16 Free Tissue Transfer
16.1 Free Venous Flap
Venous flap blood supply is from afferent and efferent veins. These flaps have been described for use of small digital defects with flaps being taken from the volar forearm. These flaps are thin, easy to locate, and can be dissected quickly. Furthermore, the donor site morbidity is low.
Free venous flaps can be used when the defect is too large for homodigital or heterodigital flaps. They can also be applied as flow through flaps in cases of revascularization with soft-tissue loss and also as a salvage procedure after unsuccessful local flap coverage.
Venous flaps can either be configured with V-V-V or arterialized A-V-V or flow through A-V-A (Chen’s venous flap classification). Higher flow rates such as in arterialized venous flaps have more chance of success.
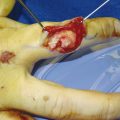
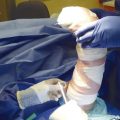
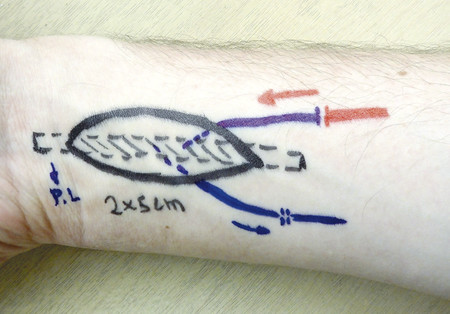
In the case illustrated, the palmaris longus (PL) was identified and marked. A 2 × 5 cm skin flap was designed along with two superficial veins, which were visible entering the skin flap. A tourniquet was applied without exsanguination of the limb in order that the veins be dilated and the flap harvest easier. The skin flap was raised on a suprafascial plane, and the marked veins were dissected in adequate length. At the level of the PL, the dissection was proceeded deeper so that the PL remained attached to the skin flap (Fig. 16‑1, Fig. 16‑2, Fig. 16‑3).
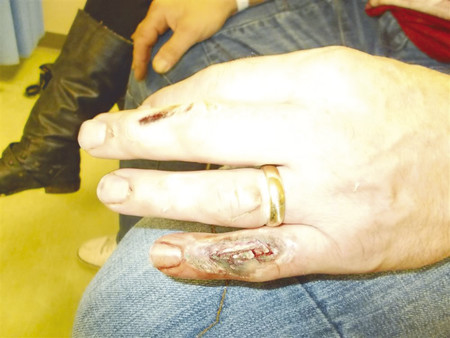
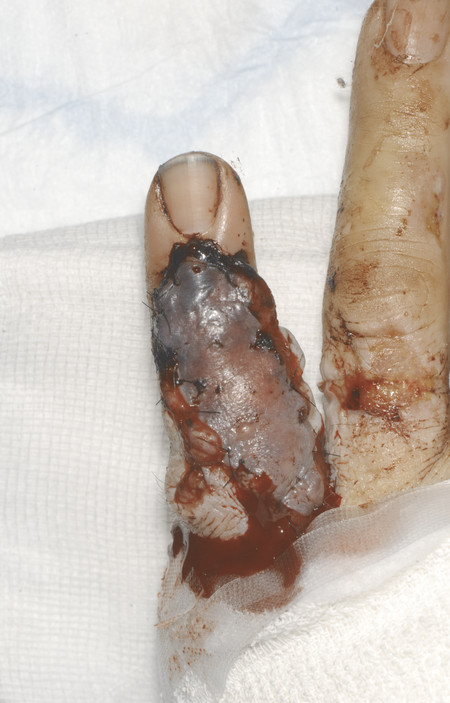
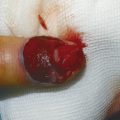
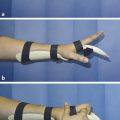
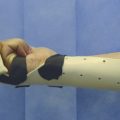
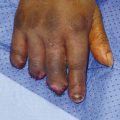
On the recipient site, debridement on the dorsum of the left little finger revealed a tissue defect of 4 × 1.5 cm along with 2.5-cm gap of the central slip of the extensor tendon. The radial digital artery and a dorsal superficial vein over the head of the fifth metacarpal were prepared for anastomosis. 11.0 nylon was used for microsurgical anastomosis. The patient had an excellent outcome (Fig. 16‑4, Fig. 16‑5, Fig. 16‑6).
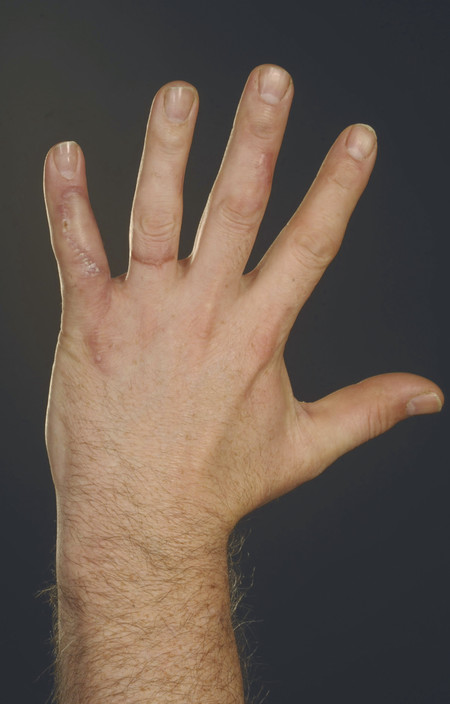
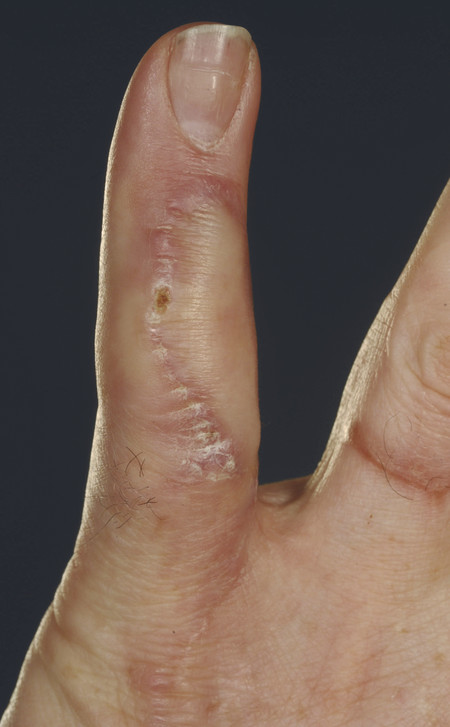

16.2 Free Anterolateral Thigh Flap
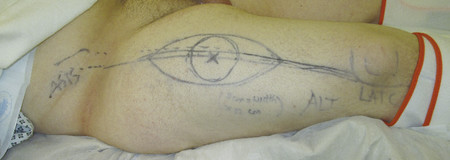
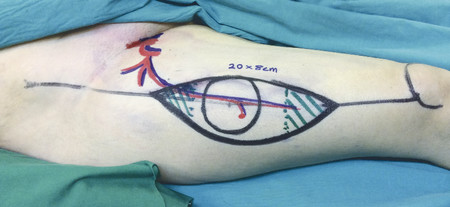
The anterolateral thigh (ALT) flap is a workhorse flap in lower limb and upper limb defects. Drawing a line from the anterior superior iliac spine to the superolateral corner of the patella marks the flap axis. The perforators are within a 3-cm radius circle on the midpoint of this line. A handheld Doppler can be used to mark out the perforators.
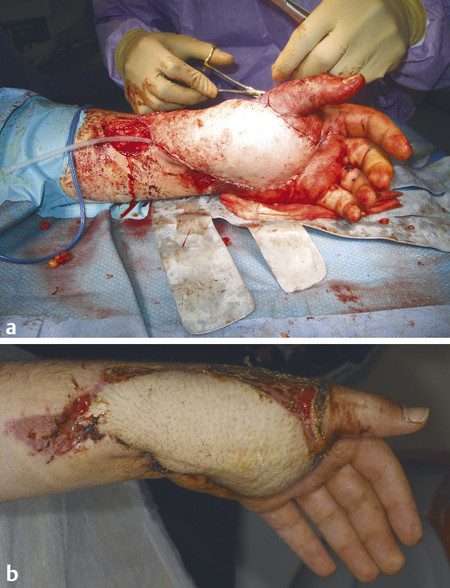
This flap can be harvested as cutaneous, fasciocutaneous, musculocutaneous, and even flow through flap. In the case shown, a fasciocutaneous free ALT flap was harvested for reconstruction of a significant crush defect to the hand.
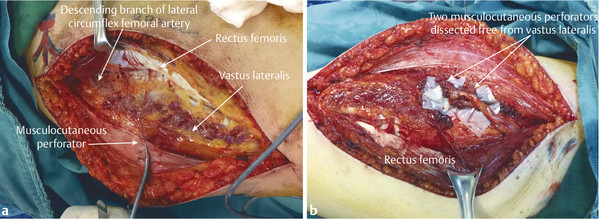
Flap elevation is started medially; a suprafascial flap can be elevated for a thin flap. In this case, the flap was elevated with underlying fascia. Flap elevation is stopped when perforators are encountered. In 20% of cases, the perforators are identified as septocutaneous and run between the vastus lateralis (VL) and rectus femoris (RF). However, in the remaining 80% of cases musculocutaneous perforators are found traversing the vastus lateralis. A yellow fatty septum between both VL and RF muscles is easily identified distally. It is much easier to identify this septum distally. The RF muscle is displaced medially away from the vastus using a retractor in order to identify the descending branch of the lateral circumflex femoral artery (LCFA) along with its associated perforators. Once adequate perforators are identified, they are traced back to the main pedicle. If the perforators traverse through the vastus, careful dissection with bipolar cautery can be performed. An alternative approach is “deroofing” the vastus lateralis muscle that lies over the perforators. The tenotomy scissors are slid over the musculocutaneous perforator protecting it while performing cutting monopolar over the vastus muscle. This technique allows for more rapid dissection of the perforators.
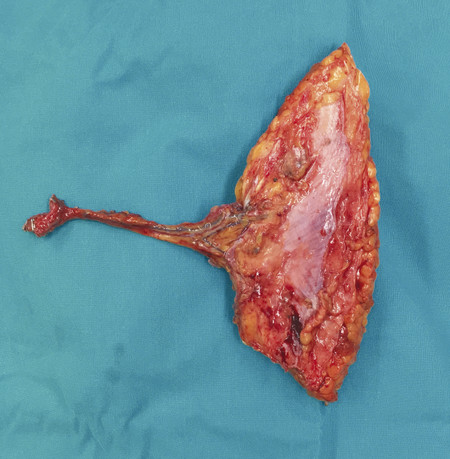
Side branches can be ligaclipped if large and if small heat sink, bipolar technique can be used. This involves holding the side branch with DeBakey’s forceps and on the side away from the pedicle performing bipolar cautery to seal the vessel. The DeBakey’s forceps act as a heat sinking interposition and protect the pedicle from thermal effects of the bipolar. The skin paddle is then finally incised laterally and the flap pedicle is divided from near its origin at the profunda femoris.
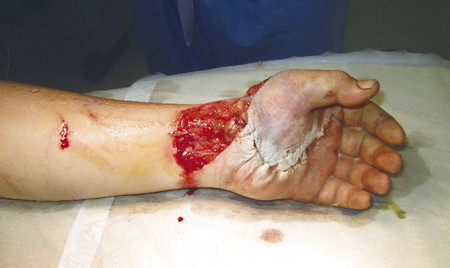
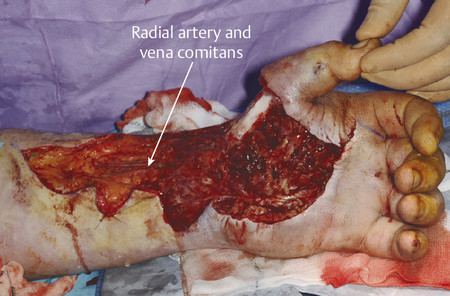
After debridement, the recipient site radial artery and vena comitans were prepared for microsurgical anastomosis. It is useful to mark the recipient and donor vessels with blue ink. This helps with alignment before anastomoses and prevents twisting and possible disruption of blood flow. End-to-end anastomosis of the radial artery to the LCFA was performed with 9.0 Ethilon; the LCFV was anastomosed to the vena comitans with a 3.0 venous coupler (Fig. 16‑7, Fig. 16‑8, Fig. 16‑9, Fig. 16‑10, Fig. 16‑11, Fig. 16‑12, Fig. 16‑13, Fig. 16‑14).

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree