Differential Diagnosis.
The differential diagnosis of dermatitis of the genital area includes all of the conditions that can result in an erythematous, scaly eruption. This includes psoriasis, tinea, perianal streptococcal dermatitis and pinworm infestation. Treated lichen sclerosus may appear erythematous rather than white [6].
Where examination reveals little more than a scaly, erythematous, poorly defined rash, dermatitis is the most likely diagnosis, even if signs are subtle. When the rash is erythematous but well defined, and particularly when there is perianal involvement, it is important to look for signs of psoriasis and enquire about a family history [7].
Investigations.
If weeping or pustules are present, a bacteriological swab from the affected area should be performed. If there appears to be a vaginal discharge, a swab from the introitus with a moistened cotton tip can be performed, but prepubertal children tolerate vaginal swabs poorly, and they are in general not indicated. If there is suspicion of a fungal infection, a fungal scraping should be performed. Urine culture is not required unless dysuria is present. Patch testing is rarely required.
Prognosis.
The prognosis of genital dermatitis is excellent, particularly when simple irritancy from an identifiable source is present, which can be easily reversed. Even when there is an underlying tendency to atopic dermatitis, the condition can easily be controlled. Remissions and exacerbations are the rule, depending on irritant exposure, but most parents rapidly learn to deal with these situations.
Management.
Many cases of genital itching are due to dermatitis, either atopic or the result of irritation from clothing or applied substances. Often, a much greater emotional overlay is attached to any condition of the genital area than to conditions in other parts of the skin. As a result, the degree of distress experienced by the parents and sometimes the child may be out of proportion to the actual problem. There is still a tendency for vulval disease to be poorly understood, and it is not uncommon for patients to visit many doctors without receiving what they consider a satisfactory explanation and effective treatment. As a result, parents are often angry and frustrated. This can make history taking difficult and leave the doctor wondering why the emotional reaction is so intense when there is so little to see.
The first step in treating genital dermatitis involves giving parents detailed environmental advice specific to the genital area. It is preferable to bathe rather than shower. No soap or bubble bath should be used; bath oil should be used in the bath and, if the child does shower, a soap substitute should be used and the parent needs to explain that the labia have to be parted and rinsed, and in boys over the age of 3 years, the foreskin retracted. This should be supervised. Shampoo should be rinsed out after the child gets out of the bath, or soap substitute used instead of shampoo.
If the child does any form of physical activity that involves wearing tight Lycra clothing, if possible this should be modified so that, at least during practice sessions, loose cotton clothes are worn. This, of course, is not possible for performances and competitions, but explain to the parents that some compromises have to be made. Even nylon tights worn as part of a school uniform may have to be discarded and parents may require a letter to take to the school.
If the child is going to swimming lessons, the chlorinated water can be a powerful irritant. Applying Vaseline® (petroleum jelly) or zinc cream before swimming is helpful, and the parents should be advised to always remove the costume straight after swimming and that the child should shower before going home.
If the child has an incontinence problem, either enuresis or constipation with overflow, this needs to be dealt with. Night nappies should be discarded if possible. Always actively ask about this; it is embarrassing, is not always volunteered, and parents do not always make a connection between incontinence and the genital irritation.
Enquiry should be made concerning over-the-counter topical applications as these may not be volunteered, the parent seeing them only as unsuccessful treatment and not a potential problem. Ask about perfumed products, such as toilet paper and wet wipes, as well. The use of such products should be stopped.
In terms of ideal clothing, loose cotton underwear is desirable, and underpants, particularly nylon ones, should be avoided at night.
Most cases of vulval dermatitis will respond to 1% hydrocortisone topically, as long as the environmental changes are also made. Ointment is preferable to creams, which may cause stinging. If the dermatitis is severe, a stronger, non-fluorinated topical steroid such as methylprednisolone aceponate 0.1% or desonide 0.05% can be used initially and be continued until the dermatitis has settled. It should be possible to reduce to 1% hydrocortisone when the rash has settled. If this is not possible, consider an alternative diagnosis.
The child should be treated for possible pinworm infestation.
Many parents are very apprehensive about using topical steroids on their children, and even more so on the vulva where they are concerned that the preparations will ‘thin the skin’. In practice, the above treatment is very safe and it is wise to pre-empt any objections with strong reassurance.
If skin swabs show infection, which will usually be with Staph. aureus, a course of appropriate antibiotics should be given. A finding of β-haemolytic streptococcus group A requires a 10-day course of appropriate antibiotics.
Much stronger reassurance is often required when skin disease affects the genital area than when it is found on other skin areas, and it is important to enquire about fears of sexually transmitted disease and child abuse.
It is best to be matter of fact and help the parents to understand that the genital area is simply part of the skin and their child’s pattern is to have involvement in this area. Make them aware that children rapidly pick up their anxieties, and that an intelligent child may capitalize on this with attention-seeking or school-avoiding behaviour.
Psoriasis of the Genital Area
Incidence.
The incidence and natural history of psoriasis in childhood are unknown. However, presentation of psoriasis in children and adults differs in type and pattern [8]. Also, few data exist on psoriasis of the genital area. It is an accepted fact that psoriasis may be confined to this part of the skin, with little evidence of the disease elsewhere.
If children with genital disease are taken as a group, psoriasis is a relatively common cause, representing about 10% of children presenting with vulval disease, and it should always be considered in the differential diagnosis of persistent genital rashes in both sexes [1,2,9]. A study in 2001 [8] indicated that the genital area was involved in 8.9% of children with childhood psoriasis. In children of less than 2 years of age, the most common type of psoriasis is nappy rash with dissemination [8].
Clinical Presentation.
In babies, psoriasis may present for the first time as a persistent nappy rash. The features at this age include a well-demarcated edge and involvement of the inguinal folds, but the typical scale of psoriasis is lacking under the nappy. The rash may remain confined to the nappy area or may disseminate with typical psoriatic lesions on the trunk, limbs and scalp [1,2,4,10].
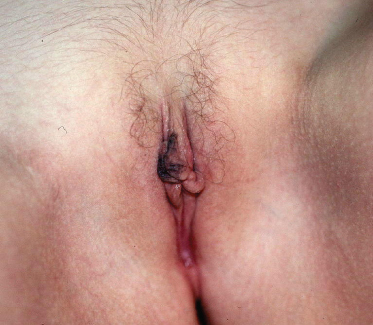
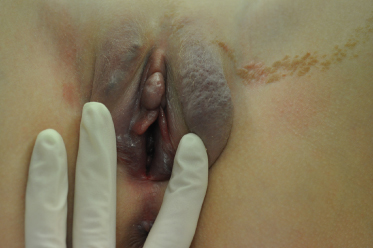
In older children, the morphology of the rash is much the same, with an itchy, red, well-demarcated, symmetrical plaque. Again, there is no scale. The vulva, penis, perineum, perianal area and often natal cleft may all be involved (Fig. 151.2). The rash may not be markedly symptomatic but parents may complain that the area is persistently erythematous [7,11].
If psoriasis is confined to the genital area, it is difficult to make a definite diagnosis unless other diagnostic clues are present. A history of cradle cap or difficult nappy rashes as a baby, nail pitting, postauricular or scalp rashes and a family history are all helpful [12].
Investigations.
If weeping or inflammation is present, a skin swab for bacteriology is indicated. Like psoriasis on other areas of the skin, infection of the genital area with group A streptococcus will worsen the disease and create treatment resistance. Other investigations are not necessary.
Prognosis.
Data are lacking on the outcome of childhood psoriasis. It is not known whether psoriatic nappy rash is a precursor to childhood or adult psoriasis, and the natural history of genital psoriasis in children is also not known [8].
Differential Diagnosis.
This includes dermatitis, erythematous lichen sclerosus and streptococcal perianal dermatitis.
Management.
Psoriasis tends to be more difficult to treat than dermatitis. Even psoriatic nappy rash may not respond to 1% hydrocortisone. Although some cases do respond to the weaker corticosteroids that are usually recommended for the genital area, it is not uncommon for stronger corticosteroids to be required to achieve relief of itching [13]. Topical pimecrolimas may be effective [14] but stinging is a significant side-effect in the genital area and initial control with topical corticosteroid is often required before other therapies can be initiated.
Low-concentration tar-containing preparations, such as 2% liquor carbonis detergens in an emollient base, are useful on the genital area, particularly for maintenance treatment. For thickened plaques, it is possible to use low-concentration dithranol with good effect. General skin care measures specific for the genital area (as outlined in Dermatitis, above) are also an adjunct to therapy.
References
1 Fischer GO. Vulval disease in pre-pubertal girls. Australas J Dermatol 2001;42:225–34.
2 Fischer GO, Rogers M. Vulvar disease in children. A clinical audit of 130 cases. Pediatr Dermatol 2000;17:1–6.
3 Paek SC, Merritt DF, Mallory SB. Pruritus vulvae in prepubertal children. J Am Acad Dermatol 2001;44:795–802.
4 Fischer G, Rogers M. Paediatric vulvovaginitis. In: Proceedings of the 3rd Symposium on Diseases of the Vulva and Vagina. Melbourne: Melbourne University, 1997: 26–9.
5 Warshaw EM, Furda LM, Maibach HI. Anogenital dermatitis in patients referred for patch testing:retrospective analysis of cross-sectional data from the North American Contact Dermatitis Group. Arch Dermatol 2008;144(6):749–55.
6 Ridley CM. Genital lichen sclerosus (lichen sclerosus et atrophicus) in childhood and adolescence. J Roy Soc Med 1993;86:69–75.
7 Siegfried EC, Frasier LD. Anogenital skin disease in the pediatric population. Pediatr Ann 1997;26:321–31.
8 Morris A, Rogers M, Fischer G et al. Childhood psoriasis. A clinical review of 1262 cases. Pediatr Dermatol 2001;18:188–98.
9 Fischer G. Chronic vulvitis in pre-pubertal girls. Australas J Dermatol 2010;51:118–23.
10 Fischer GO. The commonest causes of symptomatic vulval disease: a dermatologist’s perspective. Australas J Dermatol 1996;36:166–7.
11 Farber EM, Nall L. Genital psoriasis. Cutis 1992;50:263–6.
12 Ridley CM. Vulvar disease in the paediatric population. Semin Dermatol 1996;15:29–35.
13 Paek SC, Merritt DF, Mallory SB. Pruritus vulvae in prepubertal children. J Am Acad Dermatol 2001;44:795–802.
14 Amichai B. Psoriasis sof the glans penis in a child successfully treated with Elidel (pimecrolimus) cream. J Eur Acad Dermatol Venereol 2004;18(6):742–3.
Birthmarks in the Genital Area
Special Considerations in the Genital Area
Birthmarks may occur on the genital area as on any other part of the skin, but the importance of lesions in this location is that they may be mistaken for more sinister conditions. For example, pigmented naevi often raise queries of melanoma, where they might be ignored elsewhere, and epidermal naevi may be mistaken for warts or recalcitrant eczema. Any ulcerating lesion may cause queries of sexual abuse [1]. Haemangiomas and vascular malformations [2–11] are dealt with elsewhere in detail (see Chapters 112 and 113).
Melanocytic Naevi
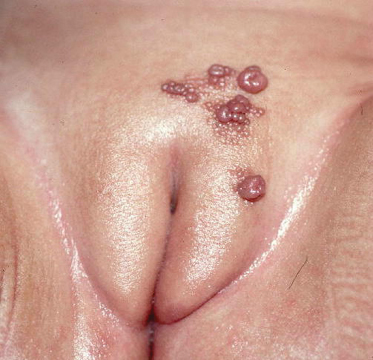
Pigmented naevi may occur on the genital and perianal area; they may be congenital lesions or appear at any stage of childhood (Fig. 151.3). The congenital lesions tend to be larger than late-onset ones. Pigmented naevi of the genital region rarely present a problem but they do frequently raise fears of melanoma [4].
Despite this, melanoma in children is rare, and there have been very few reports of childhood genital melanoma [12]. There is no documented evidence that pigmented naevi of the genital area have a particular malignant potential [13]. Pigmented naevi with the histopathology of ‘atypical naevi’ occur on the genital skin but a recent study confirms that they have a benign clinical course and cautions against overdiagnosis of melanoma [14].
Bannayan–Riley–Ruvalcaba Syndrome (Ruvalcaba–Myhre–Smith Syndrome) OMIM 153480
The PTEN hamartoma-tumour syndromes include at least two clinically different but overlapping cancer predisposition syndromes: Cowden syndrome and Bannayan–Riley–Ruvalcaba syndrome, both with autosomal dominant inheritance resulting from germline mutations in the PTEN tumour suppressor gene on chromosome 10q23.3 [15,16].
Bannayan–Riley–Ruvalcaba syndrome was first described in 1980 by Ruvalcaba et al. [17], as a classic triad of polyposis coli, pigmented macules of the penis and macrocephaly. The polyps, which may not appear until adult life, may occur throughout the gastrointestinal tract and have been reported on the tongue. They present with painless rectal bleeding and, sometimes, intussusception.
Other features described with the syndrome include developmental delay, hypotonia, myopathy, ocular abnormalities, café-au-lait macules, lipomas, haemangiomas and vascular malformations, facial verrucous or acanthosis nigricans-like lesions and multiple skin tags of the neck, axilla and groin [18]. Musculoskeletal changes and neuropathy have been reported [19].
The pigmented macules appear during childhood or adolescence and then persist and present as a speckled lentiginosis of the penis or vulva [20]. The syndrome can be differentiated from Peutz–Jeghers syndrome by the presence in the latter of pigmented macules of the lips and buccal mucosa.
Epidermal Naevi
Epidermal naevi are uncommon and about 50% are not present at birth although most develop within the first year of life, seldom appearing after the age of 7. They may continue to extend for up to 5 years after they first appear [21]. They usually have a warty surface and are usually arranged in whorls or streaks. Both verrucous and inflammatory epidermal naevi may involve the genital area. They may be localized or part of a larger lesion that extends to the leg and buttock.
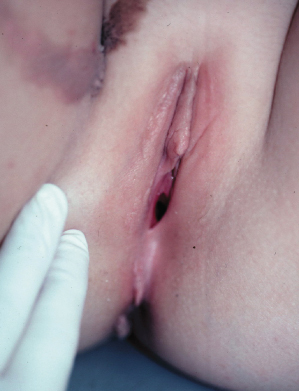
Verrucous epidermal naevi have a warty, hyperkeratotic surface (Fig. 151.4). They are usually pigmented, but when they extend onto the macerated skin of the perineum or labia minora, they may have a white appearance. They may be papillomatous in some areas (Fig. 151.5).
Inflammatory epidermal naevi (ILVEN) are linear and have a scaly, erythematous surface. They are quite itchy and are therefore commonly mistaken for recalcitrant eczema. ILVEN have been rarely described involving the inguinogenital region [21,22].
Because epidermal naevi have a tendency to extend with time, they may be confused with an inflammatory dermatosis. If they become large, they can interfere with function, particularly in the perianal area. Epidermal naevi can be mistaken for warts, in turn giving rise to queries of child abuse. If they are itchy they can be mistaken for treatment-resistant lichenified eczema or napkin dermatitis [4,38]. Naevus comedonicus has been reported on the vulva [23].
Management.
Itchy genital epidermal naevi may be very resistant to topical therapy [22] and it is not uncommon for epidermal naevi of the genital region to cause enough trouble to require at least partial excision. For example, a warty perianal lesion is best removed, and sometimes recalcitrant itching is relieved only by surgically excising the lesion. However, if they are not causing problems, it is best just to reassure the patient and leave the lesions alone. There is no significant malignant potential.
Vascular Naevi
Haemangioma of the genital area is common in both sexes and is discussed elsewhere.
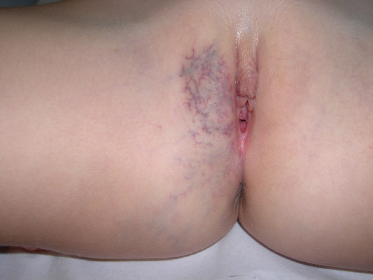
Many genital vascular lesions have been described in children including venous, lymphatic and mixed veno-lymphatic lesions (Figs 151.6–151.8). Lymphangioma of the scrotum has been described [24,25]. Both these cases presented with a scrotal mass and were associated with other genital anomalies. Lymphangioma has also been described as a penile lesion [26] and a single case of verrucous haemangioma of the glans penis has been described [27].
In a large series of female patients with vascular anomalies, 2.6% were found to have lesions of the external genitalia. These presented with cutaneous macular stains, swelling, deformity, bleeding, fluid leakage and infection [28]. Vascular lesions may increase in size at puberty [29].
Patients with Klippel–Trenaunay syndrome, characterized by vascular malformation of capillary, venous and lymphatic systems associated with soft tissue and bone hypertrophy, frequently have genitourinary involvement, including cutaneous and anatomical genital abnormalities, the overall incidence being reported to be 30%. Bleeding from genital lesions, as well as haematuria, may occur in these patients and approximately half of them eventually require surgical intervention for genitourinary complications [30,31].
Management.
Genital vascular lesions usually require magnetic resonance imaging, ultrasound, angiography and gynaecological exploration for full diagnostic clarification. They can present a very difficult therapeutic challenge and are frequently devastating for the patient and her family. Excision of these lesions may be very difficult. Treatment with direct injection venography using ethanol sclerotherapy has been described as a successful treatment for vulval venous malformation [32].
Papular Acantholytic Dyskeratosis of the Vulva
Papular acantholytic dyskeratosis of the vulva is a rare condition that presents with a papular eruption of the vulva [33]. The lesions are scattered, skin-coloured to white slightly keratotic papules associated with multiple grouped superficial erosions. The lesions are found on the labia majora.
Clinical Features.
The condition presents in childhood with white papules and erosions found bilaterally on the labia majora. There may be associated pruritus but it has also been described as asymptomatic [34]. Both the pruritus and clinical appearance may regress with time [35].
Most previous case reports have been in adults but the condition has recently been described in a child [35]. The condition does not appear to be familial.
Histology.
Histopathology is distinctive with hyperkeratosis, acantholysis, dyskeratotic cells resembling corps ronds and irregular proliferation of basaloid cells. Immunofluorescence is negative [35,36].
Differential Diagnosis.
This condition, although rare, is important as it may be confused with multiple flat genital warts or with papular lichen sclerosus. Histologically, it needs to be differentiated from Hailey–Hailey disease, Darier disease and warty dyskeratoma. Epidermal naevi, including those found on the vulva, may show acantholysis but are usually unilateral [37].
Management.
This condition runs a chronic course. Treatment described so far has been disappointing. No specific treatment has been described in children and reassurance that this is a benign condition may be all that is required.
References
1 Hosteller BR, Jones CE, Miram D. Capillary hemangioma of the vulva mistaken for sexual abuse. Adolesc Pediatr Gynaecol 1994;7:44–6.
2 Bouchard S, Yazbeck S, Lallier M. Perineal hemangioma, anorectal malformation, and genital anomaly: a new association? J Plastic Surg 1999;34:1133–5.
3 Goldberg NS, Hebert AA, Esterly NB. Sacral hemangiomas and multiple congenital abnormalities. Arch Dermatol 1986;122:684–7.
4 Fischer GO. Vulval disease in pre-pubertal girls. Australas J Dermatol 2001;42:225–34.
5 Morelli JG, Tan OT, Yohn J et al. Treatment of ulcerated haemangiomas in infancy. Arch Pediatr Adolesc Med 1994;148:1104–5.
6 Alter GJ, Trengove-Jones G, Horton C. Haemangioma of the penis and scrotum. Urology 1993;42:205–8.
7 Young AE, Senapati A. Intra-abdominal and pelvic vascular malformations. In: Mulliken JB, Young AE (eds) Vascular Birthmarks. Philadelphia: W.B. Saunders, 1988: 396.
8 Rodrigues D, Bourroul ML, Ferrer AP et al. Blue rubber bleb naevus syndrome. Rev Hosp Clin Fac Med Univ Sao Paulo 2000;55:29–34.
9 Khoudary KP, Nasrallah PF, Gordon DA. Glomus tumor of the penis. J Urol 1996;155:707.
10 Ramos LM, Payon EM, Barrilero AE. Venous malformation of the glans penis: efficacy of treatment with neodymium:yttrium-aluminum-garnet laser. Urology 1999;53:779–83.
11 Norouzi BB, Shanberg AM. Laser treatment of large cavernous haemangiomas of the penis. J Urol 1998;160:60–2.
12 Egan CA, Bradley RR, Logsdon V et al. Vulvar melanoma in childhood. Arch Dermatol 1997;133:345–8.
13 Christensen WN, Friedman KJ, Woodruff JD et al. Histologic characteristics of vulvar nevocellular nevi. J Cutan Pathol 1987;14:87–91.
14 Gleason BC, Hirsch MS, Nucci MR et al. Atypical genital naevi. A clinicopathologic analysis of 56 cases. Am J Surg Pathol 2008;32(1):51–7.
15 Lachlan KL, Lucassen A, Bunyan D, Temple IK. Cowden syndrome and Bannayan Riley Ruvalcaba syndrome represent one condition with variable expression and age-related penetrance: results of a clinical study of PTEN mutation carriers. J Med Genet 2007;44(9):579–85.
16 Boccone L, Dessi V, Zappu A et al. Bannayan–Riley–Ruvalcab syndrome with reactive nodular lymphoid hyperplasia and autism and a PTEN mutation. Am J Med Genet 2006;140(18):1965–9.
17 Ruvalcaba RHA, Myhre S, Smith DW. Sotos syndrome with intestinal polyposis and pigmentary changes of the genitalia. Clin Genet 1980;8:413–16.
18 Bishop PR, Nowicki MJ, Parker PH. What syndrome is this? Pediatr Dermatol 2000;17:319–21.
19 Erkek E, Hizel S, Sanly C et al. Clinical and histopathological findings in Bannayan–Riley–Ruvalcaba syndrome. J Am Acad Dermatol 2005;53(4):639–43.
20 Blum RR, Rahimizadeh A, Kardon L et al. Genital lentigines in a 6-year-old boy with Cowden’s disease. Clinical and genetic evidence of the genetic linkage between Bannayan–Riley–Ruvalcaba syndrome and Cowden’s disease. J Cutan Med Surg 2001;5:228–30.
21 Rogers M, McCrossin I, Commens C. Epidermal Naevi and the epidermal naevus syndrome: a review of 131 cases. J Am Acad Dermatol 1989;20:476–88.
22 Le K Wong L, Fischer G. Vulval and perianal inflammatory linear verrucous epidermal naevus. Australas J Dermatol 2009;50:115–17.
23 Gonzalez-Martinez R, Marin-Bertolin S, Martinez-Escribano J et al. Nevus comedonicus. Report of a case with genital involvement. Cutis 1996;58:418–19.
24 Joshi AV, Gupta R, Parelkar S, Gupta A, Jadhav V. An unusual congenital scrotal lymphatic malformation with absent corpora cavernosa: a case report. J Pediatr Surg 2008;43(9):1729–31.
25 Vikicevic J, Milobratovic D, Vukadinovic V, Golubovic Z, Krstic Z. Lymphangioma scroti. Pediatr Dermatol 2007;24(6):654–6.
26 Shah A, Meacock L, More B, Chandran H. Lymphangioma of the penis: a rare anomaly. Pediatr Surg Int 2005;21(4):329–30.
27 Akyol I, Jayanthi V, Luquette M. Verrucous hemangioma of the glans penis. Urology 2008;72(1):230.
28 Vogel AM, Alesbury J, Burrows PE, Fishman SJ. Vascular anomalies of the female external genitalia. J Pediatr Surg 2006;41(5):993–9.
29 Kemoinarie A, de Raeve L, Roseeuw D, Boon L, de Raeve H. Capillary–venous maformation in the labia majora in a 12-year-old girl. Dermatology 1997;194(4):405–7.
30 Husmann DA, Rathburn S, Driscoll DJ. Klippel–Trenaunay syndrome: incidence and treatment of genitourinary sequelae. J Urol 2007;177(4):1244–9.
31 Vicentini FC, Denes F, Gomes CM, Danilovic A, Silv FA, Srougi M. Urogenital involvement in the Klippel–Trenaunay Weber syndrome. Treatment options and results. Int Braz J Urol 2006;32(6):697–703.
32 Herman AR, Morello F, Strickland JL. Vulvar venous malformations in an 11-year-old girl: a case report. J Pediatr Adolesc Gynecol 2004;17(3):179–81.
33 Chorzelsky TP, Kudejko J, Jablonska S. Is papular acantholytic dyskeratosis of the vulva a new entity? Am J Dermatopathol 1984;6:557–9.
34 Bell HK, Farrar C, Curley RK. Papular acantholytic dyskeratosis of the vulva. Clin Exp Dermatol 2001;26:386–8.
35 Saenz AM, Cirocco A, Avendano M, Gonzalez F, Sardi JR. Papular Acantholytic dyskeratosis of the vulva. Pediatr Dermatol 2005;22(3):237–239.
36 Cooper P. Acantholytic dermatosis localized to the vulvocrural area. J Cutan Pathol 1989;16:81–4.
37 Cottoni F, Masala M, Cossu S. Acantholytic dyskeratotic epidermal naevus localized unilaterally in the cutaneous and genital areas. Br J Dermatol 1998;138:875–8.
38 Le K, Wong L-C, Fischer G. Vulval and perianal inflammatory linear verrucous epidermal naevus. Australas J Dermatol 2009;50:115–7.
Non-Sexually Acquired Genital Infections in Children
Streptococcal Cellulitis, Vulvovaginitis and Balanitis
Pathogenesis.
Group A β-haemolytic streptococcus is the most common cause of acute vulvovaginitis and balanitis in prepubertal children [1]. Interestingly, adults are rarely prone to this, although very occasionally a group B streptococcus may cause a true vaginitis in an adult and perianal dermatitis and balanitis caused by group A β-haemolytic streptococcus has been described in adults [2].
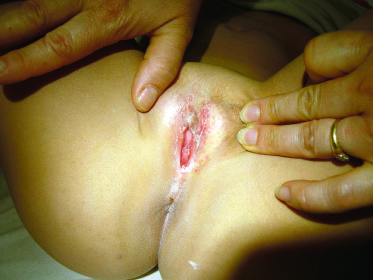
Perianal streptococcal dermatitis (also known as cellulitis) is a common cause of chronic and acute-on-chronic perianal rashes in children, more commonly in boys. Presentation is with persistent perianal erythema, swelling, scale and fissuring. It is not a true cellulitis. Symptoms include itch and pain. The rash is a non-infiltrated plaque that may extend several centimetres from the anal verge. Weeping from the surface may produce a persistent discharge, and pain on defaecation may result in chronic constipation which may in turn result in bleeding on defaecation [3].
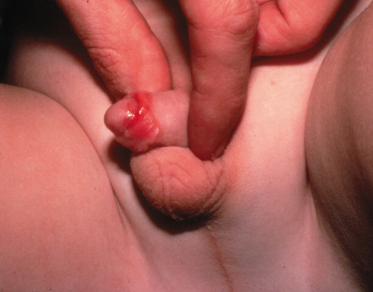
In girls with vulvovaginitis, presentation is with sudden onset of an erythematous, swollen, painful vulva and vagina, with a thin mucoid discharge. In boys with balanitis, there is acute erythema of the glans (Fig. 151.9). There may have been a preceding throat infection with the same organism or preceding perianal dermatitis. Sometimes the infection can be low grade, similar to the perianal disease, presenting as a subacute vulvitis [4].
Recurrent disease has been reported as a result of chronic pharyngeal carriage [5]. This infection does not tend to self-resolve and symptoms tend to be persistent until a diagnosis is made and appropriate treatment initiated [6].
In general, patients with this condition are systemically well; however, fever and scarlatiniform rash, followed by acral desquamation in association with perianal disease, have been reported. In this case, a streptococcal pyrogenic exotoxin was assumed to be produced by the infective organism [7]. Guttate psoriasis may be precipitated by this infection [8].
The infection is easily diagnosed by introital and perianal swabs. It is not necessary to insert the swab right into the vagina, which children usually find traumatic, particularly when the area is tender.
Differential Diagnosis.
Although a differential diagnosis of acute candidiasis would be reasonable in an adult, this is not the case in children. Psoriasis and dermatitis are also in the differential diagnosis, particularly when the vulvitis is subacute. Recurrent streptococcal infections should raise the possibility of an intravaginal foreign body [1].
Shigella species may also cause recurrent and chronic vulvovaginitis in association with diarrhoea.
There is often a blood-stained vaginal discharge that may suggest a foreign body [9]. Yersinia vaginitis in conjunction with gastroenteritis has been reported [10].
Also in the differential diagnosis, but much rarer as a cause of acute vulvitis, is the fixed drug eruption. Erythema multiforme may also affect the vulva but is usually part of a generalized reaction in children.
Management.
Any case of acute vulvitis or balanitis and any persistent perianal rash in a child should suggest this condition; swabs should be taken and the child commenced on either oral penicillin or amoxicillin, or cephalothin if they are allergic to penicillin. The course must run for a full 10 days or recurrence may occur. Concurrent use of topical mupirocin will help to prevent recurrence. Apparent poor response to therapy, with ongoing symptoms despite resolution of infection, usually indicates an underlying condition such as dermatitis, psoriasis or vaginal foreign body [1,4]. A case report has recently drawn attention to recurrent disease as a result of chronic asymptomatic pharyngeal colonization which cleared with rifampicin and amoxicillin [5].
Recurrent Toxin-Mediated Perineal Erythema (Scarlatina-Like)
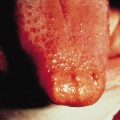
This condition, which was originally described in young men, presents with recurrent, asymptomatic erythema and desquamation of the perineum and groin area following acute pharyngitis. The eruption may be associated with swelling, erythema and desquamation of the hands and feet, or a ‘strawberry tongue’. Toxin-producing Staph. aureus or toxin-producing group A β-haemolytic streptococcus is responsible for the eruption [11].
This phenomenon is assumed to be a superantigen-related disorder [12].
A recent series reports 11 cases of this condition in children, seven boys and four girls presenting with acute onset of perineal erythema. In this series, four patients also had erythema of the hands and feet and seven had a strawberry tongue. Only three of these cases had recurrent disease. In all cases there was evidence of group A β-haemolytic streptococcus infection although this was not recovered from perineal culture and all were treated with oral antibiotics. All of the children were well and laboratory investigations normal [13].
In young children, this condition must be differentiated from Kawasaki syndrome.
Staphylococcal Folliculitis and Impetigo
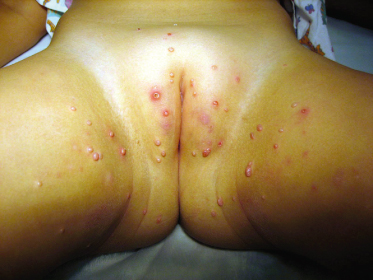
Staphylococcal folliculitis is common on the buttocks of children, particularly those with eczema and those who are still in night nappies. It may sometimes spread to the vulva or groin or can be found there primarily (Fig. 151.10). Impetigo may also sometimes occur on the genital and perianal area.
The presentation is with pustules and crusted lesions, which are often more itchy and irritating rather than painful. The diagnosis is made with a bacterial swab.
Management.
Although impetigo usually responds quickly to a course of appropriate anti-staphylococcal antibiotics, folliculitis often represents a carrier state and can be very persistent. It is often better treated with topical agents, such as bath products containing chlorhexidine or triclosan and mupirocin 2% cream. Underwear and other garments in direct contact with genital skin, such as swimming costumes and pyjamas, sheets and towels, should be hot-washed, and every attempt made to discard night nappies. If there is underlying eczema, this should be treated.
Staphylococcal Scalded Skin Syndrome
This is an exfoliative skin condition preceded by an often minor staphylococcal infection that produces an exfoliative toxin. The child presents with fever, irritability and usually a widespread erythematous eruption, with flexural accentuation. As the illness progresses, shallow blisters evolve to raw, eroded areas, particularly in the perioral, axillary and genital areas. The eruption may begin in the genital area with a tender, erythematous eruption with superficial blistering.
Pinworm (Enterobius Vermicularis)
Although many children with pinworm infestation are asymptomatic, symptoms are those of perianal and vulval itching, particularly at night, when the worms migrate onto the skin to lay eggs. An eczematous rash may occur, but the skin may be normal. Vaginal discharge and irritation may also occur. Pinworm is very well known as a cause of genital itching in children, and many children will already have been treated by their parents or their pharmacist before they see a doctor [14].
Diagnosis may be made by pressing the sticky side of clear tape to the perianal area first thing in the morning and then examining the tape under a microscope for the presence of ova.
Treatment requires oral mebendazole 100 mg or pyrantel pamoate 11 mg/kg up to 1 g. A further treatment in 2 weeks is recommended to kill worms that have hatched since the first treatment [15].
Scabies
Scabetic nodules are common on the genital area, but are usually part of a generalized eruption. The irritable nodules occur on the vulva in girls and on the glans and scrotum in boys (Fig. 151.11).
Molluscum Contagiosum
Molluscum contagiosum is a large double-stranded DNA poxvirus. DNA analysis has demonstrated four major viral types [16]. The virus codes for a number of proteins that enable it to evade the immune system by blocking immune recognition and clearance [17].
These viral lesions are very common in children. The virus is spread by close physical contact, fomites and autoinoculation. Transmission in water is well recognized, and this explains the predilection for the lower body where the child sits in the bath [18]. As a result, it is not uncommon for mollusca to be found on the genital area, often as part of a more generalized eruption [14] (Fig. 151.12).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree