Facial rashes are particularly bothersome to patients because of how conspicuous they are. These rashes have an exceptionally broad differential diagnosis and appropriately diagnosing these conditions is critical to adequate management. This chapter discusses atopic dermatitis, allergic contact dermatitis, seborrheic dermatitis, actinic keratosis, actinic cheilitis, angular cheilitis, acute cutaneous lupus, orolabial herpes, and discoid lupus. atopic dermatitis allergic contact dermatitis seborrheic dermatitis actinic keratosis actinic cheilitis angular cheilitis acute cutaneous lupus orolabial herpes discoid lupus The differential for facial AD includes irritant contact dermatitis (ICD), allergic contact dermatitis (ACD), seborrheic dermatitis, discoid lupus erythematosus, tinea faciei, and psoriasis. The biggest pitfall when managing AD in any location is failure to promote patient adherence to a dry skin care management regimen. Such a regimen is essential for achieving and maintaining disease control in patients with AD; failure to implement a daily dry skin care regimen ensures treatment failure. Patients with facial dermatitis are frequently noncompliant with therapy if topical medications with poor cosmesis (e.g., ointments) are prescribed. Failure to identify coexisting dermatoses such as ICD to cosmetics, ACD (including to topical corticosteroids), and/or head and neck dermatitis can interfere with successful management. You have atopic dermatitis, also known as “eczema.” Atopic dermatitis is usually an inherited chronic skin condition (meaning there is no cure) that occurs in people who have skin that does not retain enough water and that does not adequately protect itself against outside allergens. Your skin is sensitive, prone to dryness, and susceptible to becoming itchy and developing rashes. Individuals with atopic dermatitis develop skin inflammation from within in response to the environment around them. This inflammation makes the skin red and itchy. Importantly, there is no one allergen that causes your skin disease. Additionally, dietary changes have not been reported in the medical literature as curing your disease. Treating your skin disease requires that you keep your skin healthy by moisturizing it and by avoiding exposure to things that irritate it. To keep your skin healthy, it is important that you wash your face with a gentle cleanser twice daily using your hands instead of a washcloth. After cleansing your face, you should immediately apply a moisturizer. Some people find it helpful to use a different, lighter moisturizing cream (such as a lotion or light cream) in the morning than the one they use at night because the heavy moisturizers (heavy creams or ointments) that are better for keeping the skin hydrated (e.g., CeraVe moisturizing cream or Eucerin Advanced Repair cream) may not be cosmetically suitable for use during the daytime. While your skin is still red and irritated, it is important that you do not apply any cosmetics or fragrances because these can inflame or irritate your skin. Your doctor has prescribed you a topical mild steroid cream. You should use this cream twice daily only for 7 to 10 days, at which time the redness and irritation should be gone. Alternative steroid-sparing creams may also be prescribed for more chronic or intermittent use. These prescription creams are not a substitute for your moisturizer and should be used with your moisturizer, not instead of your moisturizer. Once the redness and irritation has resolved, you can stop the prescription cream, although you may need to restart it if the redness and irritation return. The topical steroid prescribed cream can cause side effects if you use it too frequently or if you use it for too long. This includes possible thinning of the skin, increased visibility of blood vessels in the area of application, discoloration of the skin, and potentially an acnelike rash. Additionally, if this cream is applied around the eye it can cause an increase in eye pressure, which can result in glaucoma, a vision-threatening eye disease. Please tell your doctor if you have a personal or family history of glaucoma. Atopic dermatitis is cyclical, which means you will have times when your rash is much better and times when it is much worse. Different people flare for different reasons. You should try your best to identify things that are unique triggers for your atopic dermatitis. You will have to work with your doctor over time to find a skin care regimen that is right for you and that keeps your skin disease under control. The differential for facial seborrheic dermatitis includes psoriasis, ICD, acute cutaneous lupus erythematosus, ACD, Darier disease, rosacea, and, rarely, drug reactions. There is no cure for seborrheic dermatitis. The course is chronic with waxing and waning. Failure to emphasize the importance of using a maintenance therapy virtually guarantees disease recurrence and patient dissatisfaction. Treatments for seborrheic dermatitis are primarily divided into topical antifungals and topical antiinflammatory agents. Consider a patient’s bathing habits when treating seborrheic dermatitis because infrequent bathing and infrequent shampooing are a common cause of treatment failure/nonadherence to medicated shampoos. There is no cure for seborrheic dermatitis; therefore, all patients require maintenance treatment. For facial seborrheic dermatitis, cream formulations are preferable over ointments because they are typically more cosmetically acceptable. Failure to identify concomitant personal care product-induced ICD can hinder patient improvement despite appropriate treatment. Patients with acute onset of severe seborrheic dermatitis should undergo HIV testing. Patients using antifungal shampoos should alternate daily between different types of shampoos to decrease the likelihood of secondary treatment failure. You have a rash called “seborrheic dermatitis.” It is a severe form of dandruff that can involve the face and also the scalp and chest. This is a chronic, recurrent, waxing and waning type of rash, meaning that there is no cure. Most importantly, it is a self-limited type of rash, meaning that it will not cause you internal harm. This rash is the result of inflammation caused by your immune system. The exact reason that you have developed this rash is unknown. Some experts think that it develops because your immune system overreacts to fats made by a yeast called “Malassezia” that lives on your skin; however, other experts do not think this is the case. Because this is a normal skin yeast, it is not a form of infection and is not contagious. I have prescribed you an antifungal (yeast) shampoo. You should use this shampoo 3 times per week for 4 weeks. You should apply it to your face and your scalp. You do not need another facewash while using this shampoo. It is important that you let the shampoo remain on your skin for at least 5 minutes before rinsing it out. In 4 weeks, you can decrease the frequency with which you use this shampoo to once per week. It is important that you continue to use this shampoo once every week because if you do not, it is likely that the rash will come back. On the days that you do not use the antifungal shampoo, I recommend that you use an over-the-counter shampoo containing either selenium sulfide or zinc pyrithione because these products also have antifungal properties. Examples of brands that contain these ingredients include Selsun Blue and Head & Shoulders. If one of these shampoos that you have been using chronically loses its effectiveness, switch to another type of shampoo; always use at least two different types of shampoos during the week to reduce this possibility. Allergic contact dermatitis (ACD) of the face is a delayed hypersensitivity reaction to immunogenic agents, classically soaps, shampoos, hair dyes, cosmetic agents, and nail polish. The face is one of the most common sites for development of ACD. Common geographic pattern: The major differential diagnoses for facial ACD include ICD, AD, seborrheic dermatitis, and phototoxic drug reactions. Clinical presentation, history, and, in chronic cases, patch testing help establish a diagnosis of facial ACD. General management comments: The recommended initial treatment approach for acute ACD of the face involves multiple steps. What to do if there is a partial but inadequate response after a 4-week trial of topical corticosteroid monotherapy: The rash on your cheeks is caused by allergic contact dermatitis, a skin reaction that develops when your immune system reacts to a product, chemical, or medication in your environment. This rash can be bothersome and itchy but is typically not dangerous and can be controlled with medications. There are a few ways that we manage this rash. First, we want to identify any potential triggers in your day-to-day life. Classic triggers that cause this rash to develop on the face include fragrances, moisturizers, and lotions. You may want to avoid using any skin products that you may have come in contact with recently. If you do not strongly suspect a particular product, however, we do not recommend that you avoid exposing yourself to a number of daily products because this is not usually helpful. In the meantime, we have prescribed you a topical steroid cream to control the rash. You should apply this twice daily on the affected areas of your face for 2 to 4 weeks. Most people tolerate this well over a short period of time, although some say that it causes their blood vessels underneath their skin to become slightly more noticeable. Most patients begin to see their rash resolve within 2 to 4 weeks of consistently using the cream. Some patients also find it helpful to use moisturizers, such as Aquaphor, on their face to protect their skin from further allergen contact. If your rash continues after these treatments, you may be a candidate for a special type of testing to help us identify the product causing your symptoms. This is called “patch testing,” and it is a painless test performed in a dermatologist’s office. During this test, many different allergens are placed on your back and secured with tape. They are kept there for 2 days, after which point they are evaluated to determine if you are allergic to any of the agents. This is often helpful in identifying the cause of the rash; however, it can also sometimes identify products that are not causing your immediate problem. Irritant contact dermatitis (ICD) is caused by physical, chemical, or mechanical damage to the skin and it is a common cause of facial dermatitis.
2: Face dermatitis
Abstract:
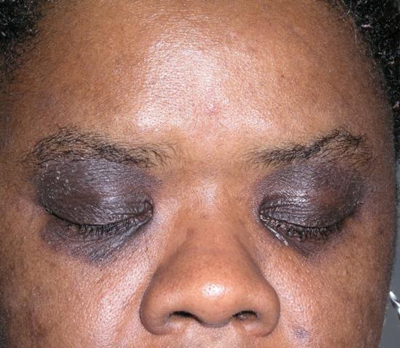
Atopic dermatitis—face
Clinical features
Differential diagnosis
Work-up
Initial steps in management
Warning signs/common pitfalls
Counseling
Periocular and periotic psoriasis (see ch 3, psoriasis)
Seborrheic dermatitis—face
Clinical features
Differential diagnosis
Work-up
Initial steps in management
Antifungals
Antiinflammatories
Warning signs/common pitfalls
Counseling
Allergic contact dermatitis—face
Clinical features
Differential diagnosis
Work-up
Initial steps in management
Warning signs/common pitfalls
Counseling
Irritant contact dermatitis—face
Clinical features
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Face dermatitis