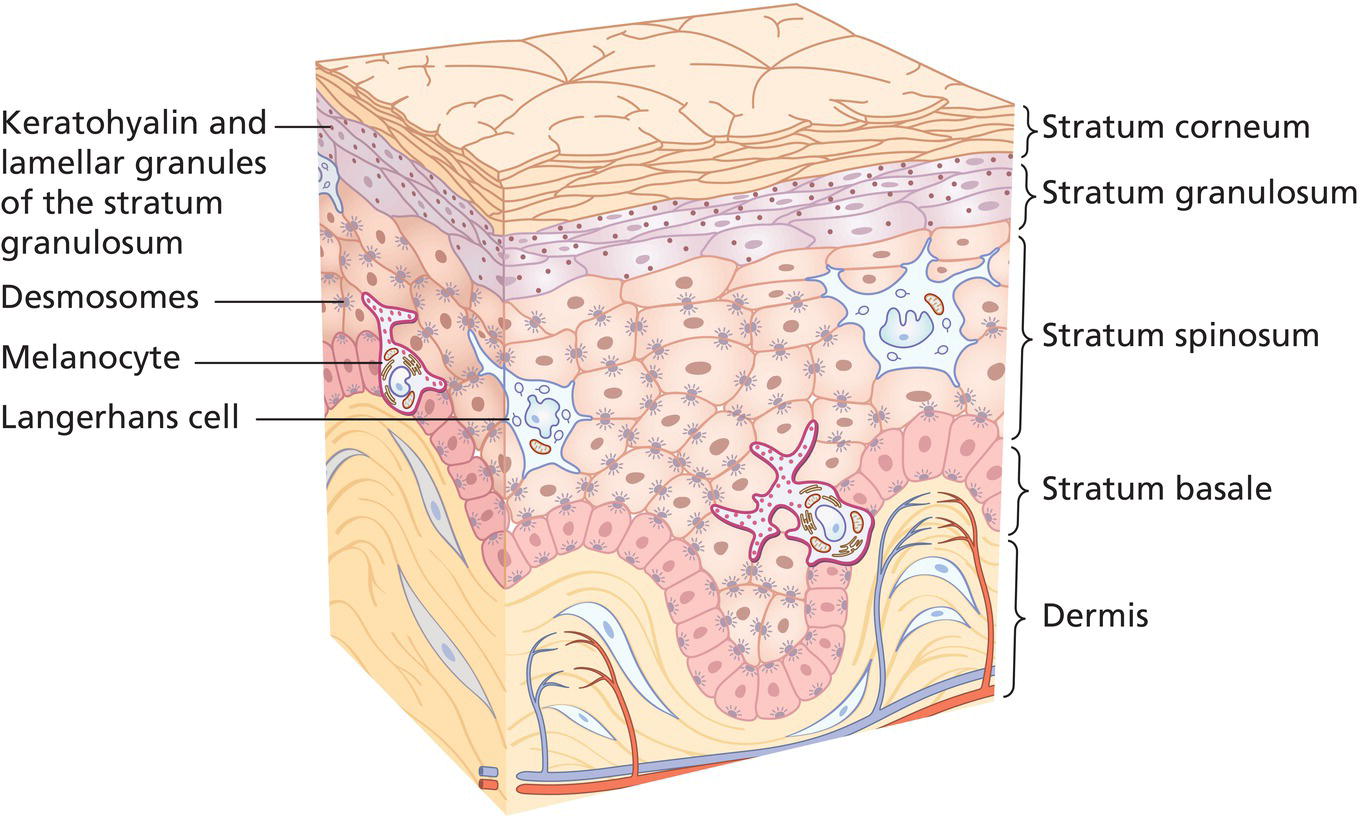
Sreekumar Pillai, Megan Manco, Christian Oresajo, and Nada Baalbaki L’Oréal Research and Innovation, Clark, NJ, USA Skin is the interface between the body and the environment. There are three major compartments of the skin, the epidermis, dermis, and the hypodermis. Epidermis is the outermost structure and it is a multilayered epithelial tissue divided into several layers. The outermost structure of the epidermis is the stratum corneum (SC), and it forms the epidermal permeability barrier which prevents the loss of water and electrolytes. Other protective/barrier roles for the epidermis include immune defense, UV protection, and protection from oxidative damage. Changes in the epidermal barrier caused by environmental factors, age, or other conditions can alter the appearance as well as the functions of the skin. Understanding the structure and function of the SC and the epidermal barrier is vital because it is the key to healthy skin and its associated social ramifications. The outer surface of the skin, the epidermis, mostly consists of epidermal cells, known as keratinocytes, that are arranged in several stratified layers – the basal cell layer, the spinous cell layer, and the granular cell layer whose differentiation eventually produces the SC. Unlike other layers, SC is made of anucleated cells called corneocytes that are derived from keratinocytes. SC forms the major protective barrier of the skin, the epidermal permeability barrier. Figure 1.1 shows the different layers of the epidermis and the components that form the epidermal barrier. SC is a structurally heterogeneous tissue composed of nonnucleated, flat, protein‐enriched corneocytes, and lipid‐enriched intercellular domains [1]. The lipids for barrier function are synthesized in the keratinocytes of the nucleated epidermal layers, stored in the lamellar bodies, and extruded into the intercellular spaces during the transition from the stratum granulosum to the SC forming a system of continuous membrane bilayers [1, 2]. In addition to the lipids, other components such as melanins, proteins of the SC and epidermis, free amino acids, and other small molecules also play important roles in the protective barrier of the skin. A list of the different structural as well as functional components of the SC is shown in Table 1.1. Corneocytes are formed by the terminal differentiation of the keratinocytes from the granular layer of the epidermis. The epidermis contains 70% water as do most tissues, yet the SC contains only 15% water. Alongside this change in water content the keratinocyte nuclei and virtually all the subcellular organelles begin to disappear in the granular cell layer leaving a proteinaceous core containing keratins, other structural proteins, free amino acids, and amino acid derivatives, and melanin particles that persist throughout the SC. From an oval or polyhedral shape of the viable cells in the spinous layers, the keratinocyte starts to flatten off in the granular cell layer and then assumes a spindle shape and finally becomes a flat corneocyte. The corneocyte itself develops a tough chemically resistant protein band at the periphery of the cell, called cornified cell envelope, formed from cross‐linked cytoskeletal proteins [3]. Figure 1.1 Diagram of the epidermis indicating the different layers of the epidermis and other structural components of the epidermal barrier. Table 1.1 Structural and functional components of the stratum corneum. Cornified envelope (CE) contains highly cross‐linked proteins formed from special precursor proteins synthesized in the granular cell layer, particularly involucrin, loricrin, and cornifin. In addition to these major protein components, several other minor unique proteins are also cross‐linked to the CE. These include proteins with specific functions such as calcium‐binding proteins, antimicrobial and immune functional proteins, proteins that provide structural integrity to SC by binding to lipids and desmosomes, and protease inhibitors. The cross‐linking is promoted by the enzyme transglutaminase that is detectable histochemically in the granular cell layer and lower segments of the SC. The γ‐glutamyl link that results from transglutaminase activity is extremely chemically resistant and this provides the cohesivity and resiliency to the SC. Lamellar granules or bodies (LG or LB) are specialized lipid carrying vesicles formed in suprabasal keratinocytes, destined for delivery of the lipids in the interface between the corneocytes. These lipids form the essential component of the epidermal permeability barrier and provide the “mortar” into which the corneocyte “bricks” are laid for the permeability barrier formation. When the granular keratinocytes mature to the SC, specific enzymes within the LB process the lipids, releasing the nonpolar epidermal permeability barrier lipids, namely, cholesterol, free fatty acids (FFAs), and ceramides, from their polar precursors‐phospholipids, glucosyl ceramides, and cholesteryl sulfate, respectively. These enzymes include lipases, phospholipases, sphingomyelinases, glucosyl ceramidases, and sterol sulfatases [4, 5]. The lipids fuse together in the SC to form a continuous bilayer. It is these lipids along with the corneocytes that constitute the bulk of the water barrier property of the SC [4, 6]. LG are enriched in a specific lipid unique to the keratinizing epithelia such as the human epidermis. This lipid (a ceramide) has a very long chain omega‐hydroxy fatty acid moiety with linoleic acid linked to the omega hydroxyl group in ester form. This lipid is processed within SC to release the omega hydroxyl ceramide that gets cross‐linked to the amino groups of the CE proteins. The molecular structure of these components suggests that the glutamine and serine residues of CE envelope proteins such as loricrin and involucrin are covalently linked to the omega hydroxyl ceramides [6, 7]. In addition, other FFAs and ceramides (Cer), may also form protein cross‐links on the extracellular side of the CE, providing the scaffold for the corneocytes to the lipid membrane of the SC. Desmosomes are specialized cell structures that provide cell‐to‐cell adhesion (Figure 1.1). They help to resist shearing forces and are present in simple and stratified squamous epithelia as in human epidermis. Desmosomes are molecular complexes of cell adhesion proteins and linking proteins that attach the cell surface adhesion proteins to intracellular keratin cytoskeletal filaments proteins. Some of the specialized proteins present in desmosomes are cadherins, calcium‐binding proteins, desmogleins, and desmocollins. Cross‐linking of other additional proteins such as envoplakins and periplakins further stabilizes desmosomes. Corneodesmosomes are remnants of the desmosomal structures that provide the attachment sites between corneocytes and cohesiveness for the corneocytes in the SC. Corneodesmosomes have to be degraded by specialized proteases and glycosidases, mainly serine proteases (SP), for the skin to shed in a process called desquamation [8]. Keratohyalin granules are irregularly shaped granules present in the granular cells of the epidermis, thus providing these cells the granular appearance (Figure 1.1). These organelles contain abundant amount of keratins “bundled” together by a variety of other proteins, most important of which is filaggrin (filament aggregating protein). An important role of this protein, in addition to bundling of the major structural protein, keratin of the epidermis, is to provide the natural moisturizing factor (NMF) for the SC. Filaggrin contains all the amino acids that are present in the NMF. Filaggrin, under appropriate conditions, is dephosphorylated and proteolytically digested during the process when granular cells mature into corneocytes. The amino acids from filaggrin are further converted to the NMF components by enzymatic processing and are retained inside the corneocytes as components of NMF [4, 9]. Perhaps the most studied and the most important function of SC is the formation of the epidermal permeability barrier [1, 4, 9]. SC limits the transcutaneous movement of water and electrolytes, a function that is essential for terrestrial survival. Lipids, particularly ceramides, cholesterol, and FFAs, together form lamellar membranes in the extracellular spaces of the SC that limit the loss of water and electrolytes. Corneocytes are embedded in this lipid‐enriched matrix, and the CE, which surrounds corneocytes, provides a scaffold necessary for the organization of the lamellar membranes. Extensive research, mainly by Peter Elias’ group has elucidated the structure, properties, and the regulation of the skin barrier by integrated mechanisms [5, 10, 11]. Barrier disruption triggers a cascade of biochemical processes leading to rapid repair of the epidermal barrier. These steps include increased keratinocyte proliferation and differentiation, increased production of corneocytes and production, processing and secretion of barrier lipids, ultimately leading to the repair of the epidermal permeability barrier. These events are described in more detail in the barrier homeostasis section below. A list of the different functions of human epidermis is shown in Table 1.2. Table 1.2 Barrier functions of the epidermis. CE provides mechanical strength and rigidity to the epidermis, thereby protecting the host from injury. Specialized protein precursors and their modified amino acid cross‐links provide the mechanical strength to the SC. One such protein, trichohyalin is a multifunctional cross‐bridging protein that forms intra and inter protein cross‐links between cell envelope structure and cytoplasmic keratin filament network [12]. Special enzymes called transglutaminases, some present exclusively in the epidermis (transglutaminase 3), catalyze this cross‐linking reaction. In addition, adjacent corneocytes are linked by corneodesmosomes, and many of the lipids of the SC barrier are also chemically cross‐linked to the CE. All these chemical links provide the mechanical strength and rigidity to the SC. The epidermal barrier acts as a physical barrier to pathogenic organisms that attempt to penetrate the skin from the outside environment. Secretions such as sebum and sweat and their acid pH provide antimicrobial properties to skin. Microflora that normally inhabit human skin can contribute to the barrier defenses by competing for nutrients and niches that more pathogenic organisms require, by expressing antimicrobial molecules that kill or inhibit the growth of pathogenic microbes and by modulating the inflammatory response [13]. Desquamation that causes the outward movement of corneocytes and their sloughing off at the surface also serves as a built‐in mechanism inhibiting pathogens from colonizing the skin. Innate immune function of keratinocytes and other immune cells of the epidermis such as Langerhans cells and phagocytes provide additional immune protection in skin. Epidermis also generates a spectrum of antimicrobial lipids, peptides, nucleic acids, proteases, and chemical signals that together forms the antimicrobial barrier (Table 1.3). The antimicrobial peptides are comprised of highly conserved small cysteine‐rich cationic proteins that are expressed in large amounts in skin. They contain common secondary structures that vary from α helical to β sheets, and their unifying characteristic is the ability to kill microbes or inhibit them from growing. Pathways that generate and regulate the antimicrobial barrier of the skin are closely tied to pathways that modulate the permeability barrier function. Expression of endogenous AMPs coincides with the presence of a number of epidermal structural components that may become part of the permeability barrier. For instance, murine cathelin‐related antimicrobial peptide CRAMP and mBD‐3 are essential for permeability barrier homeostasis. In addition, acute and chronic skin barrier disruption lead to increased expression of murine β‐defensins (mBDs)‐1, ‐3, and ‐14, and this increase in expression is diminished when the barrier is artificially restored [13]. Table 1.3 Antimicrobial components of epidermis and stratum corneum. NMF is a collection of water‐soluble compounds that are found in the SC (Table 1.4). These compounds compose approximately 20–30% of the dry weight of the corneocyte. Many of the components of the NMF are derived from the hydrolysis of filaggrin, a histidine‐, and glutamine‐rich basic protein of the keratohyalin granule. SC hydration level controls the protease that hydrolyzes filaggrin and histidase that converts histidine to urocanic acid. As NMF is water soluble and can easily be washed away from SC, the lipid layer surrounding the corneocyte helps seal the corneocyte to prevent loss of NMF. In addition to preventing water loss from the organism, SC also acts to provide hydration and moisturization to skin. NMF components absorb and hold water allowing the outermost layers of the SC to stay hydrated despite exposure to the harsh external environment. Glycerol, a major component of the NMF, is an important humectant present in skin that contributes skin hydration. Glycerol is produced locally within SC by the hydrolysis of triglycerides by lipases but also taken up into the epidermis from the circulation by specific receptors present in the epidermis called Aquaporins [14]. Other humectants in the NMF include urea, sodium, and potassium lactates and PCA [9]. Table 1.4 Approximate composition of skin natural moisturizing factor.
CHAPTER 1
Epidermal Barrier
Introduction
Structural components of the epidermal barrier
Corneocytes
Components
Function
Location
Stratum corneum (SC)
Protection
Topmost layer of epidermis
Cornified envelope (CE)
Resiliency of SC
Outer surface of the SC
Cornified envelope precursor proteins
Structural proteins that are cross‐linked to form CE
Outer surface of the SC
Lamellar granules (LG)
Permeability barrier of skin
Granular cells of epidermis
SC interfacial lipids
Permeability barrier of skin
Lipid bilayers between SC
Lipid–protein cross‐links
Scaffold for corneocytes
Between SC and lipid bilayers
Desmosomes and corneodesmosomes
Intercellular adhesion and provide shear resistance
Between keratinocytes and corneocytes
Keratohyalin granules
Formation of keratin “bundles” and NMF precursor proteins
Stratum granulosum
Natural moisturizing factor (NMF)
Water holding capacity of SC
Within SC
pH and calcium gradients
Provides differentiation signals and LG secretion signals
All through epidermis
Specialized enzymes (lipases, glycosidases, and proteases)
Processing and maturation of SC lipids, desquamation
Within LG and all through epidermis
Melanin granules and “dust”
UV protection of skin
Produced by melanocytes of basal layer, melanin “dust” in SC
Proteins of the cornified envelope
Lamellar granules and inter‐corneocyte lipids
Lipid–protein cross‐links at the cornified envelope
Desmosomes and corneodesmosomes
Keratohyalin granules
Functions of epidermal barrier
Water evaporation barrier (epidermal permeability barrier)
Function
Localization/components involved
Water and electrolyte permeability barrier
SC/corneocyte proteins and extracellular lipids
Mechanical barrier
SC/corneocytes, cornified envelope
Microbial barrier/immune function
SC/lipid components/viable epidermis
Hydration/moisturization
SC/NMF
Protection from environmental toxins/drugs
SC/corneocytes, cornified envelope
Desquamation
SC/epidermis/proteases and glycosidases
UV barrier
SC/melanins of SC/epidermis
Oxidative stress barrier
SC, epidermis/antioxidants
Mechanical barrier
Antimicrobial barrier and immune protection
Component
Class of compound
Localization
Free fatty acids
Lipid
Stratum corneum
Glucosyl ceramides
Lipid
Stratum corneum
Ceramides
Lipid
Stratum corneum
Sphingosine
Lipid
Stratum corneum
Defensins
Peptides
Epidermis
Cathelicidin
Peptides
Epidermis
Psoriasin
Protein
Epidermis
RNAse 7
Nucleic acid
Epidermis
Low pH
Protons
Stratum corneum
“Toll‐like” receptors
Protein signaling molecules
Epidermis
Proteases
Proteins
Stratum corneum and epidermis
NMF and skin hydration/moisturization
Components
% levels
Amino acids and their salts (over a dozen)
30–40
Pyrrolidine carboxylic acid (PCA) sodium salt, urocanic acid, ornithine, citrulline (derived from filaggrin hydrolysis products)
7–12
Urea
5–7
Glycerol
4–5
Glucosamine, creatinine, ammonia, uric acid
1–2
Cations (sodium, calcium, potassium)
10–11
Anions (phosphates, chlorides)
6–7
Lactate
10–12
Citrate, formate
0.5–1.0
Protection from environmental toxins and topical drugs penetration
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree