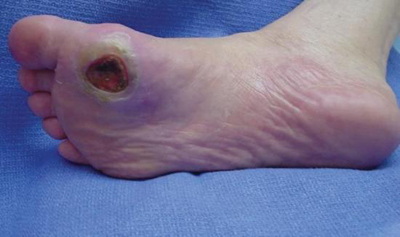
Ayman Grada, Tania Phillips Ulcers are skin injuries that result in complete absence of the epidermis. They result from a diverse range of underlying diseases. Because they frequently reflect the presence of underlying disease states, accurate diagnosis is imperative. This chapter reviews cutaneous ulcers with an emphasis on diabetic ulcers, pressure ulcers, vasculitic ulcers, arterial ulcers, pyoderma gangrenosum, and surgical site infections. diabetic ulcers pressure ulcers vasculitic ulcers arterial ulcers pyoderma gangrenosum surgical site infections Diabetic wounds are multifactorial in etiology. Patients with long-standing diabetes develop polyneuropathy, which creates sensory, motor, and proprioceptive abnormalities and can lead to insensate skin and foot deformities. Combined with vascular disease and immunosuppression, patients have a high risk for trauma, subsequent ulceration, and infection. Most diabetic foot ulcers (DFUs) result from peripheral neuropathy (60%–70%), peripheral vascular disease (15%–20%), or a combination of both (15%–20%). Approximately 2% to 3% of all patients with diabetes will develop a DFU in a given year, and 10% to 25% of all patients with diabetes will develop at least one DFU in their lifetime. Approximately 50% to 60% of patients with a DFU have clinical signs of infection at the time of hospital admission. DFU accounts for nearly two-thirds of all nontraumatic amputations performed in the United States. The differential includes nondiabetic neuropathic ulcers, arterial ulcers, pressure ulcers, calciphylaxis, venous ulcers, and drug-induced cutaneous necrosis. Treatment of tinea pedis and onychomycosis will prevent the development of skin cracks and bacterial entry (which can lead to cellulitis). If present, treat concomitant cellulitis or osteomyelitis with the appropriate antibiotics. Surgical (sharp) debridement at frequent intervals has been shown to heal neuropathic wounds more rapidly. Necrotic and callus tissue should be debrided to a healthy bleeding base. This allows for a more thorough examination of the wound and activation of platelets and allows the proliferative phase of healing to begin. Patients can avoid repetitive trauma by using mechanical off-loading and pressure relief techniques. These may include adhering to bed rest; using crutches, a walker, or a wheelchair; and wearing therapeutic shoes or sandals (matching the shoe gear to the anatomic alterations). Total contact casting can be a useful first step in managing Charcot foot. Foams and padding can also be used to off-load pressure. Patients should be tested regularly with a 10 g monofilament on the feet. Loss of this sensation increases the risk for undetected injuries, which can lead to amputations. Prevention is important and involves daily foot inspections, meticulous hygiene, and properly fitting shoes. Advise smoking cessation if applicable because smoking increases the risk for ulcer formation. Wound dressings are selected based on ulcer appearance and other wound characteristics (e.g., dry, exudative, infected). Ulcer beds should be kept clean and moist (not wet).
20: Ulcers
Abstract:
Diabetic ulcers
Clinical features
Symptoms
Location
Clinical findings
Differential diagnosis
Work-up
Initial steps in management
Infection control
Surgical debridement
Avoiding repetitive trauma
Prevention
Advanced/adjunctive options
Warning signs/common pitfalls
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Plastic Surgery Key
Fastest Plastic Surgery & Dermatology Insight Engine