18 Orbital Disorders
Abstract
“Orbital Disorders” deals with the evaluation of patients presenting with an orbital disorder such as orbital inflammation, tumors, vascular lesions, varices, degenerations, and depositions. Such patients pose a potential diagnostic challenge, and most ophthalmic surgeons encounter them relatively infrequently. Although it is tempting to save time in the evaluation of such a patient by routinely ordering orbital imaging, this should only be done where specifically indicated after a careful clinical evaluation. Likewise, a surgeon who is referred a patient who has already undergone orbital imaging may be tempted to examine the scans before seeing the patient. This is a bad habit that should be avoided, because it can cloud the surgeon’s mind and lead to shortcuts that adversely affect patient management. The scans taken may not have imaged the appropriate area satisfactorily and may not have been the imaging modality most suited to the patient’s orbital disorder. The presentation and management of a number of specific orbital disorders are discussed in this chapter. The disorders that have been selected are those that are more commonly encountered and that can be considered as very important in clinical practice.
18.1 Introduction
This chapter deals with the evaluation of patients presenting with an orbital disorder. Such patients pose a potential diagnostic challenge and are encountered by most ophthalmic surgeons relatively infrequently. Although it is tempting to save time in the evaluation of such a patient by routinely ordering orbital imaging, this should only be done where specifically indicated after a careful clinical evaluation. Likewise, a surgeon who is referred a patient who has already undergone orbital imaging may be tempted to examine the scans before seeing the patient. This is a bad habit that should be avoided, because it can cloud the surgeon’s mind and lead to shortcuts that adversely affect patient management. The scans taken may not have imaged the appropriate area satisfactorily and may not have been the imaging modality most suited to the patient’s orbital disorder.
The presentation and management of a number of specific orbital disorders are discussed in this chapter. The disorders that have been selected are those that are more commonly encountered and that can be considered as very important in clinical practice.
18.2 Evaluation of Orbital Disease
The surgeon should approach a patient presenting with an orbital disorder with the basic clinical patterns of orbital disease in mind:
Thyroid-related orbitopathy.
Neoplastic disorder.
Inflammatory disorder.
Vascular disorder.
Structural disorder.
Degeneration or deposition.
Although the patient’s disorder may occasionally fall into more than one category, this framework allows the surgeon to proceed with the evaluation of the patient in a stepwise and logical manner.
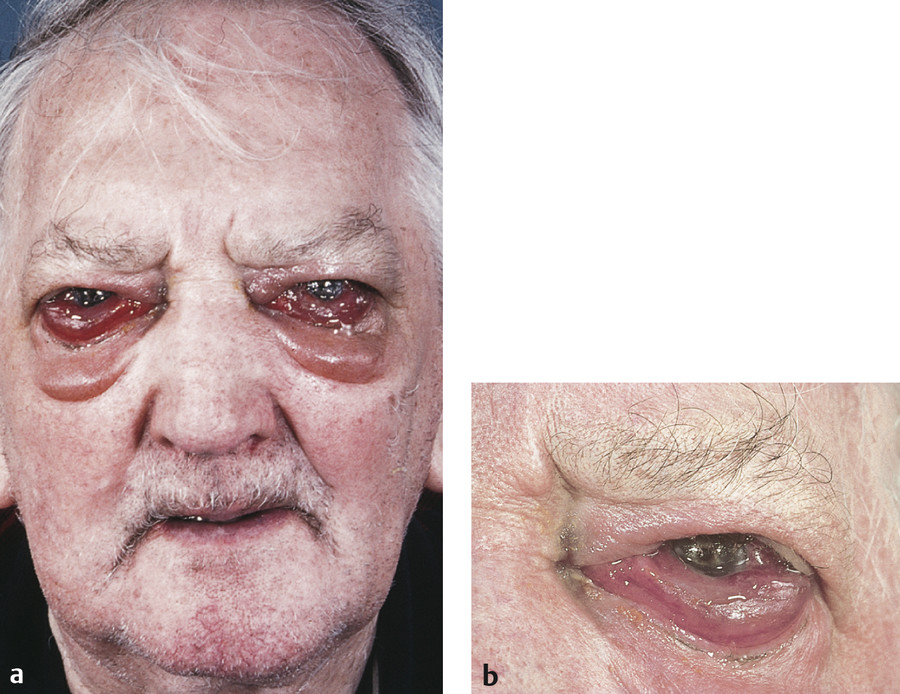
Thyroid-related orbitopathy is the most commonly encountered orbital disorder. It is the most common cause of unilateral or bilateral proptosis in an adult. It should always be considered in the differential diagnosis of a patient presenting with proptosis or orbital inflammatory signs (Fig. 18‑1). Although its classic presentation is easily recognized, it can have a variable and asymmetrical presentation, making it difficult to diagnose in some patients.
Key Point
Thyroid-related orbitopathy is the most common cause of unilateral or bilateral proptosis in an adult.
Tumors may be primary or secondary, benign, or malignant. They may spread to the orbit from the globe, from the eyelids, or from the paranasal sinuses. They may originate elsewhere in the body and metastasize to the orbit (e.g., from the breast). Cavernous hemangioma is the most commonly encountered benign orbital tumor. Lacrimal gland tumors represent a small but significant proportion of orbital disease. Lymphomas and metastatic tumors are the most commonly encountered malignant tumors in adults. In a child, a history of rapidly progressive proptosis demands the urgent exclusion of rhabdomyosarcoma as the cause.
Many orbital disorders have inflammation as their pattern of presentation. Pain is a common accompanying symptom. The inflammatory process may be acute, subacute, or chronic. Acute inflammation is typified by orbital cellulitis. Subacute inflammation may be seen with nonspecific orbital inflammatory syndrome, whereas a chronic inflammatory process is seen with idiopathic sclerosing inflammatory syndrome, or Wegener’s granulomatosis. It is important to bear in mind that some tumors may present with signs of orbital inflammation, which may respond to treatment with steroids. Such masquerade syndromes are important to exclude by means of a biopsy.
Vascular lesions that may be encountered include high- and low-flow arteriovenous fistulas, orbital varices, and lymphangiomas. These lesions may mimic other orbital disorders; for example, a low-flow arteriovenous shunt can mimic the appearance of thyroid eye disease.
Structural disorders may be congenital—including dermoid cysts, sphenoid wing hypoplasia in neurofibromatosis, encephalocele, or microphthalmia with orbital cyst—or acquired— orbital wall blowout fracture or silent sinus syndrome.
Degenerations and depositions are rarer disorders. Examples include amyloidosis, scleroderma, and Parry–Romberg’s syndrome (hemifacial atrophy).
The functional effect of the pathophysiological orbital process on the patient should also be considered. The patient may have a number of functional deficits:
Visual disturbance.
Ocular motility restriction with diplopia.
Pain.
Neurosensory loss.
It is important to be aware that orbital disease occurring in childhood has little overlap with that occurring in adulthood, although the approach to patient evaluation is very similar. Orbital cellulitis is the most commonly encountered orbital disorder of childhood. Malignant tumors, including rhabdomyosarcoma and neuroblastoma, are very rare, but rhabdomyosarcoma must be considered in any child presenting with a rapidly progressive orbital or eyelid mass and proptosis. Choristomas, such as dermoid cysts, and hamartomas, such as capillary hemangiomas, are the most common orbital lesions encountered in childhood. In contrast to adulthood, thyroid eye disease is very rarely encountered in childhood.
Key Point
Rhabdomyosarcoma must be considered in any child presenting with a rapidly progressive proptosis or orbital or eyelid mass.
18.3 History
The history should be recorded in detail. It is important to listen carefully to the patient. Specific questions should be asked:
What is the time course of the disorder? Acute, subacute, or chronic?
Have there been any visual symptoms? Visual disturbance or gaze-evoked amaurosis?
Has there been any pain?
Has the patient experienced diplopia?
Has the patient experienced any periorbital neurosensory loss?
Has there been a history of trauma?
Is the patient aware of any bruits?
Are the symptoms aggravated by any specific maneuver, such as coughing, straining, or nose blowing?
The history may suggest a specific diagnosis. A sudden dramatic proptosis with conjunctival prolapse in a child with a recent upper respiratory tract infection suggests a hemorrhage into a lymphangioma. Gaze-evoked amaurosis may be associated with an orbital apex tumor. Pain associated with a short history of a mass in the region of the lacrimal gland suggests a diagnosis of a malignant lesion, such as an adenoid cystic carcinoma, in contrast to a long history of a gradually progressive painless mass in the region of the lacrimal gland, suggestive of a benign pleomorphic adenoma. Periorbital neurosensory loss in the absence of trauma suggests a malignant lesion. A history of “tinnitus” described by the patient may indicate an arteriovenous shunt. Proptosis provoked by straining may suggest orbital varices. A history of spontaneous unilateral periorbital bruising in an adult may suggest amyloidosis. Spontaneous bilateral bruising in a child may suggest a diagnosis of neuroblastoma. A history of acquired enophthalmos in a female patient with a past history of breast carcinoma suggests a scirrhous orbital metastasis.
A full past ophthalmic, medical, and surgical history should be taken. A multitude of systemic disorders can affect the orbit. Unless prompted, the patient may omit details of a previous thyroid disorder; ear, nose, and throat (ENT) disorder; or treatment for a previous malignancy (e.g., breast carcinoma).
Old photographs may be helpful in evaluating the patient. It is always helpful to suggest that these are brought to any consultation.
18.4 Examination
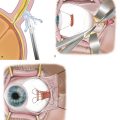
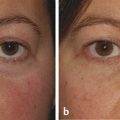
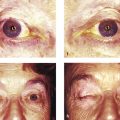
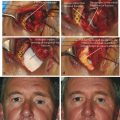
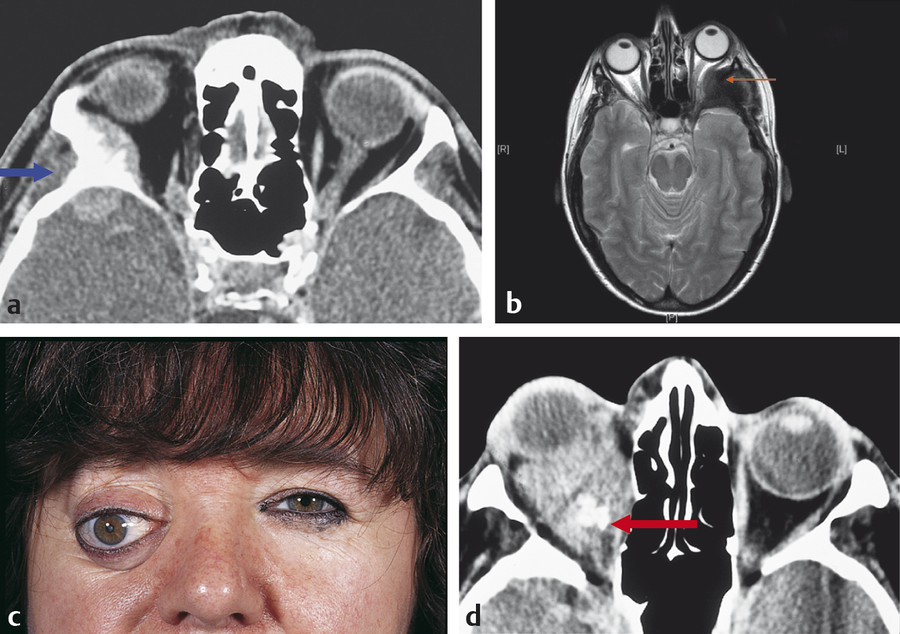
The patient should undergo a full ocular examination, a specific orbital examination, and, where indicated, a full general physical examination. A careful examination of the globe and ocular adnexa may provide important clues to the underlying diagnosis; for example, dilated episcleral vessels may suggest an arteriovenous shunt (Fig. 18‑2a,b); opticociliary shunt vessels may suggest an optic nerve sheath meningioma (Fig. 18‑2c–e); a “salmon patch” lesion beneath the upper eyelid may indicate the presence of an orbital lymphoma (Fig. 18‑2f,g), although such a lesion can also be seen in amyloidosis, sarcoidosis, leukemia, lymphoid hyperplasia, and rhabdomyosarcoma; eversion of the upper eyelid may reveal a waxy yellow infiltrate with tortuous vessels suggesting an amyloid lesion; an S-shaped deformity of upper eyelid may suggest a plexiform neurofibroma (Fig. 18‑2h–j).
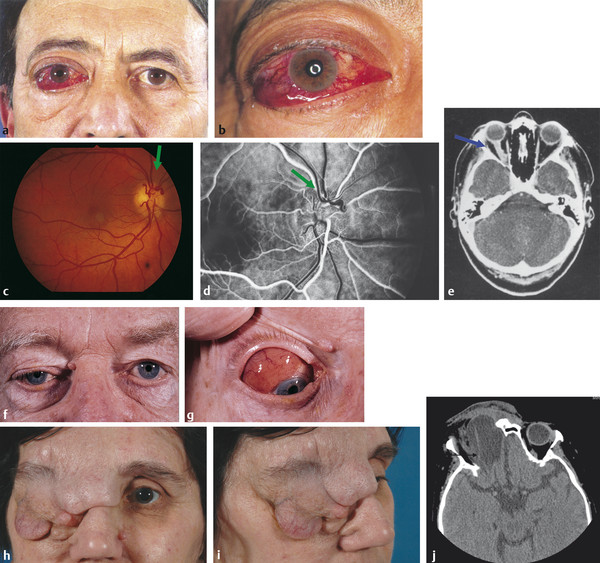
18.4.1 Specific Orbital Examination
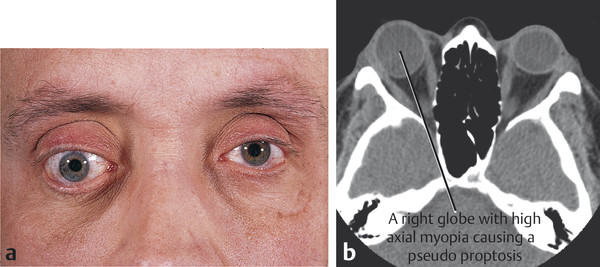
Proptosis or enophthalmos should be assessed and measured using an exophthalmometer. As a general rule, any asymmetry greater than 2 mm is considered pathological. Pseudoproptosis (unilateral and bilateral) from high myopia, contralateral enophthalmos, or facial asymmetry should be excluded (Fig. 18‑3).
It should be noted whether the proptosis is axial or nonaxial. Axial proptosis usually suggests the presence of an intraconal mass or extraocular muscle or fat enlargement in thyroid eye disease.
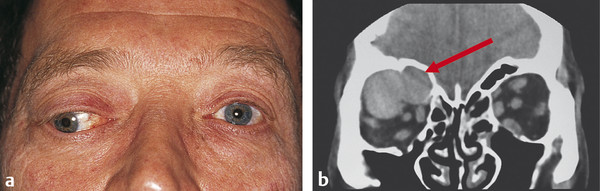
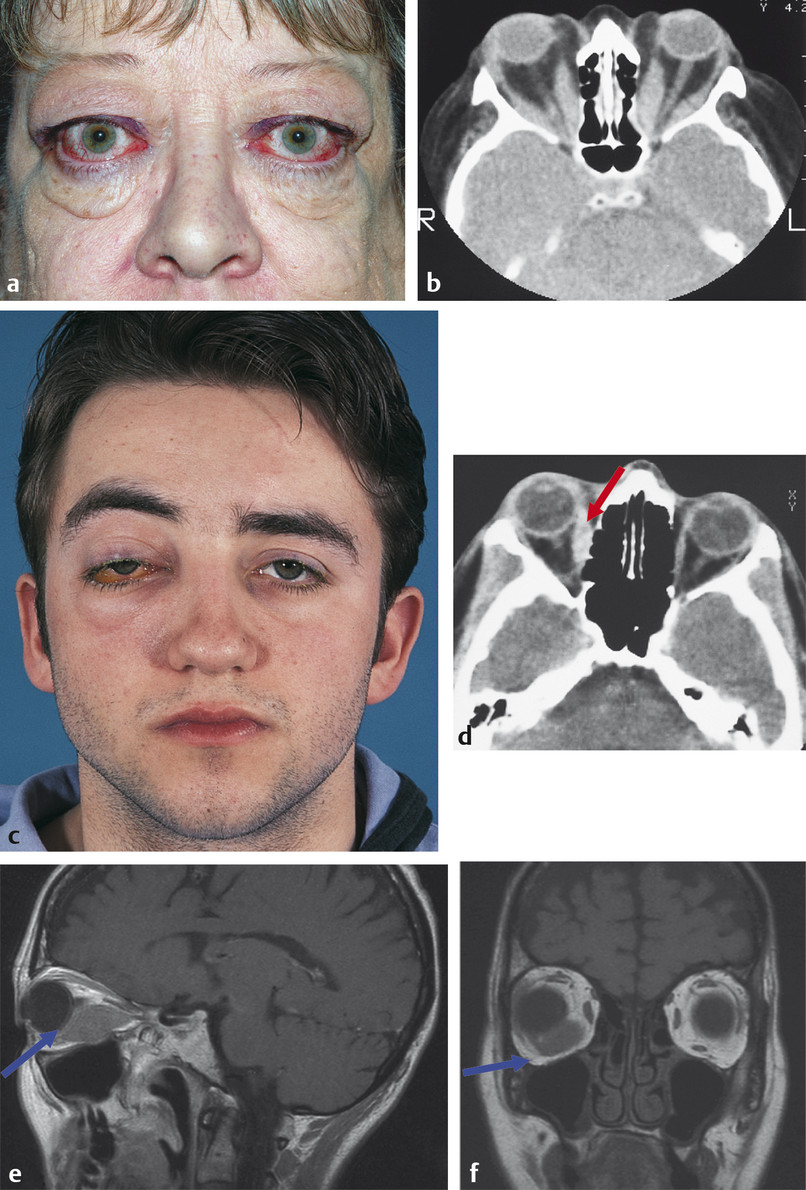
Nonaxial proptosis indicates an extraconal lesion. The globe is pushed in the opposite direction to the orbital mass lesion (e.g., a frontoethmoidal mucocele causes an inferolateral displacement of the globe) (Fig. 18‑4).
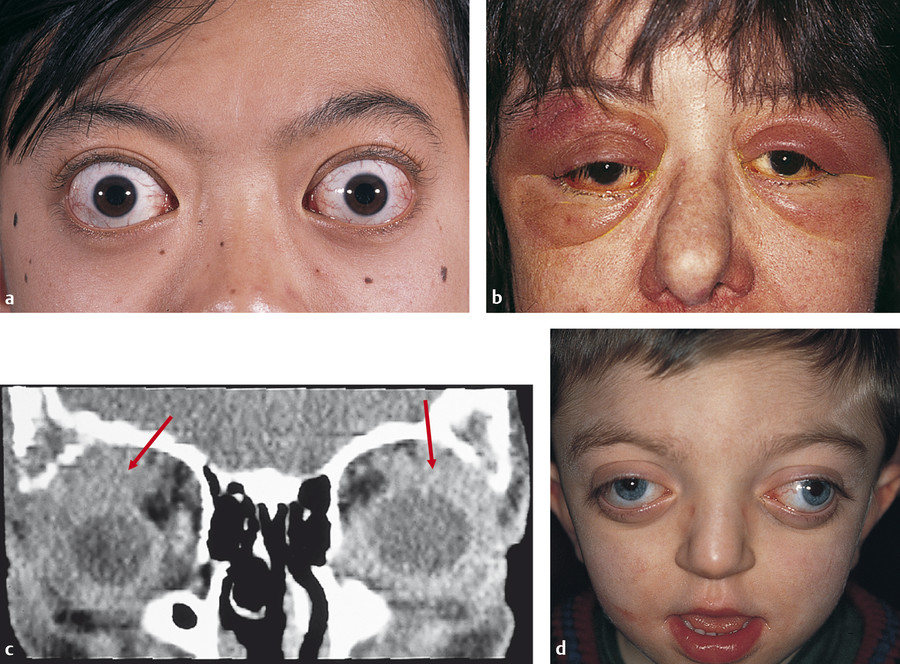
Unilateral proptosis can have a multitude of specific causes, but bilateral proptosis, in general, has a more well-defined differential diagnosis. In general, the most common causes of bilateral proptosis include the following:
Thyroid orbitopathy (Fig. 18‑5a).
Nonspecific orbital inflammatory syndrome.
Lymphomas.
Leukemias.
Myeloma (Fig. 18‑5b,c).
Metastatic lesions.
Congenital craniofacial disorders (Fig. 18‑5d).
Arteriovenous shunts
Enophthalmos may be subtle, presenting as a pseudoptosis or as a cosmetic asymmetry from the development of an upper lid sulcus. The causes are numerous and include the following:
Orbital wall blowout fracture.
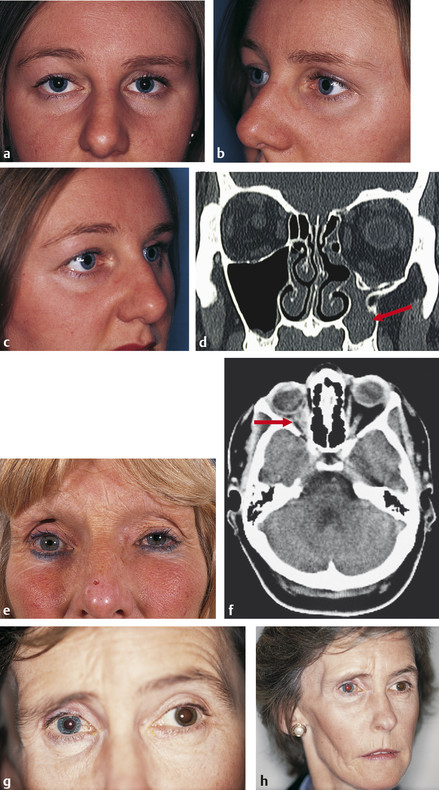
Silent sinus syndrome (Fig. 18‑6a–d).
Metastatic carcinoma (Fig. 18‑6e–f).
Parry–Romberg’s syndrome (Fig. 18‑6g,h; Fig. 17.48b–d).
Linear scleroderma (Fig. 18‑48a).
Lipodystrophy.
Orbital irradiation.
The degree of resistance to retropulsion should be assessed. A solid orbital tumor will cause marked resistance to retropulsion. This assessment of orbital compliance can help to determine the approach to orbital decompression in a patient with thyroid eye disease.
The orbital margins and eyelids should be palpated. An orbital mass may be palpable. Its characteristics should be noted: smooth or irregular, soft or hard, mobile or fixed, tender or nontender. A cystic mass may transilluminate. A clinical diagnosis may be suggested from these findings (e.g., a small, firm, smooth, fixed, nontender lesion in the superotemporal quadrant of the orbit that has gradually increased in size in an infant suggests a dermoid cyst). A smooth inferior orbital mass in an infant with microphthalmia and a coloboma suggests microphthalmia with orbital cyst, a developmental anomaly. A fullness in the adjacent temple may suggest the presence of a sphenoid wing meningioma.
The patient should be observed for spontaneous ocular pulsations. The orbit and cranium should be palpated for thrills and auscultated for bruits.
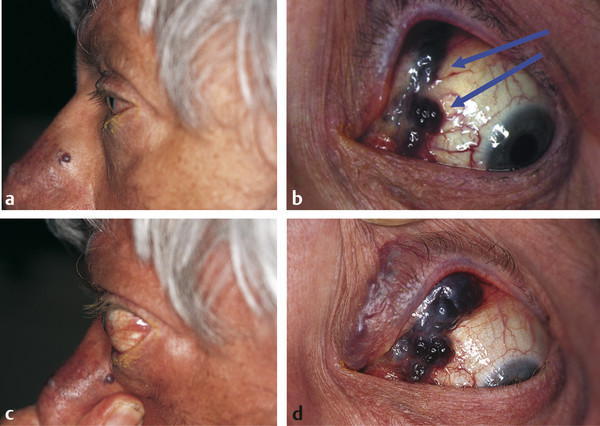
The patient should be asked to perform a Valsalva maneuver. The effect on the globe position or a surface vascular lesion is observed at the same time (Fig. 18‑7).
The intraocular pressure should be recorded in upgaze as well as in the primary position of gaze. A rise in intraocular pressure may be seen in patients with restrictive myopathy, such as with thyroid eye disease.
18.4.2 General Physical Examination
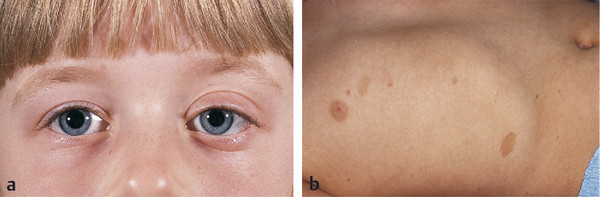
The patient’s skin and oropharynx should be assessed. The presence of cutaneous or intraoral vascular lesions may suggest an orbital lymphangioma. The presence of cafe au lait spots suggests neurofibromatosis (Fig. 18‑8).
The regional and distant lymph nodes should be palpated. The presence of a generalized lymphadenopathy suggests a systemic lymphoproliferative disorder.
Cranial Nerve Examination
A cranial nerve examination should be performed, including an assessment of periorbital and corneal sensation.
Examination of the Chest and Abdomen
An examination of the patient’s chest and abdomen is important whenever there is a possibility of a systemic malignancy, such as undiagnosed breast carcinoma.
18.5 Laboratory Investigations
A number of laboratory investigations may assist in establishing the diagnosis of an orbital disorder, particularly if the disorder is a manifestation of a systemic disease. These include the following:
Chest radiograph: sarcoidosis, bronchial carcinoma, Wegener’s granulomatosis.
Thyroid function tests and thyroid antibodies: Graves’ disease.
Angiotensin-converting enzyme: sarcoidosis.
Antinuclear cytoplasmic antibody (c-ANCA): Wegener’s granulomatosis.
Renal function tests: Wegener’s granulomatosis.
Immunology screen: systemic lupus erythematosus (SLE).
18.6 Orbital Imaging
Orbital imaging has become a cornerstone of orbital diagnosis and surgical planning. As orbital imaging technology continues to improve, the orbital surgeon has been able to refine preoperative differential diagnoses based on the imaging findings. Good communication between the surgeon and the radiologist is essential in obtaining appropriate studies. The better defined the differential diagnosis after a good history and clinical examination, the more appropriate the imaging will be. The selection of the appropriate type of scan, the area to be scanned, and whether to use contrast media are crucial in obtaining the required information. Misinterpretation of images can result when the necessary information required could not be provided by the actual type of scan performed; consequently, it is essential that the surgeon reviews the scans and discusses them with the radiologist to ensure that the appropriate studies have been performed.
The imaging modalities available for the assessment of a patient with an orbital disorder are as follows:
Ultrasonography (USG).
Computed tomography (CT).
Magnetic resonance imaging (MRI).
Magnetic resonance angiography (MRA).
Arteriography.
Positron emission tomography (PET).
18.6.1 Ultrasonography
USG has a number of potential advantages. It is relatively cheap and can be repeated at regular intervals. It provides dynamic information. It has good resolution in the area of the optic nerve and sclera. Color-flow Doppler USG demonstrates vascular flow very well. These advantages can be exploited in the assessment of selected orbital disorders; for instance, it can be used to assist in the differentiation of posterior scleritis from other orbital inflammatory syndromes.
It has a number of disadvantages. It requires a skilled and experienced operator and it may be difficult for the surgeon to interpret the findings. The modality has poor resolution in the posterior orbit. For these reasons orbital USG has been largely replaced by CT and MRI, except in highly selected situations, such as to assist in the assessment of the response of a capillary hemangioma of the orbit to treatment with steroids or propranolol.
18.6.2 Computed Tomography
CT is a medical imaging modality that uses tomography created by computer processing. CT produces a volume of data that can be manipulated, through a process referred to as windowing, demonstrate various bodily structures based on their ability to block an X-ray beam. Modern scanners allow this volume of data to be reformatted in a variety of planes or even as three-dimensional representations of structures.
CT is the single most useful orbital imaging modality. It is relatively inexpensive and is faster and easier to obtain than MRI in most centers. The scans can provide good resolution and soft tissue contrast in addition to superior assessment of bone. It is ideal as an imaging modality to assess orbital trauma and lesions affecting bone. It does, however, expose the patient to ionizing radiation, and this should be borne in mind when ordering repeated CT imaging. Its major limitation is the loss of resolution at the orbital apex where soft tissue is enveloped by bone. MRI is preferred for the evaluation of lesions involving the apex of the orbit.
Pixels in an image obtained by CT scanning are displayed in terms of relative radiodensity. The pixel itself is displayed according to the mean attenuation of the tissues that it corresponds to on a scale from +3071 (most attenuating) to -1024 (least attenuating) on the Hounsfield scale. A pixel is a two-dimensional unit based on the matrix size and the field of view. When the CT slice thickness is also factored in, the unit is known as a voxel (a volumetric pixel), which is a three-dimensional unit. Water has an attenuation of 0 Hounsfield units (HU), whereas air is -1000 HU, cancellous bone is typically +400 HU, and cranial bone can reach 2000 HU or more and can cause artifacts. The attenuation of metallic implants depends on the atomic number of the element used. Titanium usually has an amount of +1000 HU. Iron and steel can completely extinguish the X-ray and are therefore responsible for well-known line artifacts in CT images.
A single film does not have enough range of grayscale to display all the data from a scan. The data can be split and displayed on different films as soft tissue and bone windows. This is now done by computer manipulation of images stored on discs and viewed on computer screens. Bone windows should be reviewed any time a bone lesion is suspected (Fig. 18‑9a–e). Some lesions have very typical imaging characteristics seen with CT, such as the “ground glass” appearance typical of fibrous dysplasia (Fig. 18‑9f).
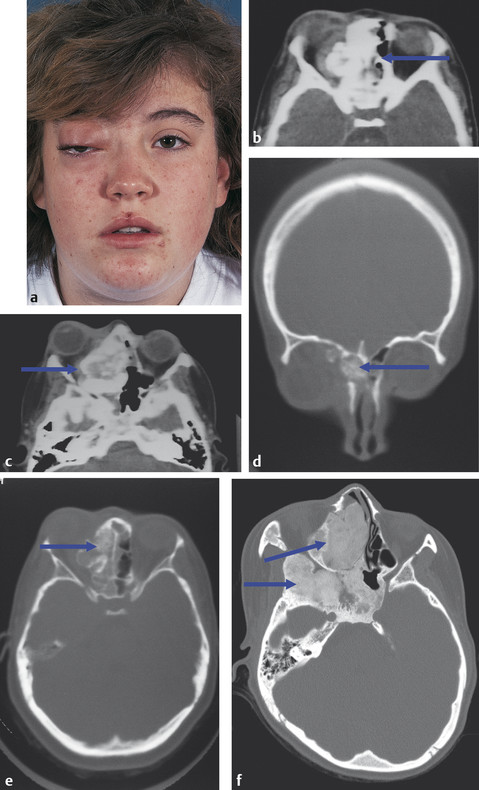
Spiral CT can produce volume data sets in the axial plane. These data sets can then be retrospectively reconstructed into thin sections in any other required plane, which minimizes the radiation dose in the acquisition of multiplanar images. It also overcomes problems of patient positioning in the scanner, because axial images are obtained in the supine position. Reconstruction is of most value in the coronal plane, which allows more detailed assessment of the inferior and superior recti and also the orbital floor. Spiral technology provides rapid image acquisition and therefore reduces problems with movement artifact. This is particularly useful when scanning younger patients.
CT can detect very small intraorbital metallic foreign bodies. Larger nonmetallic foreign bodies such as glass, some plastic materials, and dry wood may also be visible on CT. With multiplanar imaging, CT can also accurately localize foreign bodies.
CT is generally sufficient for the assessment of tumors of the lacrimal gland. In this situation, the important factors to be assessed are the effects of the lesion on the adjacent orbital bone as well as the size, shape, and consistency of the lesion. A benign pleomorphic adenoma tends to be smooth and regular in outline, be homogeneous, and cause indentation with remodeling of the lacrimal fossa. In contrast, a lacrimal gland carcinoma is irregular, with areas of enhancement and nonenhancement with contrast, and may cause irregular bone destruction (Fig. 18‑10).
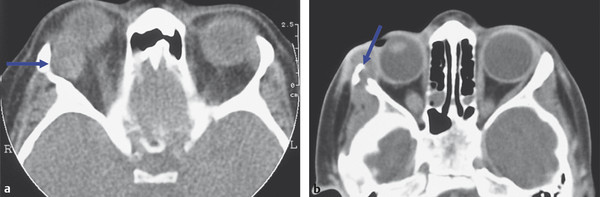
The injection of intravenous (IV) contrast media can provide more information about orbital inflammatory lesions and tumors; for example, the intraorbital and intracranial soft tissue extension of a sphenoid wing meningioma is better seen after the use of contrast. In many cases, however, it is unnecessary, given the wide range of intrinsic tissue contrast provided by various intraorbital structures against the hypodense background of orbital fat. The use of iodinated contrast media may, however, be contraindicated (e.g., with renal dysfunction or a history of allergy to iodine-containing contrast media). An acute anaphylactic reaction can be potentially life-threatening. The newer low-osmolar contrast media have an extremely low complication rate.
Key Point
CT is the single most useful orbital imaging modality for the vast majority of patients presenting with an orbital disorder.
18.6.3 Magnetic Resonance Imaging
Although MRI technology is continuing to improve, it is still more expensive than CT. It is more uncomfortable and claustrophobic for the patient. MRI is adversely affected by patient movement: it does not, however, expose the patient to ionizing radiation and has the advantage of allowing scans to be performed in any plane without the need to reposition the patient. MRI provides excellent soft tissue detail but, because bone is not differentiated from air, it is not a useful imaging modality for the evaluation of orbital fractures or lesions of bone. MRI is the preferred modality for imaging the intracanalicular and intracranial portions of the optic nerve. It is less sensitive for the detection of calcification.
For optic nerve tumors and orbital apex lesions, both CT and MRI may provide complementary information (Fig. 18‑11).
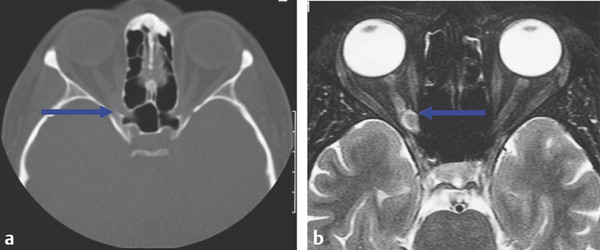
An MRI image is generated based on the movement of protons in tissues when a patient is placed into the magnetic field of a scanner and then subjected to a series of radiowave pulses. The radiowave pulses are varied by the radiologist to generate T1- and T2-weighted scans. A T1-weighted scan is recognizable by the dark appearance of the vitreous in contrast to the very bright appearance of the vitreous on a T2-weighted scan (Fig. 18‑12). T1-weighted scans provide the best anatomical detail. Fluid creates a bright signal on T2-weighted scans. A “fluid void” is seen in areas of high vascular flow where the protons are moving too rapidly to be imaged. Cortical bone appears as a dark area on MRI, because the protons are too tightly bound to generate a signal.
The use of surface coil techniques can improve resolution in the orbit, but these are more sensitive to patient movement. A number of fat suppression techniques can be used to suppress the bright signal from orbital fat on T1-weighted images that can interfere with the signal from adjacent extraocular muscles and the optic nerve. The use of these techniques is essential in postcontrast imaging to prevent enhancing lesions from getting “lost” against the background of orbital fat. The use of IV gadolinium as a contrast medium in combination with fat suppression is particularly useful in the evaluation of optic nerve sheath meningiomas. There are a number of contraindications to the use of MRI:
Iron-containing intraocular foreign bodies.
Cochlear implants.
Intracranial vascular clips.
Cardiac pacemakers.
Older styles of prosthetic cardiac valves.
Claustrophobia.
If an intraorbital foreign body is suspected, a plain radiograph of the orbit should be performed initially to ensure that MRI is safe to perform.
18.6.4 Magnetic Resonance Angiography
There are a number of imaging modalities available for the investigation of orbital vascular lesions. For many years, conventional (i.e., digital subtraction) arteriography has been considered the gold standard because of its ability to provide both spatial and temporal information about orbital vascular lesions. Arteriography can provide detailed information about the arterial blood supply and venous drainage of orbital vascular lesions, the caliber of blood vessels, the collateral circulation, flow velocity, arteriovenous shunting, and the presence of flow-related aneurysms. This imaging modality is, however, invasive and carries a small risk of a cerebrovascular accident and an ophthalmic artery thrombosis or embolization resulting in blindness.
MRI can provide greater soft tissue detail about the structure of orbital vascular lesions than can be provided by CT, but it is more susceptible to motion artifact from ocular movement because of the longer scanning times involved. MRA and venography can provide noninvasive static views of the orbital vasculature and some limited indirect information about blood flow. Although traditional MRA provides excellent spatial resolution, it cannot visualize smaller blood vessels very well and can only provide indirect flow information about larger arterial vessels.
Imaging modalities are constantly improving, and new ones are being developed. A new imaging modality, known as “Time-Resolved Imaging of Contrast KineticS” (TRICKS), uses extremely rapid acquisition of MRI to provide dynamic images of intravascular contrast flow. TRICKS delivers relatively high spatial resolution and also provides dynamic flow information that has not been previously available without more invasive studies, such as interventional angiography. This imaging modality may improve the evaluation of certain orbital vascular lesions.
18.6.5 Arteriography
Arteriography can be regarded as the gold standard to diagnose and characterize certain orbital vascular lesions, such as arteriovenous fistulae. It is not, however, without its risks and potential complications, which must be considered carefully. Interventional radiologists can also treat many of these lesions by the placement of intralesional coils via transarterial or transvenous routes. Occasionally, an orbital surgeon can assist such procedures by the placement of a cannula into the superior or inferior ophthalmic vein (Fig. 18‑43).
18.6.6 Positron Emission Tomography
Positron emission tomography (PET) currently has a limited role in the evaluation of orbital disease, but with advances in the accessibility and usability of PET scanners, PET is now established as a valuable tool for staging, prognostication, radiotherapy planning, and response evaluation in several lymphoma subtypes, particularly Hodgkin’s lymphoma and aggressive non-Hodgkin’s lymphoma.
18.6.7 Review of Images
The surgeon should review the images in a systematic fashion and not merely rely on a radiologist’s report. The basic preliminary data provided on the scan should be examined:
The patient’s name.
The date of the scan.
The technique performed.
Contrast or noncontrast.
Right–left orientation.
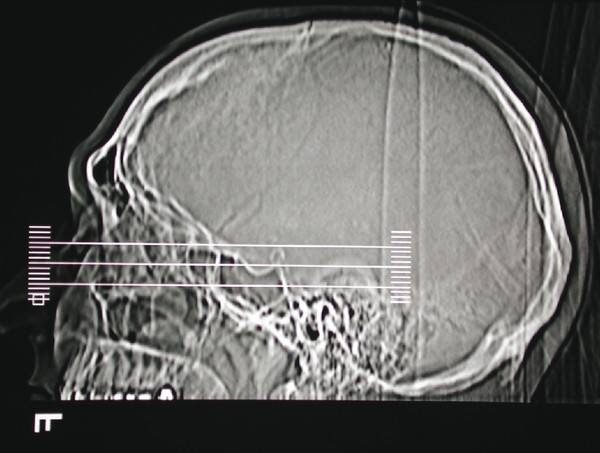
The scout film should be examined. This shows the slices as sectioned by the computer (Fig. 18‑13), which assists in orientation of the plane of scanning performed. The images should be examined systematically, comparing both sides for any asymmetry. It is important to look for any rotation of the head that can lead to misleading asymmetries of no diagnostic significance. The bone structures are examined first, followed by the soft tissues. Interpretation of the images requires practice and experience. It is extremely helpful to review the images with an experienced radiologist, preferably in a multidisciplinary team meeting.
A number of lesions can be categorized according to their imaging characteristics, such as cystic lesions (dermoid cysts, mucoceles, lymphangiomas, parasitic cysts), isolated lesions (cavernous hemangioma, schwannoma), hyperostotic lesions (sphenoid wing meningioma, metastatic prostatic carcinoma), and lesions with calcification (varices, optic nerve sheath meningioma). This can aid in the differential diagnosis (Fig. 18‑14).
Extraocular muscle enlargement, for example, suggests a number of potential differential diagnoses:
Thyroid orbitopathy (Fig. 18‑15a,b).
Myositis (Fig. 18‑15c,d).
Metastases (Fig. 18‑15e,f).
Lymphoma.
Arteriovenous shunts.
Amyloidosis.
Chronic lymphatic leukemia.
18.7 Orbital Biopsy
Direct communication with the pathologist before surgery is extremely useful. Advice should be sought about any special handling of the tissue and the use of special fixatives. A fresh specimen may be required for certain immunohistochemical studies. Previous biopsy material obtained elsewhere may need to be reviewed by the pathologist and may prove to be extremely useful in making a diagnosis.
An orbital biopsy may be incisional or excisional or may be obtained by fine-needle aspiration. An open incisional biopsy is performed with the intention of obtaining a diagnostic tissue sample with as little damage to adjacent structures as possible. It is very important to be aware of situations where this would be inappropriate, such as a pleomorphic adenoma of the lacrimal gland. In this situation, a complete extirpative excisional biopsy should be performed. An incisional biopsy requires careful preoperative planning and experience. It is essential to ensure that a representative sample is obtained that is sufficient for the pathologist to be able to examine. This can be difficult in situations in which normal orbital anatomy is obscured by edema and hemorrhage.
Fine-needle aspiration biopsy is appropriate for some situations but requires the services of a skilled and experienced cytopathologist. The tissue obtained may, however, be misleading: A mistaken diagnosis of nonspecific orbital inflammatory disease may be made from small samples of a lesion as a result of the presence of a parasite. Such misdiagnosis can have grave repercussions for the patient.
The biopsy material obtained must be handled carefully to avoid a crush artifact. Histopathology forms accompanying the specimen must provide the pathologist with all relevant clinical information.
18.8 Selected Orbital Disorders
A comprehensive discussion of all orbital disorders is beyond the scope of this text. A number of disorders have been selected that represent either common or very important orbital problems.
18.8.1 Orbital Inflammation
A significant proportion of orbital disorders present with a picture of acute or subacute inflammation. Inflammatory processes affecting the orbit can be attributed to a number of causes, both systemic and localized. A subclassification of orbital inflammatory processes can be based upon the temporal course (acute or chronic), the morphology (local or diffuse), or the anatomical location within the orbit. Discrete and classifiable disease processes can be identified in most cases, but a small proportion have no identifiable cause after an orbital biopsy and have been labeled as idiopathic orbital inflammation (IOI). This umbrella term embracing conditions that do not fit neatly into established diagnoses is gradually changing. Improvements and advances in investigational techniques have narrowed the once broad and expansive term idiopathic. IOI remains a diagnosis of exclusion but may be an orbital tissue response to some other process not yet elucidated by currently available testing techniques.
The following disorders are most commonly encountered:
Acute thyroid orbitopathy.
Orbital cellulitis.
Nonspecific orbital inflammatory disease.
Specific orbital inflammatory disease.
Acute Thyroid Orbitopathy
Thyroid-related orbitopathy is the most common orbital inflammatory disease, accounting for approximately 50% of cases seen. This disorder, in view of its unique character, is addressed separately in Chapter 20.
Orbital Cellulitis
Orbital cellulitis is an inflammation of the orbital or periorbital tissues. Microbial orbital cellulitis is a true ophthalmic emergency, requiring hospital admission and the immediate administration of antibiotics. Although the morbidity and mortality associated with orbital cellulitis have dramatically improved since the advent of antibiotics, serious complications may still occur, including blindness, meningitis, cavernous sinus thrombosis, brain abscess, and death. The ophthalmic surgeon must play an active role in helping to establish the diagnosis and must be responsible for monitoring visual function. Where this has to be delegated to nonophthalmic nursing staff, such as on an ENT ward, it is the ophthalmologist’s responsibility to ensure that the nurses know how to monitor visual function and whom to communicate with in the event of deterioration of visual function.
Key Point
Orbital cellulitis should be treated as an ophthalmic emergency.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree