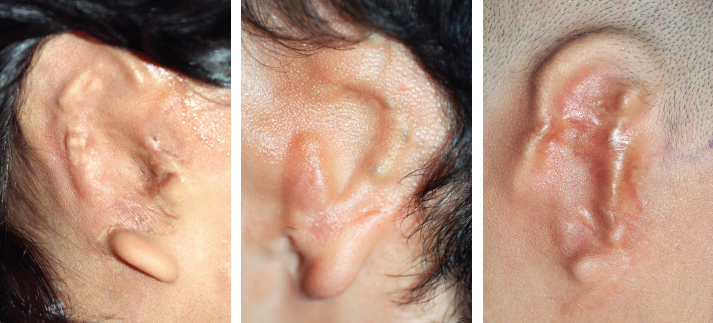
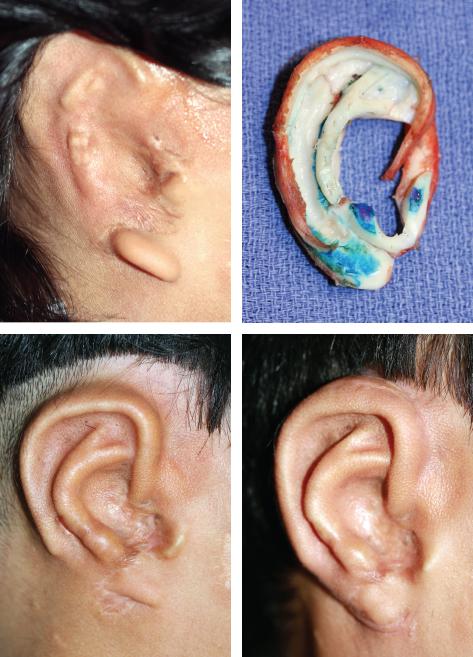
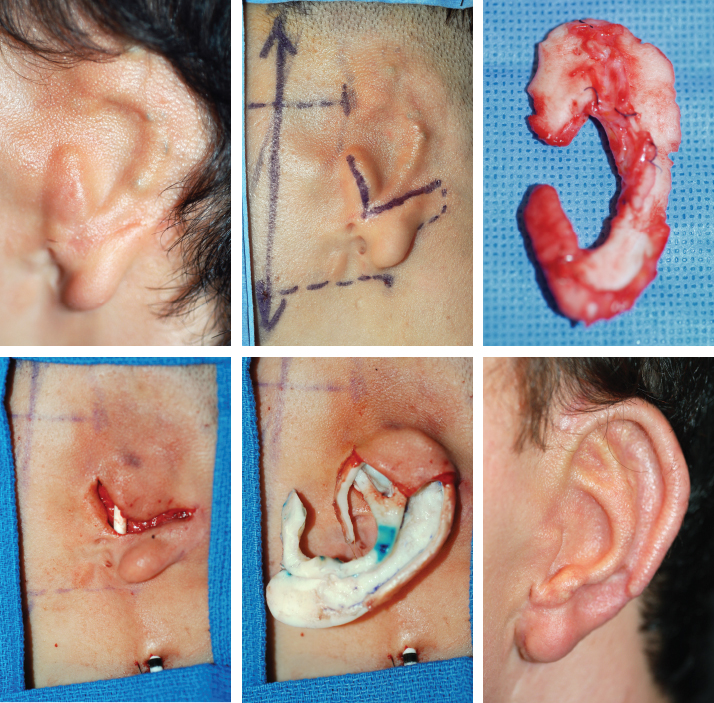
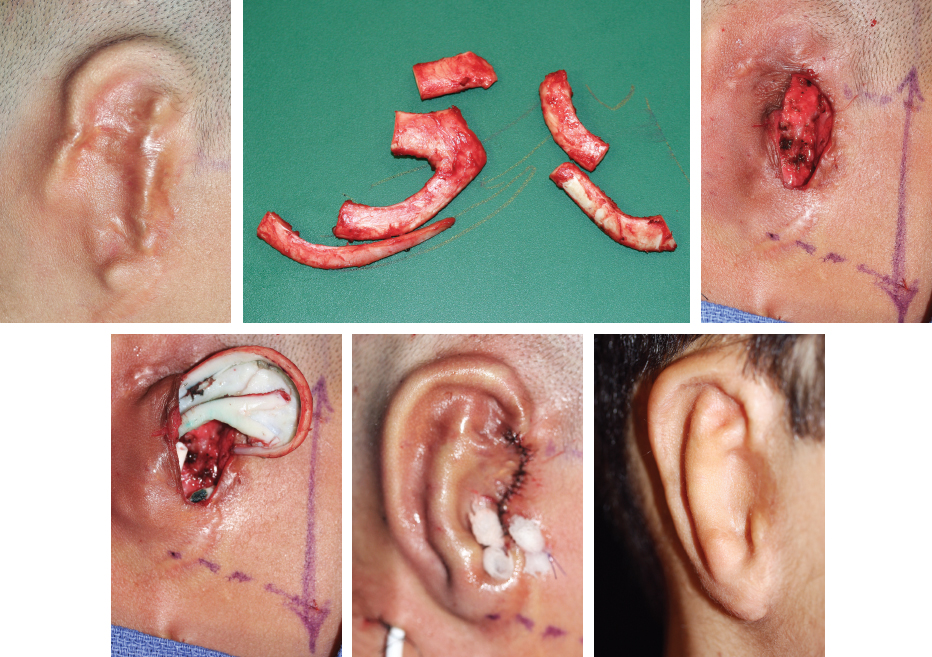
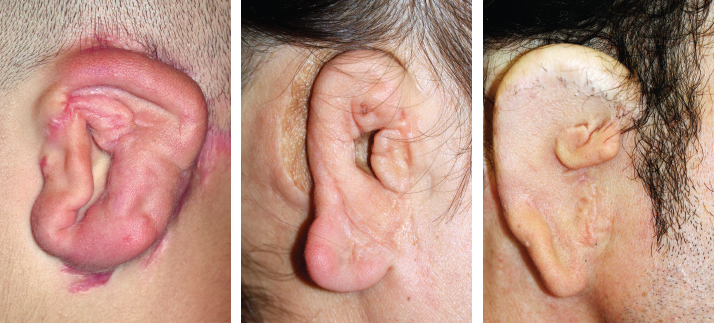
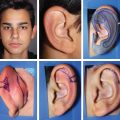
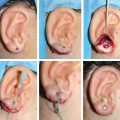
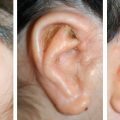
CHAPTER 8 Patients with an unsatisfactory ear reconstruction often seek treatment from another surgeon to correct the problem. These secondary cases can be some of the most difficult reconstructions to perform. Whatever the circumstances, microtia or posttraumatic amputation, the presence of scarring in the auricular region greatly increases the complexity of the required reconstruction. Evaluation of the skin potential is critical and will guide the surgical indication. Most unsatisfactory results are caused by poor definition, because the contours of the ear have not been adequately reproduced. Rarely, some of the contours can be preserved and others corrected. However, in most instances, a new and complete framework must be constructed, which requires harvesting costal cartilage from the contralateral side. In secondary reconstructions, the problem usually is not about harvesting enough cartilage and carving a new framework; rather, it is about appreciating the skin potential, covering the framework, and deciding whether local skin, indirect expansion, or fascial flaps are indicated to form the basis of the reconstruction. A prosthesis should always be considered and discussed with the patient before undergoing a secondary reconstruction, because results of secondary cases may not be as good as those of primary cases. Ear reconstructions for microtia can have many problems. Often, no external auditory meatus is present; therefore the ear may have been positioned poorly, compared with the normal ear. Occasionally, functional surgery can impede the correct placement of a reconstructed ear (if the reconstructed canal is placed ectopically, or bone-anchoring abutments are placed too anteriorly). The scars from canalplasty, for example, can compromise the anterior blood flow to the local skin. Patients may present after the first stage (after insertion of a cartilage framework); more frequently, they present after the second stage (after creation of a retroauricular sulcus). For patients who have had a first-stage reconstruction for microtia with a costal cartilage framework and have a poor aesthetic result, the existing skin cover can generally be used to cover a new framework. In these three patients, the costal cartilage framework has either been inadequately carved or has undergone resorption. A secondary reconstruction is possible and discussed in detail. Françoise Firmin’s Commandments 1. When analyzing an auricular defect, the first step is always to make a model of the normal ear and place it in the ideal position on the affected side. 2. The auricular skin is the best for reconstructing an ear; fascial flaps should only be used when auricular skin is not available. 3. Skin-only flaps without support cannot reproduce the complex contours of an ear, and the best support currently is autologous cartilage. 6. Once the three-dimensional contours of the ear are understood and after training, sculpting should become the routine part of the surgery and management of the skin the difficult part. 8. In choosing a skin approach, surgeons should always consider the existing scars and the position of the remnants. 9. Never elevate an ear whose contours are unsatisfactory after the first stage. This patient with lobular-type microtia underwent the two first stages of Brent’s technique elsewhere: insertion of the framework followed by a transposition of the lobule (type 1 skin approach). Enough skin was available to cover a completely new framework (TYPE I, PI). The former transposed lobule was used to cover the inferior part of the framework, which included the lobule. The result is satisfactory after elevation. This patient had a suboptimal result after a first-stage reconstruction performed elsewhere, with transposition of the lobule (type 1 skin approach). Contours of the ear were inadequately defined, perhaps from resorption of the framework. We used a type 2 skin approach in the secondary surgery to allow repositioning of the lobule and insertion of the framework. The elevated skin eventually adapted well to the contours of the framework. This patient underwent Brent’s first two stages elsewhere. Costal cartilage had been harvested from both sides. CT scans of the thorax demonstrated residual cartilage available, particularly on the right side. A third first stage was possible by harvesting the residual cartilage from both sides to carve a complete framework (TYPE I). The skin approach used the existing scar to create a skin pocket (type 3b), and the existing framework was excised. Pearl When very poor contours are present after the first stage, it is preferable to resculpt a new framework before elevation is performed in a second stage. Secondary reconstructions after the framework has been elevated are more difficult because of the decreased blood supply to the auricular skin flap. The second-stage incision passes around the helical border of the framework; thus, once the deformed framework is removed, the blood supply to the skin pocket comes only from the anterior direction and the branches of the superficial temporal artery. It is essential to correctly analyze whether the use of local skin is possible or whether fascial flaps should be used. These three cases demonstrate that the condition of the local skin may be poor after the second stage of reconstruction. Insertion of a new framework before elevation would have been preferable in these cases. In some patients local skin can be used. If this is not possible, indirect skin expansion and fascial flaps (temporal, occipital, and random-pattern flaps) are considered. COMMANDMENT 9: Never elevate an ear whose contours are unsatisfactory after the first stage.
Secondary Cases
SECONDARY CASES AFTER MICROTIA RECONSTRUCTION
After a First-Stage Reconstruction
After the Second Stage of the Reconstruction
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree