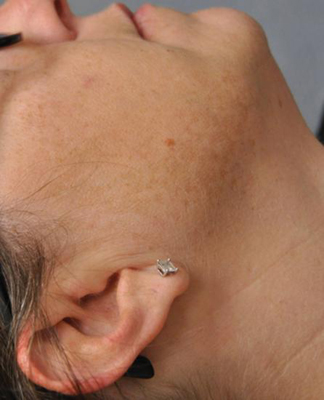
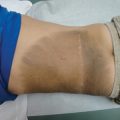
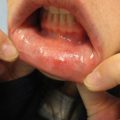
Increased skin pigmentation is a common chief complaint among millions of Americans seeking treatment for hyperpigmentation annually. Many patients self-treat with over-the-counter skin brightening and bleaching creams before seeking medical care. Unfortunately, failure to appropriately diagnose the etiology of a patient’s hyperpigmentation is likely to result in treatment failure and continued frustration. This chapter reviews melasma, lentigines, tinea versicolor, confluent and reticulated papillomatosis, and acanthosis nigricans. hyperpigmentation dyspigmentation melasma lentigo lentigines tinea versicolor Casey Abrahams and Afton Chavez Melasma is also known as “chloasma” or, colloquially, the “mask of pregnancy.” It is characterized by light to dark-brown or brown-gray patches with irregular borders that appear primarily on the face (Fig. 7.1) but also on the forearms (Fig. 7.2) and mid-upper chest. The primary differential for melasma includes drug-induced hyperpigmentation or discoloration, postinflammatory hyperpigmentation, pigmented contact dermatitis (Riehl melanosis), acquired bilateral nevus of Ota-like macules (Hori nevus), actinic lichen planus, lichen planus pigmentosus (LPP), erythema dyschromicum perstans (EDP), and exogenous ochronosis. You have melasma, a type of skin pigmentation disorder characterized by light to dark brown or brown-gray patches with irregular borders. You may notice these patches primarily on your face, but they can also be found on your forearms and mid-upper chest. If you are a young to middle-aged women with a darker skin type, you are at an increased risk for melasma. There are many treatment and prevention options for melasma. The most important step is to minimize UV exposure by wearing sun-protective hats and clothing and applying broad-spectrum sunscreen (ideally with an SPF greater than 30) daily. Melasma is exacerbated by pregnancy and estrogen-containing oral contraceptives, so you may want to consider switching to an alternative nonestrogen-containing birth control if you are on one. Your doctor may recommend as treatment the use of hydroquinone, azelaic acid, topical vitamin C, kojic acid, tranexamic acid, peels, or lasers. Topical hydroquinone should not be used for more than 3 to 6 months because of the risk for paradoxical worsening of the hyperpigmentation. Peels and lasers should only be performed by an experienced professional. If performed using an improper technique, hyperpigmentation can result. Gregory Cavanagh and Afton Chavez Lentigines are also known as “liver spots,” “age spots,” “senile freckles,” and “lentigo senilis.” They are 0.2 cm to 2 cm, well-circumscribed, round, oval, or irregularly shaped macules that vary in color from tan to dark brown or black. The differential for solar lentigines includes ephelides (freckles), PUVA (psoralen and UVA) lentigo, macular seborrheic keratosis (SK), pigmented actinic keratosis (AK), lentigo maligna, simple lentigo, junctional melanocytic nevus, and large cell acanthoma.
7: Hyperpigmented rashes
Abstract:
Melasma
Clinical features
Differential diagnosis
Work-up
Initial steps in management
Prevention and maintenance
Treatments
Warning signs/common pitfalls
Counseling
Lentigines
Clinical features
Differential diagnosis
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Plastic Surgery Key
Fastest Plastic Surgery & Dermatology Insight Engine