, but if the inframammary fold to nipple distance differs between the two sides, the reconstructed nipple will appear to be incorrectly located. The patient may have to make a choice. This dilemma needs to be discussed with her, especially if her nipple projects prominently and will be visible through the brassiere. Most patients request that the nipple–areola be placed properly on the reconstructed breast to match the other breast without a brassiere rather than eccentrically to simulate the other breast’s appearance in a brassiere.
Technical Pearl
Specific identifiable landmarks help to determine the proper nipple–areolar position visually and geometrically. These include the level of the nipple–areola, the triangles with the sternal notch and the umbilicus, and the nipple–areolar position relative to each breast and to the inframammary fold.
In ideal, youthful breasts the nipples will form an equilateral triangle with the sternal notch. These landmarks provide general guidelines for positioning but are not nearly as useful as proper visualization of the position with the patient’s help, which should be the determinant when making final decisions about the proper location of the nipple–areola. Whereas the nipple–areolar reconstruction should be symmetrical with the opposite breast, the nipple reconstruction should not only match the opposite nipple but should also be situated centrally within the areola.
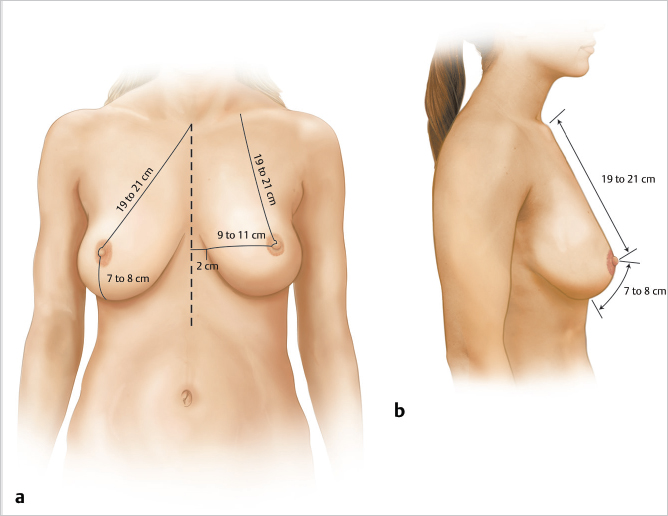
The nipple–areolar position is determined visually with the patient standing and her shoulders relaxed. If markings are made with her shoulders back, the reconstructed nipple–areola will tend to be too high postoperatively. If the arm is abducted, markings may also be inaccurate, because the nipple–areola is displaced upward and outward, distorting the circular areola (▶Fig. 64.1).
64.1.1 Positioning for Delayed Nipple Reconstruction
It is my usual practice to delay nipple reconstruction for at least 6 weeks after completion of the breast mound. This carries the advantage of allowing the breast position to settle as edema resolves and gravity exerts its effect. The nipple–areola is centered on the breast at the point of maximal convexity and projection, symmetrical with the opposite nipple–areola. Formulas or geometric patterns have not served me well.
Technical Pearl
The nipple–areolar position simply must “look right.” Proper appearance takes precedence over measurements, which merely confirm the accuracy of the visual positioning.
If nipple reconstruction is planned with a C–V flap or a nipple graft, the nipple is marked at the apex of the breast mound in a position which most closely matches the opposite side. The areola can be tattooed subsequently, which is my preference, or it can be tattooed at the time of nipple reconstruction in one operative sitting. If nipple reconstruction is planned with the skate flap, both the nipple and the areola are reconstructed in one setting. This mandates that the proposed nipple–areola be marked on the recipient site so it will most closely match the size and diameter of the nipple–areola on the opposite side.
Technical Pearl
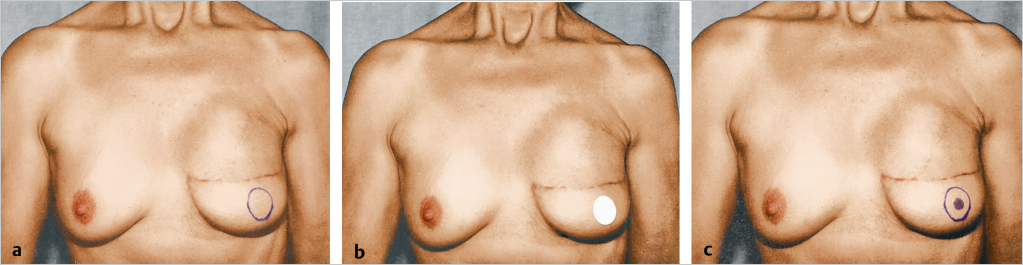
To help the patient visualize placement, an adhesive circle of a diameter similar to that of her opposite nipple or nipple–areola can be positioned and adjusted in various positions on her reconstructed breast. The patient and surgeon check the position looking down from the patient’s perspective and also in a full-length mirror.
I ask the patient to confirm the proposed nipple or nipple–areolar position and size; it should look right both to her and to me when viewed from the front and from above. Ultimately, patient satisfaction and acceptance are directly related to the patient’s sense of involvement in decisions concerning her surgery. It is understandable if she places the entire blame for any asymmetry (and there will always be some) on her reconstructive surgeon if he or she has not involved her in the decision-making process. This is particularly true for many breast cancer patients, who feel a compelling need to control their destinies and bodies. Soliciting patient input does not detract from the surgeon’s ability to produce an aesthetic result, but ensures an engaged, cooperative patient who understands problems if they occur (▶Fig. 64.2).
64.1.2 Positioning for Immediate Reconstruction
I generally do not perform immediate nipple reconstruction, regardless of whether I am dealing with an immediate or a delayed breast reconstruction. Although some surgeons do so, I have always been concerned that the influence of gravity, edema resolution, and the uncertainties of scar contracture may distort the final resting position of an immediately reconstructed nipple. It is most easily performed in a patient undergoing bilateral prophylactic mastectomies with free nipple grafting when a significant mastopexy effect is required to reshape her breasts although many of these patients can now be treated with mastopexy/reduction several months prior to mastectomy which allows preservation of the vascularized nipple on a dermal pedicle without resorting to grafting at the time of mastectomy. The use of nipple-sparing mastectomy has altered these requirements somewhat. Careful preoperative markings define the new position of the nipple–areolae. They are placed approximately 1 cm medial to the midbreast line to ensure that they will not drift laterally in the postoperative period.
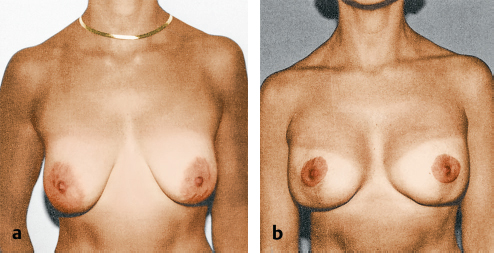
This patient had bilateral prophylactic mastectomies, followed by immediate breast reconstruction with tissue expanders that were exchanged for permanent implants. Nipple reconstruction was done with specialized tissues. The nipple–areolae were removed from the mastectomy specimens as full-thickness grafts and positioned on the reconstructed breast to give the best position and symmetry (▶Fig. 64.3).
64.2 Options for Nipple Reconstruction
See ▶Fig. 64.4.
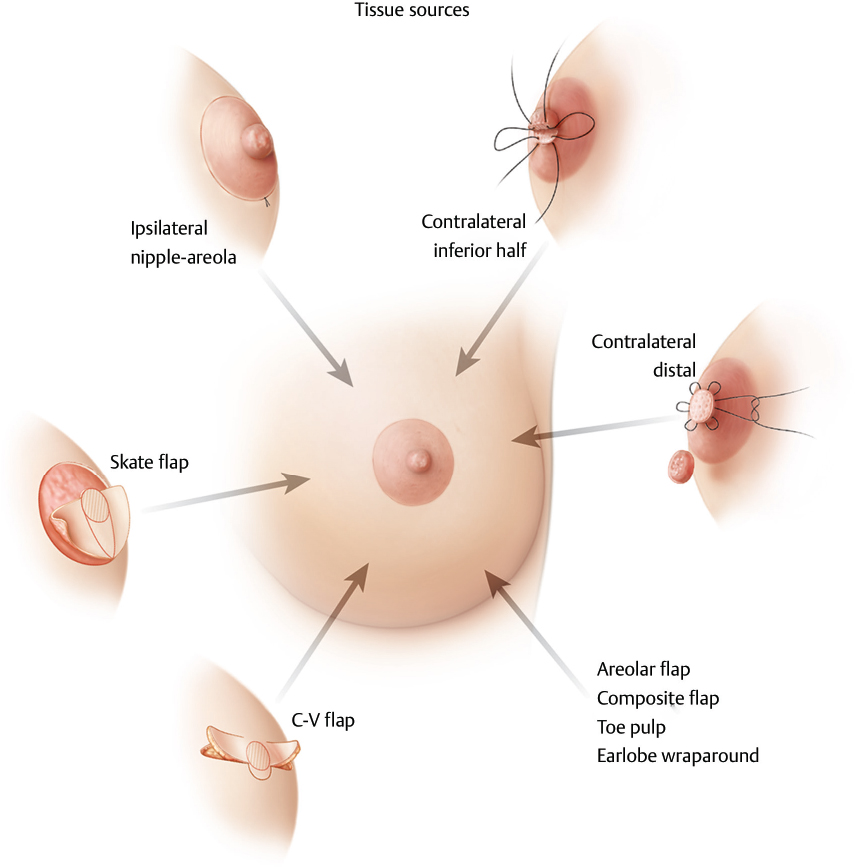
Techniques for Nipple Reconstruction
Local flaps can be used for construction of the nipple, including the following:
C–V.
Modified C–V with dermal shelf.
Fishtail.
Skate (creates both nipple and areola).
Modified skate without areolar grafting.
Contralateral nipple-sharing.
Salvage full-thickness grafts.
Earlobe.
Labia minora.
64.3 The Impact of Breast Reconstruction Technique on Nipple Reconstruction Outcome
The single most pressing issue in nipple reconstruction is maintaining longterm projection. This is strongly influenced by the tissues available for flap design. Nipple projection is most durable when the dermis of the flaps is thick and there is adequate subcutaneous tissue to reinforce the volume of the reconstructed nipple. The thinner the dermis, and the less subcutaneous fat that is present, the more likely that there will be partial or complete loss of projection. With these issues in mind, it is intuitive that the most durable nipples with the most satisfactory projection are achieved using the thick skin of the latissimus dorsi flap, followed by the less-thick skin of the abdomen, and finally by the thinnest skin of an expanded mastectomy skin flap with implant reconstruction. In recent years, the availability of fat grafting or acellular dermal grafts has allowed us to augment an inadequate flap donor site preoperatively in preparation for definitive nipple reconstruction.
64.4 Operative Technique
64.4.1 C–V Flap
The C–V flap, which evolved from the skate flap, is a versatile and reliable method for breast reconstruction. It uses local tissue and is most applicable and predictable after autologous tissue reconstructions with thicker subcutaneous tissues. The C–V flap is the technique I currently use most frequently for most nipple reconstructions if the opposite nipple is not available for nipple-sharing. This flap permits medium-to-moderate–size nipple reconstructions with primary closure of the donor site. The advantage of this approach is that a full-thickness graft or a skin graft is not needed for the areolar site. The volume of the flap depends on the volume of the underlying subcutaneous tissues as well as the width of the flap base, which will determine the final nipple length. The limits of this procedure are obvious in patients who have very thin skin with no underlying subcutaneous tissues. It is not possible to reconstruct a nipple of significant volume over very thin tissues covering a tissue expander or an implant.
The basic concept of the C–V flap nipple reconstruction is straightforward. The nipple design is composed of two V flaps and a C flap. The width of the two V flaps determines the projection of the nipple, whereas the diameter of the C flap determines the diameter and the top of the new nipple reconstruction. The flaps are designed as a V to permit primary closure, and the C flap is incised to cap the nipple reconstruction. Harvesting of the C portion of the flap permits a circular site for insetting the V flaps.
Technical Pearl
The flap is planned to the proper diameter; however, an additional 50% projection is planned to provide the best long-term result and to allow for shrinkage of the tissues after flap reconstruction. Composite nipple grafts do not shrink as much.
The position of the C–V flap is determined by placing a mark on the breast that matches the position of the opposite nipple with the patient in the upright position. This is only done after breast contour and shape are satisfactory. The patient’s input as to the proper nipple position is essential and probably the most important aspect of this positioning. It must look right to her. I usually let the patient check the positioning in a mirror.
Markings and Technique
The C–V flap is designed based on the site and the diameter planned for the new nipple. The diameter of the C flap will be similar to that of the final nipple diameter, and the overall circumference of the two V flaps will approximate the circumference of the new nipple. The Vs on each end are designed to permit primary closure of these sites, and the tips of the Vs are sometimes trimmed.
Incisions are made to define the two V flaps and the C flap. Care should be taken not to divide the base of the flap or the attachment of the C flap to the vertical wall. The blood supply to this flap comes from the underlying subcutaneous tissues; thus, it is important to leave the subdermal plexus in those subcutaneous tissues intact (▶Fig. 64.5).
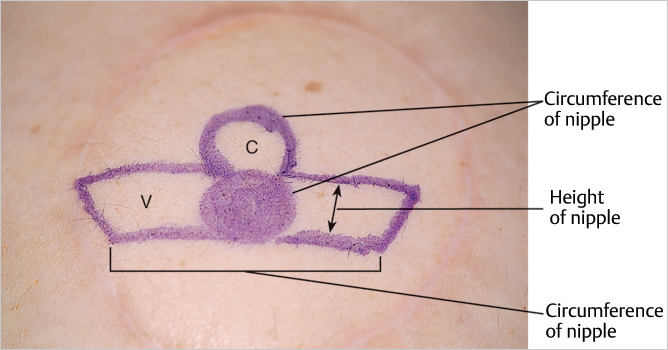
The two V flaps are then elevated from the underlying subcutaneous tissue (▶Fig. 64.6). The subdermal plexus is left on these as well as some fatty tissue, depending on the requirements for the fullness of the nipple.
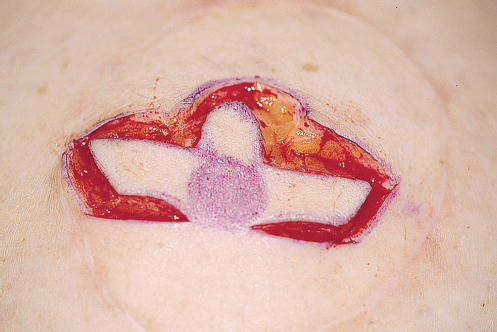
Technical Pearl
The flaps are thinned more toward their periphery than centrally to avoid devascularizing the tip of the flaps (▶Fig. 64.7)
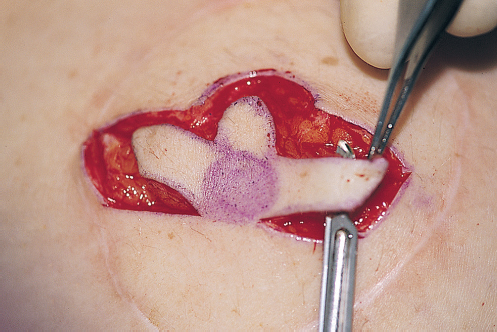
The C flap is also thinned and the subcutaneous tissue preserved in the central area of the proposed new nipple. This central tissue will provide blood supply as well as central bulk for the nipple.
The C–V flap is gradually lifted by elevating the flap and releasing some of the tightness while preserving the blood supply to the base of the flap, which also supplies the two V flaps and the C flap (▶Fig. 64.8).
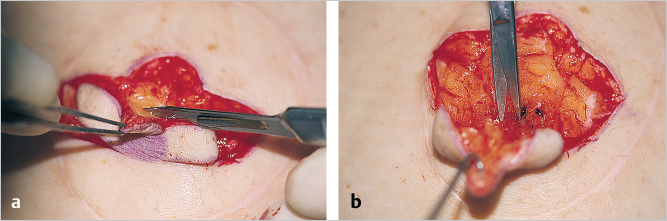
The initial flap closure involves suturing the donor base of the C flap to the base of the V flap on both sides. This effectively closes the donor site and brings the site of the C flap in as a circle to define placement of the nipple reconstruction. I use absorbable sutures (4–0 Monocryl) to approximate these two donor site flaps (▶Fig. 64.9).
After the donor sites are closed, the two V flaps and C flap are trapped outside. The V flaps appear as wings and the C flap appears as a cap.
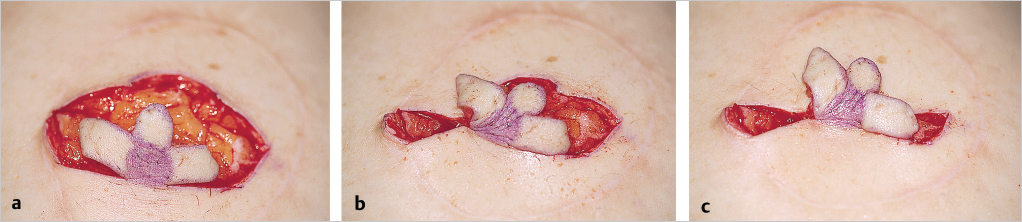
When these flaps are positioned, it can be seen that the width of the V flaps determines the vertical height of the nipple and the C flap is the top of the nipple reconstruction (▶Fig. 64.10).
The first suture secures the lowest points of the two V flaps to the center portion of the original site of the C flap. The suture locks in the V flaps. After the initial suture of the V flaps, the vertical portion of the nipple is reconstructed (▶Fig. 64.11).
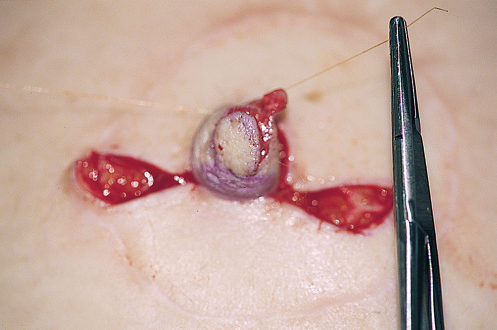
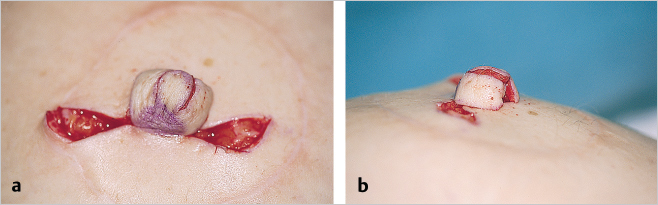
The tips of the V flaps are removed so that a vertical line can be sutured along the height of the nipple reconstruction (▶Fig. 64.12).
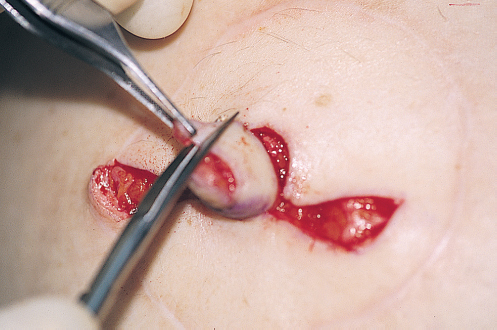
The C flap is then sutured to the upper portion of the V flaps by a single suture that grasps the tips of the V flaps in a horizontal mattress suture in the C flap and goes through the other V flap. Next, the C flap is placed down onto the vertical walls of the V flaps to form a cap (▶Fig. 64.13).
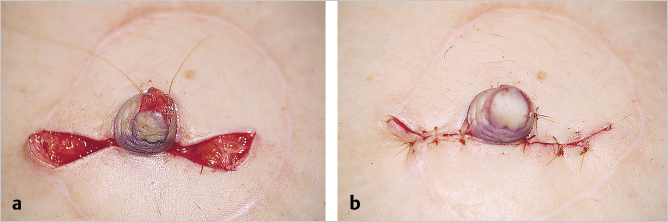
The donor site skin is closed with horizontal sutures of 5–0 plain catgut suture. These horizontal sutures permit direct closure and avoid the need for suture removal later.
The opposite nipple diameter and projection are shown for comparison (▶Fig. 64.14).
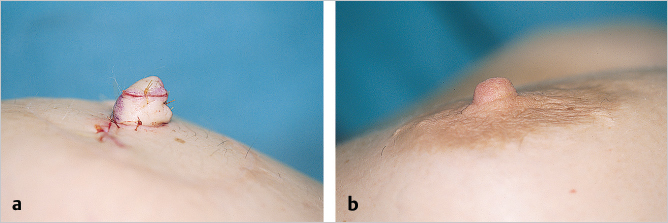
The wound is dressed with Steri-Strips to support the skin closure. A nipple protector is applied; this can be fashioned from the back end of a 10-mL syringe barrel that is cut down to size with a battery-operated electrocautery. The foam caps used to cover the handles of ophthalmic operating microscopes are also useful. The flanges of these fabricated caps are then taped to the breast mound, leaving a firm cylinder to prevent compression of the newly reconstructed nipple by the patient’s bra or clothing. The nipple cap is left in place for 10 days, and tattooing is performed at 4 to 6 weeks postoperatively.
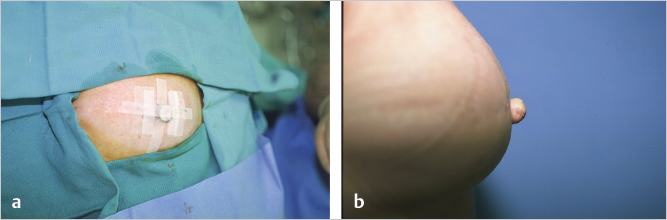
The nipple cap is shown taped in place. On the right, the final projection is shown at 3 months postoperatively (▶Fig. 64.15).
64.4.2 Modified C–V Flap with a Dermal Shelf for Nipple Support
One of the contributory factors to loss of nipple projection, particularly in transverse rectus abdominis musculocutaneous (TRAM) flaps where soft fat forms the base of the nipple, is retrusion of the nipple into the breast mound over time. In an effort to prevent this problem, I developed a technique incorporating a deepithelialized inferior dermal shelf that slides underneath the nipple at the time of donor site closure and provides more solid dermal support for the reconstructed nipple to rest on.
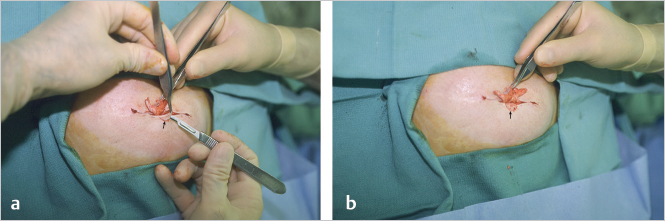
These photos show the creation of the shelf by simply raising the C-flap component of the reconstruction as a thin, partial-thickness flap, leaving the deep dermis behind for support rather than incorporating it as a full-thickness skin flap as shown in the earlier images in the previous C–V flap operative sequence. This modification is simple and adds no time to the procedure (▶Fig. 64.16).
Results
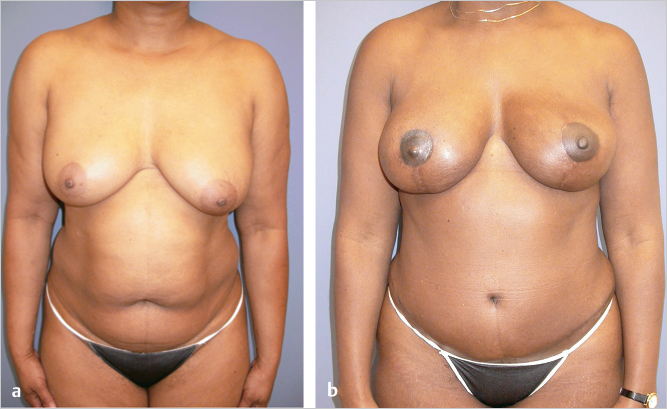
This woman with cancer of the right breast, grade 3 ptosis, and mammary hypertrophy underwent a right mastectomy with immediate TRAM flap reconstruction. She had a vertical reduction of the left breast with right C–V nipple reconstruction and subsequent areolar tattooing. The dermal shelf technique was used. She is shown 1 year postoperatively with a stable result with good projection PI (▶Fig. 64.17).
64.4.3 Fishtail Flap
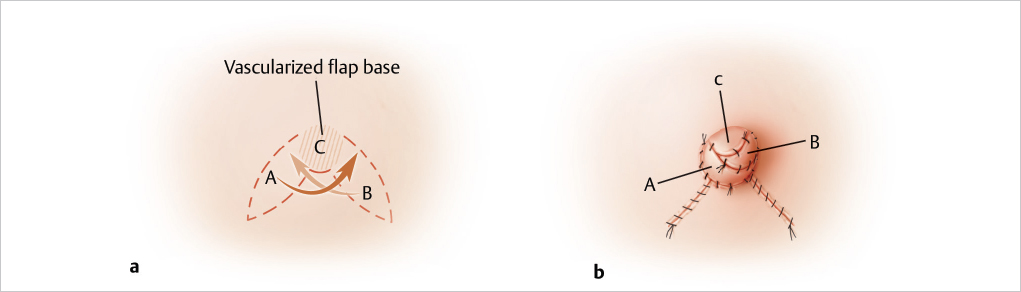
The fishtail flap is a modification of the C–V flap. The flaps are oriented in a more angulated fashion instead of being diametrically opposed to one another, as is the case with the C–V technique. In my practice, its major utility has been in those rare instances in which immediate nipple reconstruction can be performed following massive breast reductions using the lower pole breast amputation technique in patients who do not wish to undergo free nipple grafting. The flap design shown requires postoperative areolar tattooing at 4 to 6 weeks after surgery (▶Fig. 64.18).
Result
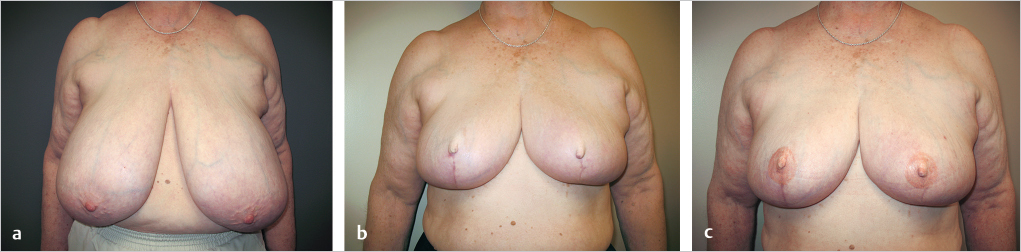
This elderly woman with massive mammary hypertrophy and grade 3 ptosis presented with a left breast cancer. She was a suitable candidate for breast conservation therapy in terms of tumor size, but her enormous breasts were at high risk for radiation-induced complications and difficulty with dosimetry. At the time of lumpectomy, lower pole breast amputation was performed, incorporating the lumpectomy site, and immediate nipple reconstruction was undertaken with fishtail flaps. Her areolae were tattooed before radiation therapy. She is shown 1 year after completion of radiation therapy with slight shrinkage of the irradiated left breast. However, symmetry is acceptable, and her nipples continue to have good projection (▶Fig. 64.19).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree