Soft Tissue Coverage of the Knee: Gastrocnemius Muscle Flap
Hani Sbitany
DEFINITION
Soft tissue defects around the knee, or the anterior third of the tibia, often cannot be treated with local fasciocutaneous flaps; instead, the most reliable local/regional coverage option is the rotational gastrocnemius muscle flap.1
This is taken as a pure muscle flap, and in defects that include skin loss, the muscle is immediately skin grafted.
This rotational muscle flap is well perfused, given its axial blood supply, and provides excellent soft tissue coverage and reliable reconstruction of defects involving the underlying bone, tendon, or exposed surgical hardware.2
ANATOMY
The gastrocnemius is a bipennate muscle, located in the superficial posterior compartment of the lower extremity.
Other muscles in this compartment include the soleus muscle and plantaris muscle.
These muscles come together, via their common insertion in the posterior surface of the calcaneus, to create the Achilles tendon.
These muscles act to cause flexion of the ankle, when the knee is extended.
The gastrocnemius muscle is the most superficial of these muscles, situated just deep to the posterior calf skin and subcutaneous tissue, and consists of a medial and lateral muscle head.
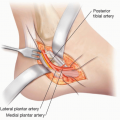
The blood supply to these gastrocnemius muscles comes from the sural artery and vein, which are direct branches from the popliteal vessels; the motor nerve innervation derives from the tibial nerve.
The medial and lateral heads of the gastrocnemius muscles can be separated from each other at their midline confluence, and each muscle belly can be isolated on its medial or lateral sural vessel pedicle, respectively.
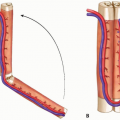
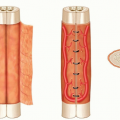
The medial head of the gastrocnemius muscle is usually longer and wider than the lateral head and thus has a greater arc of rotation and reach as a rotational flap; for this reason, the medial head is most commonly harvested for proximal lower extremity reconstruction.3
Because the Achilles tendon is made up of contribution from all four muscles in the superficial posterior compartment, the ankle can still safely flex following harvest of one belly of the gastrocnemius muscle.
PATHOGENESIS
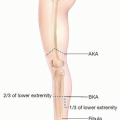
As stated, the gastrocnemius rotational muscle flap is most commonly used for soft tissue reconstruction of defects situation around the knee or the proximal third of the tibia.
There are many possible causes of defects in this region:
Traumatic wounds
Oncologic resection wounds
Soft tissue infection/necrotizing fasciitis
Burn, or burn contracture release, wounds
Breakdown of surgical wound after total knee arthroplasty
These wounds often contain exposed surgical hardware.
Breakdown of wound following patella or patellar tendon repair
PATIENT HISTORY AND PHYSICAL FINDINGS
The cause and chronicity of the soft tissue wound in this area must be carefully defined.
The patient must be questioned for a history of prior lower extremity surgery or injury along the entire limb that may have altered soft tissue anatomy or neurovascular supply.
The specific wound location and size must be recorded and examined carefully to ensure that a rotational gastrocnemius muscle flap will adequately reach this wound with minimal tension.4
With the patient contracting the calf muscles, and flexing the ankle, the distal portion of the gastrocnemius muscle belly can be visualized or palpated, and this is the point that should be used in assessing muscle flap reach.
If this is not the case, then free tissue transfer must be considered.
Physical examination of the knee and ankle must be performed, with range of motion being carefully assessed.
Range of motion at the knee (normal 135 degrees) must be defined, along with confirmation of normal flexion in all positions.
Range of motion at the ankle (normal 70 degrees) must be defined, along with normal flexion with the knee extended.
If exam reveals normal findings, then rotational medial or lateral gastrocnemius muscle flap is safe.
IMAGING
Routine imaging of the lower extremity is not necessary prior to gastrocnemius rotational muscle flap.
If the patient has a history of peripheral vascular disease, a preoperative angiogram or CT angiogram can be obtained, to assess patency of popliteal and sural arteries.
If the patient has a history of deep vein thrombosis, or venous insufficiency, then lower extremity venogram can be performed.
SURGICAL MANAGEMENT
Preoperative Planning
Once the gastrocnemius muscle flap has been chosen as the reconstructive option, the surgeon must determine location of the muscle flap donor incision.
In most cases, for knee defects (anterior, lateral, or medial knee), the muscle harvest incision is separate from the wound being reconstructed, and the muscle is tunneled underneath the intervening skin bridge.
For wounds over the proximal third of the anterior tibia, it is common to extend the harvest incision from the defect, so that they are in continuity.
Positioning
The patient is most commonly placed in a supine position on the operative table.
In some cases, based on wound location and dimensions, it is easier to harvest with the patient in a lateral decubitus position, and this is also acceptable.
When the patient is supine, the entire lower extremity should be circumferentially prepped into the operative field, such that the leg can be moved and manipulated during surgery.
This allows for placement of the leg in a “frog-leg” position, with the knee flexed and turned out, and the foot brought in such that its plantar surface is against the contralateral lower extremity.
This allows for easier harvest of the medial gastrocnemius muscle.
It is also advisable to again check the arc of rotation and the reach of the gastrocnemius muscle, relative to the wound, to ensure successful soft tissue coverage, once the patient is positioned on the table.
Approach
The incision is planned as a longitudinal incision of 10 to 15 cm length.
For the medial or lateral gastrocnemius muscle flap, the anterior border of the muscle is palpated through the skin and marked along its entire length.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree