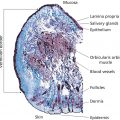
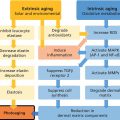
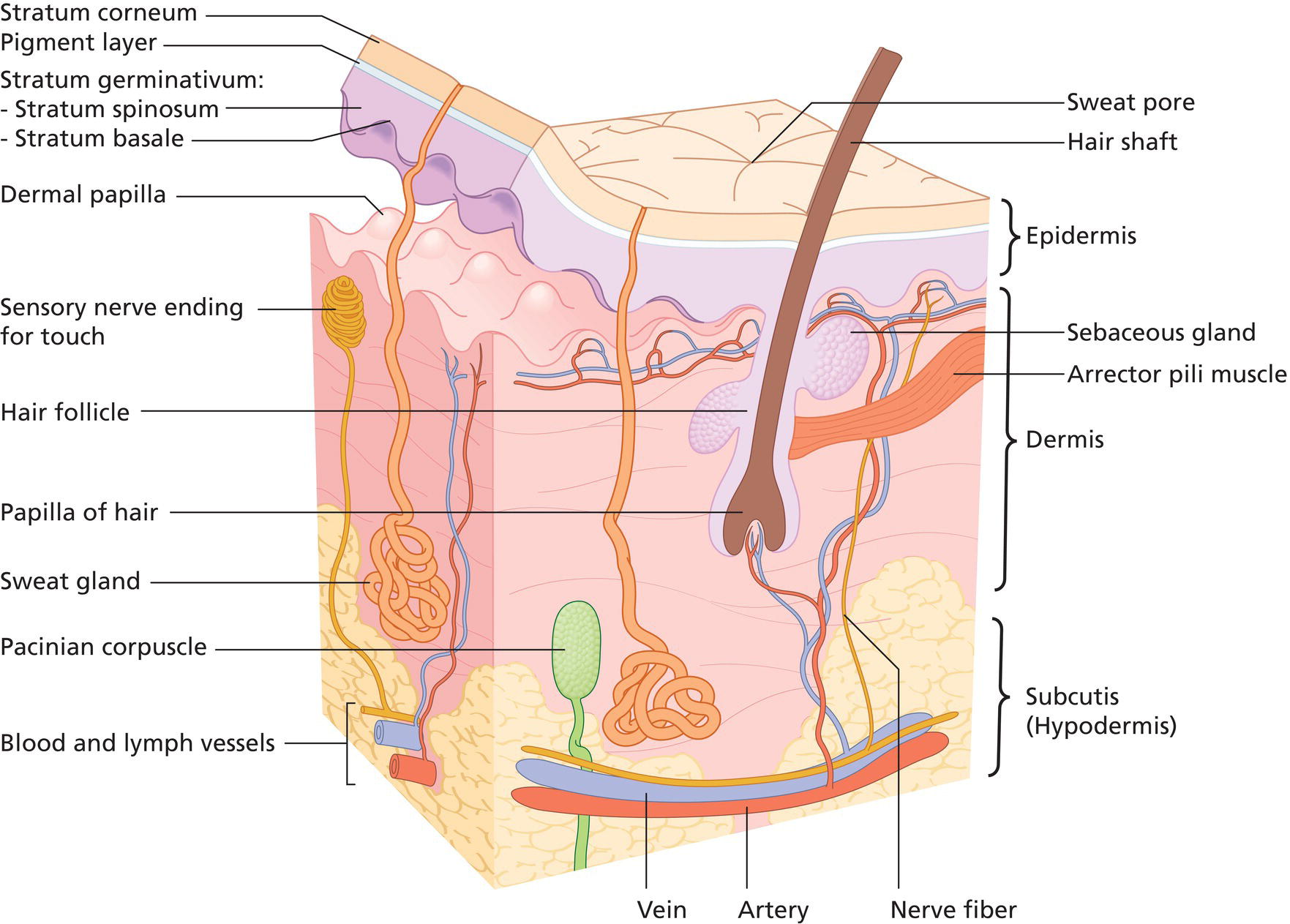
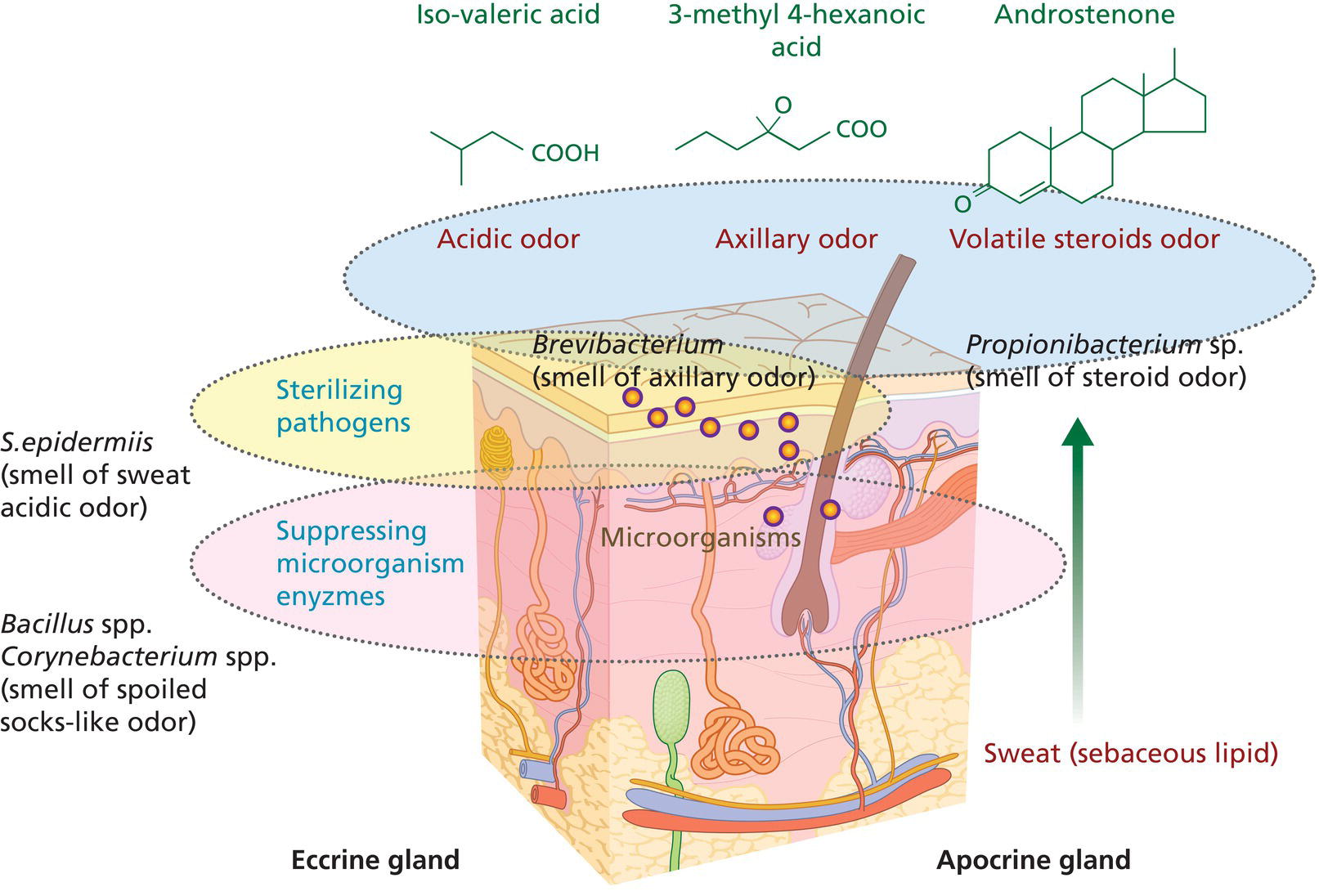
Eric S. Abrutyn TPC2 Advisors and Personal Care Consultant, Bellingham, WA, USA This chapter deals with the technologies for wetness and odor protection of the human axilla, how they are applied, and potential adverse effects of use of these products on a regular basis. Antiperspirants and deodorants have been used for centuries, evolving from simple fragrances that masked offensive odors to today’s complex ingredients based on aluminum and zirconium chemistries that act to slow or diminish sweat production, or botanical extracts with antimicrobial activity. Odors (scents) and sweating have a biological significance. Body scents are primeval and most likely evolved genetically to attract the opposite sex. Sweating is regulated by the sympathetic nervous system and is an important body temperature regulator, especially in warm weather climates or during heavy exercise, and functions to remove waste and toxic by‐products of the body. The axilla area of the body represents a small contribution to sweating to control body temperature and removal of biological by‐products, so the controlling of sweat from this area has fewer health risks than other areas of the body. There is little scientific evidence that supports the idea that the use of antiperspirants, based on aluminum or aluminum–zirconium chemistry causes appreciable lasting adverse effects other than possible temporary and reversible irritation. Sweating is necessary to control body temperature, especially during times of exercise and warm or hot surroundings. Sweat by itself is odorless and only establishes a characteristic odor when exposed to moisture (humidity) in the presence of bacterial flora on the skin surface, breaking down the sweat’s composite and resulting in unpleasant odors. The use of antimicrobial agents is a good defense in preventing odor development from bacteria and yeast present on the skin. Another defense is the reduction of excretion from the eccrine gland to minimize available moisture that can promote the degradation of axillary exudate and the appearance of uncomfortable or unsightly wetness production. According to Gray’s Anatomy [1], most people have several million sweat glands distributed over their bodies, to include the underarm axilla, thus providing plenty of opportunity for body odors to develop. Skin has two types of sweat gland: eccrine glands and apocrine glands (Figures 22.1 and 22.2). Eccrine glands open directly on to the surface of the underarm axilla and exude sweat, subsequently contributing to odor formation. These glands are located in the middle layer of the skin called the dermis, which is also made up of nerve endings, hair follicles, and blood vessels. Sweat is produced in a long coil embedded within the dermis where the long part is a duct that connects the gland to the opening (pore) on the skin’s surface. When body temperature rises, the autonomic nervous system stimulates these glands to secrete fluid onto the surface of skin, where it then cools the body as it evaporates. The composition of the eccrine gland secretion is about 55–60% fluid, mostly water with various salts (primarily: sodium chloride, potassium chloride) and various electrolytic components (ammonia, calcium, copper, lactic acid, potassium, and phosphorus) (Figure 22.3). Figure 22.1 Underarm sweat gland mechanism. Figure 22.2 Cross‐section of skin and sweat glands. The apocrine glands are triggered by exercise and emotional stress, contracting the tubule gland to push out fatty organic and steroidal matter to the surface of skin where bacterial flora begins breaking it down. (Figure 22.3) These glands are dormant until puberty; at which time they start to secrete. The warmth and limited air flow are conducive to allowing for rapid decomposition of organic matter made up of primarily low molecular weight volatile fatty acids and steroidal compounds that propagate the recognizable body odors. In the Food and Drug Administration (FDA) Final regulatory Antiperspirant Monograph [2], through the Food Drug and Cosmetic Act, defines antiperspirants as an over‐the counter (OTC) drug when applied topically to reduce production of underarm sweat (perspiration). They are considered drugs because they can affect the function of the body by reducing the amount of sweat that reaches the skin surface. In the United States, OTC drugs are subjected to monograph rules, which define standards and requirements, premarket approval process, acceptable actives, and allowable formulation percentages of actives. Other countries’ regulations vary in content and scope. Some countries consider antiperspirants as cosmetics and not affecting the biologic physiology of the body; as such they are not held to the same strict standards as in the United States. As an example, Canada (2008) ruled that antiperspirants were no longer being considered a drug; their use only needs to comply with cosmetic regulations. The consumer typically confuses what antiperspirants and deodorants do, mostly caused by a misunderstanding of marketing claims and product positioning. For the most part, antiperspirants are based on aluminum‐based cationic salt chloride complexes (as well as complexes with zirconium acid salts) and are referred to as “actives” on the back label of consumer antiperspirant products. There are numerous types of antiperspirant actives listed in the FDA monograph as well as in the US Pharmacopia/National Formulary [3]. Antiperspirant actives are responsible for blocking sweat expulsion through the formation of temporary plugs within the sweat duct, thus stopping or slowing down the flow of sweat to the surface of the ecrrine gland. A theory of wetness control that has been accepted over the years is that the hydrated aluminum or aluminum–zirconium cationic salt chloride is transported to the ecrrine gland, interacting with the protein contained within the gland. In this basic protein environment, the antiperspirant active is reduced, producing a gelatinous proteinaceous plug. Dr. Shaotang Yuan and associates have recently provided research details on the formation of the proteinaceous plug [4], substantiating the reaction of aluminium containing antiperspirant actives with protein. The authors were also able to confirm, that by measuring the Zeta potential, a reduction in the size of the aluminium containing antiperspirant active improves the mobility of the active into the ecrrine gland to increase the effectiveness of wetness control. Figure 22.3 Sweat metabolism cycle. By plugging the gland, sweat is prohibited from transporting to the surface, causing osmotic pressure. Though it should be noted that the effectiveness of plugging all the ecrrine glands in the axilla is probably no more than 80% efficient. Eventually, within 2–3 weeks on stoppage of antiperspirant application, all the proteinaceous plugged in the ecrrine glands are pushed out, considered the washout period, and the gland is allowed to operate again in its normal fashion. Without going into detail, one can describe how antiperspirants are tested for their Wetness Inhibiting Performance (“WIP”™1) effectiveness. The FDA prescribes a methodology for testing the effectiveness of an antiperspirant by having participants tested in a controlled environment – 30–40% relative humidity at approximately 100°F. Sweat is continuously collected during two 20‐minute intervals and reported as the production or percentage change in production over the average of two 20‐minute collection periods [2, 5
CHAPTER 22
Antiperspirants and Deodorants
Introduction
Physiology
Sweat glands and how they work
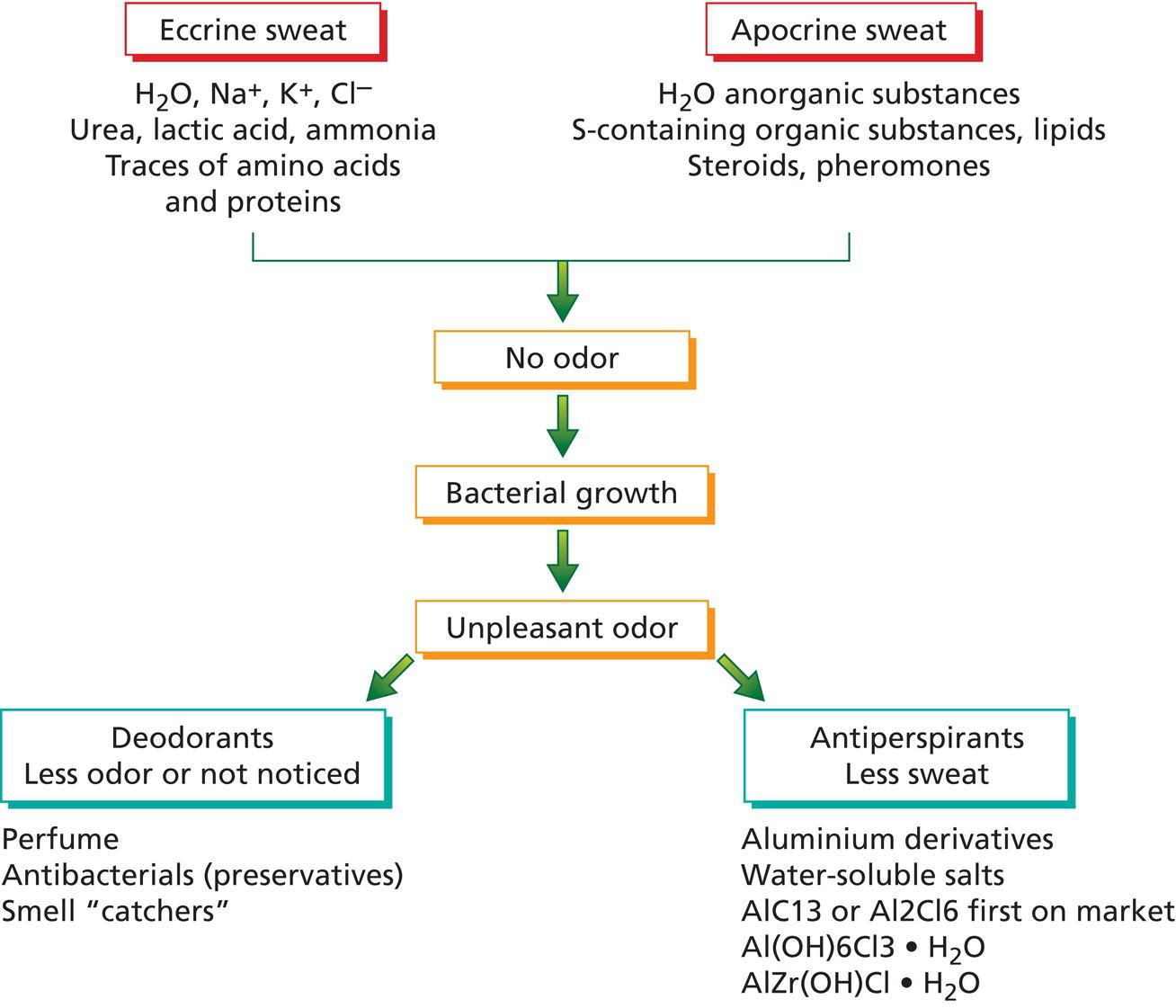
Wetness and odor control and testing
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree