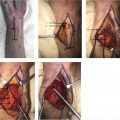
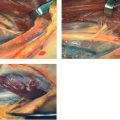
29 Submuscular Ulnar Nerve Transposition
Abstract
Ulnar nerve compression at the elbow typically causes symptoms including numbness in the ring and small fingers, and potentially weakness in the hand with loss of grip strength. While patients with minimal symptoms may be treated nonoperatively, those patients with severe or progressive symptoms usually require surgical intervention. A number of treatment options exist for patients with cubital tunnel syndrome including ulnar nerve decompression with or without nerve transposition. This chapter describes ulnar nerve decompression and submuscular nerve transposition.
29.1 Key Principles
A complete release of the ulnar nerve at all potential sites of compression is critical, including adequate release of the following:
Arcade of struthers
Osborne’s fascia
Medial intermuscular septum
Superficial and deep fascia overlying the two heads of flexor carpi ulnaris (FCU)
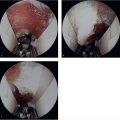
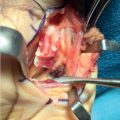
Additional more rare sites of compression including cysts or an anconeus epitrochlearis must be identified and adequately addressed if present. 1 After adequate decompression, if the ulnar nerve is unstable and subluxates over the medial epicondyle, an anterior transposition is performed. Close attention should be paid to ensure that after transposition, the nerve is free to glide smoothly and that the transposition itself does not act as an additional point of compression. Several techniques for placement of the nerve and securing the transposition have been described. The ulnar nerve can be positioned superficial, intramuscular, or submuscular depending upon the clinical scenario and surgeon preference. The remainder of this chapter will review the intramuscular and submuscular transposition options, which are reliable surgical techniques that provide symptomatic relief. 2
29.2 Expectations
Ulnar nerve decompression with submuscular nerve transposition provides a release of the ulnar nerve and a relocation of the nerve to prevent painful and symptomatic subluxation of the nerve over the medial epicondyle. The duration and severity of ulnar nerve compression at the elbow can influence the time course for ulnar nerve recovery. Typically, this procedure is well tolerated and provides decompression and stabilization of the nerve, leading to return of function and symptomatic relief.
29.3 Clinical Findings and Indications
This procedure is indicated in patients with clinically identifiable ulnar nerve compression at the elbow. Most surgeons reserve submuscular transposition for severe compressive neuropathy or for revision cases. Clinical findings of ulnar nerve compression are variable but typically include diminished sensation in the ulnar nerve distribution of the hand including the small and ulnar half of the ring fingers. Compression of the ulnar nerve at the elbow also produces decreased sensation in the distribution of the dorsal cutaneous branch that innervates the dorsal ulnar skin of the hand. Other physical exam signs consistent with ulnar nerve compression at the elbow may include but are not limited to a positive Tinel’s sign at the elbow, a positive flexion-compression test, mechanical snapping of the nerve over the medial epicondyle, Froment’s sign, Wartenberg’s sign as well as intrinsic wasting.
Nonoperative treatment may be attempted including night splinting with the elbow held in relative extension to relieve pressure on the nerve. 3 In cases where the diagnosis is unclear, obtaining electrodiagnostic studies is reasonable to differentiate cubital tunnel syndrome from other pathologies.
29.4 Contraindications and Considerations
It is critical to rule out other conditions that may mimic the symptoms of cubital tunnel syndrome, including:
Cervical radiculopathy
Peripheral neuropathy
Ulnar tunnel syndrome
Carpal tunnel syndrome
Thoracic outlet syndrome
Careful physical examination, electrodiagnostic studies, and appropriate imaging can assist the surgeon in eliminating other potential pathologies. Additionally, if patients present with ulnar nerve compression at the elbow, but no symptomatic nerve instability is noted, an ulnar nerve in situ decompression without nerve transposition may be an appropriate procedure.
29.5 Special Instructions, Positioning, and Anesthesia
This is typically an outpatient procedure and patients can plan for discharge after recovery in the postoperative area.
Supine position.
Hand Table.
An upper arm tourniquet is used with care taken to avoid interference with the operative field. Depending upon the patient’s body habitus, a sterile tourniquet may be preferred if there is any concern.
Regional anesthesia with a brachial plexus nerve block is typically used to avoid the side effects associated with general anesthesia.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree