9
The Combined Approach to Atopic Dermatitis
Christopher Bridgett1, Peter Norén2, and Richard Staughton1
1 Imperial College, Chelsea & Westminster Hospital, London, UK
2 Laserkliniken in Uppsala, Department of Medical Sciences, Uppsala University, Uppsala, Sweden
Introduction
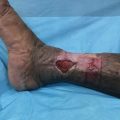
Atopic dermatitis (AD), also commonly known as atopic eczema (Figure 9.1) is an increasingly common, chronic, and debilitating inflammatory skin disease that characteristically runs a chronic course of remissions and relapses, usually beginning in childhood and often remitting by adulthood. Atopy is a descriptive term meaning “strange disease” that was introduced in the 1920s to account for the link between asthma, eczema, infantile food hypersensitivity, and hay fever (seasonal rhinitis) (Figure 9.2). Although some now define atopy as the ability to develop particular antibodies in response to certain environmental allergens [1, 2], a small but significant percentage of individuals with “typical” AD do not show this immune reaction. More fundamental to AD is an impaired epidermal barrier function resulting in dry, itchy, and sensitive skin that is prone to significant bacterial colonization and frequent skin infections [3–6]. Between acute inflammatory and intensely itchy flares, in relative remission the skin in AD may not return to normal but often remains thickened and vulnerable, with the characteristic distribution of lichenification secondary to habitual rubbing and scratching, a common behavioral complication of AD [7]. AD therefore is a chronic condition in two senses: its course is usually longstanding, and both during and between acute episodes the skin shows both clinically and histologically a lichenification related to scratching.

Figure 9.1 Synonymous terms.
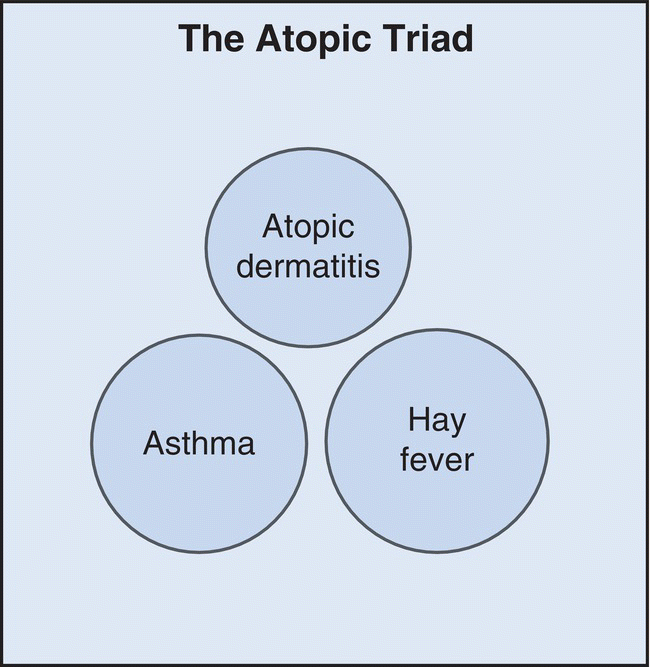
Figure 9.2 The atopic triad.
AD also has important psychosocial correlates. There is a reciprocal relationship with stress, which is reported as a frequent trigger for relapse, while the experience of AD is commonly reported as having an adverse effect on wellbeing and healthy adjustment. In both childhood and adulthood the social ramifications of AD are important, including the triggering of clinical presentation [8, 9].
Conventional treatment of AD targets the impaired epidermal function and the acute inflammatory reaction. Mainstay treatments are therefore the long‐term use of emollient and moisturizing creams and ointments, and intermittent short‐term use of anti‐inflammatory topical corticosteroid creams and ointments. In a recommended stepped approach according to severity, topical immunosuppressant (calcineurin inhibitors) can be introduced, then phototherapy, and then systemic immunosuppressant therapy. Finally and most recently, biologic therapy provides specific, targeted anti‐inflammatory effects by blocking particular and local immune responses (Figure 9.3).

Figure 9.3 Conventional stepped treatment for AD.
Ancillary to these treatments can be added a range of conventional measures depending on clinical judgment, including oral antihistamines, topical antiseptics, topical and oral antibiotics, wet wrap bandaging, and the reduction of contact with environmental allergens (Figure 9.4).

Figure 9.4 Conventional ancillary AD treatment.
Adherence to treatment in AD is seen as the cornerstone of successful treatment [10], while undertreatment of AD, through lack of education and fear of side effects, has been identified as “the biggest problem” [2]. There is an increasing public interest in complementary treatments for AD. It is important that this is taken into account when AD is assessed, as frequently such treatments have been used and continue to be used alongside, or instead of, recommended conventional treatment. The reasons for this include general dissatisfaction with conventional treatment of AD, fear of side effects from conventional treatment, and lack of access to conventional dermatological expertise. It has been noted that alternative therapies are subject to minimal regulation and have been associated with serious side effects. The range of complementary and alternative medicine treatments in use for AD is extensive, reflecting a wide array of cultural and philosophical perspectives (Figure 9.5) [11–14].

Figure 9.5 Complementary and Alternative Treatment for AD.
Within Western medicine there is therefore an increasing recognition of the importance of taking a full biopsychosocial approach to AD in order to maximize treatment outcome. We present here our experience to date with a multidimensional, integrated approach to the treatment of AD that combines optimal conventional treatment with a simple psychological intervention: the behavior modification technique habit reversal for habitual scratching. We find it simple to use, acceptable to our patients, and cost‐effective to provide. In our experience it is feasible to offer our treatment program alongside all of the complementary treatments listed. It is also possible to incorporate into our approach all the conventional treatments listed (Figures 9.3, 9.4), but we see it as important to consider the approach as an option, preferably before introducing systemic treatment.
Our approach to AD originated in the 1980s in Uppsala, Sweden, when one of us (Peter Norén) noted the evident importance of habitual scratching as a cause of the skin lichenification seen in chronic AD. Enlisting the help of colleagues, research then showed that combining a simple behavior modification technique, habit reversal, to eliminate habitual scratching, with optimal treatment with emollients and topical steroids, produced results superior to using conventional treatment on its own [15]. We have since used the treatment program successfully on a routine basis. The program is adapted according to the age of the patient. Our manual for practitioners contains both patient handbooks and clinic protocols [7].
Program for Adults and Older Children
What follows is an outline of our integrated treatment program for chronic AD offered in our clinic for children 16 years and older, as well as for adults. The approach is a staged process (Figure 9.6): assessment, treatment, troubleshooting review, and follow‐up. It has been successfully offered by a variety of clinicians, including nurse practitioners – without any specialist psychological therapy training. The format can be varied according to the circumstances: setting, time available, and needs of the patient. A self‐help version is available [16], intended for use with primary care professional support. A website [17] provides additional support.

Figure 9.6 Treatment stages – adults and older children.
Stage One: The First Visit – Assessment
Nearly all our patients have had AD for a long time and have been at least moderately affected. Between acute relapses the skin remains affected by lichenification, an unstable state of affairs that adds to the likelihood of acute relapses. Almost invariably there are major effects on quality of life and psychological wellbeing, these effects often involving not only the patient. We believe it is important that this demoralizing state of affairs is recognized, taken account of, and discussed at assessment. Active participation is involved, both by the patient and often by significant others, in a treatment regime requiring a positive attitude and a commitment to use what is essentially a self‐help technique. We ourselves have been delighted by the treatment results. It is important and relevant therefore that, right from the start, we share our enthusiasm for the approach with all who come to us for treatment: attitude is contagious.
Initial assessment includes a review of the history of relapses and remissions, subjective review of triggers of acute episodes, and objective review of immune status and sensitivity to particular environmental allergens. Appropriate recommendations can then be made regarding measures to be taken to improve outcome [18].
The approach is an educational program, and is helped by involving others. It is supported by a loose‐leaf patient handbook that is handed out in stages, and into which is written out a discussed and agreed‐upon personal treatment plan. We aim to produce an optimal outcome by first ensuring the nature of the condition and the principles of treatment are properly understood, and then by ensuring the treatment is applied and followed through correctly. There is an important initial discussion on the nature of atopy, on the relationship between AD and allergy, on the significance of dry skin, and especially on the difference between itching and scratching. Dry skin is a common cause of itch in AD. Itch leads to scratching, and repetitive scratching leads to habitual scratching (sometimes without itch), and chronic damage to the skin is the undesirable consequence.
Thus what is happening between episodes of acute AD, during relative remissions, is seen as crucial to understand. Continuing habitual rubbing and scratching
- further disrupts epidermal integrity and barrier function
- enhances the presentation and penetration of allergens, such as dust mite and pet danders [18]
- is a cause in itself of ongoing chronic inflammation.
We explain how this chronic eczema is relatively resistant to treatment with moisturizers and topical steroids, and can lead to the overuse of topical steroids, and steroid side effects.
The Combined Approach therefore adds to the first two levels of conventional treatment – moisturizers and topical steroids – a third level of treatment to deal with habitual scratching, habit reversal. Once this is in place and scratching is significantly reduced, the skin’s histologic architecture can return to normal, and lichenification disappears.
A key initial question asked is, “What percentage of your scratching do you think is due to itch?.” In a series of 50 consecutive patients before treatment, we found a mean 60% of scratching was attributed to itch: the rest was linked to a variety of issues and factors, including stress, opportunity, boredom, frustration, and tiredness – but not itch. Habitual behavior begins with a specific conscious response to a particular stimulus – at first, scratching is due to itch. As time passes however and the behavior is repeated, it becomes relatively automatic and unconscious, and generalizes from being a specific response to itch, to being a general response to a wide range of factors which vary from person to person. Such scratching, or self‐grooming, can be normal and instinctive – and often goes unnoticed: it is unconscious. It cannot however be taken for granted, if chronic atopic eczema is going to be successfully treated.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree