14 Fracture Fixation Techniques
14.1 Jahss Maneuver
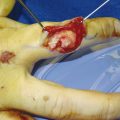
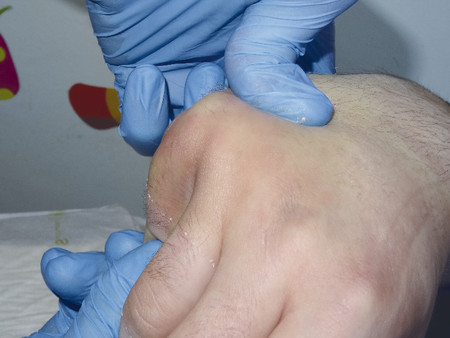
This is a useful technique to help manipulate the neck of fifth metacarpal fractures. It is also useful intraoperatively when fixing fifth metacarpal fractures. The fracture is reduced by flexing the metacarpophalangeal joint (MCPJ) and proximal interphalangeal joint (PIPJ) of the little finger to 90 degrees and using the proximal phalanx to push up the head of the fifth metacarpal thereby reducing it (Fig. 14‑1, Fig. 14‑2, Fig. 14‑3).
14.2 Salter-Harris 2 Fractures of the Proximal Phalanx
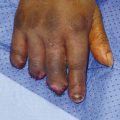
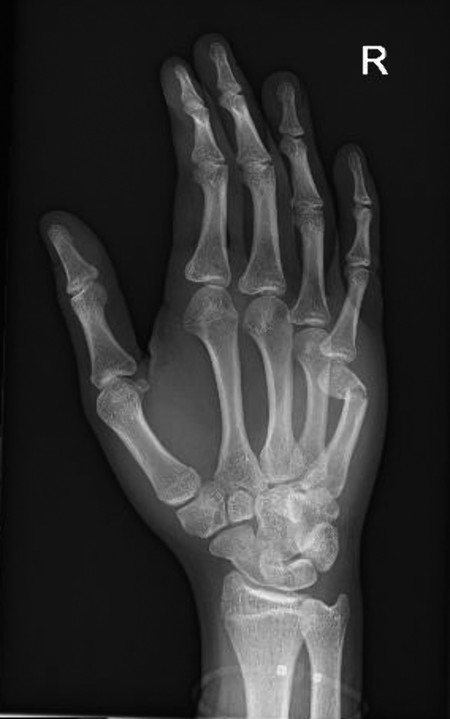
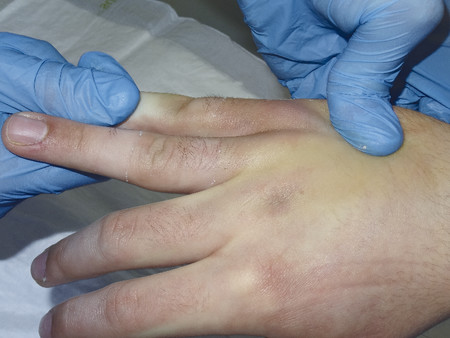
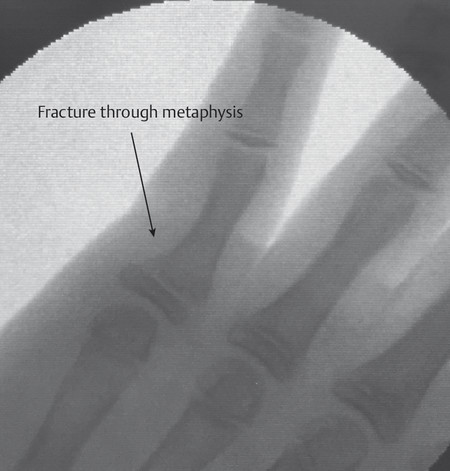
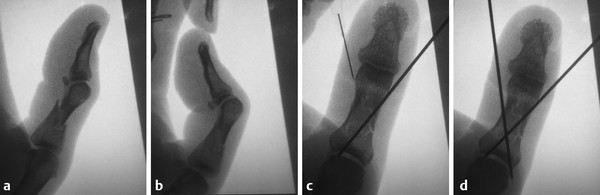
The most common type of Salter-Harris fracture involves fracture through the metaphysis of the proximal phalanx and it has an incidence of 80% (Fig. 14‑4). These injuries are very common in the emergency department and can easily be reduced using a pen as a fulcrum (Fig. 14‑5).
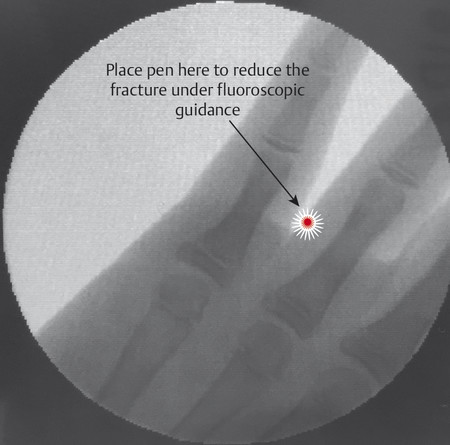
In older children, this manipulation can be done under local anesthetic and checked with fluoroscopic scan; otherwise, general anesthesia is needed. After reduction, the adjacent finger is buddy strapped to the injured finger and the hand is rested in a volar splint before active mobilization at 1 week.
14.3 Conservative Management of Fractures
Hand surgeons, young and old, like to fix fractures. However, it is important to be selective and to identify cases where nonoperative management may be preferable (Fig. 14‑6). Many hand fractures can be treated conservatively as long as the fracture is stable, minimally displaced with no rotation or scissoring.
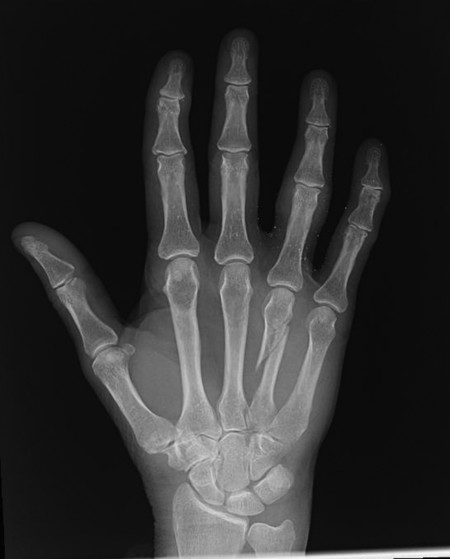
Placing metal work can interfere with tendon glide and these patients may need further surgery to remove the plate with the need for extensor tenolysis. The aim of all fracture fixations is a solid fixation so that early hand therapy can commence. It is no longer acceptable to keep patients in a plaster of Paris for 3 to 4 weeks postoperation.
14.3.1 Rehabilitation after Conservative Management
Patients are placed in a volar resting splint after assessment or fracture reduction. Early referral to the hand therapy team for education, protection of the fracture as necessary, and early edema control is important. If there are any concerns regarding stability, a repeat radiograph at 1 week will confirm if the reduction of the fracture has been maintained. Early motion is essential for all stable fractures to prevent stiffness.
14.4 Kirschner Wire Fixation
Percutaneous K-wire fixation should be considered in many closed hand fracture configurations, where a satisfactory closed reduction has been achieved, but is unlikely to be maintained with splints or casts alone (Fig. 14‑7). However, K-wiring is not always easy to perform and sometimes multiple passes are made in error. To minimize problems, a number of simple steps can be performed.
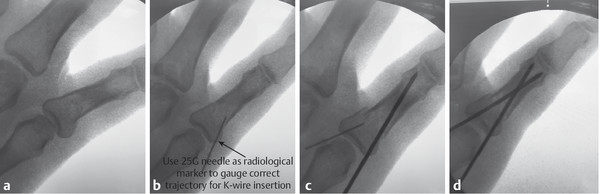
One must mark the joints with a pen to help with the 3D understanding of the fracture. Radiologic markers such as a 25-gauge orange needle can help guide the trajectory of the K-wire (Fig. 14‑8, Fig. 14‑9). However, when passing the K-wire one should go by feeling the resistance of the cortical bone. Furthermore, making small stab incisions through the skin with a 15 blade is useful rather than stabbing the K-wire through the skin inadvertently catching the extensor mechanism. If repeated attempts are made during surgery, a new K-wire should be loaded on the driver. Repeated attempts and high revolutions should be avoided as thermal damage to bone can result in problems with union and infection.
14.4.1 Rehabilitation after Kirschner Wire Fixation
The fracture is protected postsurgery in a volar plaster of Paris cast, which is replaced with a smaller splint after referral to hand therapy. Gentle active range-of-motion exercises are generally started after 1 week. The K-wire is removed at 3 to 4 weeks when fracture tenderness has reduced.
14.5 Fracture Dislocations of the Base of the Fourth and Fifth Metacarpals
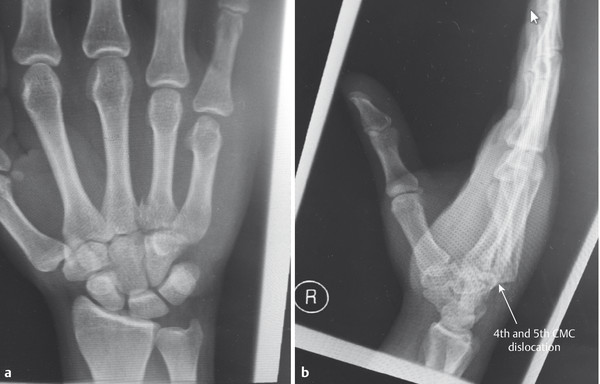
These injuries can be easily missed and that is why it is essential to always examine three views (anteroposterior [AP], lateral, oblique) in the emergency department (Fig. 14‑10 a,b). They are inherently unstable and even after reduction under anesthesia the base of the fourth and fifth metacarpal will often re-dislocate even in a well-molded plaster cast.
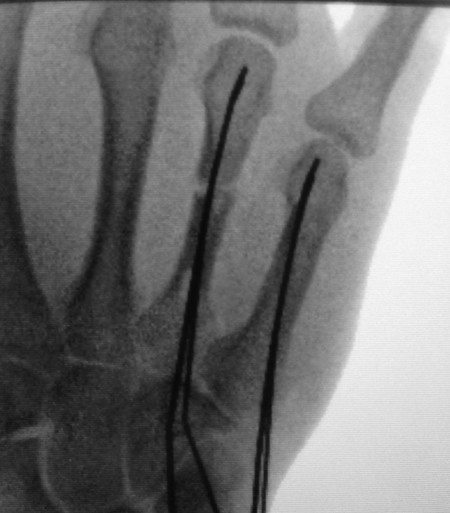
The best approach is closed reduction and Kirschner wires going into the hamate bone from the fourth and fifth metacarpals (Fig. 14‑11). Rarely, it is necessary to open these fractures to achieve reduction.
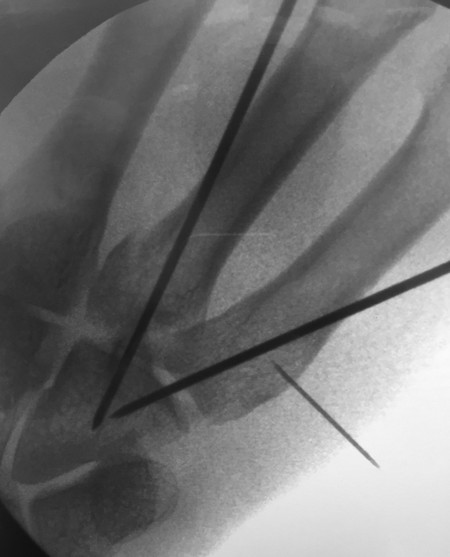
14.6 Bouquet Pinning
The case illustrates bouquet osteosynthesis in a neck of fifth metacarpal fracture and a transverse shaft of fourth metacarpal fracture (Fig. 14‑12). A 2-cm transverse incision is made at the base of the fourth and fifth metacarpal. The sensory branch of the ulnar nerve is protected and the periosteum off the metacarpal base is lifted off. A burr is used to make a hole of sufficient size to accommodate two or three round-tip K-wires. The Jahss maneuver, as previously described, is performed for reduction before the K-wires are passed into the medullary canal. The bouquet osteosynthesis has the advantage of maintaining reduction without opening the fracture site and interfering with the extensor mechanism. Patients can start early mobilization after this fixation technique.
14.7 Plating of Metacarpal and Phalangeal Fractures
Third and fourth metacarpal fractures can often be managed conservatively unless there is significant displacement or rotation resulting in scissoring. This is because they are supported on either side by the transverse metacarpal ligaments that traverse from the second and fifth metacarpals.
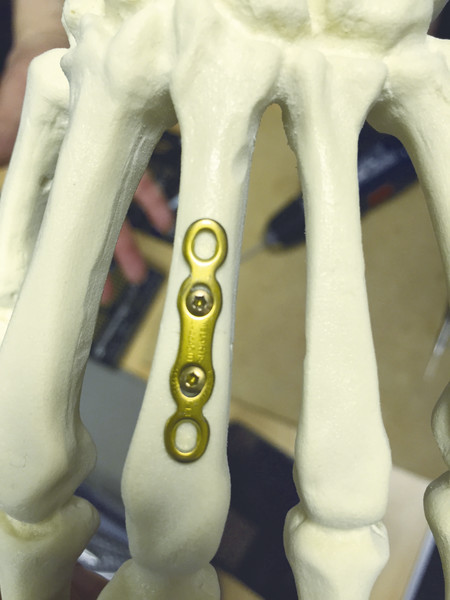
For transverse shaft fractures requiring plate fixation, dynamic compression can be obtained by eccentric screw placement in the plate (Fig. 14‑13). The plate is first secured by a neutral screw on one side of the fracture site, then a second screw is eccentrically inserted on the other side of the fracture site. Size 2.0-mm plates should be used for metacarpals, but there are cases when a 1.5-mm plate is appropriate in the smaller adult hand. In the case illustrated, a third metacarpal fracture was fixed with a 2.0-mm plate due to significant scissoring (Fig. 14‑14, Fig. 14‑15, Fig. 14‑16, Fig. 14‑17, Fig. 14‑18, Fig. 14‑19, Fig. 14‑20, Fig. 14‑21, Fig. 14‑22).
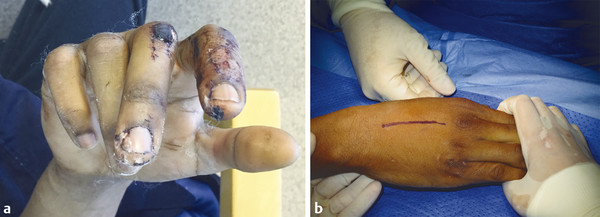
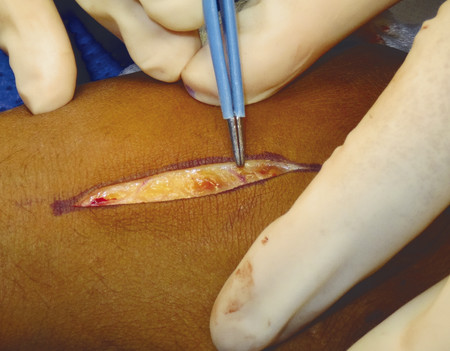
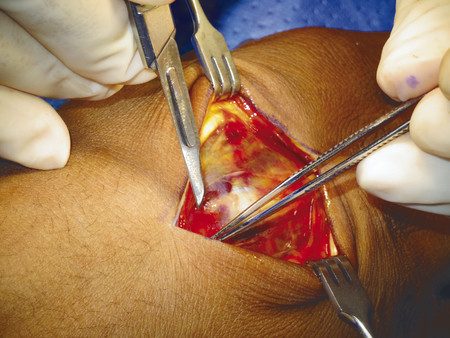
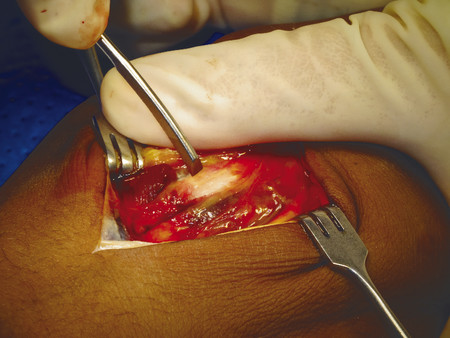
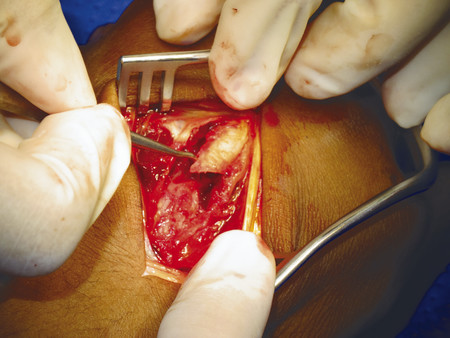
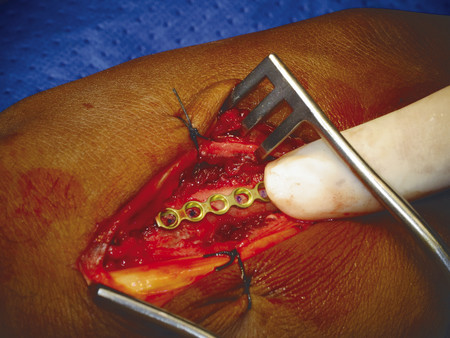
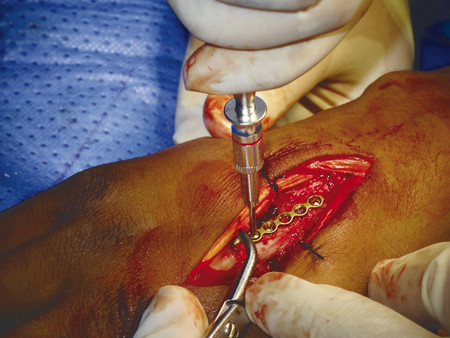
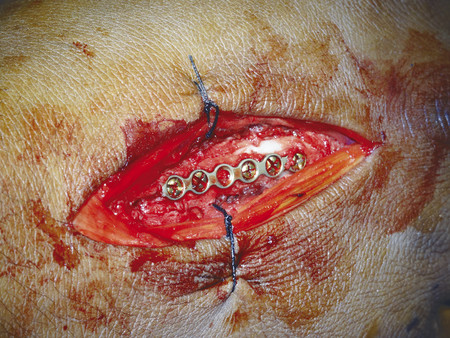
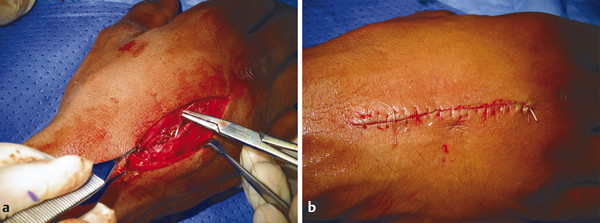
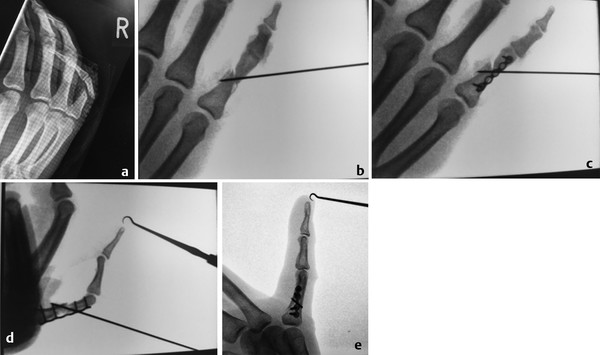
In some fractures, it is challenging to maintain reduction even with an assistant; a temporary K-wire can be used to hold the fracture before plate fixation (Fig. 14‑23). In proximal phalanx fractures, if the fracture configuration is closed, access is through a dorsal curvilinear incision and the extensor tendon is split longitudinally. A 1.5-mm plate can be placed beneath the extensor tendon. An alternative approach is to place the plate over the side of the proximal phalanx to avoid splitting of the tendon and the subsequent risk of tendon adhesions (Fig. 14‑23 e).
Placing any metalwork in the hand can interfere with tendon glide and these patients should be warned of the possibility of further surgery to remove the metalwork and perform tenolysis.
14.7.1 Rehabilitation of Metacarpal and Proximal Phalanx Fractures
The aim of all internal fixations is to provide a fracture fixation secure enough to allow early mobilization. Open reduction and internal fixation followed by immobilization is a recipe for long-term stiffness.
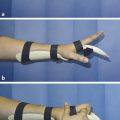
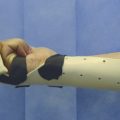
A forearm-based volar resting splint with the MCPJs in flexion and PIPJs in full extension is used in the immediate postoperative period. This is then changed for a thermoplastic splint. Active motion exercises are started immediately to prevent scar tethering and reduced motion. Splint protection is also utilized to maintain good joint positions and provide protection as necessary.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree