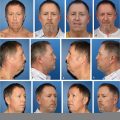
Plastic surgery helps in cancer treatment and recovery when tumor removal leaves defects that affect function, appearance, or both. In oncology, reconstructive procedures are used after breast, skin, head and neck, and other cancer surgeries to restore tissue coverage, rebuild shape, and support daily functions such as speaking, swallowing, or closing a wound properly.
As reported by PMC, 18.6 million people in the United States were living with a history of cancer in the past year. This shows why cancer care often includes not only tumor treatment, but also reconstruction, recovery, and long-term function after surgery.
What Does Reconstructive Plastic Surgery Do in Cancer Care?
Reconstructive plastic surgery restores form and function after cancer treatment. Its role is broader than appearance alone because surgeons may need to rebuild skin, soft tissue, muscle, bone, or breast shape after tumor removal. That is why reconstruction is often planned alongside cancer surgery rather than treated as a separate cosmetic step.
Breast Shape and Symmetry
Breast reconstruction is one of the best-known examples of plastic surgery in oncology. The American Cancer Society notes that reconstruction can begin at the same time as mastectomy or lumpectomy or be done later, and the two main approaches are implant reconstruction and tissue, or flap, reconstruction.
Facial and Oral Function
In head and neck cancer, reconstruction often supports much more than appearance. Free skin, bone, and muscle transfer may be used to reconstruct the tongue, floor of the mouth, cheek, lip, pharynx, and jaw. This helps restore facial structure and supports swallowing, speech, and chewing.
Tissue Coverage and Wound Closure
Flap surgery moves healthy tissue from one part of the body to another to repair damaged areas. In cancer reconstruction, it is used when tumor removal leaves tissue that cannot heal well or needs stronger coverage. Microsurgical free flaps are especially important in major head and neck and facial reconstruction because they allow safe transfer of complex tissue.
Where to Find Oncology News Today on Reconstruction and Recovery?
Following updates on reconstructive surgery and recovery after cancer treatment can help patients and caregivers better understand how surgical care fits into the broader treatment plan. It also gives more context on what happens after tumor removal and how recovery may affect function, appearance, and daily life.
For readers looking for oncology news today, this type of coverage can also help track wider developments in reconstruction, survivorship, and post-treatment recovery. It adds useful context around how oncology care continues beyond diagnosis and primary treatment.
When Is Reconstruction Done?
Reconstruction may be immediate or delayed, and the best timing depends on the cancer treatment plan. Some patients have reconstruction during the same operation as tumor removal, while others need to wait until radiation, healing, or broader treatment decisions are complete.
The timing usually depends on these factors:
- Immediate reconstruction: This starts at the time of mastectomy or another cancer operation and may reduce the number of separate surgical stages for some patients.
- Delayed reconstruction: This is often chosen when cancer treatment is still ongoing or when the team wants to wait until the body has recovered from initial therapy.
- Radiation planning: Radiation can affect healing and reconstruction outcomes, so flap reconstruction is often delayed.
- Overall health and readiness: Surgical timing also depends on the patient’s health, recovery capacity, and priorities after diagnosis and tumor treatment.
How Does Plastic Surgery Help After Breast Cancer?
Plastic surgery helps after breast cancer by rebuilding breast shape, improving symmetry, and restoring tissue lost during mastectomy or lumpectomy. Reconstruction can be done at the same time as a mastectomy or later, using either implants or tissue from another part of the body.
Implant Reconstruction
Implant reconstruction is often chosen when a patient wants a shorter operation and an easier initial recovery. It usually starts with a tissue expander before the final implant is placed. This approach is less invasive, but implants may later need replacement or removal over time.
Flap Reconstruction
Flap reconstruction uses the patient’s own tissue and is often chosen when a more natural feel is important or when radiation has affected the chest wall. It can restore breast shape and replace damaged tissue, but recovery is more complex, and a donor-site scar remains after surgery.
Example: Flap reconstruction is often more suitable after prior radiation, when the chest wall becomes tight, scarred, or poorly supplied with blood and needs healthy tissue from another part of the body to improve coverage and healing.
Timing With Radiation
Radiation often affects reconstruction timing because it can slow healing and raise the risk of complications. Because of this, some patients delay reconstruction until radiation is complete, although immediate reconstruction may still be possible in selected cases with careful planning.
How Does Plastic Surgery Help After Skin Cancer?
Plastic surgery helps after skin cancer by closing the wound safely, restoring function, and improving how the repaired area looks. It may use direct closure, flaps, or grafts depending on the size and location of the defect, especially in areas such as the nose, lips, eyelids, scalp, or ears.
- Closing the defect safely: Some wounds can be closed directly, while larger or deeper defects need more advanced repair.
- Preserving function: Reconstruction is especially important when cancer affects the nose, lips, eyelids, scalp, or ears, where repair must preserve function and looks.
- Using the right tissue method: Flaps and grafts are common in facial skin cancer reconstruction because they replace damaged areas with healthy tissue.
- Limiting visible distortion: Because Mohs surgery preserves healthy tissue, reconstruction can be planned more precisely once the final defect is clear.
One common example is a defect on the nose after Mohs surgery, which may require a flap or graft to preserve contour, support healing, and protect function.
How Does Plastic Surgery Help After Head and Neck Cancer?
Plastic surgery is especially important after head and neck cancer because tumor removal can affect speech, swallowing, chewing, facial movement, and appearance at the same time. Reconstruction in this area may involve transfer of skin, muscle, or bone to rebuild the tongue, floor of mouth, cheek, lip, pharynx, skull, scalp, or jaw.
Restoring Oral and Facial Structures
When tumors involve the jaw, mouth, or cheek, reconstructive surgery can replace missing tissue and help preserve facial structure. After jaw tumor surgery, reconstruction may involve bone grafts, skin grafts, free flap surgery, or prosthetic devices to restore form and oral function.
Supporting Speech and Swallowing
This is one of the clearest examples of reconstruction serving a medical function rather than only a cosmetic one. Tissue transfer may be used to rebuild the tongue, floor of the mouth, cheek, lip, or pharynx after major cancer surgery, which directly supports speech and swallowing recovery.
Example: After partial tongue removal, soft tissue from another part of the body may be used to restore bulk and mobility, helping the patient control food in the mouth and speak more clearly.
Rebuilding With Free Flaps
Free flap reconstruction is often used when the defect is too large or complex for simple closure. It allows surgeons to move healthy tissue with its own blood supply into an area that needs more advanced repair, which is especially important in difficult head and neck defects.
Example: When cancer surgery removes part of the jaw and surrounding soft tissue, a free flap can help rebuild the lower face, support oral function, and improve structural stability during recovery.
How Does Plastic Surgery Support Recovery?
Plastic surgery supports recovery by helping wounds heal properly, restoring function, and reducing the long-term burden of tissue loss after cancer surgery. Recovery does not mean the same thing in every cancer type, but reconstruction often improves how well the body closes, protects, or uses the treated area after tumor removal.
- Better tissue coverage: Flaps and grafts can cover exposed structures and improve healing in areas that would otherwise close poorly.
- Functional recovery: In head and neck cancer, reconstruction can support swallowing, speech, chewing, and facial movement.
- Stepwise physical recovery: Recovery usually happens in stages, with longer healing after flap procedures than after implants.
- Quality-of-life support: Reconstruction can ease the daily burden of a visible or functionally difficult defect, even when full restoration is not possible.
When Is Plastic Surgery Not Recommended?
Plastic surgery may not be recommended when healing is less reliable or the risk is higher. This can include smoking, poor circulation, diabetes, obesity, or situations where a non-surgical option better fits the patient’s health, preferences, or recovery goals.
Smoking
Smoking can reduce blood flow, slow healing, and increase the risk of complications after reconstruction. Because of this, some patients are advised to stop smoking before surgery, especially before flap procedures, where a stable blood supply is essential for tissue survival.
Circulation Problems
Good blood flow is essential for flap survival and reliable healing after reconstruction. Conditions that affect circulation can make tissue repair less predictable, limit oxygen delivery to healing tissue, and raise the risk of flap failure or other surgical complications.
Diabetes and Obesity
Diabetes and obesity can increase complication risk and make recovery more difficult after reconstruction. These conditions may slow wound healing, raise infection risk, and complicate the overall surgical course, especially when the procedure is extensive or recovery is already expected to be demanding.
Need for Alternatives
Plastic surgery is not always the right choice when surgery is not wanted or medically advisable. In these cases, some patients choose prostheses, breast forms, or no reconstruction after treatment, especially when a non-surgical option better matches their health status, preferences, or recovery priorities.
Conclusion
Plastic surgery helps in cancer treatment and recovery when reconstruction is needed to restore tissue, protect healing, or recover function after tumor removal. It is most clearly useful after breast, skin, and head and neck cancer surgery, where the effect of treatment often goes beyond the tumor itself and changes how the body looks or works.
Its value is strongest when it is planned as part of oncology care rather than added as an afterthought. The right timing, method, and goals depend on cancer type, radiation plans, overall health, and whether the priority is wound closure, function, appearance, or all three at once.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree