Key Words
short-term medical mission (STMM), orthosis/orthoses, splinting, hand therapy, lower- and middle-income countries (LMICs), visiting medical team (VMT)
Synopsis
This chapter presents information to guide hand therapists in providing care on international short-term medical missions. It reviews principles of hand therapy evaluation and treatment in this setting with recommendations to guide instruction to local therapists in host countries. The goal is to impart hand therapy knowledge and skills to local therapists, in particular splint/orthosis fabrication, promotion of independence, and facilitation of ongoing patient care.
Clinical Issues
Opportunities are expanding for hand therapists to participate in international short-term medical missions (STMMs). From Guatemala to Southeast Asia, lower- and middle-income countries (LMICs) welcome medical teams from more developed countries. These visiting medical teams (VMTs) offer expertise and instruction and introduce materials and resources. As part of the team, hand therapists share their knowledge and skills as they discover new cultures and health care systems. In the process, the therapists’ abilities and creativity are stretched as they provide care in a culture and environment vastly different from their own.
There are several agencies that have established STMMs around the world. The United States–based American Society of Hand Therapists (ASHT) website maintains a list that includes: Guatemala Healing Hands, Health Volunteers Overseas, International Medical Volunteers Association, ReSurge International, United Kingdom–based Sierra Leone, Hands Across Borders, and Medical Teams International.
The Visiting Medical Team
The VMT may include plastic and/or orthopedic surgeons, anesthesiologists, nurses, translators, and a hand therapist. Sometimes the team may be smaller with only surgeons and a therapist. The roles of each team member are not as delineated as they are in hospitals in more developed countries. The team members work closely together and need to be flexible. Hand therapists may be involved in casting, taking photos, transporting patients, and gathering supplies in addition to providing hand therapy.
The relationships that are formed between the VMT and the host medical staff are critical to facilitate the successful exchange of ideas, information, and skills. The receiving hospital typically has a host or point person. Communicating with this person before going on the mission is helpful to establish initial contact, learn about the basic setup of the facility, determine the makeup of the patient list, and find out whether there is a local therapist on staff.
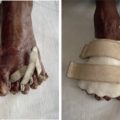
Due to the small window of time that the VMT is at the site, the ability to take care of acutely injured patients is limited. Adult patients may present with healed trauma-related injuries, amputations, burns, arthritis, stroke, nonunion or malunion of fractures, and sub-acute tendon and nerve injuries. In the pediatric population, the team may encounter congenital contractures, cerebral palsy, thumb hypoplasia with radial longitudinal deficiency, burn scars, syndactyly, and polydactyly.
The short-term goals for the VMT include:
- 1.
Providing quality care to as many patients as possible during the 1 to 2 weeks at the host hospital.
- 2.
Teaching and equipping the local staff by transfer of knowledge and skills that can be used to deliver care to the community once the VMT departs.
The effect of the VMT in each of these areas depends on the availability of personnel and physical resources.
The long-term goal of the VMT is to decrease dependency on visiting STMMs and to empower the local health care team to address the needs of its patients.
Hand Therapy in the Developing World
The primary role of the visiting hand therapist includes instructing local therapists and providing evaluation and treatment to both surgical and nonsurgical patients.
The presence of a local physical or occupational therapist or other health care provider interested in serving in the therapist’s role is vital for the transfer of hand therapy techniques and the development of local resources. Both textbooks and lectures that provide visual explanations of therapy intervention can serve as useful resources. However, the hands-on experience, such as working with patients side by side, is instrumental in solidifying the delivery of care in a safe and effective manner. The local practitioners are able to observe hand therapy assessment and treatment, as well as practice splint/orthosis fabrication.
A patient list is created by the host hospital before the visiting team arrives. The VMT typically begins its work with a clinic to evaluate all of the potential patients. Some of the patients will require surgery, and others may be referred for hand therapy intervention only.
Surgical patients may require hand therapy intervention both in the operating room and post-operatively. The VMT surgeons and hand therapist determine whether the patient would benefit from a splint in the operating room to allow more optimal positioning than a cast, as well as early wound monitoring and dressing changes. The splint can be modified after wound healing is complete to maintain optimal positioning.
Post-operative hand therapy includes evaluation, wound care, and treatment including range-of-motion (ROM) exercises, splint fabrication, and home program instruction.
Some of the patients assessed in the initial clinic will not be surgical candidates but will need hand therapy. For example, patients with congenital contractures, arthritic patients with joint stiffness, pain, and weakness, and patients with spasticity may require exercises and splint intervention only.
In general, patients may be seen one to three times by the visiting therapist, depending on how long the VMT is in the country. It is possible for patients to have longer follow-up if there is a competent local therapist. However, this depends on the ability of the patients to travel back to the hospital, the length of time patients can stay in the hospital, and the parameters of the health care system.
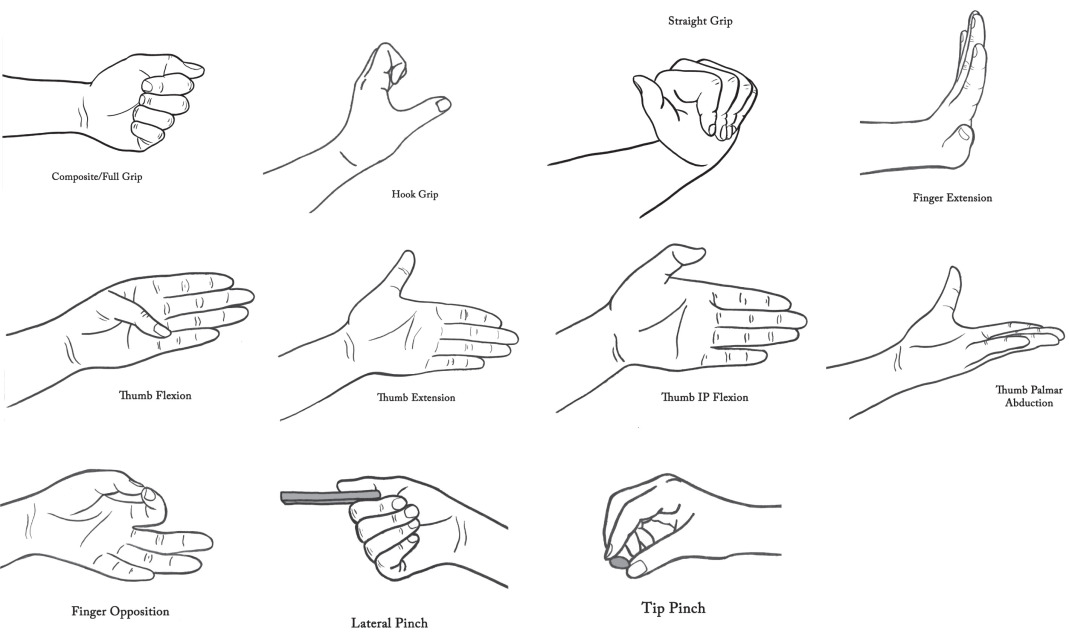
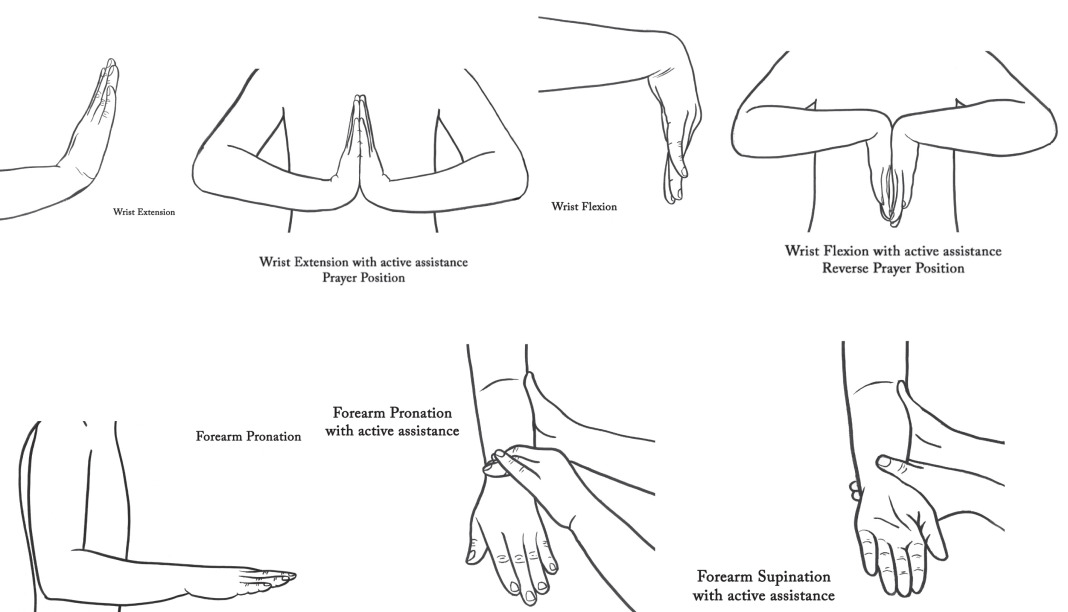
Most likely there will be limited therapist-patient face-to-face time. As a result, a good home program is crucial. It is recommended that the therapist bring exercise sheets with illustrations of the most common upper limb exercises to prescribe to patients. If the patients have access to a cell phone with a camera, they can photograph exercises for reference. If there is a language barrier, having an interpreter is critical, though illustrations and demonstration are needed regardless. Patients or caregivers of young children should demonstrate exercises with the therapist to ensure understanding. Fig. 5.10.1 shows sample illustrations of upper limb ROM exercises that are suitable to use with patients.
Visiting therapists should be culturally sensitive to the norms that influence patient care, communication, and interactions between local therapists and other medical staff. For example, in most developed countries therapists and surgeons work closely together. In other cultures, the surgeons may not work as closely with the therapists; there may be hierarchical norms that influence working relationships.
Hand Therapy Evaluation
The hand therapy initial evaluation needs to be efficient and succinct due to the limited time the therapist has with each patient. As part of the medical team, the therapist should discuss any patient precautions or unique concerns with the surgeons beforehand if it is a post-operative patient. This will optimize the evaluation and recommended treatment. It is also beneficial to gather information regarding the home setup and basic resources available to the patient, such as physical access to the hospital and family support.
The following is an outline of a succinct evaluation suitable for use on STMMs:
- •
Observation: Observe the general appearance and resting position of the affected limb. Is the patient protecting his hand because he appears to be in pain? Is the hand postured abnormally? How does the affected area differ from the noninvolved side? A normal resting posture is typically with the wrist in neutral and the fingers progressively more flexed from the radial to the ulnar side of the hand. Observe for bone prominence, presence and location of wounds, skin color, obvious edema, and the patient’s general health.
- •
Wounds: Observe the general condition of wounds. Is there evidence of infection? Is there potential scar formation that may affect motion?
- •
Sensation: Determine whether there is a change in sensation. What type of sensory change is being experienced? Where is the location?
- •
ROM: Assess the entire limb and limitations in the area of concern. This includes the patient’s abilities to grasp and pinch, with assessment of the distance to touch fingertips to distal palmar crease in composite fist, hook fist, and straight fist, and the ability to make a lateral and 3-point pinch.
- •
Strength: Determine whether the patient is able to move the involved area with gravity eliminated or against gravity. If the patient is unable to move against gravity, is he able to be placed into an anti-gravity position and to sustain it? In addition, patients may need guidance on how to progress their home program from active range of motion (AROM) to resistive tasks.
- •
Functional limitations: How is the patient’s independent function affected?
For non-surgical patients, the evaluation may also include:
- •
Greater emphasis on abilities to perform activities of daily living: Is the patient able to dress, feed, and perform grooming activities independently? Is he/she able to enjoy recreational activities?
- •
Fine motor skills: Is the patient able to use tools and utensils, hold a writing implement, and open packages?
- •
Functional strength: Is there weakness that affects the ability to manipulate heavier or resistive objects? A more thorough manual muscle test, in muscle groups of suspected involvement, may be indicated.
- •
Compensation for limitations: Would adaptive equipment or an orthosis improve positioning or functional abilities?
Hand Therapy Treatment
Treatment in LMICs needs to address patients’ greatest needs and the resources available to them, and must be simple enough for good follow-through. Patient problems to be addressed in this setting include:
- •
Wound care
- •
Scarring
- •
ROM
- •
Edema
- •
Weakness
- •
Hypersensitivity
- •
Splinting/orthotic needs
Wound Care
Determine the stage of wound healing and whether there are any signs of infection. Provide and instruct patients and caregivers in how to appropriately clean the wound and apply dressings.
Scar Care
- •
ROM exercises are needed if the scar crosses over a joint to prevent the scar from limiting motion.
- •
Paper tape use is inexpensive and more readily available than elastomer or silicone gel sheeting. Apply tape along the incision as soon as epithelialization takes place to prevent wound site tension. It is recommended to wash the wound area and replace the tape daily. Getting the tape wet will promote removal.
- •
Massage: Scar massage is recommended at the proliferation stage with a basic lubricant 2 to 3 times per day for 3 to 5 minutes.
Range of Motion
Before addressing ROM, the patient may benefit from use of heat or cold modalities. Be cautious if patients have decreased sensation by monitoring their upper extremity closely.
Use of heat for 15 to 20 minutes before stretching exercises may decrease symptoms of pain and can increase the extensibility of the tissues. Heat causes increased blood flow to the area, and that increases nutrition for aiding healing. Examples of accessible sources of heat are a hot water compress, a raw rice compress in a sock or other enclosed fabric heated with a dry heat source, or soaking in a warm bath.
Application of cold can be less comfortable for patients than heat. A barrier such as a piece of cloth may be used to increase comfort. Cold acts to decrease muscle spasm and can decrease inflammation during early healing. Cold is also beneficial to decrease post-exercise pain. Inexpensive sources of cold include ice (if there is access to a freezer), a cold water compress, or a cold water bath for soaking the extremity.
ROM exercise instructions will include active, active assisted, and passive exercises for appropriate phases of rehabilitation. Most post-surgical and non-surgical patients will need specific active ROM exercises. Positioning and joint motions need to be reviewed and practiced to ensure proper movement of affected joints. It should be emphasized to patients that the exercises will decrease stiffness and edema and preserve or increase gliding between tissues to avoid scar tissue buildup. Exercises for the entire upper limb may be necessary to prevent stiffness and weakness from guarding. It is important to keep programs simple, to provide pictorial references if possible, and to have patients demonstrate understanding by performing the exercises correctly.
Active assisted ROM may include “place and hold” or a combination of active motion with gentle passive assist at end range.
Instruction in controlled passive ROM should include verbally cautioning patients to provide gentle stretching with increased firmness as healing progresses. Patients should avoid sharp or severe pain. More aggressive joint mobilization should not be performed without specific training in this skill.
Edema
Control of edema is crucial to control scar formation and to allow increased mobility.
Use of cold modalities and compression may be beneficial. Compression may be applied with elastic bandage, Coban wrap, or strips of cloth from distal to proximal in a spiral manner with care to avoid constriction. It is recommended that the patient leave the distal tip open to check for adequate circulation without indications of cyanosis or cold or numb fingertips. Patients should position the limb in elevation above the heart level during the day. The arm should also be elevated at night with pillows or on the patient’s chest.
Active exercise also assists to decrease edema. Patients should be instructed to raise their hand overhead and make 5 to 10 strong fists so the muscles act as a pump. This is dependent on the type of surgery. Patients or caregivers may also be instructed in retrograde massage if it is not contraindicated, such as post-fracture.
Weakness
Strengthening exercise instruction should include the careful monitoring of pain and edema. Patients should be instructed to progress slowly; they should not exercise with significant pain. Objects that are readily available should be used for exercise. Examples include squeezing a washcloth, opening a screw-top bottle, pulling up pants, grasping a handle or using hand brakes, peeling a banana, or washing clothes.
Patient engagement in purposeful activities is beneficial to increasing upper-extremity strength, with the added benefits of improving upper limb function and reintegration. It has been observed that many patients have greater use and skill in using the involved extremity when doing tasks instead of performing strengthening exercises alone. Engaging the injured extremity in activities of daily living promotes reintegration of the injured hand into functional daily life and improves endurance.
Hypersensitivity
Hypersensitivity and pain can be addressed with the graded application of textures, tapping, pressure, and vibration. Patients are instructed in a detailed home program to start graded application of input outside the area of hypersensitivity and to progressively work toward the most sensitive areas. Because some patients have more pain with each on/off application of the stimulus, they should be instructed to keep continuous contact with the area and vary the pressure. Typically, the process takes time and persistent effort to decrease symptoms.
Splinting/Orthoses Fabrication
One of the primary patient interventions and skills that the visiting hand therapist teaches the local therapist is fabrication of splints/orthoses. Principles to be reviewed include the goals of splinting, anatomical landmarks, creation of splint patterns, and fabrication of splints with thermoplastic material.
The goals of splinting are to relieve pain, maintain gains in ROM or improved positioning from surgery, protect healing wounds, protect a repair after cast removal, and prevent contracture formation. For non-surgical patients, goals are to provide positioning to improve function, facilitate motion at stiff joints, support a joint to decrease pain, and prevent or improve contractures.
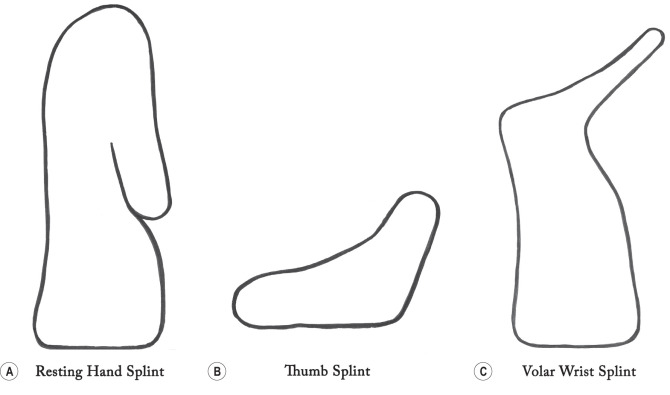
Anatomical landmarks guide splint design to allow freedom of movement of uninvolved joints, prevent pressure over sensitive areas, and ensure proper support of involved joints. The key landmarks that should be reviewed are the distal palmar crease, thenar crease, wrist crease, first web space, and head of the ulna. Fabrication of a splint that allows free finger motion needs to end proximal to the distal palmar crease. Free thumb motion is allowed if the splint does not extend over the thenar crease, and free wrist motion requires a hand-based splint that does not extend proximal to the wrist crease. A splint that covers the ulnar head must have sufficient room over the bony prominence to avoid skin breakdown and discomfort.
Splint design complexity and variety should be limited to promote mastery by the local therapist and to ease placement and removal by the patient. Most patient needs can be addressed with a forearm-based resting hand splint, a hand-based thumb splint, and a volar- or dorsal-based wrist splint with fingers and thumb free. Single-finger and elbow splints should also be included and may not be as complicated as the other designs to a new, inexperienced splint fabricator. These patterns and modifications to the primary three designs may be reviewed as time and learner aptitude permit. The learning therapist should keep a set of the patterns fitted to his own hand for future reference. Fig. 5.10.2 shows examples of splint patterns.