Abstract
Flexor tendon lacerations are disabling injuries that require surgeons to have an indepth comprehension of anatomy, surgical techniques, and dedicated rehabilitation protocols in order to optimize functional outcome. While basic principles have remained constant, certain elements in management have evolved over the past three decades and will be discussed. Clinical outcomes of flexor tendon repair have significantly improved due to advances in suturing techniques and postoperative rehabilitation.
In this chapter, we will review the anatomy, basic principles and repair techniques for flexor tendon injuries, as well as select rehabilitation protocols. As primary repair is not an option in delayed presentation of flexor tendon injuries, we will also discuss potential reconstruction options. Despite all of this, successful outcomes are not always a guarantee as patient compliance with rehabilitation is critical.
14 Flexor Tendon Injury, Repair, and Reconstruction
I. Anatomy
A. Flexor Tendon
The flexor digitorum superficialis (FDS) is innervated in the forearm by the median nerve. The flexor digitorum profundus (FDP) lies deep to FDS and is innervated by the ulnar nerve (small and ring fingers) and the median nerve (index and long fingers).
FDP has a common muscle belly, but index finger may arise independently. At the carpal tunnel, the FDS to index and small fingers lie beneath the ring and long fingers.
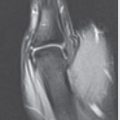
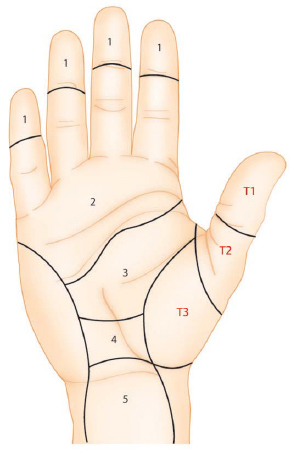
Flexor tendons are divided into five zones (► Fig. 14.1).
B. Pulleys
At the metacarpal neck, FDS and FDP enter a synovial sheath (A1 pulley). Here, the FDS splits (decussation) to allow FDP to become superficial. FDS slips then rejoin at Camper’s chiasm (over proximal phalanx) and split again to insert on the middle phalanx.
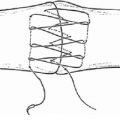
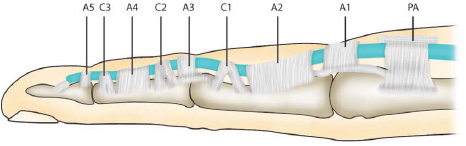
Pulley system (► Fig. 14.2): Five annular (A) and three cruciate (C) pulleys:
A1,3, and 5 originate from the volar plates of the joints, while A2 and A4 arise from the volar bone of the proximal and middle phalanx, respectively.
C1, C2, and C3 lie between the A pulleys.
C. Thumb
Flexor pollicis longus (FPL) is innervated by the anterior interosseous nerve. The thumb pulley system consists of the A1, oblique (AO), and A2 pulleys. A1 and A2 originate off the volar plate of the metacarpophalangeal (MCP) and interphalangeal (IP) joints, whereas the AO runs obliquely over proximal phalanx and is critical to FPL function. The oblique pulley is the most important for prevention of FPL bowstringing.
II. Tendon Biology
A. Nutrition (Two Sources)
Synovial diffusion (imbibition).
Direct blood supply: Vincula (short and long), intrinsic longitudinal vessels, FDP tendon insertion into distal phalanx, and proximal synovial fold.
Each tendon has hypovascular zones located between the two vincula.
B. Tendon Histology
Tendons consist of a cellular and acellular matrix of collagen (primarily Type I) and elastin, embedded within a proteoglycan-water matrix.
Cross-linking of collagen molecules and the parallel alignment of the fibers make tendons ideal for tension bearing.
C. Tendon Healing
Both intrinsic and extrinsic healing occur; extrinsic healing leads to adhesions, so goal is intrinsic healing.
Three phases:
Inflammatory (day 1 to day 5): Inflammatory cells migrate into the repair site, leaving hematoma and granulation tissue. The strength of the repair is dependent on the suture. Highest risk for tendon rupture during this time.
Proliferative (day 5 to day 21): Fibroblasts migrate and collagen synthesis occurs—mainly type III collagen.
Remodeling (3 weeks to 6 months): Collagen organization and cross-linking occurs—mainly type I collagen. Repair gains tensile strength.
III. Patient Evaluation
A. Clinical Examination
Look at finger cascade to see resting flexor tone (► Fig. 14.3).
Check sensation distal to injury (radial and ulnar sides) and finger perfusion (doppler or pulse oximeter).
Digital block after sensory examination can help to better assess motor examination.
Check FDS and FDP functions independently.
Assess for partial versus complete tendon laceration (visual inspection) and document percentage of laceration (if partial).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree